Quick Answer: Tooth resorption is a complex dental condition where parts of a tooth’s structure — either enamel, dentin, or cementum — are progressively lost due to the activity of specific cells. This process can occur internally or externally, often progressing without symptoms until significant damage is present, making early detection crucial for effective treatment and preserving oral health.
Key Takeaways
- Tooth resorption involves the breakdown of tooth structure by the body’s own cells, leading to cavities or defects.
- It can be internal (starting inside the tooth) or external (starting on the root surface).
- Causes range from trauma and orthodontics to infection and genetics, often remaining unclear.
- Symptoms are often absent in early stages, making routine dental check-ups essential.
- Diagnosis typically involves dental X-rays and sometimes advanced imaging like CBCT scans.
- Treatment varies by type and severity, from root canal therapy to tooth extraction and replacement.
- Early detection significantly improves the prognosis and can prevent tooth loss.
- In some cases, if a tooth cannot be saved, dental implants in Dallas offer a reliable solution for missing teeth.
- Regular oral health education is key to understanding and addressing this condition effectively.
What Exactly is Tooth Resorption?
Tooth resorption is a condition where the hard tissues of a tooth, such as the cementum, dentin, and sometimes the enamel, begin to break down and are reabsorbed by the body. This is distinct from typical tooth decay, which is caused by bacteria, and instead involves specialized cells that normally remodel bone. The process can affect any part of the tooth, from its external surface to its internal pulp chamber, and can lead to significant structural compromise if left untreated.
Resorption can be broadly categorized into two main types: external and internal. External resorption, the more common form, originates from the outer surface of the tooth root, while internal resorption starts within the pulp chamber. Understanding the specific type is critical for determining the most appropriate course of treatment to address the damage.
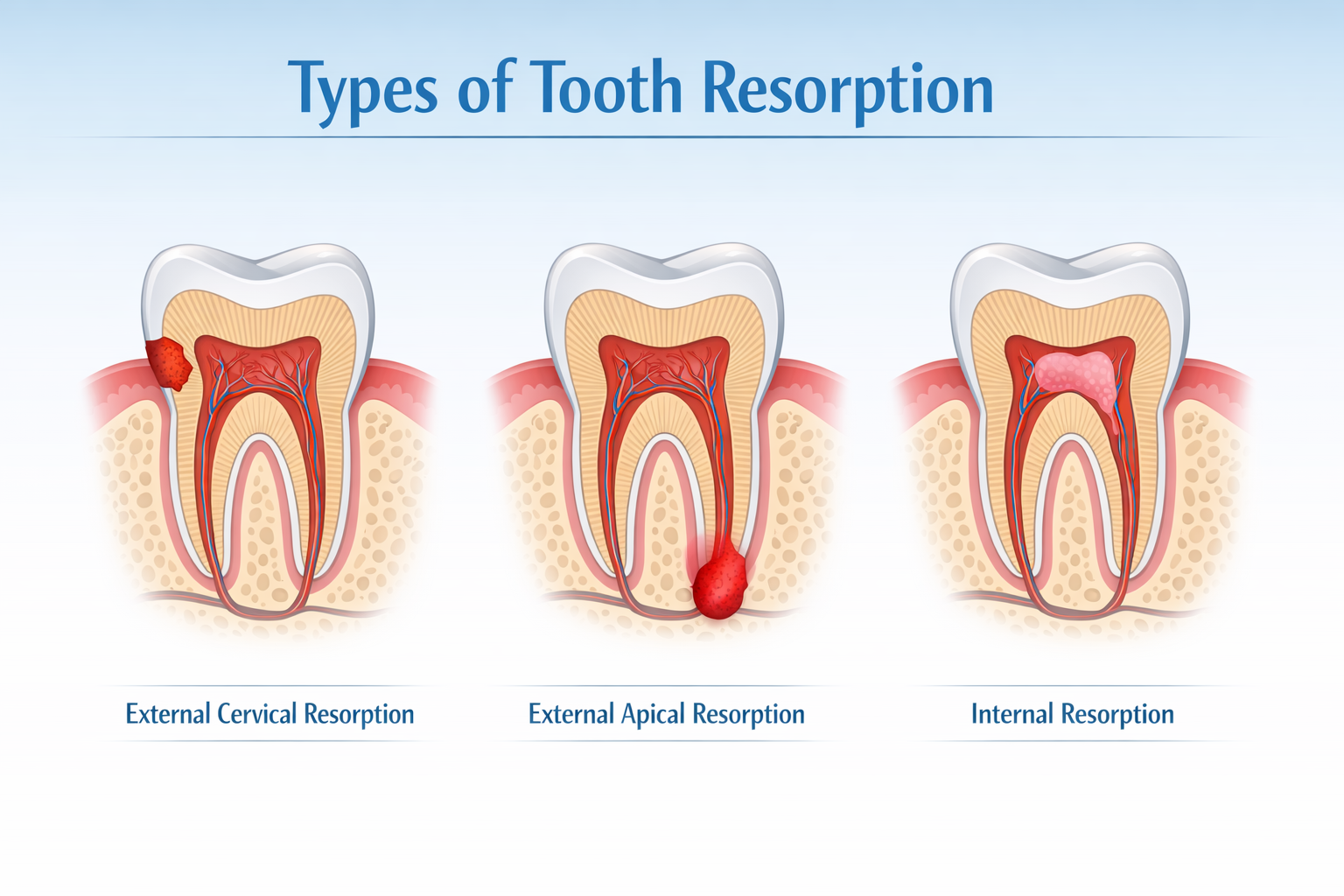
Understanding the Different Types of Tooth Resorption
Tooth resorption manifests in several forms, each with distinct characteristics and origins, requiring tailored diagnostic and treatment approaches. Identifying the specific type of tooth resorption is the first crucial step toward effective management.
- External Cervical Resorption (ECR): This is one of the most common and often aggressive forms of external resorption. It typically begins at the gumline (cervical area) and progressively invades the tooth structure. ECR is often insidious, meaning it can advance significantly without causing noticeable symptoms, sometimes appearing as a pinkish discoloration on the tooth if the pulp is involved. Causes are often linked to trauma, orthodontic treatment, or dental procedures.
