Dental implants offer a durable and aesthetically pleasing solution for missing teeth, providing a foundation for long-term oral health and a confident smile. However, like any medical procedure, it’s crucial for patients to understand the potential for complications, especially those that can arise years after the initial placement. This comprehensive 2026 guide will delve into late dental implant complications, offering insights into what they are, why they occur, and how they are managed, especially for our community here in Dallas, Texas.
Key Takeaways
- Late dental implant complications typically appear years after implant placement and can impact the implant’s long-term success.
- Peri-implantitis, an infection around the implant, is the most common biological complication and a primary cause of late implant failure.
- Mechanical complications, such as screw loosening or prosthetic fractures, can also occur due to factors like occlusal overload or design issues.
- Patient-specific risk factors, including poor oral hygiene, smoking, certain systemic diseases (e.g., diabetes, osteoporosis), and bruxism, significantly increase the likelihood of late complications.
- While dental implants boast a high success rate (often above 90% in the first 10 years), this rate can decline significantly after 10-20 years, highlighting the importance of lifelong care.
- Regular dental check-ups, meticulous oral hygiene, and addressing any underlying health conditions are critical for preventing and managing late complications.
- Early detection and intervention by a qualified dental professional are crucial for successfully treating late complications and preserving the implant.
- For residents in Dallas, choosing an experienced dental implant specialist and maintaining consistent follow-up care are vital for long-term implant success.
Quick Answer
Late dental implant complications refer to problems that emerge months or even years after a dental implant has been successfully placed and integrated into the jawbone, ranging from infections like peri-implantitis to mechanical failures. While dental implants are highly successful, these delayed issues necessitate careful monitoring and proactive management to ensure the longevity of your tooth replacement options.
What Are Late Dental Implant Complications?
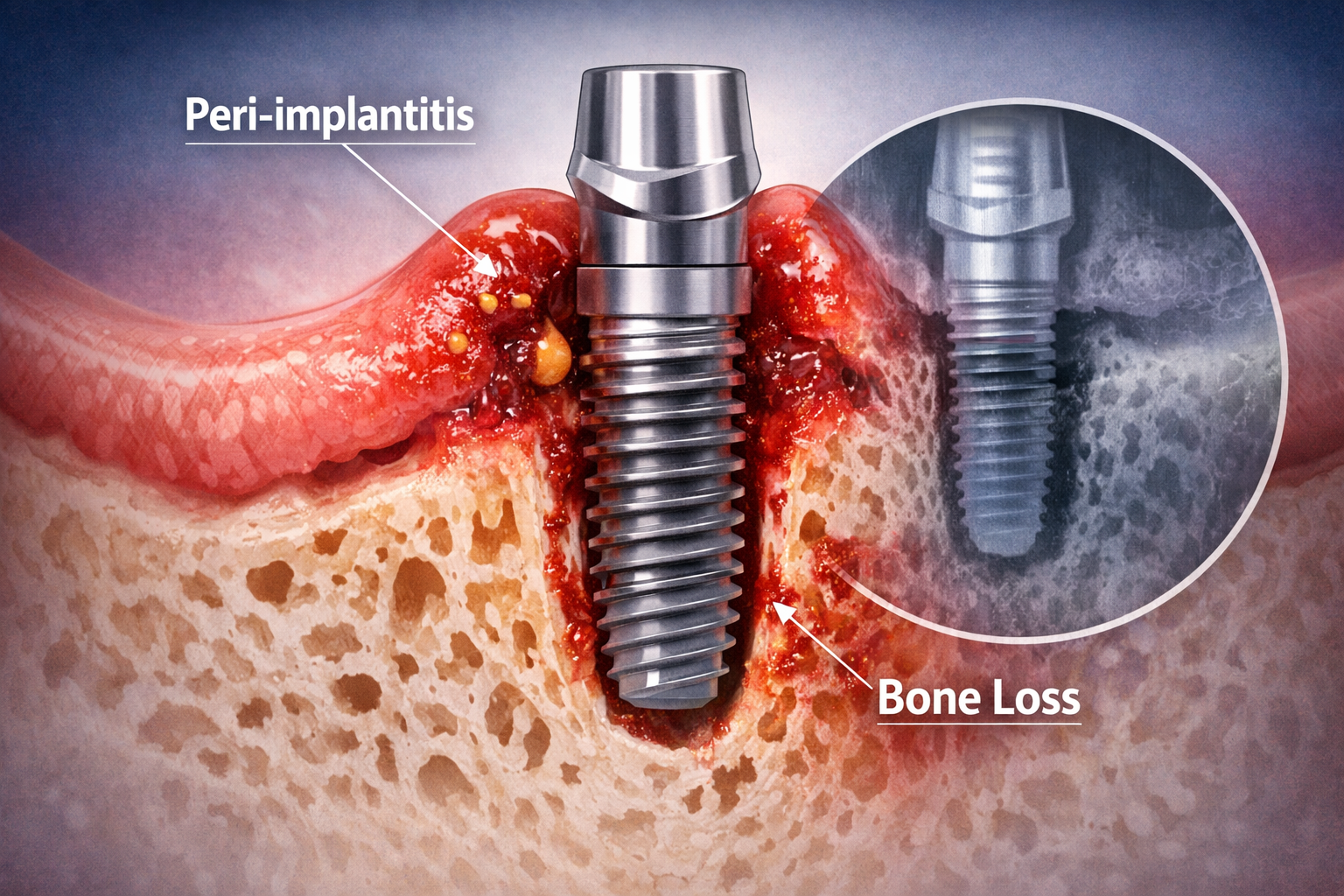
Late dental implant complications are health issues or structural failures that develop around a dental implant long after its initial placement and successful osseointegration, often years into its functional life. These complications can significantly impact the long-term oral health and stability of the implant, making continuous patient care and professional follow-ups essential.
