Experiencing a tight sensation around your new dental implant can be a common and often normal part of the healing process, even if it feels unusual to you. When your dentist assures you that your “implant feels tight but dentist says normal,” it typically indicates that the osseointegration process, where the implant fuses with your jawbone, is progressing as expected, or that initial prosthetic components are seating securely. This article aims to provide a comprehensive understanding of why you might experience this feeling, what’s considered normal, and when to seek further advice, particularly for individuals in Dallas, Texas, navigating their journey with dental implants.
Key Takeaways
- A feeling of “tightness” in a dental implant is often normal during the healing phase as the implant integrates with the jawbone.
- This sensation can also result from the initial seating of the abutment or crown, which must fit snugly.
- Osseointegration, the fusion of the implant with bone, creates stability that can be perceived as tightness.
- Minor swelling or muscle tension around the implant site can contribute to this feeling in the early stages.
- Persistent or increasing pain, swelling, redness, or a loose feeling are signs that warrant immediate re-evaluation by your dentist, even if your implant initially felt tight.
- Open communication with your Dallas dentist about any post-operative sensations is crucial for proper care and peace of mind.
- Regular follow-up appointments are essential to monitor the healing and integration of your dental implant.
- Understanding the distinction between normal healing sensations and potential complications empowers patients to make informed decisions about their long-term oral health.
Quick Answer
When your “implant feels tight but dentist says normal,” it usually signifies that the dental implant is successfully integrating with your jawbone (osseointegration) or that the prosthetic components, like the crown or abutment, are seated firmly. This sensation is often a sign of stability and proper healing, reflecting the secure foundation being established for your new tooth replacement.
Why Does My Dental Implant Feel Tight? Understanding Normal Sensations
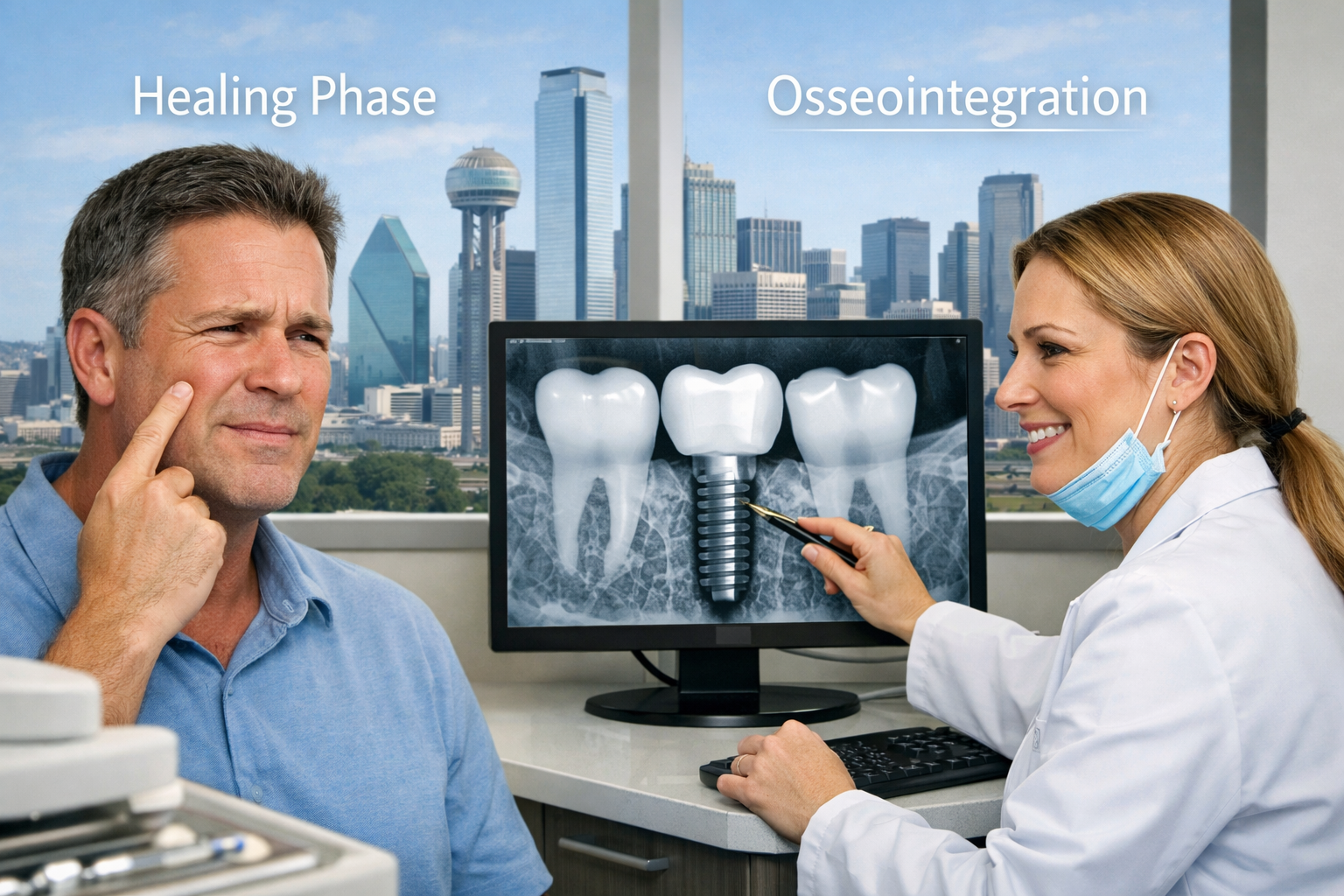
The sensation of a dental implant feeling tight is a common experience for many patients, and it’s frequently a normal indicator of the healing process. This feeling often stems from the implant’s integration with the jawbone, known as osseointegration, or the secure placement of prosthetic components [8]. Understanding these normal physiological responses can help alleviate concerns when your “implant feels tight but dentist says normal.”
