When considering dental implants in Dallas, one of the most critical aspects for long-term success is osseointegration—the biological process where the dental implant fuses directly with your jawbone. But how do dentists objectively confirm this fusion has occurred successfully? The answer lies in the Implant osseointegration test, a crucial diagnostic step that assures the implant is stable enough to support a new tooth. Understanding this test is vital for anyone exploring tooth replacement options, as it directly impacts the safety and longevity of their dental implant procedure.
Key Takeaways
- The Implant Stability Quotient (ISQ), measured by devices like the Osstell Beacon, is the gold standard for objectively assessing implant osseointegration.
- An ISQ score of ≥70 is generally considered stable enough for initiating prosthetic loading, especially for non-splinted implants.
- Modern advancements like bioactive surfaces and AI-integrated imaging are enhancing osseointegration predictability and outcomes in 2026.
- Understanding your implant’s stability helps dentists determine the optimal time for placing your crown, bridge, or denture, leading to long-term oral health.
- Regular follow-ups and advanced testing ensure patient safety and the lasting success of your dental implant.
What is an Implant Osseointegration Test?
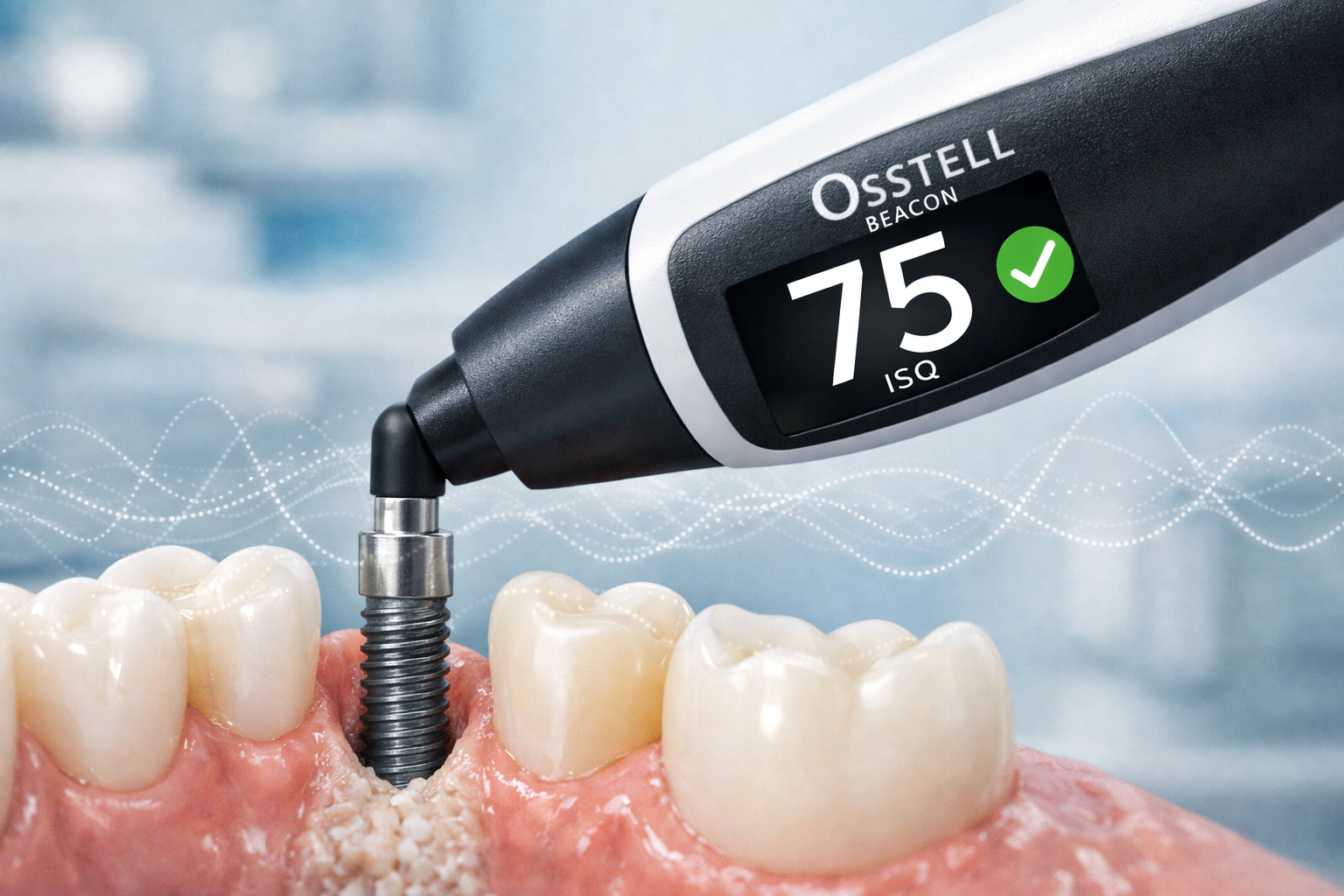
An implant osseointegration test is a non-invasive diagnostic procedure used by dental professionals to objectively measure the stability of a newly placed dental implant, confirming that it has successfully fused with the surrounding jawbone. This test is crucial for determining when an implant is ready to support a prosthetic tooth, ensuring the long-term success and durability of your new smile. Without proper osseointegration, an implant cannot withstand the forces of chewing and speaking.
The most widely accepted and scientifically backed method for performing an implant osseointegration test is Resonance Frequency Analysis (RFA) [2]. Devices like the Osstell Beacon utilize RFA to assess the implant’s stability, providing a quantitative value known as the Implant Stability Quotient (ISQ) [2]. This ISQ scale ranges from 1 to 99, with higher values indicating greater implant stability. A common clinical threshold for non-splinted implants to proceed with functional loading is an ISQ of ≥70, which typically becomes achievable after 4-8 weeks of healing with modern protocols [2]. For patients exploring dental implants in Dallas, understanding this measurement offers reassurance regarding the readiness and safety of their implant.