The nature of these complications can vary, but they generally fall into two main categories: biological and mechanical. Understanding the distinction helps in diagnosis and treatment.
Biological Complications: Peri-implantitis and Other Soft Tissue Issues
Peri-implantitis is the leading biological late complication, characterized by inflammation of the gum tissue and progressive bone loss around a dental implant [4]. This condition is akin to periodontitis in natural teeth and can ultimately lead to implant mobility and loss if not addressed.
- Symptoms of Peri-implantitis: Patients may notice redness, swelling, bleeding upon probing, pus discharge, or increased pocket depths around the implant. A noticeable sign can be a sensation that the “dental implant feels weird” or loose over time [https://dentalimplantsdallastx.com/how-long-until-a-dental-implant-stops-feeling-weird-or-like-a-foreign-object/].
- Prevalence: Approximately 34% of implant patients develop peri-implantitis at some point, although not all cases result in implant loss [4]. This highlights the widespread nature of the issue.
- Causes: Poor oral hygiene is a significant risk factor, as it allows bacteria to accumulate around the implant, leading to infection [4][5]. Systemic conditions, smoking, and previous history of periodontitis can also contribute. Our guide on “Can Dental Implants Get Infected Years Later? Your 2026 Guide” offers more detailed information on infections.
- Treatment: Early intervention is key. Treatment options range from professional cleaning and antiseptic rinses to surgical procedures aimed at decontaminating the implant surface and regenerating lost bone.
Beyond peri-implantitis, other soft tissue complications can include mucositis (inflammation limited to the soft tissue around the implant without bone loss), which is often reversible, and soft tissue recession, which can expose the implant’s metallic collar.
Mechanical Complications: Component Failures and Fractures
Mechanical late dental implant complications involve the implant components themselves or the restoration (crown, bridge, denture) attached to them. These issues are often related to the forces exerted during chewing or the materials used.
- Abutment Screw Loosening/Fracture: The abutment is the connector between the implant and the prosthetic crown. Screws holding this connection can loosen or, less commonly, fracture due to sustained biting forces. Symptoms might include a “dental implant clicking noise” or a feeling of instability in the crown.