- External Apical Resorption (EAR): Affecting the very tip (apex) of the tooth root, EAR is frequently associated with orthodontic forces or chronic inflammation from issues like periodontal disease or dental trauma. It usually involves a gradual blunting or shortening of the root end, which can be seen on dental X-rays. While some degree of EAR is common after orthodontic treatment, excessive loss can compromise tooth stability.
- External Surface Resorption: This mild and typically self-limiting form involves small, superficial areas of the root surface. It often occurs after minor trauma or pressure and, in many cases, the body repairs itself by depositing new cementum in the affected area, making intervention unnecessary.
- Internal Resorption: This type originates within the pulp chamber of the tooth and progresses outwards. It is usually caused by chronic inflammation of the pulp, often due to trauma or infection that has gone untreated. Internal resorption can present as a uniform, balloon-like enlargement of the root canal space on an X-ray, sometimes referred to as a “pink tooth” if the resorptive tissue reaches the enamel.
What Causes Tooth Resorption and Who is at Risk?
Tooth resorption can be triggered by a variety of factors, often making it challenging to pinpoint a single cause, but some risk factors are well-established. These factors often create an environment where the body’s own cells mistakenly begin to break down tooth structure.
While the exact mechanisms are not always fully understood, several predisposing conditions and events are commonly associated with the development of tooth resorption. Identifying these can help patients and dentists in Dallas understand individual risk and potentially implement preventive strategies.
Common Causes and Risk Factors
- Dental Trauma: A history of tooth injury, such as a knock or blow, is a significant risk factor for both internal and external resorption, which can develop months or even years after the initial event. The trauma can damage the protective layer of the tooth, allowing resorptive cells to activate.
- Orthodontic Treatment: While modern orthodontics is generally safe, the forces applied during tooth movement can sometimes lead to external apical resorption. This is usually mild, but severe cases require careful monitoring and management by an orthodontist.
- Dental Procedures: Certain dental procedures, including bleaching (especially internal bleaching), pulp capping, and even some restorative treatments, have been linked to an increased risk of resorption. The chemicals or physical stress involved can sometimes initiate the resorptive process.
