Experiencing implant pain when biting down can be a distressing and concerning issue for individuals with dental implants. While dental implants are a highly effective and durable solution for missing teeth, designed to function like natural teeth, persistent discomfort during chewing or biting indicates an underlying problem that requires professional attention. This article provides a comprehensive overview of the potential causes of implant pain when biting down, how dentists diagnose these issues, and the available treatment options in 2026, offering crucial information for maintaining your long-term oral health.
Key Takeaways
- Implant pain when biting down is a warning sign that requires prompt dental evaluation.
- Common causes include peri-implantitis, improper bite alignment, implant failure, nerve damage, or issues with the crown.
- Early diagnosis and intervention are crucial to prevent more significant complications and ensure the longevity of your dental implant.
- Treatment ranges from conservative adjustments to surgical interventions, depending on the underlying cause.
- Maintaining excellent oral hygiene and regular dental check-ups are key to preventing implant complications.
- Bite force on implants increases significantly over 6-18 months, making proper alignment and stability critical for comfort [1, 2].
- Maxillary anterior implants may be more vulnerable to overload concerns due to thinner bone [1, 2].
- For those considering dental implants in Dallas, understanding these potential issues is part of informed decision-making.
Quick Answer
Implant pain when biting down typically indicates a problem with the dental implant itself, the surrounding tissues, or the prosthetic crown. It can stem from issues like inflammation (peri-implantitis), excessive bite force, implant instability, or even nerve impingement. Immediate consultation with a dental professional in Dallas is essential for accurate diagnosis and timely treatment to safeguard the implant and your overall oral health.
What Causes Implant Pain When Biting Down?
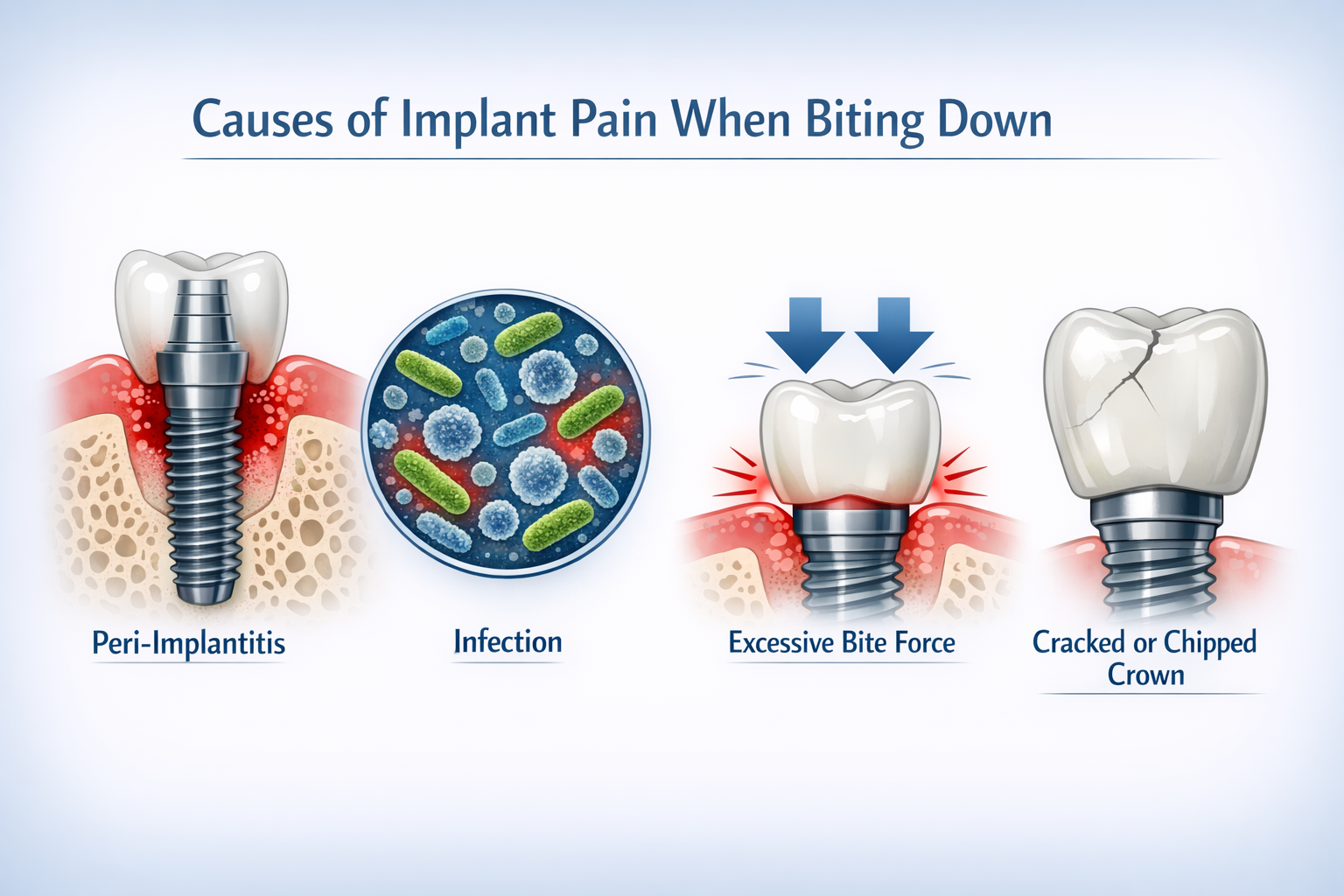
Implant pain when biting down is a clear indicator that something is amiss with your dental implant, the surrounding bone, or the prosthetic crown. Identifying the specific cause is the first step toward effective treatment. Various factors can contribute to this discomfort, ranging from biological complications to mechanical issues [3, 5].
One of the most common causes of implant pain during biting is peri-implantitis, an inflammatory condition affecting the tissues surrounding a dental implant, leading to progressive bone loss [9]. This condition is similar to periodontal disease in natural teeth and can be triggered by bacterial infection. If left untreated, peri-implantitis can compromise the stability of the implant and ultimately lead to implant failure [3, 5, 10]. Early signs often include redness, swelling, bleeding around the implant, and pus, in addition to pain when pressure is applied.