- Prosthetic Fractures: The porcelain or ceramic material of the crown, bridge, or denture can chip, crack, or fracture, especially if subjected to excessive force (e.g., from bruxism or chewing hard objects).
- Implant Fractures: While rare, the implant body itself can fracture, often due to extreme occlusal overload or fatigue over many years. This is a severe complication that usually necessitates implant removal.
- Peri-implant Bone Loss under Functional Loading: This refers to bone loss around the implant not primarily due to infection but rather from excessive mechanical stress or inadequate bone-to-implant contact [1]. This can sometimes be exacerbated by bruxism, which can be mitigated by solutions discussed in “Bruxism & Dental Implants: Prevent Damage in 2026“.
- Causes: Occlusal overload (excessive biting forces), poor implant positioning, inadequate bone support at the time of placement, or material fatigue can contribute to mechanical failures [1]. The success rates of dental implants are generally high, with one meta-analysis showing 97% success at 10 years, but a significant decline in survival can occur between 10 and 20 years, indicating that mechanical complications become more prevalent over time [4][2].
When experiencing any unusual symptoms around your dental implant, such as pain, swelling, or instability, it’s critical to consult with a dentist promptly. Ignoring these signs can lead to more complex and costly treatments down the line. For emergencies, patients in Dallas should seek “Emergency Dental Implant Care Dallas 2026“.
What Factors Increase the Risk of Late Dental Implant Complications?
Several factors can significantly increase a patient’s susceptibility to late dental implant complications, ranging from individual health conditions and lifestyle choices to the characteristics of the implant placement itself. Recognizing these risk factors is crucial for prevention and for dentists to tailor long-term care plans, particularly for patients considering tooth replacement options in Dallas.
Patient-Specific Risk Factors
An individual’s general health, habits, and oral hygiene play a profound role in the long-term success of dental implants.
- Poor Oral Hygiene and Lack of Compliance: This is perhaps the most significant modifiable risk factor for biological complications, especially peri-implantitis [4][5]. Insufficient brushing and flossing allow plaque and bacteria to accumulate around the implant, initiating inflammation and infection. Patients with poor compliance show twice the risk of implant loss compared to those with regular compliance [2]. Meticulous home care, often guided by specific instructions like those for using a “Sulcus Brush for Implants“, is paramount.
- Smoking: Tobacco use significantly compromises healing and immune response, dramatically increasing the risk of peri-implantitis and overall implant failure [5]. Smokers experience higher rates of late complications compared to non-smokers.
- Systemic Diseases: Certain medical conditions can impair the body’s ability to heal and fight infection, making late complications more likely.
- Diabetes (uncontrolled): Patients with uncontrolled Type 2 diabetes face higher risks due to impaired wound healing and increased susceptibility to infections [3]. However, well-controlled diabetics can have successful implant outcomes, emphasizing the need for diligent management of their condition. Our guide on “Diabetic Dental Implant Recovery” provides more information.
- Osteoporosis: This condition, especially when managed with certain medications (bisphosphonates), can affect bone quality and density, potentially impacting the implant’s stability and bone integration. Male sex and osteoporosis are considered independent critical risk factors for implant failure [1].
- Cardiovascular Disease: While not as directly linked as diabetes or osteoporosis, overall systemic health can influence healing and resilience.
- Bruxism (Teeth Grinding/Clenching): Chronic grinding or clenching places excessive force on dental implants, which lack the natural shock-absorbing ligament of natural teeth. This can lead to mechanical complications like screw loosening, prosthetic fractures, and even peri-implant bone loss under functional loading [1]. A nightguard is often recommended for patients with bruxism to protect their implants.
- Previous History of Periodontitis: Patients who lost natural teeth due to periodontal disease are at a higher risk of developing peri-implantitis around their implants, as the bacterial flora and inflammatory predisposition may persist.
