Experiencing pain when chewing after receiving an implant crown can be concerning, especially after investing in a long-term tooth replacement option like dental implants in Dallas. While a slight degree of discomfort during the initial healing phase is normal, persistent or increasing pain, particularly when biting or chewing, warrants immediate attention. This article from Dental Implant Education – Dallas TX will help you understand the common reasons behind pain when chewing after an implant crown, what steps you should take, and how to work with your dental professional to resolve the issue for long-term oral health.
Key Takeaways
- Pain when chewing after an implant crown is not always normal, especially if it’s persistent or sharp.
- Common causes include bite misalignment, loose crowns, food impaction, gum irritation, and, in rare cases, implant complications.
- Unlike natural teeth, dental implants lack a periodontal ligament, making them less forgiving to uneven pressure.
- Immediate consultation with your dentist in Dallas is crucial for accurate diagnosis and timely treatment.
- Treatment options range from simple crown adjustments to addressing underlying implant issues like peri-implantitis.
- Early detection and intervention are key to preventing minor issues from escalating into more significant complications.
- Proper oral hygiene and regular follow-up appointments are essential for the longevity and comfort of your dental implant.
Quick Answer
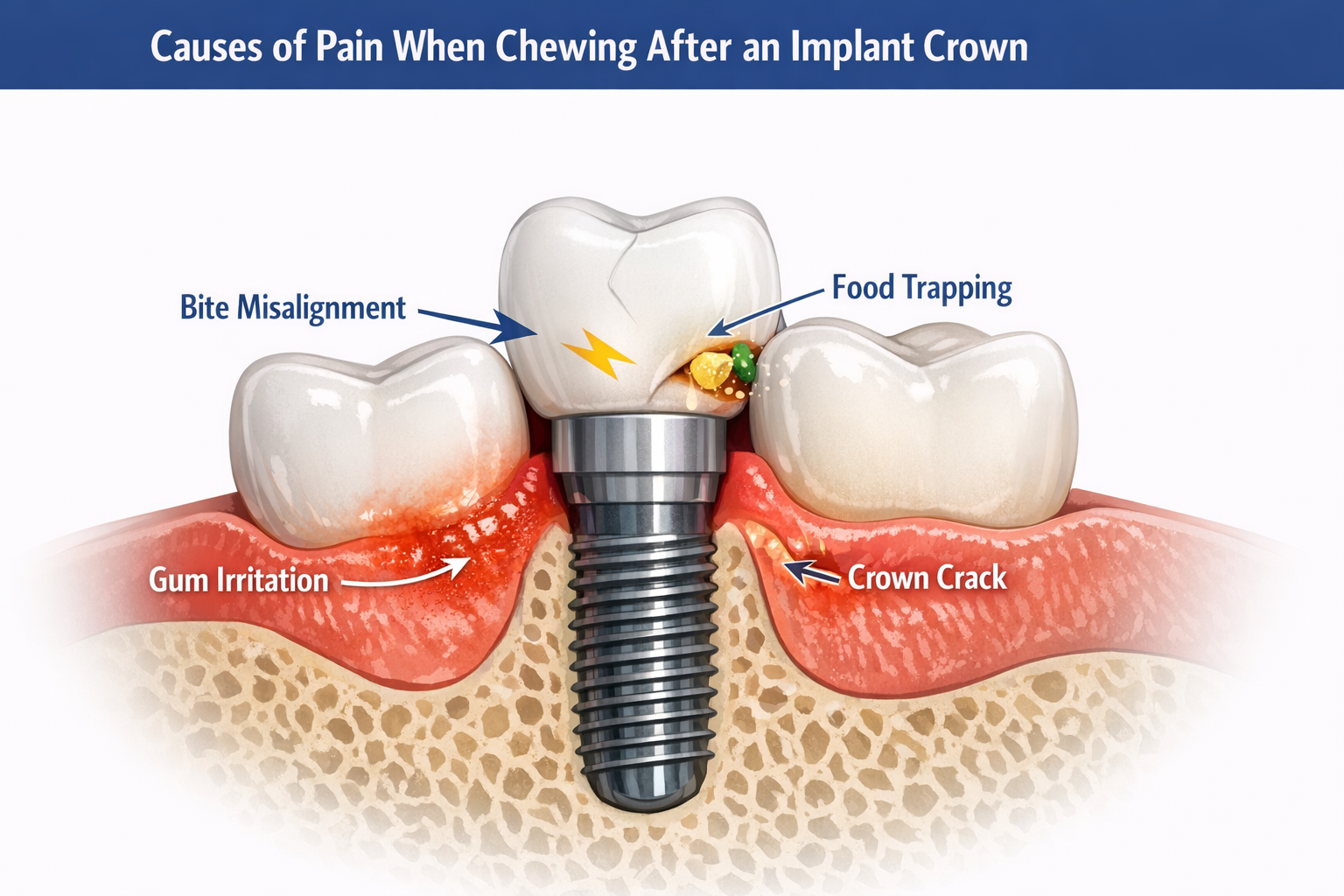
Pain when chewing after an implant crown typically indicates an underlying issue that requires professional evaluation, as discomfort should subside significantly after the initial healing period. Common culprits include problems with the crown’s fit, alignment, or the surrounding gum tissue, which can often be resolved with simple adjustments or treatment by your dentist in Dallas.