Another significant factor is occlusal overload, which refers to excessive bite force on the implant. A properly functioning dental implant should distribute bite forces evenly, similar to a natural tooth. However, if the implant-supported crown is too high or improperly aligned with opposing teeth, it can bear undue pressure. Studies show that bite force on implant-retained crowns significantly increases during the initial 6 to 18 months post-implantation as osseointegration improves and patients adjust [1, 2]. This increased force, especially in posterior molar regions where bite forces are naturally higher, can sometimes lead to micro-movements, inflammation, or even fracture if not managed properly [1, 2]. Maxillary anterior implants, due to thinner cortical bone, may be particularly susceptible to overload concerns [1, 2].
Other potential causes include:
- Implant instability or failure: While rare, an implant might not have fully osseointegrated (fused with the bone) or could have loosened over time due to various factors, including poor bone quality, excessive initial stress, or infection [9]. A significant association exists between bite force and dental implant stability over the observation period [1, 2].
- Nerve damage or impingement: Though uncommon, during implant placement, a nerve could have been irritated or damaged, leading to pain or numbness. This can manifest as sharp pain when biting down, even years later [5].
- Cracked or fractured crown/abutment: The prosthetic crown or the abutment (the connector between the implant and the crown) can fracture under excessive force or wear, exposing sensitive areas or causing instability that results in pain during chewing.
- Trauma: A direct blow to the implant area can cause pain and damage, similar to a natural tooth.
- Adjacent tooth issues: Sometimes, the pain might not originate from the implant itself but from a neighboring tooth that has developed a cavity, gum disease, or a fracture. The pain can be referred, making it feel like the implant is the source of discomfort.
- Sinus involvement: For upper jaw implants, if the implant has penetrated the sinus cavity, it can lead to discomfort, pressure, or even infection, particularly when biting or chewing [5]. This can sometimes be related to previous procedures like a sinus lift. For more information on this, you can read about Sinus Lift and Bone Graft Procedures in Dallas.
- Residual cement: Excess cement from crown placement can irritate surrounding gum tissues, leading to inflammation and pain when biting.
Understanding these possibilities underscores the importance of a thorough diagnostic examination by a qualified dental professional.
Diagnosing Implant Pain When Biting Down
When you experience implant pain when biting down, a precise diagnosis is paramount to determine the appropriate course of action. Your dentist will employ a combination of clinical examination, imaging, and patient history to pinpoint the exact cause of your discomfort. It is crucial to schedule a visit to a dentist in Dallas promptly when such symptoms arise.
