When considering tooth replacement options, dental implants are often highlighted as a superior, long-lasting solution for missing teeth. They offer remarkable stability, function, and aesthetics. However, not everyone is an ideal candidate for this advanced procedure. Understanding “who is NOT a candidate for dental implants” is crucial for making informed decisions about your oral health. This article from Dental Implant Education – Dallas TX will help clarify the factors that may make dental implants unsuitable, ensuring you understand the medical responsibilities involved and what to discuss during a consultation with a dentist.
Key Takeaways
- Certain pre-existing medical conditions, like uncontrolled diabetes or recent cardiovascular events, can prevent you from being a candidate for dental implants.
- Poor oral health, including severe gum disease or insufficient jawbone density, often necessitates preparatory treatments or makes implants unsuitable.
- Specific medications, such as IV bisphosphonates, and certain treatments like head/neck radiation, are significant contraindications.
- Lifestyle choices, particularly smoking, can dramatically reduce the success rate of dental implants and may disqualify a candidate.
- A thorough consultation with a qualified dental professional in Dallas is essential to assess individual candidacy and explore all tooth replacement options.
Quick Answer
While dental implants are highly effective for replacing missing teeth, individuals with certain uncontrolled systemic health conditions, severe oral health deficiencies, specific medication regimens, or lifestyle habits that compromise healing are generally not candidates for dental implants. These factors increase the risks of complications, implant failure, and poor healing, making a thorough pre-assessment by a dental professional critical.
General Health Conditions: Who is NOT a Candidate for Dental Implants Due to Systemic Illness?

Individuals with certain systemic health conditions are generally not candidates for dental implants because these conditions can significantly impair the body’s ability to heal, integrate the implant, or withstand the surgical procedure itself. These health challenges increase the risk of complications and compromise the long-term success of the dental implant procedure [1].
Understanding Systemic Contraindications
Several medical conditions require careful consideration, and in some cases, outright preclude dental implant placement.
- Uncontrolled Diabetes: Patients with uncontrolled diabetes face a higher risk of infection and delayed healing after surgery [1, 5]. Poorly managed blood sugar levels can compromise the body’s immune response and affect bone regeneration, which is vital for the implant to fuse with the jawbone (osseointegration). For those with controlled diabetes, however, successful implant outcomes are possible with proper management and close monitoring [5]. For more information on recovery, see our guide on Diabetic Dental Implant Recovery: Guide for 2026.
- Recent Cardiovascular Events: A recent history of myocardial infarction (heart attack) or cerebrovascular accident (stroke) is a significant contraindication [1, 2, 3]. Elective surgical procedures, including implant surgery, are typically postponed until a patient has stabilized and received clearance from their cardiologist, usually several months after the event.
- Active Cancer or Cancer Therapy: Patients undergoing active cancer treatment, especially chemotherapy or radiation therapy to the head and neck region, are generally not candidates [1, 2]. Radiation can significantly impair bone healing and increase the risk of osteoradionecrosis (bone death) in the irradiated area, making successful osseointegration unlikely and complications severe [5, 6].
- Bleeding Disorders and Coagulation Issues: Uncontrolled bleeding disorders or conditions requiring significant anticoagulation therapy make any surgical intervention, including implant placement, highly risky due to the potential for serious bleeding complications [1, 2]. Management of these conditions must be thoroughly discussed with both the dentist and the patient’s physician.
- Compromised Immune Systems: Conditions that compromise the immune system, such as HIV/AIDS or autoimmune diseases, can increase the risk of infection and impair healing following implant surgery [1, 5]. While not always an absolute contraindication, these cases require additional safety precautions and a detailed risk assessment.
- Severe Systemic Connective Tissue Diseases: Conditions like systemic lupus erythematosus, scleroderma, and severe rheumatoid disease can affect bone quality and the body’s ability to heal, making dental implants a less predictable option [2].
Decision Rule: If you have any of these significant medical conditions, a comprehensive medical evaluation from your physician is necessary before a dental implant consultation. Your dental professional in Dallas will work closely with your medical team to determine the safest and most effective tooth replacement options for your unique health profile.
Oral Health and Lifestyle Factors: Who is NOT a Candidate for Dental Implants Due to Local Conditions or Habits?