- Age and Sex: While implants are successful across age groups, advanced age can sometimes correlate with other health issues. Some literature suggests male sex as an independent critical risk factor for implant failure, though data can be conflicting [1]. Senior patients should particularly pay attention to “Senior Dental Implant Healing Time” considerations.
Treatment-Related and Implant-Specific Factors
Beyond the patient’s health, certain aspects of the dental implant procedure itself can contribute to the risk of late complications.
- Implant Position and Surgical Technique: Poor implant angulation or placement too close to adjacent teeth or vital anatomical structures can lead to difficulties in cleaning, compromised esthetics, and increased mechanical stress. The precision offered by 3D guided implant surgery can mitigate some of these risks, as highlighted in “Dallas TX Dentists Using 3D Guided Implant Surgery 2026“.
- Inadequate Bone Volume or Quality: Sufficient healthy bone is crucial for implant stability and long-term success. If bone grafting was necessary (see “Bone Graft Costs for Dental Implants in Dallas“) but the quantity or quality remained suboptimal, the risk of late complications increases. Maxillary implants, for example, often show lower survival rates due to poorer bone quality compared to mandibular implants [1][2].
- Immediate vs. Delayed Implant Placement: Some studies suggest that delayed implants (placed 3-4 months post-extraction) may demonstrate better long-term survival rates compared to immediate implants, especially in high-risk populations, though research varies [1].
- Prosthetic Design and Material: The design of the crown or bridge, particularly how it distributes biting forces and allows for hygiene access, is critical. Improper design or material choices can contribute to mechanical complications or make cleaning difficult, leading to peri-implantitis.
- Lack of Regular Follow-up Care: Lifelong follow-up appointments with your dental professional are essential for early detection and management of any potential issues. Regular check-ups allow for professional cleaning, evaluation of the implant and surrounding tissues, and identification of problems before they escalate. Our “Dental Implant Specialist Follow Up Dallas 2026” guide emphasizes this importance.
Understanding these multifaceted risk factors empowers patients to make informed decisions and maintain proactive care. A thorough consultation with a dentist in Dallas can help assess individual risks and establish a personalized long-term maintenance plan.
How Are Late Dental Implant Complications Diagnosed?
Diagnosing late dental implant complications relies on a combination of regular dental examinations, patient-reported symptoms, and advanced imaging techniques. Early detection is paramount to successful management and to preserve the longevity of your dental implant.
Clinical Examination and Patient Symptoms
The initial step in diagnosing any late complication involves a comprehensive clinical examination by a qualified dental professional. This includes:
- Visual Inspection: The dentist will carefully examine the gum tissue around the implant for signs of inflammation such as redness, swelling, or the presence of pus. They will also look for any signs of receding gums that might expose the implant.
- Probing Depths: A periodontal probe is used to measure the depth of the gum pocket around the implant. Increased probing depths can indicate inflammation or bone loss, especially if bleeding occurs upon probing.
- Mobility Check: While implants should ideally be immobile, the dentist will gently check for any signs of movement in the implant or the attached crown. Mobility is often a late sign of significant bone loss or mechanical failure.
- Patient Feedback: Your input is vital. Report any new or unusual symptoms, such as pain or discomfort around the implant, a change in how your bite feels, a “dental implant clicking noise“, bad breath from the dental implant, or a sensation that the “dental implant feels weird” [https://dentalimplantsdallastx.com/bad-breath-from-dental-implants-causes-prevention-and-solutions-in-2026/]. These subjective reports can guide the diagnostic process.
Radiographic Evaluation
X-rays are an indispensable tool for assessing the bone level around the dental implant, which is not visible during a clinical examination.
- Periapical and Panoramic X-rays: These standard dental X-rays provide two-dimensional images that help evaluate the height and density of the bone supporting the implant. Comparison with baseline X-rays taken after implant placement is crucial to detect any progressive bone loss.