How Does the Implant Osseointegration Test Work?
The implant osseointegration test primarily works by measuring the implant’s stiffness in the bone, which indicates how well it has integrated with the surrounding jawbone. This is typically done using a small, hand-held device that provides an objective, numerical score.
The most common device, the Osstell Beacon, employs Resonance Frequency Analysis (RFA) [2]. Here’s a simplified breakdown of the process:
- Attaching a Smartpeg: A small, disposable transducer rod called a Smartpeg is temporarily screwed into the top of the dental implant. This Smartpeg has a known mass and stiffness.
- Sending Magnetic Pulses: The Osstell device then emits magnetic pulses that cause the Smartpeg to vibrate.
- Measuring Resonance Frequency: The vibrations are measured, and the device calculates the resonance frequency. This frequency is directly influenced by the implant’s stability within the bone. A more stable implant will vibrate at a higher frequency.
- Calculating the ISQ Value: Based on the resonance frequency, the device generates an Implant Stability Quotient (ISQ) value, ranging from 1 to 99 [2]. A higher ISQ number signifies stronger integration with the bone.
This objective measurement eliminates much of the guesswork previously involved in assessing implant stability, which often relied on subjective methods like tapping the implant or trying to feel movement. Objective measurements allow dentists to make informed decisions about when it’s safe to place the final restoration, thus minimizing the risk of complications and enhancing long-term success for your missing teeth solutions. For example, if an implant receives an ISQ score below 45 at placement, the dentist might re-evaluate and consider bone grafting before re-attempting placement [2].
When Is an Implant Osseointegration Test Performed?
An implant osseointegration test is typically performed at two key stages during the dental implant procedure: immediately after placement and again before the final prosthetic restoration is attached. These measurements help track the healing progress and ensure the implant is ready for loading.
Initially, an ISQ measurement is taken immediately after the implant surgery process to establish a baseline stability reading [2]. This initial score reflects the mechanical stability achieved during placement. Over the next several weeks to months, as the bone heals and grows around the implant (osseointegration), the ISQ score should gradually increase.