Beyond systemic health, a patient’s existing oral health and certain lifestyle choices play a critical role in determining who is NOT a candidate for dental implants. Optimal local oral conditions are essential for the long-term success and stability of the implant.
Assessing Local Oral Health Contraindications
Poor oral hygiene, insufficient bone, and active infections are major roadblocks to successful implant placement.
- Insufficient Jawbone Density or Quality: Dental implants require a sufficient amount of healthy bone in the jaw to fuse with and provide stable support [1, 5]. If there isn’t enough bone due to long-term tooth loss, periodontal disease, or trauma, a bone graft may be necessary to rebuild the bone before an implant can be placed [5]. However, in cases of severe bone loss where grafting is not feasible or successful, patients may not be suitable candidates. For insights into healing after grafting, see our article on Bone Graft Healing for Dental Implants: Your 2026 Timeline.
- Active Periodontal Disease (Gum Disease): Untreated or uncontrolled gum disease is an absolute contraindication for dental implants [1, 5]. The bacteria and inflammation associated with periodontal disease can spread to the implant site, leading to peri-implantitis (implant infection) and eventual implant failure. Any gum disease must be thoroughly treated and under control before implant consideration.
- Poor Oral Hygiene Habits: Patients who do not maintain excellent oral hygiene are at a significantly higher risk of peri-implantitis and implant failure [1, 5]. Dental implants, just like natural teeth, require diligent brushing, flossing, and regular dental check-ups. A commitment to oral care is non-negotiable for implant success.
- Bruxism (Teeth Grinding or Clenching): Severe, uncontrolled bruxism can place excessive force on dental implants, particularly during the critical healing phase, potentially leading to implant failure or damage to the prosthetic crown [5]. While not always an absolute contraindication, managing bruxism (e.g., with a night guard) is essential for candidates who clench or grind their teeth.
- Severe Dental Malocclusion (Bad Bite): An improper bite that places uneven or excessive stress on specific areas can also compromise the longevity of dental implants and their restorations. Correcting severe malocclusion may be a prerequisite for implant placement.
The Impact of Lifestyle Choices
Lifestyle habits can significantly influence the success rate of dental implants.
- Smoking: Smoking is one of the most significant risk factors for dental implant failure [1, 5, 6]. Nicotine constricts blood vessels, reducing blood flow to the surgical site and impairing healing and osseointegration. Smokers also have a higher risk of developing peri-implantitis. Many dental professionals require patients to quit smoking entirely or at least significantly reduce it before and after the implant procedure.
- Alcohol and Drug Abuse: Chronic alcohol abuse and illicit drug use can compromise overall health, immune function, and adherence to post-operative instructions, making patients poor candidates for elective surgeries like dental implants [2, 3]. These habits can also affect bone quality and the body’s ability to heal effectively.
- Poor Nutrition: A diet lacking essential vitamins and minerals can hinder the body’s healing capabilities, which are crucial for successful osseointegration. A balanced diet supports overall health and surgical recovery.
Common Mistake: Many patients underestimate the impact of smoking on implant success. It’s not just a minor risk; it dramatically increases the chance of complications and failure. Dentists in Dallas emphasize strict adherence to smoking cessation guidelines for successful long-term outcomes.
Medications and Treatments: Who is NOT a Candidate for Dental Implants Due to Medical Interventions?
Certain medications and past medical treatments can significantly impact bone metabolism, healing, and overall surgical safety, thus determining who is NOT a candidate for dental implants. It is crucial to provide your dental professional with a complete medical history, including all medications, supplements, and past treatments.
Medications That Can Affect Implant Candidacy
The following medications are particularly important to discuss with your dentist:
- Intravenous (IV) Bisphosphonates: These medications, commonly prescribed for osteoporosis or certain cancers, are a major contraindication for dental implants [1, 4]. IV bisphosphonates can lead to a severe complication called osteonecrosis of the jaw (ONJ), where the jawbone tissue dies and fails to heal, especially after surgical procedures like implant placement. While oral bisphosphonates carry a lower risk, they still require careful evaluation and discussion with both your dentist and physician.
- Anticoagulants (Blood Thinners): Patients taking blood thinners like warfarin, aspirin, or novel oral anticoagulants (NOACs) have an increased risk of bleeding during and after surgery [1]. While minor procedures might be manageable, implant surgery often requires careful coordination with the patient’s physician to potentially adjust medication dosages or temporarily cease medication under medical supervision to minimize bleeding risks.