- Cone Beam Computed Tomography (CBCT): For more complex cases or when two-dimensional X-rays are inconclusive, a CBCT scan provides detailed three-dimensional images. This allows the dentist to visualize the bone structure, implant position, and surrounding anatomical features with greater precision, aiding in the diagnosis of subtle bone loss, implant fractures, or other issues.
- Purpose: Radiographic evaluation helps determine the extent of bone loss associated with peri-implantitis or identify mechanical issues like abutment screw loosening or implant fractures that might not be evident clinically.
Regular check-ups and cleanings, typically recommended every six months, are the best defense against developing late dental implant complications. For residents seeking optimal long-term oral health, scheduling a consultation with a dentist in Dallas is a proactive step.
What Are the Treatment Options for Late Dental Implant Complications?
Treating late dental implant complications depends heavily on the specific nature and severity of the issue, with the primary goal being to stabilize the implant and preserve long-term oral health. Early intervention is key for effective management.
Managing Biological Complications (Peri-implantitis and Mucositis)
Treatment for infections around the implant ranges from conservative non-surgical approaches to more involved surgical procedures.
- Non-Surgical Treatments:
- Improved Oral Hygiene: Reinforcing meticulous home care, including specific instructions for interdental cleaning and using tools like a “Sulcus Brush for Implants“, is fundamental.
- Professional Debridement: The dental hygienist or dentist will thoroughly clean the implant surface, removing plaque and calculus above and below the gum line. This can involve scaling, root planing, and polishing.
- Antiseptic Rinses and Local Antibiotics: Chlorhexidine mouth rinses can help reduce bacterial load. In some cases, localized antibiotic gels or fibers may be placed into the peri-implant pocket.
- Laser Therapy: Certain dental lasers can be used to decontaminate the implant surface and promote tissue healing.
- Indication: Non-surgical methods are often effective for mucositis and early stages of peri-implantitis where bone loss is minimal.
- Surgical Treatments:
- Access Surgery with Debridement: For more advanced peri-implantitis with significant bone loss, surgical access is often necessary. This involves lifting the gum tissue to thoroughly clean and decontaminate the exposed implant surface. Various mechanical, chemical, and laser methods can be used for decontamination.
- Osseous Resective Surgery: In some cases, reshaping the bone around the implant might be performed to create a more maintainable environment and eliminate deep pockets.
- Regenerative Procedures: If there’s sufficient bone defect, bone grafting (using synthetic, animal, or patient’s own bone) and guided bone regeneration membranes can be used to try and rebuild lost bone around the implant [6].
- Implant Surface Modification: In some surgical procedures, the implant surface itself might be treated to make it more biocompatible and less prone to bacterial adhesion.
- Implant Removal (Explantation): In severe, untreatable cases where the implant is highly mobile, infected, or causes significant discomfort, removal of the dental implant may be the only viable option. This is considered a “revision dental implant surgery” and can lead to further bone grafting needs before a new implant can be considered. For more on this, consult “Unveiling the Cost of Dental Implant Removal in 2025“.
Addressing Mechanical Complications
Treatment for mechanical failures often involves repair, replacement, or, in severe cases, implant removal.
- Abutment Screw Loosening: The most common mechanical issue, this is usually resolved by simply tightening the abutment screw. If the screw is fractured, it will need to be carefully removed and replaced.
- Prosthetic Fractures (Crown, Bridge): Chipped or fractured crowns often require repair or, more commonly, replacement of the prosthetic. If a dental implant crown replacement is needed, understanding the “Dental Implant Crown Replacement Cost Dallas 2026 Guide” is helpful.
- Implant Fractures: Unfortunately, if the dental implant body itself fractures, it almost always necessitates surgical removal of the implant. After adequate healing and potentially bone grafting, a new implant might be placed. This represents a significant late dental implant complication, making “Dental Implant Repair Cost” a relevant consideration.
The treatment strategy for late dental implant complications is always individualized. Consulting with an experienced dental implant specialist in Dallas is essential to receive an accurate diagnosis and a tailored treatment plan for your specific situation. This ensures the best possible outcome for your long-term oral health.