During the initial weeks and months following dental implant surgery, your jawbone gradually grows around and fuses with the implant post. This critical process provides the stable foundation necessary for long-term success of the dental implant. As this fusion occurs, the implant becomes incredibly stable and immobile, which can be perceived by the patient as a feeling of tightness or firmness in the area. It’s essentially your body working to create a strong, permanent anchor for your new tooth. This sensation is distinct from pain or discomfort and usually reflects a successful biological integration.
Moreover, once the implant has sufficiently healed, the abutment (connector piece) and the final crown are attached. These components are designed to fit very precisely and snugly. The act of placing and securing these parts can also lead to a temporary feeling of tightness, as the new restoration settles into place and the surrounding tissues adapt. This is similar to how a new dental filling or crown on a natural tooth might feel slightly different or “tight” initially before your bite adjusts. Your dentist in Dallas will ensure these components are correctly seated, contributing to this secure feeling.
**Patient Insight:** “Many patients describe the ‘tight’ feeling as a sense of firm pressure or solidness, rather than sharp pain. It’s often a reassuring sign that the implant is becoming a stable part of their mouth, much like a natural tooth root.”
Factors Contributing to Normal Tightness:
- Osseointegration: The natural process of bone growing around and fusing with the titanium implant surface. This creates an incredibly strong bond, leading to a feeling of solidity.
- Abutment and Crown Placement: The secure seating of the abutment and final crown. These components are precisely manufactured to fit snugly, which can initially feel tight.
- Minor Swelling: Even weeks after surgery, residual minor swelling can contribute to a feeling of pressure or tightness around the implant site [8].
- Muscle Adaptation: The muscles around the jaw and mouth adapt to the presence of the new implant and restoration. This can sometimes manifest as a sensation of tightness, especially when clenching or chewing.
It’s important to differentiate this normal tightness from discomfort or pain. Normal tightness is generally manageable, doesn’t worsen over time, and often diminishes as you fully adapt to the implant. If you’re comparing tooth replacement options and considering dental implants in Dallas, understanding these normal sensations is part of the informed decision-making process. For more information on what to expect, consider reviewing our guide on Post-Op Dental Implant Instructions: 2026 Recovery Guide.