What Causes Pain When Chewing After an Implant Crown?
Experiencing pain when chewing after an implant crown can stem from several factors, ranging from minor issues with the crown itself to more significant concerns related to the dental implant or surrounding tissues. Unlike natural teeth, which have a periodontal ligament that allows for slight movement and cushioning, dental implants are directly fused with the jawbone, meaning they don’t absorb chewing forces in the same way [2]. This difference makes them particularly sensitive to uneven pressure or misalignments. Understanding these potential causes is the first step toward effective resolution.
Bite Misalignment
One of the most frequent causes of pain when chewing after an implant crown is an improper bite. Even a slight misalignment can create excessive pressure points on the implant crown during chewing, leading to discomfort [2][5]. Since implants cannot shift or adjust like natural teeth, any uneven contact can cause direct stress on the implant and the surrounding bone. Your dentist can assess your bite using articulating paper to identify and correct these high spots. This adjustment is often a quick and effective solution.
Loose Implant Crown
A loose implant crown can cause pain and instability during chewing. When the crown is not firmly attached to the implant abutment, it can wobble, creating abnormal pressure and irritation [1]. Symptoms of a loose crown might include clicking or popping sounds when you chew, a sensation of movement, or food getting trapped underneath [1]. A loose crown needs to be re-tightened or recemented by a dental professional to ensure proper function and prevent further damage to the implant or surrounding structures.
Food Impaction and Gum Irritation
If the implant crown does not fit perfectly against adjacent teeth or the gum line, small gaps can form. These gaps can allow food particles to become trapped, leading to gum irritation, inflammation, and potential infection around the implant site [2]. This irritation can manifest as pain when chewing, especially if the pressure pushes food deeper into the irritated areas. Maintaining excellent oral hygiene, including regular brushing and flossing, is crucial, but a persistent issue often indicates a need for the crown to be re-contoured or replaced to eliminate the gaps.
Peri-Implantitis
Peri-implantitis is a serious inflammatory condition affecting the tissues surrounding a dental implant, similar to gum disease around natural teeth. It’s an infection that can lead to bone loss around the implant, causing pain, swelling, and even implant failure if left untreated [8][9]. While less common as an immediate cause of pain after crown placement, it can develop over time and become noticeable when chewing as the implant loses stability. Signs include gum swelling, bleeding, pus, or a foul taste, along with pain or discomfort [6]. If your dentist suspects peri-implantitis, they will recommend specific treatments to manage the infection and preserve the implant.
Nerve Compression or Damage
Though rare, persistent pain when chewing could indicate nerve compression or damage that occurred during the initial implant surgery [5]. Symptoms might include numbness, tingling, or sharp, shooting pain. This is a more complex issue requiring specialized diagnostic imaging and possibly consultation with an oral surgeon. If you experience these symptoms, especially if they are severe or accompanied by numbness, seek immediate professional evaluation.
Healing Abutment Issues
Sometimes, the pain might originate from the healing abutment itself, even if the final crown has been placed. If the healing abutment was recently removed or if it was not fully settled, it could cause temporary discomfort. However, persistent pain is not typical.
Other Dental Issues
Sometimes the pain you’re experiencing might not be directly related to the implant or crown but rather to an adjacent tooth, gum issue, or even a sinus problem [5]. Referred pain from other areas of your mouth or face can sometimes mimic pain coming from the implant site. A thorough dental examination will help differentiate the source of the discomfort.