Preventing Late Dental Implant Complications in 2026
Preventing late dental implant complications is a long-term commitment that involves both patient diligence and professional care, significantly contributing to the longevity and success of your tooth replacement options. In Dallas and beyond, proactive measures are the best defense.
Maintaining Optimal Oral Hygiene
Consistent and thorough oral hygiene is the cornerstone of preventing biological complications like peri-implantitis.
- Daily Brushing and Flossing: Brush your implants just like your natural teeth, twice a day, using a soft-bristled toothbrush. Flossing, or using interdental brushes specifically designed for implants, is crucial to clean around the implant abutment where bacteria can accumulate. Using a “Sulcus Brush for Implants” can be particularly effective.
- Antiseptic Mouthwashes: Your dentist may recommend an antimicrobial mouthwash to further reduce bacterial plaque, especially if you have a history of gum inflammation.
- Professional Cleanings: Regular professional cleanings (typically every 6 months, or more frequently if advised by your dentist) are vital. Dental hygienists have specialized tools and expertise to clean around implants without causing damage and to identify early signs of problems. This is a critical part of “Dental Implant Specialist Follow Up Dallas 2026“.
Regular Dental Check-ups and Monitoring
Even with excellent home care, routine professional oversight is indispensable for detecting and addressing potential issues early.
- Scheduled Follow-up Appointments: Adhere strictly to your dental professional’s recommended schedule for check-ups. These appointments allow the dentist to:
- Assess the health of your gum tissues and bone around the implant.
- Take radiographs to monitor bone levels.
- Check the integrity of the implant components and prosthetics.
- Address any concerns you may have, such as a “dental implant feels weird“.
- Early Detection: Many late dental implant complications, particularly peri-implantitis, are much easier and less invasive to treat when caught in their early stages. Regular monitoring helps prevent minor issues from escalating into significant problems like “Dental Implant Failure Symptoms: Early Warning Signs Guide 2025“.
Addressing Risk Factors and Lifestyle Modifications
Proactively managing systemic health and making healthy lifestyle choices can greatly reduce the risk of late complications.
- Quit Smoking: If you smoke, quitting is one of the most impactful steps you can take to improve your overall oral health and the long-term prognosis of your dental implants.
- Manage Systemic Diseases: Work closely with your medical doctor to ensure conditions like diabetes and osteoporosis are well-controlled. Communicate any changes in your health status or medications to your dentist. For example, well-controlled “Diabetic Dental Implant Recovery” is crucial.
- Wear a Nightguard for Bruxism: If you grind or clench your teeth (bruxism), a custom-fitted nightguard is essential to protect your implants and natural teeth from excessive force. Our article “Bruxism & Dental Implants: Prevent Damage in 2026” details these preventative measures.
- Avoid Chewing Hard Objects: Refrain from chewing on ice, pens, or other very hard foods, which can cause mechanical damage to your implant restoration or even the implant itself.
By embracing these preventative strategies, patients in Dallas can significantly improve the chances of their dental implants lasting a lifetime, ensuring long-term oral health and maintaining their confident smile. A consultation with an experienced dental implant professional in Dallas can provide personalized guidance for your specific situation.
What to Expect During Long-Term Follow-up for Dental Implants in Dallas

Long-term follow-up for dental implants in Dallas is crucial for their lasting success, involving a proactive partnership between the patient and their dental care team. This ongoing care aims to monitor the implant’s health, detect any emerging issues early, and address patient concerns, ensuring your long-term oral health.
Routine Check-ups and Maintenance
Just like natural teeth, dental implants require regular professional attention. Expect your follow-up appointments to be structured and thorough.
- Frequency: Typically, patients with dental implants are advised to have check-ups and professional cleanings every six months, though this can be more frequent (e.g., every 3-4 months) if you have specific risk factors for late dental implant complications, such as a history of periodontitis or poor oral hygiene.
- Comprehensive Examination: During these visits, your dentist will:
- Visually inspect the implant and surrounding soft tissues for any signs of inflammation, redness, or swelling.