- Chronic Infection/Inflammation: Prolonged inflammation within the tooth (pulpitis) or surrounding the root (periodontitis) can stimulate resorptive cells. For example, an untreated cavity leading to pulp infection can cause internal resorption.
- Periodontal Disease: Chronic gum disease can expose the root surfaces, making them more vulnerable to external resorption, particularly at the cervical area.
- Genetic Predisposition: Some individuals may be genetically more prone to developing tooth resorption, even without obvious external triggers.
- Impacted Teeth: Teeth that fail to erupt fully and remain embedded in the jawbone can sometimes exert pressure on adjacent teeth, leading to resorption of the neighboring root. Wisdom teeth are a common example where impaction can affect second molars.
How is Tooth Resorption Diagnosed and What are the Symptoms?
Diagnosing tooth resorption can be tricky because it often progresses silently, without noticeable symptoms, until it has caused significant damage. However, recognizing subtle signs and utilizing advanced diagnostic tools are key for early intervention and preserving the affected tooth.
Regular dental check-ups, especially in Dallas, are paramount for detecting these issues, as a dentist may spot abnormalities during routine examinations or through X-rays even before a patient experiences any discomfort.
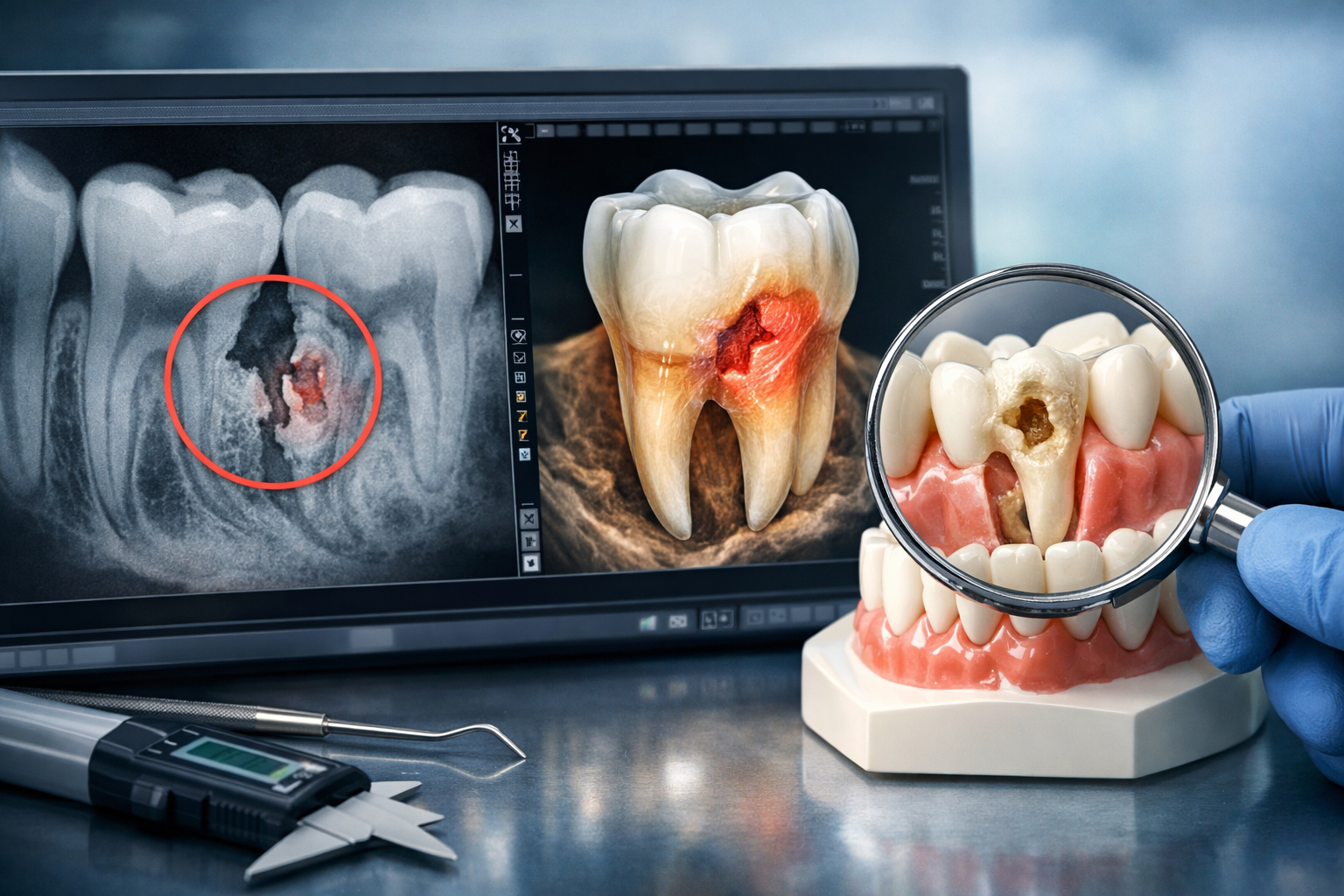
Key Diagnostic Methods and Potential Symptoms
- Routine Dental X-rays: Periapical and bitewing X-rays are usually the first line of defense. They can reveal early signs of bone loss around the tooth or changes in the root canal shape, indicating internal or external resorption. These are standard during annual check-ups.