The diagnostic process typically begins with a detailed clinical examination. Your dentist will visually inspect the implant site, checking for signs of inflammation, redness, swelling, or pus around the gum line. They will also gently probe the area around the implant to assess for bleeding, pocketing (indicating bone loss), or any tenderness [3, 5, 10]. They may also use a specialized tool to check the implant’s stability, looking for any mobility that might suggest a lack of osseointegration or a failing implant [1, 2].
Next, your dentist will evaluate your occlusion (bite). They will use articulating paper to check how your upper and lower teeth meet when you bite down. This helps identify any premature contacts or high spots on the implant crown that could be causing excessive force and contributing to your implant pain when biting down [1, 2]. An improper bite can place undue stress on the implant and surrounding bone, especially as bite force naturally increases in the months following implant placement [1, 2].
Radiographic imaging is an indispensable tool for diagnosing implant issues. Dental X-rays, including periapical radiographs and potentially a cone-beam computed tomography (CBCT) scan, provide detailed images of the bone structure around the implant. These images allow the dentist to assess bone levels, identify any signs of bone loss indicative of peri-implantitis, check the integrity of the implant and abutment, and rule out any nerve impingement or sinus involvement [5, 9]. Optimal dental implant X-ray frequency is important for long-term monitoring. More information on this topic can be found in our guide on Optimal Dental Implant X-Ray Frequency.
In addition to these, your dentist will also take a thorough patient history. They will ask about when the pain started, its intensity, what makes it worse or better, and any other symptoms you might be experiencing. They will also inquire about your overall health, medications, and oral hygiene habits, as these can all influence implant health [5]. For instance, certain medical conditions like diabetes can affect healing and increase the risk of implant complications [5]. If you have diabetes, understanding the specific considerations for Diabetic Dental Implant Recovery can be very helpful.
Diagnostic Tools and Techniques:
- Visual and Manual Examination: Assessing gums for inflammation, probing for pockets, checking for pus or bleeding.
- Occlusal Analysis: Using articulating paper to identify bite discrepancies and excessive force on the implant.
- Dental X-rays (Periapical, Panoramic, CBCT): To evaluate bone levels, implant integrity, and rule out underlying structural issues.
- Implant Stability Quotient (ISQ) Measurement: A non-invasive test that measures implant stability, which has a significant association with bite force [1, 2].
- Patient Symptom Description: Gathering detailed information about the nature and onset of pain.
Early diagnosis is critical. If your implant pain when biting down is due to an infection like peri-implantitis, timely treatment can often prevent severe bone loss and save the implant. Conversely, ignoring the pain can lead to implant failure, requiring more complex and costly interventions like implant removal and potentially bone grafting.
Treatment Options for Implant Pain When Biting Down
Once the cause of implant pain when biting down has been accurately diagnosed, your dental professional will recommend a tailored treatment plan. The approach will vary significantly depending on whether the issue is inflammatory, mechanical, or structural.
If the pain is attributed to occlusal overload (excessive bite force), the treatment is often straightforward. Your dentist will adjust the height and contours of the implant crown to ensure it aligns properly with your opposing teeth, thereby reducing the undue pressure on the implant [1, 2]. This process involves selectively grinding down tiny amounts of the crown material until a balanced bite is achieved. This can often alleviate the pain almost immediately by redistributing chewing forces more evenly across your dental arch. If the implant crown is fractured or excessively worn due to overload or bruxism (teeth grinding), a replacement crown may be necessary. For those experiencing bruxism, proactive measures to Prevent Damage to Dental Implants from Teeth Grinding are crucial.
For cases of peri-implantitis, treatment strategies depend on the severity of the infection and bone loss. Early-stage peri-implantitis, characterized by soft tissue inflammation without significant bone loss, may be managed with non-surgical approaches:
- Thorough debridement: Cleaning the implant surface and surrounding tissues to remove plaque, calculus, and bacterial biofilms.
- Antimicrobial therapy: Use of antiseptic rinses or local antibiotic application to control the infection.
- Improved oral hygiene instructions: Educating the patient on proper brushing techniques, including the use of special brushes like a sulcus brush for implants, and flossing around the implant to prevent recurrence. Learn more about optimal care with a Sulcus Brush for Implants.