When Is a Tight-Feeling Implant Not Normal?
While a tight-feeling implant can be a normal part of the healing and settling process, it’s crucial to distinguish between these expected sensations and potential warning signs that might indicate a problem. An “implant feels tight but dentist says normal” usually holds true, but there are specific symptoms that, when accompanying tightness, warrant immediate re-evaluation by your dental professional [1].
The most concerning signs that differentiate normal tightness from a problem include increasing or persistent pain, noticeable swelling or redness, tenderness, a bad taste or odor, or any mobility of the implant itself [2, 3]. While initial soreness and tightness are common after implant surgery, especially within the first few days, these symptoms should gradually improve, not worsen [8]. If the sensation of tightness evolves into throbbing pain that doesn’t subside with over-the-counter pain relievers, or if you notice new or increased swelling around the implant site, it could indicate an infection or other complication [4].
Another red flag is any sign of inflammation or infection, such as pus discharge, persistent redness of the gums around the implant, or a foul odor that can’t be explained by poor oral hygiene [5]. These symptoms suggest that bacteria might be compromising the implant site, potentially leading to peri-implantitis, an inflammatory condition that can affect the tissues surrounding a dental implant [7]. Early detection and treatment of peri-implantitis are vital for the long-term success of the implant. You can learn more about managing this condition by exploring Peri-Implantitis Prevention Dallas: Early Signs, Treatment C.
Finally, any perception of movement or looseness in the implant, abutment, or crown is a serious concern that requires immediate attention [1]. A successful dental implant should feel completely stable and unmoving, similar to a natural tooth root [5]. If the “tight” feeling transitions into a wobbly or loose sensation, or if you can detect any subtle movement when touching the implant or biting down, it could signify implant failure or a problem with the prosthetic components [7]. This is an edge case where what initially felt like normal tightness could be masking an underlying issue.
**Mistake to Avoid:** Never assume worsening pain or new symptoms are just part of normal healing. Always contact your dentist if your sensations change or become more severe. Delaying evaluation can lead to more complex problems and higher repair costs.
Warning Signs to Watch For:
- Increasing or Persistent Pain: Pain that gets worse instead of better, or lasts beyond the expected healing period [9].
- Swelling and Redness: Noticeable swelling, redness, or tenderness of the gums and soft tissues around the implant, especially if it doesn’t decrease over time [3].
- Fever or Chills: Systemic signs of infection.
- Pus or Discharge: Any fluid discharge from the implant site.
- Bad Taste or Odor: A persistent unpleasant taste or smell coming from the implant area [5].
- Implant Mobility: The implant itself, the abutment, or the crown feels loose or wobbly [1]. This is a critical indicator of potential failure.
- Gum Recession: Gums pulling away from the implant, exposing more of the metal [6].
- Difficulty Chewing: New or increased difficulty or pain when chewing, especially if accompanied by other symptoms.
If you experience any of these symptoms in Dallas, TX, it’s essential to contact your dental implant specialist immediately. Early intervention can often resolve problems before they become more severe, potentially saving your implant.