“While mild discomfort is common after dental procedures, persistent or sharp pain when chewing after an implant crown should always be evaluated by a dental professional. Addressing the cause early can prevent more serious complications and ensure the long-term success of your implant.”
When Should You Be Concerned About Pain When Chewing After an Implant Crown?
You should be concerned about pain when chewing after an implant crown if it is persistent, sharp, increasing in intensity, or accompanied by other worrying symptoms. While some mild, temporary discomfort can occur as you adjust to a new crown, a healthy dental implant and its crown should not cause significant or long-lasting pain during normal function [3][5].
Normal vs. Concerning Discomfort
- Normal Discomfort: It is typical to experience mild soreness or sensitivity for a few days after the final crown is placed, especially if minor adjustments were made or if your gums were manipulated. This usually subsides quickly and can often be managed with over-the-counter pain relievers [3].
- Concerning Symptoms: You should promptly contact your dentist if you experience any of the following:
- Persistent or Sharp Pain: Pain that doesn’t improve after a few days, or that is sharp and intense, particularly when you bite down [2].
- Pain Triggered by Cold: Sensitivity or sharp pain when exposed to cold temperatures or cold water, which could indicate issues with the crown or underlying tooth structure [2].
- Gum Swelling, Bleeding, or Redness: Inflammation, bleeding gums, or visible redness around the implant crown can signal infection or irritation [2][6].
- Pus or Foul Taste: The presence of pus or a persistent bad taste in your mouth around the implant site is a strong indicator of infection.
- Looseness or Movement: If you feel any movement in the crown or the implant itself, or hear clicking/popping sounds during chewing, this needs immediate attention [1].
- Difficulty Chewing: If the pain makes it genuinely difficult or impossible to chew comfortably, it’s a clear sign that something is amiss.
- Fever or General Malaise: These systemic symptoms, along with localized pain, suggest a more significant infection.
It is important to remember that dental implants boast a high success rate, with over 90% being successful overall and a 95-98% long-term survival rate [2][3]. However, vigilance for concerning symptoms is key to maintaining this success. Only about 5% of patients report long-lasting pain after implant procedures, and over 95% experience pain reduction within three weeks [3]. If you find yourself in the minority experiencing ongoing issues, seeking professional help quickly is essential. For guidance on managing discomfort, you might find our Dental Implant Pain Relief Guide: Manage Discomfort in 2026 helpful.
What Should You Do if You Have Pain When Chewing After Your Implant Crown?
If you are experiencing pain when chewing after your implant crown, the most important step is to contact your dental professional in Dallas immediately. Do not attempt to diagnose or treat the problem yourself, as delays could potentially worsen the condition.
Step-by-Step Actions:
- Contact Your Dentist Promptly: Schedule an appointment as soon as possible. Clearly describe your symptoms, including when the pain started, its intensity, what triggers it (e.g., chewing specific foods, cold), and any other accompanying symptoms like swelling or clicking [2].
- Avoid Chewing on the Affected Side: Until you see your dentist, try to avoid putting pressure on the implant crown when eating. Stick to soft foods that require minimal chewing.
- Maintain Excellent Oral Hygiene: Continue to brush and gently floss around the implant site, even if it’s sensitive. Good hygiene can help prevent further irritation or infection, provided there isn’t a structural issue [2]. You might find information on using a Sulcus Brush for Implants: 2026 Guide to Optimal Care helpful.
- Over-the-Counter Pain Relief (as directed): For temporary relief, you can use over-the-counter pain relievers like ibuprofen or acetaminophen, as long as you have no medical contraindications. However, these are only for symptom management and do not address the underlying cause [4].
- Do Not Ignore It: Dental implant pain, especially when chewing, is typically not normal beyond the initial healing period. Ignoring it could lead to more complex and costly problems down the line, potentially affecting the long-term success of your dental implant [5]. For urgent situations, our guide on Emergency Dental Implant Care Dallas 2026: Urgent Guide can provide additional insights.
During Your Dental Visit:
Your dentist will conduct a thorough examination, which may include:
- Visual Inspection: Checking the crown, gums, and surrounding teeth for any visible issues.
- Bite Analysis: Using articulating paper to identify any high spots or uneven pressure points on the crown [2].
- X-rays: To assess the implant’s position, the bone level around it, and rule out any deeper issues like bone loss or infection [5].
- Palpation: Gently feeling the tissues around the implant to check for tenderness or swelling.