- Immunosuppressants: Medications that suppress the immune system, often prescribed after organ transplantation or for autoimmune diseases, can increase the risk of infection and impair the healing process [1, 5]. Close collaboration between the dental team and the patient’s medical specialists is vital to manage these risks.
- Steroids (Corticosteroids): Long-term use of corticosteroids can weaken bones and impair the immune response, affecting bone healing and increasing infection risk [1]. This requires careful assessment of the patient’s overall health and the potential impact on implant success.
- Certain Antidepressants: While less common, some antidepressants, particularly selective serotonin reuptake inhibitors (SSRIs), have been linked in some studies to a potential reduction in bone density, which could theoretically impact osseointegration [7]. This is typically a relative contraindication, meaning it requires careful discussion rather than an absolute ban.
Past Medical Treatments as Contraindications
Past treatments can also have lasting effects on eligibility.
- History of Head and Neck Radiation Therapy: As mentioned previously, radiation to the head and neck area severely compromises bone healing and increases the risk of ONJ in the irradiated region [5, 6]. This makes the placement of dental implants in previously radiated areas highly risky and often contraindicated. The extent of radiation and the time since treatment are critical factors in assessment.
- Chemotherapy: Recent or ongoing chemotherapy treatments can suppress the immune system and impair healing, making it ill-advised to undergo elective dental surgery. Patients are typically advised to complete their chemotherapy regimen and achieve medical clearance before considering implants.
Edge Case: Patients with a history of head and neck radiation therapy might still be candidates for dental implants in non-radiated areas of the mouth, or in specific cases, with advanced pre-surgical preparations such as hyperbaric oxygen therapy. However, these are complex situations requiring extensive evaluation and specialized care.
| Factor | Potential Impact on Dental Implant Candidacy | Recommendation |
|---|---|---|
| Uncontrolled Diabetes | Impaired healing, infection risk | Achieve blood sugar control; medical clearance required |
| Recent Heart Attack/Stroke | Surgical risk, healing complications | Postpone surgery until medically cleared, typically 6-12 months [1, 3] |
| IV Bisphosphonate Use | High risk of Osteonecrosis of the Jaw (ONJ) | Absolute contraindication; alternative tooth replacement options considered [4] |
| Active Gum Disease | Infection, implant failure | Must be treated and controlled before implant placement [5] |