The Importance of Communication and Follow-Up Appointments
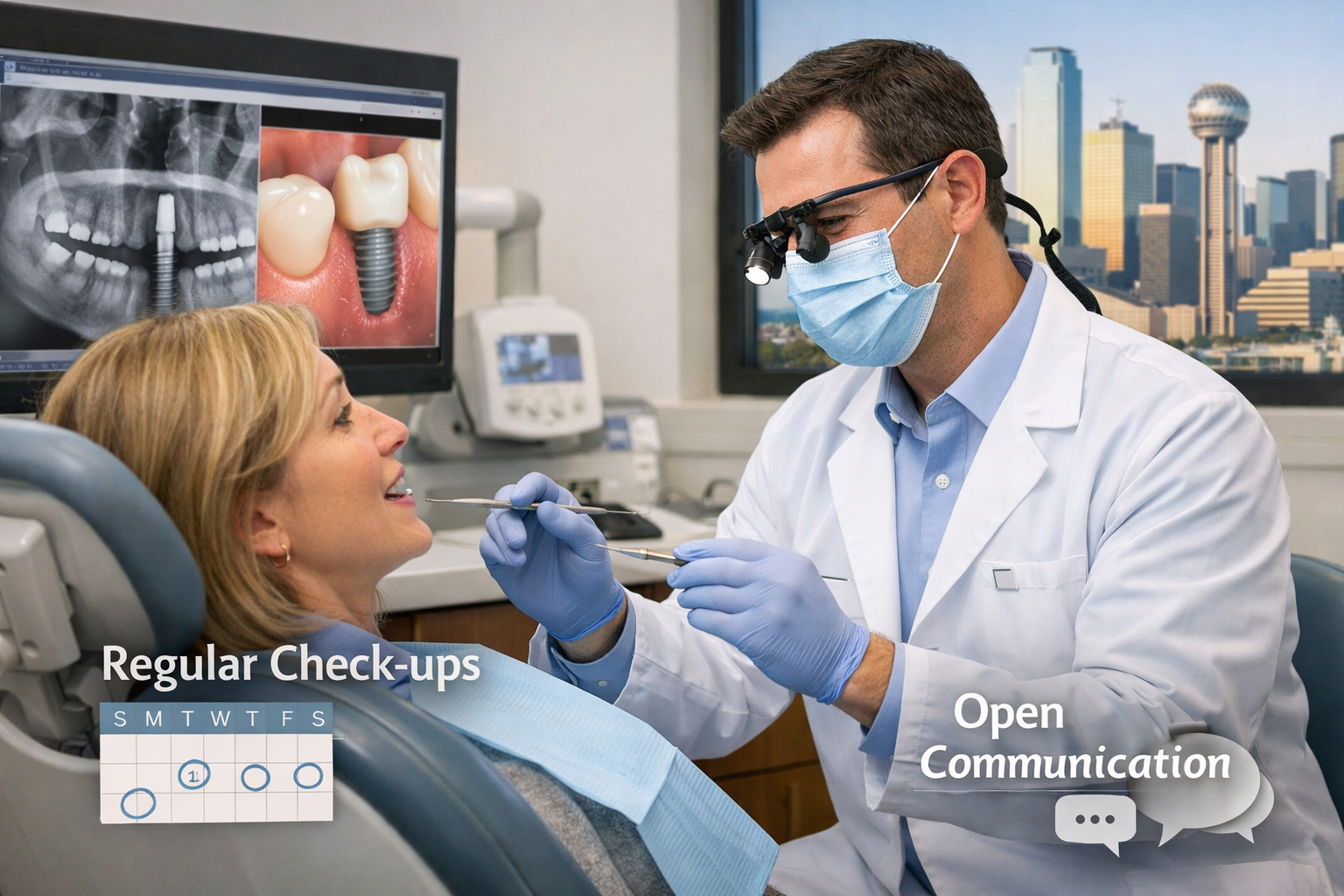
Effective communication with your dental professional and diligent attendance at follow-up appointments are paramount when you have a dental implant, especially if you perceive that your “implant feels tight but dentist says normal.” These interactions ensure your healing is monitored, address any concerns you may have, and protect your long-term oral health.
Your dentist relies on your feedback to understand your experience post-surgery. Even if a sensation like tightness is common, describing it accurately—whether it’s a dull pressure, a sharp pain, or an intermittent feeling—provides valuable diagnostic information [9]. Don’t hesitate to ask questions or express any worries, no matter how minor they seem. This open dialogue helps your dentist differentiate between a normal healing response and a subtle sign of a developing issue. For example, if the tightness is accompanied by sensitivity to hot or cold, that might point to a different problem than simple osseointegration. Preparing a list of Essential Questions to Ask Your Dentist About Implants in 2 can be highly beneficial.
Follow-up appointments are scheduled to physically assess the implant site, review X-rays, and confirm proper healing and integration. These visits allow your dental team to:
- Visually Inspect the Site: Check for any signs of inflammation, infection, or gum recession that might not be obvious to you [7].