- Clinical Examination: Your dentist might notice a pinkish discoloration on the tooth crown (suggesting internal resorption) or detect a rough or eroded area near the gumline during a visual inspection or with a dental probe (indicating external cervical resorption).
- Cone Beam Computed Tomography (CBCT): For a definitive diagnosis and to understand the full extent and three-dimensional nature of the resorption, a CBCT scan is often necessary. This advanced imaging provides detailed cross-sectional views, which are crucial for treatment planning, especially for complex cases of external cervical resorption.
- Pulp Vitality Tests: These tests (e.g., cold test, electric pulp test) determine the health of the tooth’s nerve. In cases of internal resorption, the pulp might still be vital, whereas in advanced external resorption, the pulp can become necrotic (dead) due to invasion.
- Symptoms (when present):
- Pain: While often asymptomatic, some individuals may experience mild to severe pain, especially if the resorption is deep or if the pulp becomes infected.
- Sensitivity: Increased sensitivity to hot or cold temperatures.
- Swelling: Swelling or redness in the gums surrounding the affected tooth.
- Pink Spot on Tooth: A visible pink or reddish area on the tooth crown, which can indicate extensive internal resorption nearing the surface.
- Tooth Mobility: In advanced stages, significant loss of tooth structure can lead to the tooth becoming loose.
- Tooth Fracture: Severely weakened teeth can unexpectedly fracture.
If you experience any of these symptoms or have a history of dental trauma, it’s vital to schedule a consultation with a dentist in Dallas promptly.
Treatment Options for Tooth Resorption
The treatment for tooth resorption depends heavily on its type, location, and the extent of the damage. The primary goal is to halt the resorptive process, preserve the tooth structure, and restore its function and aesthetics. In some advanced cases, saving the tooth may not be possible, leading to discussions about tooth replacement options.
A comprehensive assessment, often including advanced imaging like CBCT, guides the treatment plan. It’s important to have a consultation with a dentist who has experience in managing these complex conditions to determine the best approach for your long-term oral health.