A second, more critical ISQ measurement is taken just before the restorative phase—when the permanent crown, bridge, or denture is to be attached [2]. This reading confirms that the implant has achieved sufficient biological stability to withstand chewing forces. For most non-splinted implants, an ISQ of 70 or higher is the general benchmark for functional loading [2]. This allows for safe progression to attaching the final tooth replacement, improving patient safety and confidence in their long-term oral health. If the ISQ score isn’t sufficiently high, the dentist may recommend additional healing time before proceeding. This methodical approach is a cornerstone of modern dental implant care, especially for those seeking reliable dental implants in Dallas.
Benefits of the Implant Osseointegration Test for Patients
The implant osseointegration test offers several significant benefits, primarily by ensuring patient safety, optimizing treatment timing, and contributing to the long-term success of dental implants. For individuals considering tooth replacement options, these benefits translate directly into peace of mind and predictable outcomes.
Enhanced Patient Safety
By providing an objective measure of implant stability, the test minimizes the risk of early implant failure. If an implant isn’t adequately integrated with the bone, prematurely placing a crown could lead to implant loosening or loss. The ISQ score gives dentists a clear go/no-go signal, preventing unnecessary stress on an unstable implant [2]. This is crucial for safeguarding your investment in dental implants in Dallas.
Optimized Treatment Timeline
The test allows for more precise timing of prosthetic loading. In some cases, high initial ISQ values mean that immediate or early loading protocols can be pursued, allowing patients to receive their new teeth much sooner [2]. Conversely, if stability is lower than expected, the test indicates the need for extended healing, preventing premature loading that could compromise the implant. This individualized approach ensures the most efficient yet safe treatment plan.
Predictable Long-Term Success
A confirmed high ISQ value before loading significantly increases the predictability of the implant’s long-term success. Knowing that the implant is firmly integrated means it is more likely to endure the functional demands of everyday life for many years, supporting your long-term oral health [2]. It also helps in identifying potential issues early, allowing for timely intervention if osseointegration is not progressing as expected.