- Measure probing depths around the implant to check for gum pocket formation, which can indicate early peri-implantitis.
- Assess the stability of the implant and the attached restoration, ensuring there’s no movement or loosening of components.
- Review your oral hygiene routine and provide personalized advice or demonstrations for optimal home care, including specific tools like a “Sulcus Brush for Implants“.
- Professional Cleaning: A dental hygienist specializing in implant care will gently clean around your implants, removing plaque and calculus using non-abrasive instruments that won’t scratch the implant surface. This is critical to prevent bacterial accumulation that can lead to infections.
- Radiographic Monitoring: Periodically, X-rays (usually once a year or every few years, depending on your risk profile) will be taken to monitor the bone level around your implants. Comparing these to previous X-rays allows the dentist to detect any subtle bone loss that might not be visible during a clinical exam.
Addressing Emerging Issues and Patient Concerns
Long-term follow-up is also the time to address any new sensations or problems you might be experiencing.
- Patient Communication: It’s essential to openly communicate any concerns to your dental team. Don’t hesitate to mention:
- Any discomfort or pain around the implant.
- A sensation that your “dental implant feels weird” or loose.
- Signs of bleeding gums when brushing or flossing.
- Changes in your bite or the fit of your crown/bridge.
- A “dental implant clicking noise” or other unusual sounds.
- Concerns about bad breath from dental implants.
- Early Intervention: If any early signs of late dental implant complications are detected, your dentist will discuss the findings and recommend appropriate interventions. Catching issues like mucositis or early peri-implantitis quickly often means that less invasive and more successful treatments can be employed, potentially avoiding the need for “Revision Dental Implant Surgery Dallas” later on.
- Prosthetic Assessment: The prosthetic components (crown, bridge, denture) will also be checked for wear, chips, or cracks. If a “Dental Implant Crown Replacement Cost Dallas 2026” is necessary, your dentist can discuss options.
For individuals with dental implants in Dallas, committing to these long-term follow-up appointments is a vital investment in protecting your smile and ensuring the lasting success of your dental implant procedure.
When Should You Seek Emergency Dental Implant Care in Dallas?
Seeking prompt emergency dental implant care in Dallas is critical if you experience sudden or severe symptoms that could indicate a serious late dental implant complication. While routine check-ups address most issues, certain signs warrant immediate professional attention to prevent further damage or discomfort.
Immediate Action Required
If you notice any of the following symptoms, contact your dental implant specialist or an emergency dentist in Dallas immediately:
- Severe Pain: Intense or throbbing pain around the implant that doesn’t subside with over-the-counter pain relievers. This could indicate an acute infection, nerve impingement, or a fractured implant.
- Sudden Swelling or Abscess: Rapidly developing swelling in the gums, cheek, or jaw near the implant, especially if accompanied by pus discharge or a bad taste in your mouth. This is a strong indicator of a serious infection, such as an abscess or acute peri-implantitis.
- Significant Bleeding: While some light spotting is normal after initial implant procedures, heavy or uncontrolled bleeding around an implant years later is not normal and requires immediate assessment. If you are “Spitting Blood After Dental Implant: Is It Normal?“, especially in large amounts, seek help.
- Mobile Implant or Crown: If the implant itself feels loose or wobbly, or if the crown attached to it becomes noticeably mobile or falls off. This can signify a severe loss of bone support (implant failure) or a significant mechanical failure requiring urgent attention. A mobile implant is a serious “Dental Implant Failure Symptoms” and should not be ignored.
- Trauma to the Implant Site: Any direct injury or trauma to the area around your dental implant that results in pain, swelling, or loosening of the implant.
- Numbness or Tingling: Persistent numbness or tingling in the lip, chin, or tongue, which could indicate potential nerve damage, though this is a rare late complication.
For situations like these, our guide on “Emergency Dental Implant Care Dallas 2026: Your Urgent Guide” provides comprehensive advice on how to proceed.