In more advanced cases where significant bone loss has occurred, surgical intervention may be required. This could involve:
- Flap surgery: Lifting the gum tissue to gain access to the implant surface for thorough cleaning and decontamination.
- Bone grafting: If sufficient bone loss has occurred, a bone graft procedure may be performed to regenerate lost bone around the implant, enhancing its stability and supporting the surrounding tissues [5]. For information on this, see Bone Graft Costs for Dental Implants in Dallas.
- Guided tissue regeneration: Using membranes to promote the growth of new bone and soft tissue around the implant.
If the implant itself is found to be unstable or failing, especially if severe bone loss has occurred, implant removal might be the only viable option [10]. After removal, the area would need time to heal, and often, bone grafting is performed to prepare the site for a potential new implant placement in the future. The decision for removal is usually made when conservative treatments have failed, or the implant is deemed non-restorable [9].
For issues like nerve damage or residual cement, specific treatments would be implemented. Nerve compression might require surgical intervention to relieve pressure, while residual cement is typically removed through a minor procedure. If a neighboring tooth is the source of referred pain, that tooth will be treated for its specific pathology.
It’s important to note that post-surgical pain from implant placement typically peaks around 6 hours after surgery and is generally mild, resolving quickly [7]. Persistent or new onset pain when biting down, especially weeks or months after implant placement, is not typical healing discomfort and should be evaluated. Patients seeking dental implants in Dallas should prioritize finding a dentist who emphasizes patient safety and long-term oral health.
Preventing Implant Pain When Biting Down
Preventing implant pain when biting down involves a combination of vigilant oral hygiene, regular professional care, and being mindful of certain habits. Proactive measures are always more effective and less invasive than treating existing problems.
1. Maintain Excellent Oral Hygiene: This is perhaps the most critical factor in preventing peri-implantitis, a common cause of implant pain. Just like natural teeth, dental implants require meticulous cleaning to remove plaque and food debris.
- Brush twice daily: Use a soft-bristled toothbrush or an electric toothbrush, paying close attention to the areas around your implants.
- Floss daily: Use dental floss, interdental brushes, or a water flosser specifically designed for cleaning around implants to reach areas a toothbrush might miss.
- Use an antimicrobial mouthwash: Your dentist may recommend a therapeutic mouthwash to reduce bacterial load.
2. Regular Dental Check-ups and Professional Cleanings: These appointments are vital for the long-term success of your dental implants. Your dentist and dental hygienist can identify early signs of problems, such as inflammation or excessive bite force, before they become painful or severe. During these visits, the professional cleaning will remove hardened plaque (calculus) that cannot be removed by brushing alone. For insights into the financial aspects of these crucial follow-ups, you can explore the 2026 Dallas Dental Implant Cost Update.
3. Address Bruxism (Teeth Grinding): If you grind or clench your teeth, especially at night, the excessive forces can put tremendous stress on your implants, potentially leading to occlusal overload, implant pain when biting down, or even crown fracture [1, 2]. Your dentist might recommend a custom-fitted nightguard to protect your implants and natural teeth from these destructive forces. Our article on Bruxism & Dental Implants: Prevent Damage in 2026 offers comprehensive guidance.
4. Proper Bite Alignment: Ensure your dentist checks and adjusts your bite during and after the placement of your implant crown. As mentioned, bite forces can increase significantly over the first 6-18 months after implant insertion [1, 2], making regular occlusal checks important. Any “high spots” on the crown need to be adjusted to prevent uneven pressure.
5. Avoid Hard and Sticky Foods (Especially Early On): While implants are strong, it’s wise to be cautious with extremely hard candies, ice, or sticky caramels that could potentially damage the crown or place undue stress on the implant, especially during the initial healing phase.
6. Avoid Smoking and Excessive Alcohol Consumption: Both smoking and heavy alcohol use can significantly increase the risk of peri-implantitis and hinder the body’s ability to heal and maintain bone health around the implant [5, 9]. Quitting smoking is one of the best steps you can take for your overall and oral health.
7. Monitor for Early Warning Signs: Pay attention to any changes in your mouth. If you notice persistent tenderness, redness, bleeding gums around the implant, or a sensation that the implant feels “different,” contact your dentist immediately. Early detection of issues like peri-implantitis can prevent more serious complications and costly treatments like dental implant removal.