Clear Communication and Reassurance
The objective nature of the ISQ score allows dentists to communicate the implant’s status clearly to patients. For instance, explaining that an ISQ of “75” means the implant is very stable can be far more reassuring than a subjective assessment. This transparency fosters trust and helps patients feel more involved and informed about their dental implant procedure. This is especially important when discussing complex decisions with a dentist.
Understanding Your ISQ Score
Your Implant Stability Quotient (ISQ) score is a numerical value that quantifies the stability of your dental implant, directly reflecting the progress of osseointegration. A higher ISQ indicates better integration and readiness for prosthetic loading.
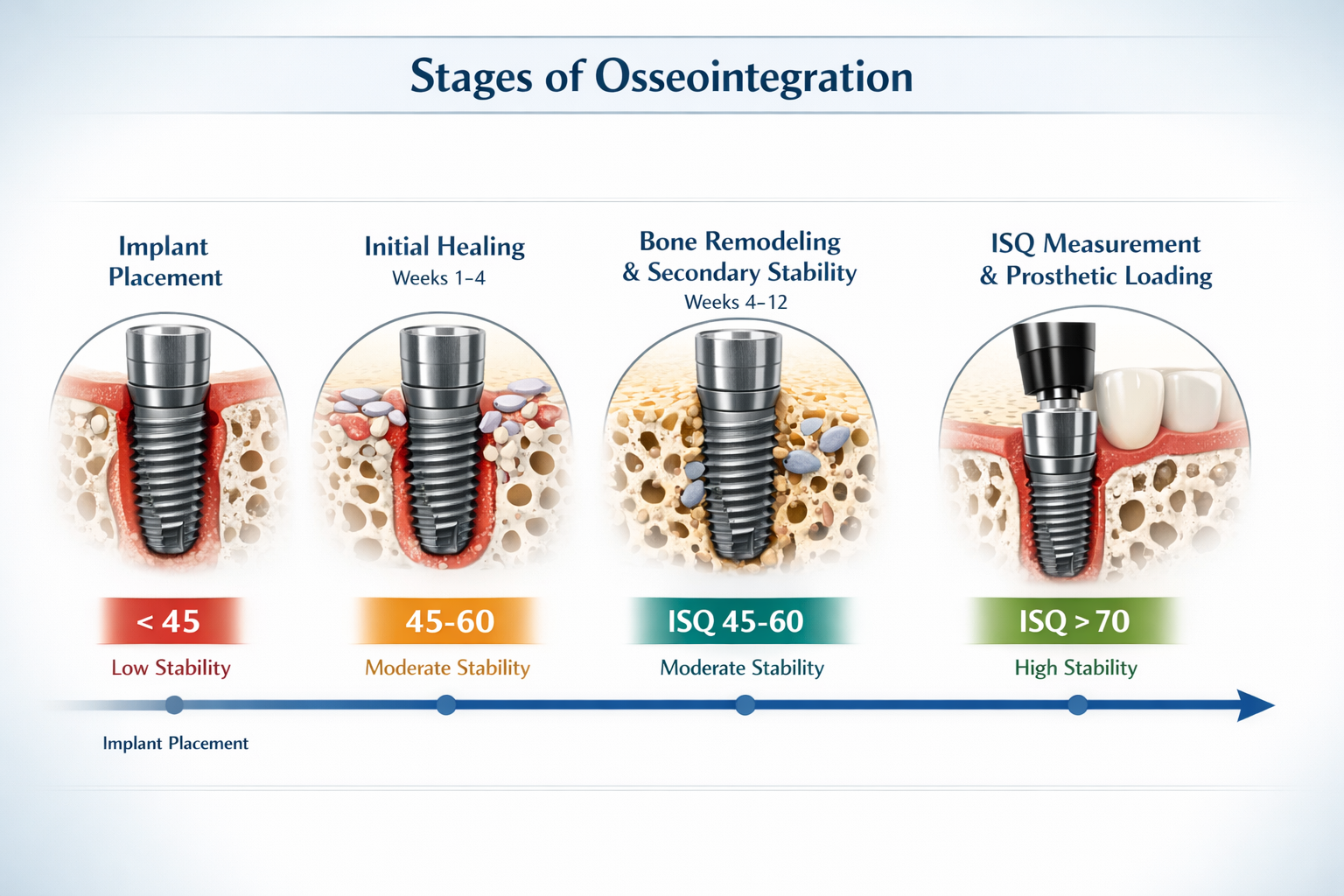
The ISQ scale ranges from 1 to 99, where:
- Low ISQ Values (<45): These scores, especially at the time of implant placement, may suggest insufficient primary stability. While not always a cause for immediate alarm if there are no other issues, consistently low readings can prompt a re-evaluation of the treatment plan, possibly requiring additional healing time or even removal and regrafting before re-attempting placement [2].
- Intermediate ISQ Values (45-69): Implants with scores in this range after initial healing are generally progressing well. They often require more time for osseointegration to mature before being loaded with a permanent restoration.
- High ISQ Values (≥70): A score of 70 or higher is typically considered the clinical threshold for initiating prosthetic rehabilitation with functional loading, particularly for single-tooth implants [2]. This indicates excellent secondary stability, meaning the implant has strongly fused with the surrounding bone and is ready to support a crown, bridge, or denture.
It’s important to remember that ISQ values can vary between individuals and even between different implants in the same patient. Factors such as bone quality, implant design, surgical technique, and healing time all play a role. Your dentist will interpret your ISQ scores in conjunction with clinical observations and X-rays (see Dental Implant X-Ray Frequency Guide 2026) to make the most appropriate decisions for your individual case. The OsstellConnect cloud-based solution can even track ISQ progression over time, facilitating shared decision-making between your surgeon, restorative dentist, and you [2].