| Smoking (Heavy) | Reduced healing, increased failure rate | Smoking cessation highly recommended, often required [5, 6] |
| Insufficient Jawbone | Lack of support for implant | Bone grafting may be needed; severe cases may preclude implants [5] |
| Head/Neck Radiation (Past) | Impaired bone healing, ONJ risk | May be an absolute contraindication in irradiated areas [6] |
| Poor Oral Hygiene | High risk of peri-implantitis | Commitment to excellent oral hygiene is mandatory |
What Happens During a Dental Implant Consultation in Dallas?
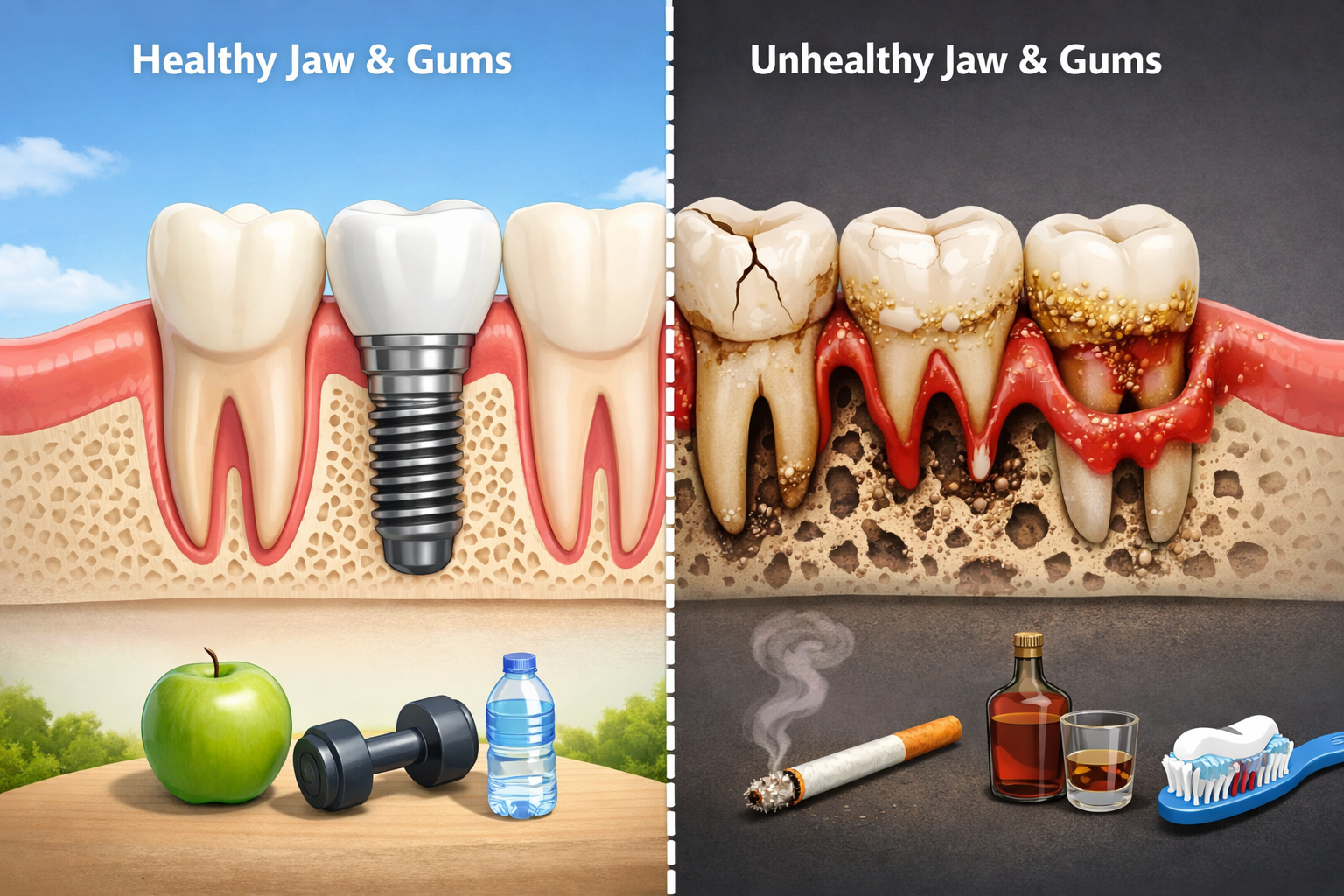
Understanding who is NOT a candidate for dental implants is the first step; the next is a professional evaluation. During a dental implant consultation in Dallas, a qualified dentist or oral surgeon will perform a thorough assessment to determine your eligibility and discuss all available tooth replacement options. This process is comprehensive, patient-focused, and ensures your safety and the long-term success of any treatment plan.
The Assessment Process
A dental implant consultation typically involves several key components:
- Comprehensive Medical and Dental History Review: This is where you disclose all health conditions, medications (including over-the-counter and supplements), allergies, and past surgeries [7]. Be open and honest about your habits, like smoking or alcohol consumption. This information is critical for identifying any potential contraindications or risks.
- Thorough Oral Examination: The dentist will examine your mouth, focusing on the site of missing teeth, the health of your remaining teeth, and the condition of your gums. They will look for signs of gum disease, infections, and assess your overall oral hygiene [7].
- Advanced Imaging: X-rays, including panoramic X-rays and often 3D cone-beam computed tomography (CBCT) scans, are essential. These images provide detailed views of your jawbone structure, nerve locations, and sinus cavities, allowing the dentist to assess bone density, volume, and identify any anatomical limitations [7].
- Discussion of Treatment Goals and Expectations: Your dentist will talk with you about what you hope to achieve with dental implants, explain the procedure in detail, including potential risks and benefits, and set realistic expectations for the outcome and recovery.
- Assessment of Candidacy and Alternative Options: Based on all the gathered information, the dentist will determine if you are a suitable candidate for dental implants. If you are not, or if there are significant risks, they will discuss alternative tooth replacement options such as dental bridges or dentures, explaining their pros and cons. They might also suggest preparatory procedures like bone grafting if needed to improve candidacy.