- Review Radiographs (X-rays): Monitor bone healing around the implant and ensure the implant is stable and there’s no bone loss [2]. This is particularly important for checking osseointegration.
- Assess Bite and Prosthetic Fit: Ensure the abutment and crown are seated correctly and that your bite is comfortable, preventing undue stress on the implant [8].
- Provide Oral Hygiene Guidance: Reinforce proper cleaning techniques specific to dental implants, which are crucial for preventing complications like peri-implantitis.
- Address Concerns: Provide professional reassurance or take corrective action if any issues are identified.
For individuals in Dallas, TX, seeking the best long-term outcomes for their tooth replacement options, regular follow-up care with a skilled dental implant specialist is non-negotiable. These appointments are part of the ongoing commitment to patient safety and the longevity of your implant. They are an opportunity for both you and your dentist to collaborate on maintaining your long-term oral health. You can find more details about post-treatment care by exploring our insights into Dallas Dental Implant Follow-Up: Ensuring Lasting Smile Suc.
Checklist for Effective Communication and Follow-Up:
- Keep a Log: Note down when you feel the tightness, how long it lasts, what makes it better or worse, and any other accompanying symptoms.
- Be Specific: Instead of “it feels tight,” try to describe it as “a constant pressure,” “a dull ache,” or “it feels like something is pushing against my gum.”
- Don’t Self-Diagnose: Avoid relying solely on online information. Always discuss your symptoms with your dentist.
- Attend All Scheduled Appointments: Even if you feel fine, these appointments are crucial for professional monitoring.
- Prepare Questions: Write down any questions or concerns before your appointment to ensure you don’t forget anything.
Example Scenario:
- Patient: “My implant feels tight, almost like it’s clenched, especially in the mornings.”
- Dentist: (After examination and X-ray) “Your implant is integrating well, which can feel very solid. The morning tightness suggests you might be clenching or grinding your teeth at night. We can discuss a nightguard to protect your implant and natural teeth.”
This highlights how specific communication can lead to tailored solutions and continued patient comfort, ensuring your dental implant procedure continues smoothly.
What is Osseointegration and How Does it Cause Tightness?
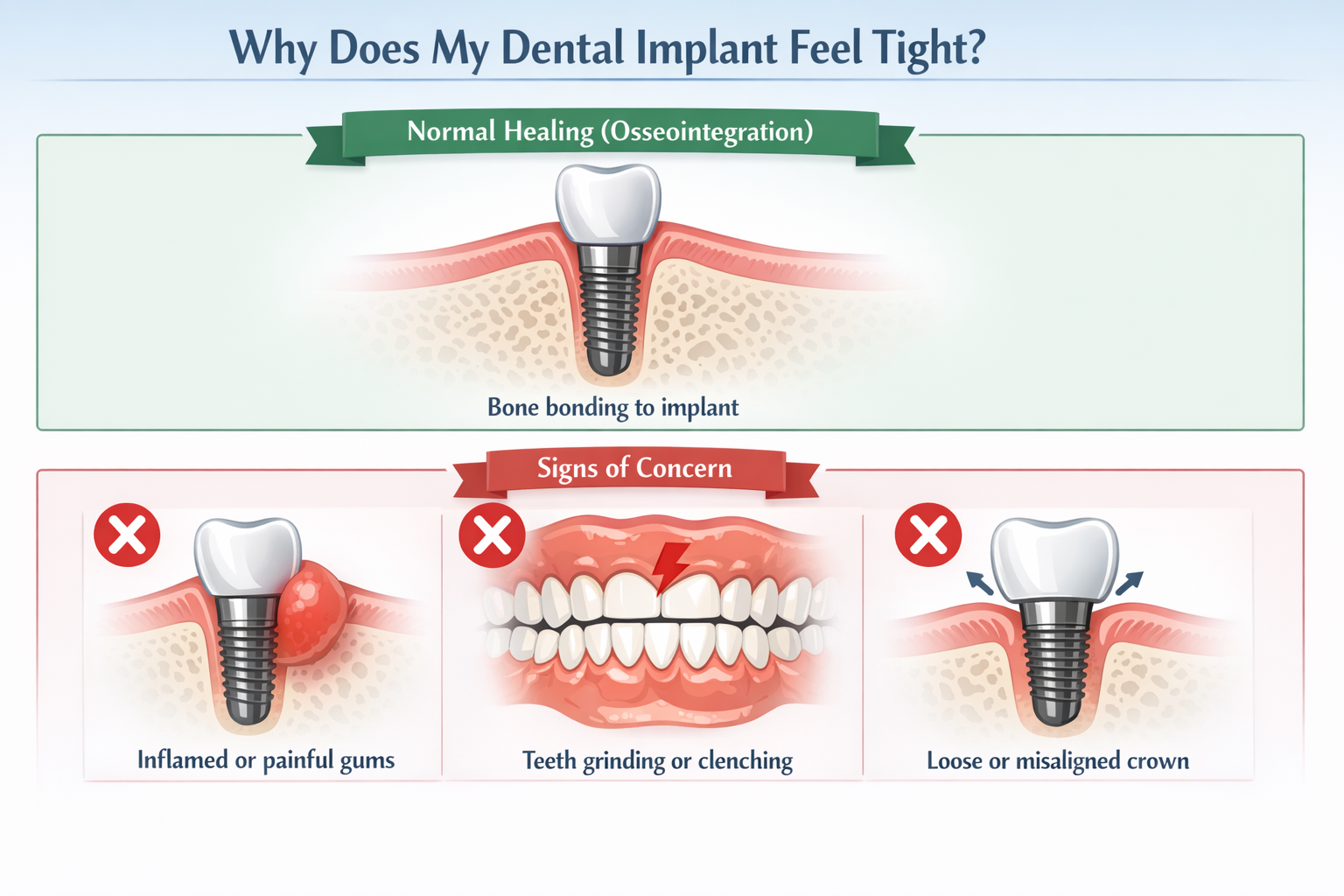