What to Do While Awaiting Emergency Care
While you wait for your appointment, you can take a few steps to manage symptoms:
- Rinse with Salt Water: A warm salt water rinse can help alleviate swelling and clean the area, especially if an infection is suspected.
- Apply a Cold Compress: For swelling, a cold compress applied to the outside of your cheek can help reduce inflammation.
- Over-the-Counter Pain Relievers: Medications like ibuprofen or acetaminophen can help manage pain until you see a dentist.
- Avoid the Area: Try to avoid chewing or putting pressure on the affected implant.
It is crucial not to ignore any severe or sudden symptoms related to your dental implant. Prompt professional care from a qualified Dallas dental implant specialist can make a significant difference in the outcome and help preserve your long-term oral health.
Conclusion
Understanding late dental implant complications is essential for anyone considering or living with dental implants as a tooth replacement option. While dental implants boast a high success rate, typically over 90% for the first decade, their long-term viability requires vigilance and consistent care. Issues like peri-implantitis, a common infection around the implant, and mechanical failures, such as screw loosening or prosthetic fractures, can arise years after placement, particularly between 10 and 20 years post-surgery.
The good news is that many late dental implant complications are manageable, especially with early detection and intervention. Meticulous daily oral hygiene, regular dental check-ups, and open communication with your dental implant specialist are paramount for prevention and prompt treatment. Factors like smoking, uncontrolled systemic diseases (e.g., diabetes, osteoporosis), and bruxism significantly increase risk, underscoring the importance of addressing overall health.
For residents in Dallas, maintaining your long-term oral health with dental implants means partnering with an experienced dental team committed to comprehensive follow-up care. Don’t hesitate to seek professional advice for any unusual symptoms; early action is the best defense against complex and costly treatments. By staying informed and proactive, you can ensure your dental implants continue to provide a stable, healthy, and confident smile for many years to come.
Actionable Next Steps
- Prioritize Oral Hygiene: Commit to brushing twice daily and flossing around your implants to prevent bacterial buildup. Consider using an implant-specific brush like a sulcus brush.
- Schedule Regular Check-ups: Ensure you attend all recommended follow-up appointments with your Dallas dental implant specialist for professional cleanings and monitoring.
- Address Risk Factors: If you smoke, consider quitting. If you have systemic health conditions, manage them diligently with your medical doctor and inform your dentist.
- Report Concerns Promptly: If you notice any pain, swelling, mobility, or a “weird” feeling around your implant, contact your dentist immediately for an assessment.
- Consult a Specialist: For complex concerns or to discuss your personalized long-term care plan, schedule a consultation with a qualified dental implant professional in Dallas.
References
[1] Full – https://www.frontiersin.org/journals/dental-medicine/articles/10.3389/fdmed.2025.1563641/full
[2] Pmc11416373 – https://pmc.ncbi.nlm.nih.gov/articles/PMC11416373/
[3] Managing Late Implant Complications In A Medically Complex Patient – https://dimensionsofdentalhygiene.com/managing-late-implant-complications-in-a-medically-complex-patient/
[4] Dental Implant Failure Rates What The Research Actually Says And What It Means For You – https://biteclubchi.com/dental-implant-failure-rates-what-the-research-actually-says-and-what-it-means-for-you/
[5] Dental Implant Failure Risks Statistics – https://sunflowerdentalspa.com/dental-implant-failure-risks-statistics/
[6] onlinelibrary.wiley – https://onlinelibrary.wiley.com/doi/10.1111/prd.12474
Related Reading
- Dental Implant Recovery Complications Dallas: Guide to Safe
- Dental Implant Failure Symptoms: Early Warning Signs Guide 2025
- Can Dental Implants Get Infected Years Later? Your 2026 Gui
- Emergency Dental Implant Care Dallas 2026: Urgent Guide
- Dental Implant Specialist Follow Up Dallas 2026 | Guide & Pl

Leave a Reply
Share your thoughts or ask a question about dental implants. Your email address will not be published.