Why a Local Expert is Essential
Choosing a local Dallas dental professional for your implant consultation ensures:
- Personalized Care: You receive tailored advice based on your specific oral health needs and general medical profile, provided by someone familiar with local patient demographics and dental standards.
- Continuity of Care: Establishing a relationship with a local dentist allows for consistent follow-up appointments, which are vital for monitoring implant healing and long-term maintenance. For details on ensuring lasting success, read about Dallas Dental Implant Follow-Up: Ensuring Lasting Smile Suc.
- Access to Immediate Care: Should any dental implant complications in Dallas arise, a local specialist can provide prompt and effective intervention.
- Understanding of Local Financing Options: A local clinic can also guide you through Dallas Dental Implant Financing Options | Payment Plans 2025 specific to the area.
The Role of Age in Dental Implant Candidacy
While often a concern for many patients, advanced age alone is generally NOT a direct contraindication for dental implants [9]. The critical factors are a patient’s overall health, bone density, and ability to heal, rather than their chronological age [9].
Age-Related Considerations
- Overall Health is Key: A healthy 80-year-old with good bone density and well-managed systemic conditions may be a better candidate than a 50-year-old with multiple uncontrolled health issues [9]. The focus is always on physiological health rather than just the number of years.
- Healing Capacity: As individuals age, their healing capacity might slow down slightly, but it doesn’t typically prevent successful osseointegration. Dental professionals in Dallas are experienced in managing recovery for older patients, including offering tailored post-operative instructions. For more specific information, check out our guide on Senior Dental Implant Healing Time: Guide for 2026.
- Bone Density: Bone density can decrease with age, especially in women due to osteoporosis. However, localized bone loss in the jaw can often be addressed with bone grafting procedures. A thorough 3D imaging assessment is vital to evaluate bone quality and quantity regardless of age.
- Medication Review: Older adults often take multiple medications. A detailed review of all prescriptions is crucial to identify any potential contraindications or interactions that could impact implant success.
- Desire for Improved Quality of Life: Dental implants can significantly improve the quality of life for seniors by restoring chewing ability, speech, and confidence. Many older patients seek implants to enjoy their food, maintain nutrition, and socialize without embarrassment, making it a highly desirable tooth replacement option.
Important Note: While age isn’t a barrier, some very young individuals (typically under 18) are not candidates for dental implants because their jawbones are still developing [1]. Implant placement before jaw growth is complete can lead to complications as the surrounding natural teeth continue to shift.
When Are Dental Implants Absolutely Contraindicated?
While many conditions are relative contraindications that can be managed or resolved, there are specific scenarios where dental implants are absolutely contraindicated, meaning they cannot or should not be placed under any circumstances due to severe risks to patient health or a near-certain chance of failure.
Absolute Contraindications to Be Aware Of
- Active Intravenous Bisphosphonate Therapy: Patients currently receiving or with a history of IV bisphosphonate treatment (e.g., Aredia, Zometa) are at extremely high risk for osteonecrosis of the jaw (ONJ) if a surgical procedure like implant placement is performed [1, 4]. This complication is severe, difficult to treat, and can lead to significant morbidity.
- Recent Myocardial Infarction (Heart Attack) or Cerebrovascular Accident (Stroke): Within a specific timeframe (usually 6-12 months) of a major cardiovascular event, elective surgeries are strictly avoided due to the increased risk of further cardiac or neurological events under surgical stress [1, 3].
- Untreated or Uncontrolled Malignancy (Cancer): For patients with active cancer, especially those with tumors in the head and neck region, or those undergoing active radiation or chemotherapy, dental implant placement is contraindicated [1, 2]. The procedure could exacerbate the cancer, interfere with treatment, or lead to severe healing complications.
- Severe, Uncontrolled Bleeding Disorders: Conditions like severe hemophilia or other severe coagulopathies that cannot be adequately managed pose an unacceptable risk of life-threatening hemorrhage during and after surgery [2].
- Severe Immunocompromised States (e.g., uncontrolled HIV/AIDS, severe active autoimmune disease): In cases where the immune system is severely compromised and cannot adequately fight infection or heal, the risk of overwhelming infection and implant failure is too high [1, 5].