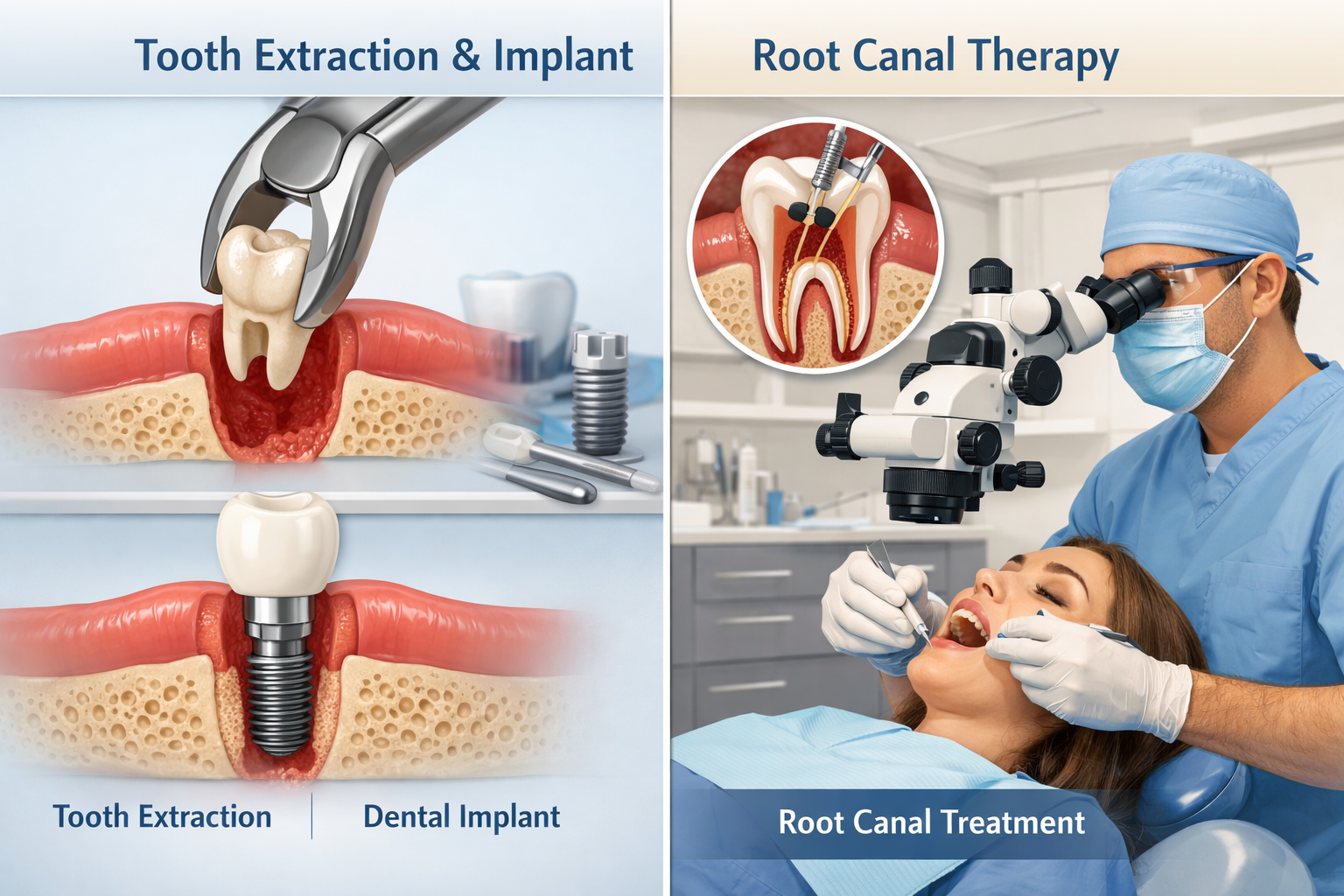
Common Treatment Approaches
- Monitoring (for mild external surface resorption): In very minor cases of external surface resorption, especially after trauma, the body may spontaneously repair the damage. Regular monitoring with X-rays might be the initial approach to see if the condition resolves itself.
- Root Canal Therapy (Endodontic Treatment): For internal resorption, and sometimes for external resorption that has perforated into the pulp, root canal therapy is the standard treatment. This procedure involves removing the inflamed or infected pulp tissue, thoroughly cleaning the root canal system, and filling it to prevent further breakdown.
- Surgical Intervention:
- External Cervical Resorption (ECR) Treatment: Early ECR can sometimes be treated by surgically removing the resorptive tissue from the tooth surface, followed by restoration with a tooth-colored filling material. This approach requires precise access and removal of all affected tissue to prevent recurrence.
- Intentional Replantation: In specific, challenging cases, a tooth might be extracted, the resorptive lesion removed and restored outside the mouth, and then the tooth replanted into its socket. This is a complex procedure with specific indications.
- Orthodontic Management: If resorption is linked to orthodontic forces, adjustments to treatment mechanics or even a temporary cessation of tooth movement might be necessary.