- Periotest or similar device: To check the stability of the implant if peri-implantitis is suspected.
Based on their findings, your dentist will recommend the appropriate treatment. This could range from a simple bite adjustment to re-tightening a loose crown, treating an infection, or, in rare cases, needing a Dental Implant Crown Replacement Cost Dallas 2026 Guide if the crown itself is faulty. Early intervention is key to preserving your dental implant and ensuring your comfort.
How is Pain When Chewing After an Implant Crown Diagnosed?
Diagnosing the precise cause of pain when chewing after an implant crown involves a comprehensive approach by your dentist, combining clinical examination with diagnostic imaging. An accurate diagnosis is crucial for effective treatment and to ensure the long-term success of your dental implants in Dallas.
Clinical Examination
Your dentist will begin by listening to your symptoms, asking detailed questions about the nature, location, and triggers of your pain. This is followed by a thorough intraoral examination, which typically includes:
- Visual Inspection: The dentist will carefully examine the implant crown, surrounding gums, and adjacent teeth for any signs of inflammation, redness, swelling, or trauma [2]. They will also check for visible cracks or chips in the crown itself.
- Bite Analysis (Occlusal Evaluation): This is a critical step. Your dentist will use articulating paper (a thin, colored paper) to check your bite. You will be asked to bite down on the paper, which leaves marks on the crown indicating areas of heavy contact or uneven pressure [2]. High spots or improper contacts are a common cause of chewing pain.
- Palpation: Gentle pressure will be applied to the gums around the implant to check for tenderness, swelling, or the presence of pus.
- Probing: A periodontal probe may be used to measure the gum pocket depth around the implant, which can indicate gum disease or peri-implantitis [8].
Diagnostic Imaging
X-rays are an indispensable tool for diagnosing issues that are not visible during a clinical examination.
- Periapical X-rays: These detailed X-rays provide a clear view of the bone level around the implant, the integrity of the implant-bone interface, and can reveal signs of infection, bone loss, or nerve involvement [5].
- Panoramic X-rays or CBCT Scans: In more complex cases, or if nerve damage is suspected, a panoramic X-ray or a Cone Beam Computed Tomography (CBCT) scan may be taken. A CBCT scan provides a detailed 3D image of the jawbone, nerves, and surrounding structures, offering invaluable diagnostic information.
Differentiating Causes
Through this systematic diagnostic process, your dentist can differentiate between various potential causes:
- Bite Misalignment: Identified by heavy contact marks on articulating paper and often confirmed by patient reports of pain only when biting down [2].
- Loose Crown/Abutment: Can sometimes be felt during a physical examination, and confirmed by checking the screw or cementation. Clicking or popping sounds are also key indicators [1].
- Gum Irritation/Infection (Peri-implantitis): Diagnosed by redness, swelling, bleeding, deep pocket depths, and potentially bone loss visible on X-rays [2][6][8].
- Implant Overload: Often a consequence of untreated bite misalignment, leading to stress on the implant and surrounding bone, visible as bone changes on X-rays [5].
- Nerve Damage: Suspected with symptoms like numbness, tingling, or sharp, shooting pain, often requiring advanced imaging to confirm [5].
A thorough diagnosis ensures that the prescribed treatment targets the actual cause of your pain, providing effective and lasting relief. Regular Dallas Dental Implant Follow-Up: Ensuring Lasting Smile Suc visits are critical for early detection of such issues.
Treatment Options for Pain When Chewing After an Implant Crown
Treatment for pain when chewing after an implant crown depends entirely on the underlying cause identified during diagnosis. Your dental professional will tailor a treatment plan to address the specific issue, aiming to restore comfort and ensure the long-term success of your dental implant in Dallas.
1. Bite Adjustment (Occlusal Adjustment)
If bite misalignment is the cause, your dentist will gently reshape the chewing surface of the implant crown to eliminate high spots and achieve a balanced bite [2][5]. This is often a quick and non-invasive procedure.
- Procedure: Using fine dental burs, the dentist carefully grinds away small amounts of porcelain or composite material from the crown where contact is too heavy.
- Outcome: This redistributes chewing forces evenly across the implant and surrounding teeth, relieving pressure and discomfort.
- When to choose: This is the primary treatment for bite-related pain when no other pathology is present.
2. Tightening or Recementing a Loose Crown/Abutment
A loose crown can often be resolved by tightening the screw that connects the crown to the implant (if it’s a screw-retained crown) or by recementing it (if it’s cement-retained) [1].