- Pregnancy and Lactation: While not a permanent contraindication, elective dental surgeries, including implant placement, are typically postponed during pregnancy and lactation to avoid exposing the fetus or infant to medications (anesthetics, antibiotics) and to minimize stress on the mother [1, 2].
- Active Substance Abuse (Drugs or Alcohol) and Severe Psychiatric Illnesses: Patients with active drug or alcohol addiction or severe, uncontrolled psychiatric conditions may be unable to comply with essential pre- and post-operative instructions, compromising their safety and the success of the implant [2, 3].
Important Distinction: It’s vital to differentiate between an absolute contraindication, which means “do not proceed,” and a relative contraindication, which means “proceed with caution, possibly after managing the underlying issue.” For instance, controlled diabetes is a relative contraindication, while uncontrolled diabetes is often considered an absolute one until control is achieved.
Alternatives for Missing Teeth When Implants Aren’t an Option

If you’ve been informed that you are not a candidate for dental implants, either temporarily or permanently, it’s reassuring to know that other effective tooth replacement options are available to restore your smile and oral function. The goal remains to find a solution that is safe, effective, and suits your individual needs and health profile.
Common Tooth Replacement Options
- Dental Bridges: A dental bridge uses crowns on adjacent natural teeth (abutments) to support a false tooth (pontic) that “bridges” the gap left by a missing tooth [8].
- Pros: Can be a quick solution, restores aesthetics and chewing function, doesn’t require surgery.
- Cons: Requires modifying healthy adjacent teeth, does not stimulate the jawbone (leading to bone loss over time), and has a shorter lifespan than implants.
- Consideration: For a detailed comparison, see Dental Bridge vs. Implant Cost in 2025.
- Partial Dentures: Removable partial dentures consist of replacement teeth attached to a gum-colored plastic base, connected by a metal framework or clasps that attach to your natural teeth.
- Pros: Less invasive, generally more affordable upfront, can replace multiple missing teeth.
- Cons: Removable (can feel less secure than fixed options), may affect speech and eating, can put stress on supporting natural teeth, does not prevent bone loss.
- Complete Dentures: If all teeth in an arch are missing, complete dentures (full dentures) are an option. They are custom-made to fit over your gums and can restore the appearance and some function.
- Pros: Replaces all teeth, generally cost-effective, non-invasive.
- Cons: Can be unstable, may slip or click, requires adhesives, does not prevent jawbone shrinkage, can make eating certain foods difficult.
- Implant-Supported Dentures (Hybrid Option): While you might not be a candidate for individual implants, some patients may still be eligible for a limited number of implants to support a full denture, offering greater stability than traditional dentures without requiring an implant for every missing tooth. This often depends on the specific reasons for initial contraindication.
- Consideration: Explore Removable Dental Implant Options for a Stable Smile | 2025 Guide.
- No Treatment (Leaving the Gap): While often not recommended, simply leaving a missing tooth untreated is an option.
- Cons: Can lead to adjacent teeth shifting, opposing teeth supra-erupting, bone loss in the jaw, difficulty chewing, altered speech, and impact on self-confidence and appearance.
Scenario Example: A patient with severe, uncontrolled gum disease and significant bone loss is not a candidate for dental implants. After successful treatment of their gum disease, they may still lack sufficient bone for implants. In this case, a dental bridge might be considered if healthy adjacent teeth are available, or a removable partial denture if multiple teeth are missing and a fixed option is not suitable. The choice hinges on the patient’s oral health, aesthetic goals, and budget.
Frequently Asked Questions
Can I get dental implants if I have osteoporosis?
Yes, having osteoporosis does not automatically make you ineligible for dental implants. The primary concern is jawbone density and the medications used to treat osteoporosis, particularly IV bisphosphonates, which can be a contraindication [4, 5]. Oral bisphosphonates require careful evaluation but are not always an absolute barrier.
Is age a barrier to getting dental implants?
No, advanced age itself is not a barrier to dental implants. A person’s overall health, bone density, and ability to heal are more important than their chronological age [9]. Many healthy seniors are excellent candidates.
Can smokers get dental implants?
While not an absolute contraindication, smoking significantly increases the risk of implant failure and complications like peri-implantitis [1, 5]. Many dentists strongly recommend or require patients to quit smoking before and after the procedure to improve success rates.
What if I have gum disease?