Factors Influencing Osseointegration and ISQ Scores
Several factors can significantly influence the success of osseointegration and, consequently, your implant’s ISQ scores. Understanding these elements can help patients in Dallas better appreciate the complexities and care involved in a dental implant procedure.
Patient-Specific Factors
- Bone Quality and Quantity: Adequate bone density and volume are critical for initial implant stability and successful osseointegration. Patients with insufficient bone may require bone grafting procedures before implant placement. Conditions like osteoporosis can also affect bone healing.
- Systemic Health: Chronic diseases such as uncontrolled diabetes, autoimmune disorders, and certain medications (e.g., bisphosphonates) can impair bone healing and increase the risk of implant failure.
- Oral Hygiene: Excellent oral hygiene before and after surgery is paramount. Poor hygiene can lead to peri-implantitis, an infection that compromises osseointegration.
- Smoking: Smoking significantly impairs blood flow and healing, reducing osseointegration rates and increasing complication risks.
- Bruxism (Teeth Grinding): Excessive clenching or grinding can place undue stress on implants, especially during the healing phase, potentially hindering osseointegration. A dental implant night guard may be recommended.
Implant-Specific Factors
- Implant Material and Design: While titanium remains the gold standard, zirconia implants are showing promising osseointegration with new surface treatments [3]. Implant shape, thread design, and length also influence initial stability.
- Surface Characteristics: Modern implants often feature specialized surface treatments (e.g., laser etching, nano-texturing) designed to enhance bone cell attachment and accelerate osseointegration kinetics [1]. Bioactive surface technologies are emerging trends specifically designed to reduce healing timelines [3].
Surgical and Post-Surgical Factors
- Surgical Technique: Precise surgical placement, minimizing trauma to the bone, is crucial for achieving high primary stability and promoting uneventful healing.
- Loading Protocol: Whether an implant is immediately loaded or allowed a longer healing period (delayed loading) directly impacts the stresses placed on it during osseointegration. Objective ISQ measurements support immediate and early loading protocols when conditions are optimal [2].