- Tooth Extraction: When resorption is extensive, has severely weakened the tooth, or if treatment attempts have failed, extraction may be the only viable option. This is often the case when the tooth is deemed non-restorable, posing a risk to adjacent teeth or overall oral health.
- Tooth Replacement Options: Following extraction, it’s crucial to consider tooth replacement to maintain oral function and aesthetics.
- Dental Implants in Dallas: For many patients, dental implants are the preferred solution for missing teeth. A dental implant consists of a titanium post surgically placed into the jawbone, acting as an artificial tooth root, which then supports a custom-made crown. They offer excellent stability, longevity, and a natural feel. Learn more about dental implants after tooth extraction in Dallas.
- Dental Bridges: A dental bridge uses adjacent healthy teeth as anchors to support an artificial tooth (pontic) that fills the gap.
- Partial Dentures: Removable partial dentures are another option, particularly if multiple teeth are missing or if implants are not suitable.
When considering tooth replacement options in Dallas, it’s important to have a detailed consultation with a local dental professional to discuss your individual needs, costs, and the most suitable long-term solution for your oral health.
Preventing Tooth Resorption: What You Can Do
While some cases of tooth resorption are unpredictable, there are proactive steps individuals can take to minimize their risk, particularly for certain types. Prevention often involves a combination of good oral hygiene, careful dental care, and awareness of risk factors.
The emphasis on long-term oral health, a core value for dental care in Dallas, means understanding preventive measures is just as important as knowing treatment options. Regular communication with your dental team is crucial for managing potential risks effectively.
Prevention Strategies
- Maintain Excellent Oral Hygiene: Brushing twice daily and flossing once a day helps prevent cavities and gum disease, which can contribute to chronic inflammation and increase the risk of resorption.
- Regular Dental Check-ups and X-rays: Routine visits to your dentist in Dallas are vital for early detection. Your dentist can monitor for subtle changes that might indicate resorption, often before symptoms appear. Regular X-rays allow for the visualization of internal tooth structures.
- Protective Measures Against Trauma: If you participate in sports or activities with a risk of facial injury, always wear a custom-fitted mouthguard. This can significantly reduce the risk of dental trauma, a major cause of resorption.
- Careful Orthodontic Treatment: If undergoing orthodontic treatment, ensure you are under the care of an experienced orthodontist who monitors root health. While some minor root shortening is normal, significant external apical resorption should be addressed.
- Prompt Treatment of Dental Issues: Do not delay treatment for cavities, gum disease, or tooth infections. Addressing these issues quickly can prevent chronic inflammation that might lead to resorption.
- Avoid Internal Bleaching (if at risk): Discuss with your dentist the risks and benefits of internal tooth bleaching, especially if you have a history of trauma or previous root canal therapy, as it can be a trigger for external cervical resorption.
- Regular Self-Checks: Occasionally inspect your teeth for any unusual pink spots, swelling, or sensitivity. While not a substitute for professional examination, being aware of changes can prompt an earlier visit to the dentist.
By taking these preventive steps and maintaining open communication with your dental provider, you can significantly contribute to your long-term oral health and reduce the likelihood of developing severe tooth resorption.
When Resorption Leads to Tooth Loss: Dental Implants in Dallas
When tooth resorption progresses to a point where a tooth cannot be saved, resulting in tooth loss, finding a reliable and long-lasting replacement solution becomes a priority for maintaining oral health and quality of life. For many in Dallas, dental implants offer the most effective and durable option for missing teeth.
Choosing to replace a lost tooth is a significant decision, and understanding all available tooth replacement options, especially dental implants, is key. Our commitment to patient-first, non-promotional oral health education aims to help you make an informed choice.
Why Consider Dental Implants in Dallas?
- Superior Stability and Function: Unlike dentures or bridges, dental implants are surgically anchored into the jawbone. This provides a stable foundation that mimics a natural tooth root, allowing you to chew and speak with confidence and comfort.
- Preservation of Jawbone: When a tooth is lost, the jawbone in that area can begin to resorb and shrink over time. Dental implants stimulate the bone, preventing this loss and helping to maintain facial structure.
- Long-Term Solution: With proper care, dental implants can last a lifetime, making them a highly cost-effective and long-term oral health investment compared to other tooth replacement options that may require more frequent replacement or repair.