By following these preventive measures, you can significantly reduce your risk of developing implant pain when biting down and ensure the long-term success and comfort of your dental implants. For those considering tooth replacement options, it’s important to understand the full scope of care required.
When to See a Dentist in Dallas for Implant Pain
If you are experiencing implant pain when biting down, it is important to seek professional dental attention promptly. While some mild, temporary discomfort might occur during the initial healing phase after implant surgery, persistent or worsening pain, especially during chewing or biting, is not normal and indicates a potential problem.
You should schedule an appointment with a dentist in Dallas as soon as possible if you notice any of the following symptoms:
- Persistent pain when biting down or chewing: This is the primary warning sign and should never be ignored, especially if it’s a new or increasing sensation.
- Swelling or redness around the implant site: These are classic signs of inflammation or infection, such as peri-implantitis [3, 5].
- Bleeding gums around the implant: While minor bleeding can occasionally occur, consistent bleeding, particularly when brushing or flossing, warrants investigation.
- Pus discharge from the implant area: This is a definitive sign of infection and requires immediate treatment.
- A loose feeling in the implant or crown: Any mobility, however slight, indicates a problem with the implant’s integration or the crown’s attachment.
- Changes in your bite: If your implant crown feels “high” or uncomfortable when you bite, it could be an occlusal issue needing adjustment [1, 2].
- Receding gums around the implant: This can expose parts of the implant that should be covered and is often a sign of underlying issues.
- Fever or general malaise: These systemic symptoms, combined with localized pain, suggest a more widespread infection.
Delaying treatment for implant pain when biting down can lead to more severe complications, including significant bone loss, implant failure, and the need for more complex and costly procedures [9, 10]. Early intervention often allows for less invasive and more successful treatment outcomes. For those concerned about complications, understanding Dental Implant Risks and Complications in 2026 can provide further context.
When choosing a dental implant specialist in Dallas, look for a dentist with extensive experience in implant dentistry and a commitment to patient-first care. They should be able to provide clear explanations of your condition and treatment options, fostering informed decision-making. You can learn more about how to select the right professional in our guide, “How to Choose a Dental Implant Dentist Near You.” Remember, addressing concerns promptly is key to ensuring the longevity and health of your dental implants and your overall long-term oral health.
Understanding the Long-Term Outlook for Dental Implants with Pain Issues
Understanding the long-term outlook for dental implants, particularly when experiencing pain, is crucial for patients. While dental implants are known for their high success rates and durability, issues like implant pain when biting down can affect their longevity if not addressed properly. The prognosis largely depends on the underlying cause of the pain, the timeliness of intervention, and the patient’s commitment to ongoing care.
If the implant pain is due to a mechanical issue like occlusal overload or a poorly fitting crown, the long-term outlook is generally very good once the issue is corrected. Simple adjustments to the bite or replacement of a damaged crown can resolve the discomfort and restore the implant to full function. These types of problems do not inherently threaten the implant’s integration with the bone. However, continued neglect of occlusal issues can lead to persistent inflammation, micro-fractures, or even implant failure over time [1, 2, 5].
For peri-implantitis, the long-term outlook is more variable and depends heavily on the stage of the disease at diagnosis and the effectiveness of treatment.
- Early-stage peri-implantitis: When caught early, before significant bone loss occurs, non-surgical treatments combined with improved oral hygiene can often successfully manage the infection and stabilize the implant. In these cases, the implant can continue to function well for many years.
- Advanced peri-implantitis: If bone loss is extensive, surgical interventions like bone grafting or guided tissue regeneration may be necessary. While these procedures aim to save the implant and regenerate lost bone, they carry a higher risk of complications and may not always fully restore the original bone support. The long-term prognosis, even after successful treatment, might involve closer monitoring and a slightly increased risk of recurrence [9].
In cases where the implant is unstable or failing due to a lack of osseointegration, severe infection, or significant bone loss that cannot be successfully treated, the implant may need to be removed [10]. While this is certainly a setback, it doesn’t mean that future dental implants are impossible. After the removal of the failing implant, the site can be cleaned, healed, and potentially augmented with bone grafts to prepare it for a new implant placement. This process, however, adds to the overall timeline and cost of tooth replacement options.