- Procedure: The dentist will access the screw, tighten it to the appropriate torque, or clean and re-cement the crown onto the abutment.
- Outcome: Eliminates movement, reduces irritation, and restores stability for comfortable chewing.
- Common mistake: Patients sometimes try to ignore a loose crown, which can lead to further damage to the implant or even aspiration of the crown. Always seek professional help immediately [1].
3. Addressing Food Impaction and Gum Irritation
If food impaction is the problem due to a poorly fitting crown, solutions involve improving the crown’s contour or replacement.
- Procedure: Your dentist may reshape the crown slightly to eliminate gaps, or in some cases, a new crown might be necessary to achieve a precise fit against adjacent teeth and the gum line [2].
- Outcome: Prevents food trapping, reduces gum inflammation, and restores a healthy gum environment around the implant. For information on replacement costs, refer to our guide on Dental Implant Crown Replacement Cost Dallas | 2026 Guide.
4. Treatment for Peri-Implantitis
If peri-implantitis (implant infection) is diagnosed, treatment focuses on eliminating the infection and preserving the implant.
- Non-Surgical Treatments: In early stages, this may involve professional cleaning around the implant, antimicrobial rinses, or local antibiotic application [8].
- Surgical Treatments: More advanced cases may require surgical intervention to debride the infected tissues, disinfect the implant surface, and possibly perform bone grafting to regenerate lost bone [8].
- Outcome: Controls infection, prevents further bone loss, and aims to stabilize the implant. Early diagnosis is critical; see our Peri-Implantitis Prevention Dallas: Early Signs, Treatment C for more details.
5. Addressing Nerve Compression or Damage
In the rare event of nerve compression or damage, treatment can be more complex.
- Procedure: This may involve medication, nerve block injections, or, in severe cases, surgical intervention to relieve pressure on the nerve [5].
- Outcome: Aims to reduce pain and restore nerve function, though recovery can be lengthy.
- Who it’s for: This is an edge case that requires a specialized approach, often involving an oral surgeon or neurologist.
6. Managing Bruxism (Teeth Grinding)
If bruxism is contributing to excessive chewing forces on the implant, a night guard may be recommended.
- Procedure: A custom-fitted Dental Implant Night Guard: Essential Protection in 2026 is fabricated to wear at night, protecting the implant crown and distributing forces more evenly.
- Outcome: Reduces stress on the implant, prevents wear on the crown, and alleviates associated jaw pain.
Ultimately, preventing and treating pain when chewing after an implant crown relies on proactive patient care and timely professional intervention. Always follow your dentist’s post-operative instructions and attend regular check-ups to ensure the longevity and comfort of your dental implant.
Preventing Pain When Chewing After an Implant Crown
Preventing pain when chewing after an implant crown involves a combination of careful planning, diligent oral hygiene, and regular professional oversight. While some issues are unpredictable, many can be avoided or caught early through proactive measures.
1. Choose an Experienced Dental Professional
The foundation of a successful and pain-free dental implant journey begins with selecting a highly skilled and experienced dental implant specialist in Dallas. An experienced dentist or oral surgeon uses advanced techniques, precise planning (often with 3D guided implant surgery), and quality materials to minimize complications [7].
- Decision Rule: Choose a dentist with extensive experience in dental implants and prosthodontics who emphasizes patient safety and long-term oral health. Don’t hesitate to ask about their experience with dental implant procedures and post-operative care.
2. Follow Post-Operative Instructions Meticulously
After your implant surgery and again after crown placement, your dentist will provide specific instructions. Adhering to these instructions is crucial for proper healing and to prevent undue stress on the implant.
- Key actions: This includes guidance on diet, oral hygiene, activity restrictions, and medication usage. Avoid hard or sticky foods, especially during the initial healing phase and immediately after crown placement.
- Common mistake: Rushing back to a normal diet too quickly or neglecting prescribed medications can hinder healing and introduce complications.
3. Maintain Excellent Oral Hygiene
Just like natural teeth, dental implants require meticulous oral care to prevent issues like peri-implantitis and gum inflammation.
- Daily routine: Brush twice daily with a soft-bristled toothbrush, floss around the implant, and use any prescribed mouth rinses. Special brushes, like a sulcus brush, can be beneficial for cleaning around implants [2].