Osseointegration is the foundational biological process that makes dental implants a successful and durable tooth replacement option. It is the direct structural and functional connection between living bone and the surface of a load-carrying implant [8]. This critical phenomenon, where the jawbone physically grows into and fuses with the titanium implant, is often the primary reason why an “implant feels tight but dentist says normal” during the healing phase.
When a dental implant is surgically placed into the jawbone, the body’s natural healing mechanisms are activated. Over several weeks to months, specialized bone cells begin to migrate to the implant surface and deposit new bone tissue directly onto it. The unique biocompatibility of titanium, the material typically used for implants, allows this direct bone-to-implant contact without forming fibrous tissue in between. This process essentially locks the implant into the bone, creating an incredibly strong and stable anchor, much like a natural tooth root.
The sensation of tightness or firmness arises as this osseointegration progresses. As the bone integrates and hardens around the implant, the implant becomes less mobile and more intimately connected with the surrounding bone structure. Patients often perceive this increased stability as a feeling of solidity or pressure in the area. It signifies that the implant is becoming a stable, permanent fixture within your jaw. This sensation is generally a positive indicator that the implant is on its way to successful integration, forming the bedrock for your new crown, bridge, or denture.
The Stages of Osseointegration and Perceived Tightness:
- Initial Stability (Post-Surgery): Immediately after surgery, the implant’s stability comes from its mechanical fit in the bone. There may be some tenderness and swelling, which can contribute to a feeling of pressure.
- Early Healing (Weeks 1-6): The initial bone healing begins. New bone cells start to form around the implant. During this phase, the implant’s mechanical stability might slightly decrease before biological integration fully takes over.
- Active Osseointegration (Months 2-6): This is the crucial period where significant bone growth and fusion occur. As the bone strengthens around the implant, the patient may experience a growing sense of firmness or “tightness” as the implant becomes more robustly integrated.
- Maturation and Remodeling (Beyond 6 Months): The bone continues to remodel and strengthen around the implant, leading to long-term stability. The tight feeling often subsides into a natural, stable sensation similar to that of a natural tooth.