The patient’s overall health and lifestyle choices also play a significant role in the long-term success of implants and the prevention of future pain. Conditions like uncontrolled diabetes, smoking, and certain medications can negatively impact healing and the ability to fight infection [5]. Adherence to professional advice, including regular dental check-ups, meticulous oral hygiene, and managing systemic health conditions, is paramount for a positive long-term outlook.
In summary, while implant pain when biting down is a serious concern, it is often treatable. Early diagnosis and appropriate intervention, combined with diligent patient care, can lead to a successful resolution and a long-lasting, functional dental implant. Patients considering dental implants in Dallas should discuss these factors thoroughly with their dental professional to ensure informed decision-making and optimal long-term oral health.
Case Study: Sarah’s Experience with Implant Pain in Dallas
Sarah, a 48-year-old marketing executive living in Dallas, had received a single dental implant to replace a missing molar in her lower jaw two years prior. The initial procedure and healing were uneventful, and she had enjoyed the full function of her new tooth. However, in early 2026, she began experiencing a dull ache in the area of her implant, which sharpened significantly whenever she bit down on food, especially anything hard or chewy.
Initially, Sarah thought it might be a temporary sensitivity, but the pain persisted for over a week, causing her to favor the other side of her mouth. Concerned, she contacted her local dental implant specialist in Dallas for an urgent appointment.
During her visit, the dentist performed a comprehensive examination. Visually, there was slight redness around the gum tissue of the implant, but no overt swelling or pus. When testing her bite with articulating paper, the dentist noted that the implant crown was making premature and heavy contact with the opposing upper molar, indicating occlusal overload. Radiographs (X-rays) were also taken, which revealed no significant bone loss around the implant, but did show a hairline fracture on the porcelain surface of the crown, likely a consequence of the uneven bite forces. The implant itself appeared stable in the bone, and an Implant Stability Quotient (ISQ) measurement confirmed good osseointegration.
The diagnosis was clear: Sarah was experiencing implant pain when biting down due to an improperly balanced bite and a fractured crown, likely exacerbated by the natural increase in bite force over time. The solution involved two main steps:
- Occlusal Adjustment: The dentist carefully adjusted the height of the implant crown by grinding down tiny amounts of porcelain until Sarah’s bite was perfectly balanced, ensuring even distribution of pressure.
- Crown Replacement: Due to the hairline fracture, a new, custom-fabricated crown was ordered to ensure long-term integrity and comfort.
Sarah received a temporary crown while the permanent one was being made. Within days of the occlusal adjustment, her pain when biting down significantly diminished. Once the new permanent crown was seated, her discomfort resolved completely. The dentist also recommended a custom nightguard, as Sarah admitted to occasional teeth grinding during stressful periods, to prevent future overload issues.
This case highlights the importance of addressing even seemingly minor discomfort around dental implants promptly. Early intervention for issues like occlusal overload can prevent more serious complications like peri-implantitis or implant failure, ensuring the long-term success of the dental implant procedure. Sarah’s commitment to seeking timely professional consultation helped preserve her implant and long-term oral health.
FAQ: Implant Pain When Biting Down
Q1: Is it normal to have implant pain when biting down immediately after surgery?
A1: Mild discomfort or tenderness is normal immediately after dental implant surgery, typically peaking around 6 hours and resolving quickly [7]. However, sharp or severe pain when biting down directly on the implant site within the first few days could indicate an issue and should be reported to your dentist.
Q2: What if my implant hurts when biting down months or years after placement?
A2: If implant pain when biting down develops months or years after placement, it is not normal and indicates a problem. This could be due to infection (peri-implantitis), improper bite alignment (occlusal overload), implant instability, or a fractured crown [3, 5, 10]. Contact your dentist for an immediate evaluation.
Q3: Can an improper bite cause implant pain when biting down?
A3: Yes, an improper bite (occlusal overload) is a common cause of implant pain when biting down. If the implant crown is too high or unevenly aligned, it can bear excessive force, leading to discomfort, inflammation, and potential damage to the implant or crown [1, 2].
Q4: What is peri-implantitis, and how does it relate to implant pain?
A4: Peri-implantitis is an inflammatory condition affecting the tissues around a dental implant, similar to gum disease. It is often caused by bacterial infection and can lead to bone loss, implant instability, and significant implant pain when biting down or chewing [5, 9].