Active gum disease is an absolute contraindication for dental implants [1, 5]. It must be treated and completely under control before any implant procedure can be considered to prevent infection and failure.
Do I need enough jawbone for dental implants?
Yes, sufficient jawbone density and volume are crucial for the stability and long-term success of dental implants [5]. If you have insufficient bone, procedures like bone grafting may be recommended to build up the site before implant placement.
Can I get dental implants if I have uncontrolled diabetes?
Uncontrolled diabetes increases the risk of infection and impairs healing, making dental implants generally not recommended until blood sugar levels are well-managed [1, 5]. Patients with controlled diabetes, however, can often successfully receive implants.
Are there any medications that prevent dental implants?
Yes, certain medications like intravenous (IV) bisphosphonates are a major contraindication due to the risk of osteonecrosis of the jaw (ONJ) [1, 4]. Other medications, such as blood thinners or immunosuppressants, require careful evaluation and management with your medical doctor.
What happens if I’m not a candidate for dental implants?
If you are not a candidate for dental implants, your dental professional will discuss alternative tooth replacement options, such as dental bridges, partial dentures, or complete dentures, which can still effectively restore your smile and chewing function.
Conclusion
Understanding who is NOT a candidate for dental implants is an essential part of the journey toward restoring your smile. While dental implants offer a remarkable and durable solution for missing teeth, they are a surgical procedure that requires specific health and oral conditions for successful integration and long-term stability. From systemic health issues like uncontrolled diabetes or recent cardiovascular events to localized oral problems like severe gum disease or insufficient jawbone, and even specific medications or lifestyle choices such as smoking, various factors can influence candidacy.
At Dental Implant Education – Dallas TX, we emphasize medically responsible guidance and patient-first care. Our goal is to ensure you are fully informed about all aspects of dental implant procedures, including the potential risks and contraindications. If you are researching tooth replacement options in Dallas, the most crucial next step is to schedule a comprehensive consultation with a qualified dental professional. They can thoroughly evaluate your unique medical and dental history, assess your oral health, and utilize advanced imaging to determine the safest and most effective path forward for your long-term oral health. Even if implants aren’t suitable, there are always viable alternatives to help you achieve a confident, healthy smile.
Key Takeaways
- Uncontrolled systemic health conditions (e.g., uncontrolled diabetes, recent heart attack/stroke, active cancer) significantly impact dental implant candidacy.
- Poor oral health (severe gum disease, insufficient bone) and lifestyle factors (smoking, poor hygiene) are common local contraindications.
- Certain medications, especially IV bisphosphonates, and radiation therapy to the head/neck area, are critical factors preventing implant placement.
- Age is typically not a contraindication; overall health and healing capacity are more important.
- A thorough consultation with a dental professional in Dallas is essential to assess individual eligibility and discuss all available tooth replacement options.
- If not a candidate for implants, alternatives like dental bridges or dentures remain effective solutions for missing teeth.
- Making informed decisions requires transparent discussions with your dental and medical teams.
- Prioritizing patient safety and long-term oral health is paramount throughout the treatment planning process.
References
[1] Contra Indications For Dental Implants – https://www.dentavacation.com/contra-indications-for-dental-implants/
[2] Contraindications For Dental Implantation – https://alpha-dent.net/de/contraindications-for-dental-implantation/
[3] Contraindications To Dental Implant Placement – https://www.dentaldidacticsce.com/blog/contraindications-to-dental-implant-placement/
[4] Watch – https://www.youtube.com/watch?v=PDcX1P6JIDE
[5] When Is A Dental Implant Not Recommended – https://www.toothsomeimplantsbaulkhamhills.com.au/when-is-a-dental-implant-not-recommended/
[6] Who Should Avoid Dental Implants – https://greatlakesda.com/blog/who-should-avoid-dental-implants/
[7] Contraindications To Dental Implant Placement – https://www.smilesforlifedentalgroup.com/blog/contraindications-to-dental-implant-placement/
[8] Implants – https://www.uhcprovider.com/content/dam/provider/docs/public/policies/dental/implants.pdf
[9] Is Age A Contraindication For Dental Implants – https://www.gentledentistrytampa.com/is-age-a-contraindication-for-dental-implants/


Leave a Reply
Share your thoughts or ask a question about dental implants. Your email address will not be published.