- Natural Appearance and Feel: Implants are topped with custom-made crowns that are designed to match your existing teeth in color, shape, and size, blending seamlessly with your smile. You’ll likely forget which tooth is an implant.
- No Impact on Adjacent Teeth: Unlike traditional dental bridges, which require altering neighboring healthy teeth for support, dental implants stand alone. This preserves the integrity of your natural teeth.
- Improved Oral Health: By filling gaps and preventing bone loss, dental implants contribute to better overall oral health, making it easier to maintain good hygiene.
If you are facing tooth loss due to severe tooth resorption, a consultation with a dentist specializing in dental implants in Dallas is recommended. They can assess your specific situation, discuss the dental implant procedure, and provide a clear understanding of the implant cost in Dallas, ensuring you make the best decision for your unique needs. We also have information on single tooth implant cost in Dallas 2026 for those considering individual tooth replacements.
Frequently Asked Questions About Tooth Resorption
Q1: Can tooth resorption be reversed?
No, once tooth structure is resorbed, it cannot be regenerated or reversed. The goal of treatment is to halt the process and prevent further damage.
Q2: Is tooth resorption painful?
Not always. Many cases are asymptomatic in early stages. Pain typically occurs when the resorption is extensive, reaches the pulp, or causes inflammation.
Q3: How common is tooth resorption?
External cervical resorption is relatively common, estimated to affect 1-10% of the population, with varying degrees of severity. Internal resorption is less common.
Q4: Can children get tooth resorption?
Yes, children can experience resorption, often following dental trauma or issues related to erupting permanent teeth affecting primary (baby) teeth.
Q5: Will a root canal always save a tooth with internal resorption?
Root canal therapy is highly effective for internal resorption if performed before the tooth structure is too severely compromised or perforated.
Q6: Does orthodontic treatment always cause tooth resorption?
No, while mild external apical root resorption can occur in some orthodontic patients, severe resorption is rare and typically manageable under careful supervision.
Q7: If a tooth is extracted due to resorption, what are the best replacement options?
Dental implants are often considered the gold standard for tooth replacement due to their stability and longevity. Other options include dental bridges or partial dentures.
Q8: What is the difference between tooth resorption and tooth decay?
Tooth resorption is the body’s own cells breaking down tooth structure, often triggered by trauma or inflammation. Tooth decay is caused by bacteria producing acids that dissolve tooth enamel and dentin.
Q9: Can tooth resorption recur after treatment?
Yes, if the underlying cause is not fully addressed or if there are genetic predispositions, resorption can recur. Regular follow-up with your dentist is important.
Conclusion
Tooth resorption is a nuanced dental condition that, while often asymptomatic in its early stages, can lead to significant tooth damage and even loss if left undiagnosed and untreated. From external cervical resorption often linked to trauma or orthodontics, to internal resorption stemming from pulp inflammation, understanding its various forms and causes is vital for effective management. Early detection through regular dental check-ups and advanced imaging like CBCT is paramount for successful intervention.
When treatment involves saving the tooth, procedures like root canal therapy or surgical repair are often employed. However, in cases where the tooth is beyond repair, tooth replacement options become a crucial part of restoring oral health. For residents of Dallas, dental implants offer a robust, long-lasting, and natural-feeling solution for missing teeth, providing both functional and aesthetic benefits. We encourage informed decision-making and a consultation with a qualified dentist in Dallas to explore your options and ensure long-term oral health. Prioritizing patient safety and comprehensive oral health education ensures that you are equipped to make the best choices for your smile.
Related Reading:
- The Psychological Impact of Tooth Loss and How Dental Implants in Dallas Can Restore Confidence
- Dental Implants After Tooth Extraction Dallas: Timing, Costs
- Navigating the Dental Implant Consultation: Key Questions for Dallas Patients
- Why Dallas Dental Implant Prices Vary So Widely: Provider Expertise, Materials, Technology Explained
- Minimally Invasive Dental Implants Dallas: Lower Pain, Faster Recovery 2026 Costs

Leave a Reply
Share your thoughts or ask a question about dental implants. Your email address will not be published.