Q5: What diagnostic tests will my dentist perform for implant pain?
A5: Your dentist will typically perform a clinical examination, assess your bite, and take dental X-rays (periapical, panoramic, or CBCT scans) to evaluate bone levels, implant integrity, and identify any underlying issues [5].
Q6: Can nerve damage cause implant pain when biting down?
A6: While less common, nerve damage or impingement during implant placement can sometimes lead to chronic pain, including pain when biting down. This requires careful diagnosis, often involving specialized imaging.
Q7: What are the treatment options for implant pain when biting down?
A7: Treatment varies based on the cause. It can range from bite adjustments, crown replacement, and professional cleaning for peri-implantitis, to surgical interventions like bone grafting, or in severe cases, implant removal [5].
Q8: How can I prevent implant pain when biting down in the future?
A8: Prevention involves diligent oral hygiene, regular dental check-ups, addressing bruxism (teeth grinding) with a nightguard, ensuring proper bite alignment, and avoiding hard/sticky foods [1, 2].
Q9: Does grinding my teeth affect dental implants?
A9: Yes, bruxism (teeth grinding) can place excessive force on dental implants, contributing to occlusal overload, implant pain when biting down, and potentially leading to crown fractures or peri-implantitis [1, 2]. A nightguard can help mitigate this.
Q10: What is the long-term outlook for an implant that causes pain when biting down?
A10: The long-term outlook depends on the cause and promptness of treatment. If addressed early and effectively, many implants causing pain can be saved and continue to function well. Delaying treatment can lead to implant failure [10].
Conclusion
Experiencing implant pain when biting down is a clear signal that your dental implant requires professional attention. While dental implants offer a durable and effective solution for missing teeth, issues like peri-implantitis, occlusal overload, or even mechanical problems with the crown can lead to discomfort. Ignoring these symptoms can lead to more significant complications, potentially jeopardizing the long-term success of your implant and your overall oral health.
We encourage anyone in Dallas experiencing implant pain when biting down to schedule a consultation with a qualified dental professional without delay. Early diagnosis through comprehensive clinical examination, bite analysis, and advanced imaging allows for targeted and often less invasive treatment. Whether it involves a simple bite adjustment, a deep cleaning to combat infection, or a more involved procedure, timely intervention is key to restoring comfort and function.
Maintaining excellent oral hygiene and adhering to regular dental check-ups are paramount for preventing these issues and ensuring the longevity of your dental implants. By understanding the potential causes and knowing when to seek help, you can make informed decisions about your long-term oral health and enjoy the full benefits of your tooth replacement options. For those considering dental implants in Dallas or managing existing ones, prioritizing patient safety and professional guidance is always the best approach.
References
[1] Pmc12818635 – https://pmc.ncbi.nlm.nih.gov/articles/PMC12818635/
[2] File – https://journals.plos.org/plosone/article/file?type=printable&id=10.1371%2Fjournal.pone.0340355
[3] Early Signs Of Dental Implants Needing Repair – https://dentist-foresthills.com/blog/our-office/2026/15965/early-signs-of-dental-implants-needing-repair/
[4] The Implant Surge In 2026 And What It Means For Missing Tooth Solutions – https://trinitydentalcares.com/the-implant-surge-in-2026-and-what-it-means-for-missing-tooth-solutions/
[5] Dental Implant Risks Complications In 2026 – https://www.oceanicdental.com/resource/dental-implant-risks-complications-in-2026
[6] How Dental Implants Improve Speech Chewing – https://dentalgroupoflubbock.com/how-dental-implants-improve-speech-chewing/
[7] Can Cause Roof Of Mouth Pain After Implants – https://allin1dental.com/can-cause-roof-of-mouth-pain-after-implants/
[8] Clinical Study January 2026 Patient Perspectives On Immediate Zirconia Implant Therapy – https://www.swissdentalsolutions.com/us/blog/clinical-study-january-2026-patient-perspectives-on-immediate-zirconia-implant-therapy
[9] Full Arch Dental Implant Failure Causes – https://www.minotdentalpartners.com/blog/full-arch-dental-implant-failure-causes/
[10] Tooth Implant Failure Signs – https://int.livhospital.com/tooth-implant-failure-signs/


Leave a Reply
Share your thoughts or ask a question about dental implants. Your email address will not be published.