- Post-Operative Care: Adhering to post-surgical instructions, including diet modifications (e.g., coffee after dental implant surgery) and maintaining proper hygiene with tools like a sulcus brush for implants, is vital for successful healing.
By carefully managing these factors, dental professionals aim to maximize the chances of successful osseointegration and achieve high ISQ scores, contributing to the long-term success of your missing teeth solutions.
The Role of Technology in Enhancing Osseointegration in 2026
Dental technology is continuously evolving, and 2026 brings exciting advancements that are significantly enhancing osseointegration, making dental implant procedures even more predictable and successful. These innovations directly impact the speed and quality of bone fusion, which in turn influences the outcomes of the implant osseointegration test.
Advanced Implant Surface Treatments
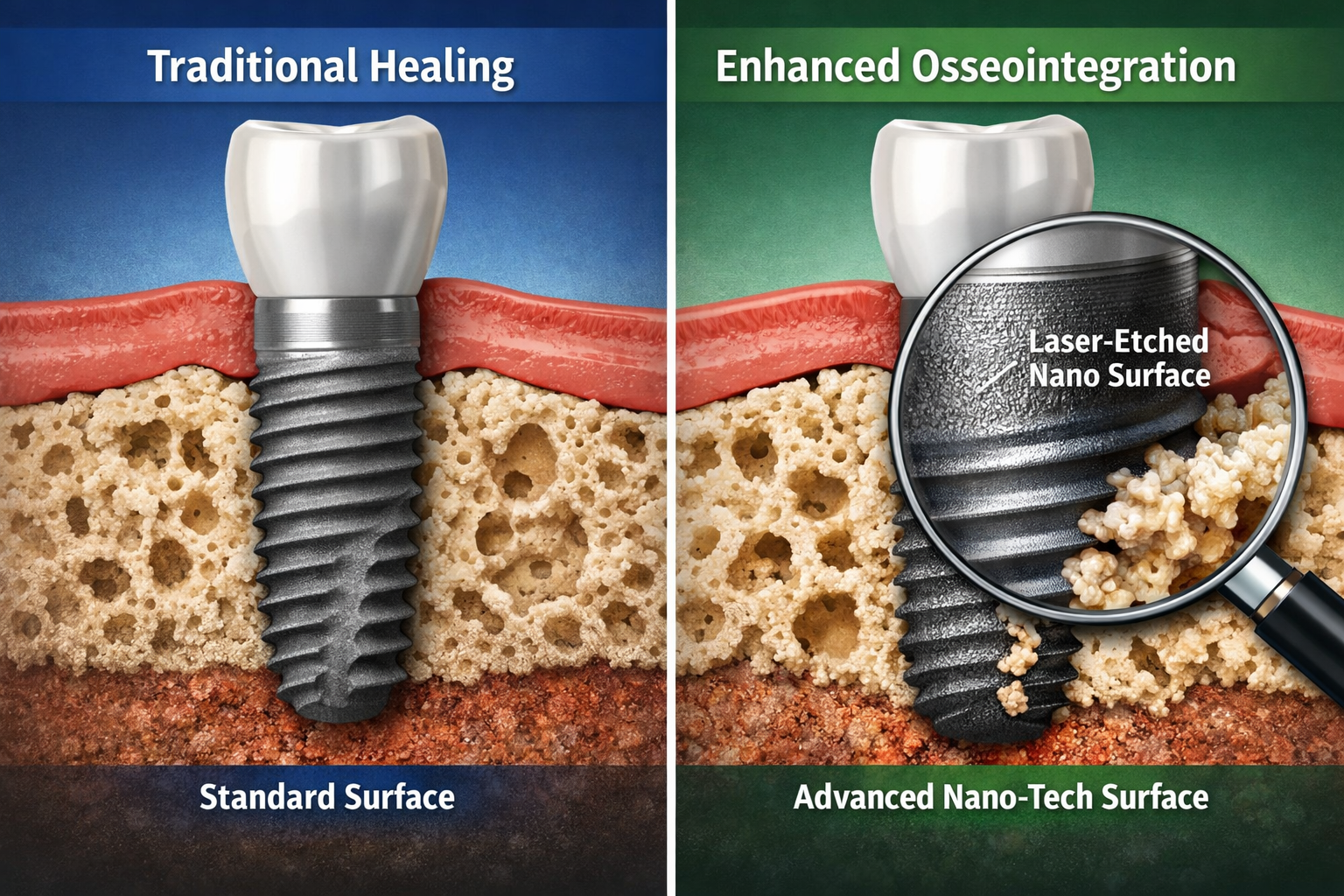
The surfaces of dental implants are no longer simply smooth metal. In 2026, manufacturers are increasingly incorporating sophisticated surface treatments designed to promote faster and stronger bone growth [1].
- Laser Etching and Nano-texturing: These techniques create microscopic irregularities on the implant surface, increasing its surface area and biocompatibility. This provides an ideal scaffold for bone cells to attach and proliferate, accelerating the osseointegration process [1].
- Bioactive Coatings: Emerging bioactive surface technologies are designed to actively stimulate bone cell activity and enhance integration [3]. These coatings can include growth factors or other osteoinductive (bone-forming) substances that encourage faster and more robust bone-to-implant contact.
AI-Integrated Imaging and Planning
Artificial Intelligence (AI) is transforming the planning phase of dental implant surgery.
- 3D CBCT (Cone Beam Computed Tomography) with AI: Advanced 3D imaging combined with AI algorithms can now predict optimal implant sizing and precise placement locations, considering bone density and anatomical structures [1]. This pre-surgical precision minimizes surgical variables, reduces trauma, and improves initial implant stability, which are all crucial for successful osseointegration. It helps ensure the implant is placed in the ideal spot for long-term health.
Evolving Materials: Zirconia Implants
While titanium has long been the gold standard, zirconia implants are gaining traction, particularly for patients seeking metal-free options or those with aesthetic concerns.