- Why it works: Good hygiene removes plaque and food debris, preventing bacterial buildup that can lead to gum irritation or infection around the implant [6].
4. Regular Dental Check-ups and Cleanings
Consistent follow-up appointments with your dentist are vital for monitoring the health of your dental implant and crown.
- Frequency: Typically, bi-annual check-ups and professional cleanings are recommended, but your dentist may suggest more frequent visits for implant maintenance [6].
- What happens: During these visits, your dentist will examine the implant and crown, check your bite, and take X-rays if needed to assess bone levels and overall implant health. Early signs of bite issues, loose components, or gum inflammation can be detected and addressed before they become painful problems. For information on essential follow-ups, see our guide on Dallas Dental Implant Follow-Up: Ensuring Lasting Smile Suc.
5. Address Bruxism (Teeth Grinding)
If you grind or clench your teeth, especially at night, communicate this to your dentist. Bruxism can place excessive forces on dental implants, leading to complications.
- Solution: Your dentist may recommend a custom-fitted night guard to protect your implant and other teeth from the damaging effects of grinding [5]. A Dental Implant Night Guard: Essential Protection in 2026 can significantly reduce stress.
By taking these preventative steps, you significantly increase the chances of a smooth, comfortable experience with your dental implant crown and ensure its long-term success as a durable tooth replacement option.
Frequently Asked Questions About Pain When Chewing After Implant Crown
Is it normal to have pain after a dental implant crown is placed?
Mild soreness or sensitivity for a few days after the crown is placed is common as your tissues adjust, but persistent, sharp, or increasing pain when chewing is not considered normal and should be evaluated by a dentist [2][4].
Can a dental implant crown be adjusted if it’s causing pain?
Yes, if the pain is due to bite misalignment, the crown can often be adjusted by your dentist to remove high spots and create a balanced bite [2].
How long does it take for a dental implant crown to feel normal?
Most patients report their dental implant crown feels normal within a few days to a week after placement. If discomfort persists beyond this, it warrants a dental visit [3].
What are the signs of a loose dental implant crown?
Signs of a loose crown include a feeling of movement, clicking or popping sounds when chewing, or food getting trapped underneath [1].
Can gum inflammation around an implant crown cause chewing pain?
Yes, gum inflammation (mucositis) or infection (peri-implantitis) around an implant can cause pain, swelling, and discomfort, particularly when chewing [2][6].
Is it possible for an implant itself to hurt, even with a crown on it?
While the implant itself shouldn’t hurt once integrated into the bone, issues like peri-implantitis (infection around the implant) or, rarely, nerve compression can cause pain that feels like it’s coming from the implant [5][8].
Should I avoid certain foods if my implant crown hurts when chewing?
Yes, if you’re experiencing pain, it’s advisable to avoid hard, chewy, or sticky foods that put excessive pressure on the implant crown until the cause of the pain is diagnosed and treated. Stick to softer foods [2].
What happens if I ignore pain when chewing after my implant crown?
Ignoring pain can lead to more serious complications, such as exacerbating gum infection, bone loss around the implant, damage to the implant components, or even implant failure [5][6].
Does biting down hard immediately after crown placement cause issues?
Biting down hard on a newly placed crown that is not properly adjusted can create pressure points and cause discomfort or even damage to the crown or implant [2]. Your dentist will ensure your bite is correctly aligned before you leave.
Can a night guard help with pain when chewing after an implant crown?
If teeth grinding (bruxism) is contributing to the pain by placing excessive force on the implant, a custom night guard can help protect the implant and alleviate discomfort [5].
Conclusion
Experiencing pain when chewing after an implant crown can be unsettling, but understanding the potential causes and knowing when to seek professional help are crucial steps toward resolution. While dental implants are an excellent, durable solution for missing teeth, issues like bite misalignment, loose crowns, or gum irritation can arise. The good news is that most causes of pain when chewing after an implant crown are treatable, especially when addressed promptly.
At Dental Implant Education – Dallas TX, we emphasize patient-first care and comprehensive oral health education. If you are experiencing discomfort, do not hesitate to schedule a consultation with a dentist in Dallas. Early diagnosis and treatment are key to ensuring the long-term success and comfort of your dental implants. Taking proactive steps, from meticulous oral hygiene to regular dental check-ups, is vital for maintaining your implant health and enjoying your restored smile for years to come.

Leave a Reply
Share your thoughts or ask a question about dental implants. Your email address will not be published.