- Improved Zirconia Surfaces: New surface treatments for zirconia implants in 2026 have significantly enhanced their osseointegration capabilities, making them a more viable alternative to titanium [3]. This means patients considering different materials can expect similar high levels of bone integration and success rates. For more on materials, refer to our Titanium vs Zirconia Implant Maintenance: 2026 Guide.
These technological strides in 2026 mean that the journey to a restored smile through dental implants in Dallas is becoming even more efficient, safe, and successful. They provide better conditions for implants to achieve the high ISQ scores indicative of strong osseointegration.
What Happens if Osseointegration Isn’t Optimal?
If an implant osseointegration test reveals that an implant has not achieved optimal stability, it means the implant has not adequately fused with the jawbone, posing a risk to its long-term function and success. In such cases, your dentist will explore various management strategies to ensure your oral health.
Potential Issues
- Insufficient Primary Stability: Sometimes, the initial mechanical stability of the implant immediately after placement is too low (e.g., ISQ <45). This can happen due to poor bone quality or surgical technique [2].
- Failure of Secondary Stability: Even if primary stability was good, osseointegration might fail to progress due to infection, excessive loading during healing, or compromised healing capacity. An implant that loses stability during the healing phase may become mobile.
Management Strategies
- Extended Healing Period: For implants with slightly lower-than-optimal ISQ scores but no signs of infection or mobility, the simplest solution is often to allow for additional healing time. The body may still integrate the implant given more weeks or months. Regular follow-up with your dental implant specialist in Dallas will be crucial.
- De-loading the Implant: If an implant has been prematurely loaded and shows signs of instability, the dentist may remove the prosthetic component to allow the implant to heal without stress.
- Guided Bone Regeneration (GBR): In cases where bone loss around the implant is detected, a bone grafting procedure might be performed to encourage new bone growth around the implant and improve its stability.
- Implant Removal and Re-placement: If the implant is significantly unstable, mobile, or infected (peri-implantitis), the dentist may recommend removing it. After a healing period, which may include bone grafting, a new implant can often be placed. For more on preventing complications, refer to Dental Implant Complications Dallas | Recovery & Prevention.
- Alternative Treatment Options: In rare cases where repeated attempts at implant placement are unsuccessful, your dentist might discuss alternative tooth replacement options, such as a dental bridge or removable denture, though dental implants generally offer superior benefits (see Dental Implant vs Bridge vs Denture: 2026 Guide).
The decision on how to proceed is always made in consultation with your dentist, taking into account your specific circumstances, overall health, and long-term oral health goals. The implant osseointegration test provides critical data to guide these important decisions.
Conclusion
The implant osseointegration test, particularly through Resonance Frequency Analysis (RFA) and its resulting ISQ score, stands as a cornerstone of successful dental implant treatment in 2026. This objective measurement provides dentists with invaluable data, ensuring that your dental implant has achieved the necessary stability to function as a long-lasting, healthy tooth replacement. For patients in Dallas considering dental implants, understanding this test reinforces the commitment to patient safety and predictable outcomes.
Modern advancements in implant design, surface technology, and AI-integrated planning are continuously improving osseointegration rates, making the implant procedure more reliable than ever. By collaborating with a knowledgeable dental professional, you can navigate the process with confidence, knowing that advanced diagnostics are ensuring the foundation of your new smile is strong and secure.
If you are exploring tooth replacement options or have questions about the dental implant procedure, we encourage you to schedule a consultation with a dentist. An informed decision is the first step toward achieving the long-term oral health you deserve.
References
[1] Whats New In Dental Implants For 2025 – https://www.coastaldental.com.au/whats-new-in-dental-implants-for-2025/
[2] osstell – https://www.osstell.com
[3] Dental Implant Materials Full Comparison Guide 2026 – https://implanttrainingcourses.com/blog/dental-implant-materials-full-comparison-guide-2026/


Leave a Reply
Share your thoughts or ask a question about dental implants. Your email address will not be published.