For patients considering dental implants in Dallas, understanding osseointegration helps manage expectations for the healing timeline and sensations. It underscores why patience is a virtue during this process and why regular check-ups with your dental professional are so important. The success of dental implant procedures heavily relies on this biological fusion.
Distinguishing Between Normal Healing Discomfort and Implant Complications
It’s common for patients to experience some level of discomfort after dental implant surgery. However, knowing the difference between normal healing sensations and potential complications is crucial for your long-term oral health. When your “implant feels tight but dentist says normal,” it’s often about understanding this distinction.
Normal healing discomfort is typically characterized by mild to moderate pain that gradually subsides over days or weeks, manageable with over-the-counter pain relievers [8, 10]. Swelling and bruising are also common in the initial days following surgery and should decrease steadily. The “tight” feeling often falls into this category, representing the feeling of the implant integrating or the new prosthetic components settling into a secure position. This type of discomfort should not worsen over time; rather, it should steadily improve. The surrounding tissues might feel firm to the touch, and there might be a slight pressure sensation when biting, but it shouldn’t be sharp or debilitating pain. For more on what to expect during recovery, see our guide on Senior Dental Implant Healing Time: Guide for 2026.
In contrast, signs of a complication often involve symptoms that are persistent, worsening, or atypical [1, 2]. These may include:
- Severe or Worsening Pain: If the pain increases in intensity or doesn’t respond to medication, it’s a red flag [4].
- Significant or Prolonged Swelling: Swelling that doesn’t decrease, or gets worse after the initial few days, could indicate an infection [3].
- Redness and Warmth: Increased redness and warmth around the implant site, beyond what’s expected for normal inflammation.
- Pus or Discharge: Any yellow or white discharge from the implant site is a clear sign of infection.
- Implant Mobility: The most critical sign of implant failure is if the implant, abutment, or crown feels loose or moves when touched or chewed upon [5, 7].
- Nerve Damage Symptoms: Numbness, tingling, or altered sensation in the lip, tongue, or chin, which may indicate nerve impingement [1].
- Difficulty Opening Mouth or Swallowing: These could be signs of more severe swelling or infection.
For individuals with missing teeth solutions being addressed in Dallas, TX, it’s vital to communicate any persistent or concerning symptoms to your dentist immediately. Early detection of complications, such as peri-implantitis or issues with osseointegration, significantly increases the chances of successful intervention and salvaging the implant [7]. Waiting too long can lead to more extensive treatment, potential implant removal, and additional costs like those associated with Dental Implant Repair Cost: Your Comprehensive Guide for 2025.
Comparison Table: Normal Healing vs. Complication
| Feature | Normal Healing Discomfort | Potential Complication |
|---|---|---|
| Feeling | Mild tightness, dull pressure, solidness, transient | Worsening sharp pain, throbbing, intense pressure |
| Pain Level | Manageable with OTC pain relievers, gradually decreases | Severe, persistent, unresponsive to medication |
| Swelling | Initial, subsides within a few days/week | Persistent, increasing, or new swelling |
| Redness/Warmth | Mild and localized initially | Increasing, spreading redness; warmth |
| Discharge | None | Pus, foul odor, bad taste |
| Implant Stability | Absolutely stable, no movement | Any noticeable movement or looseness in implant/crown/abutment |
| Duration | Improves steadily over days/weeks | Persists or worsens over time |
Understanding these distinctions empowers patients to be active participants in their dental implant journey and seek help promptly when needed, ensuring the best possible long-term oral health outcomes.
Managing the Sensation of Tightness: What You Can Do
When your “implant feels tight but dentist says normal,” managing this sensation primarily involves understanding the healing process and adhering to your dentist’s post-operative instructions. While the feeling of tightness is often benign, certain actions can help you cope and ensure optimal healing for your dental implants in Dallas.
First and foremost, continue to follow the oral hygiene recommendations provided by your dental implant specialist. Keeping the implant site clean is crucial for preventing infection and promoting healthy tissue integration. This typically involves gentle brushing around the area with a soft-bristled toothbrush, using prescribed antiseptic mouthrinses, and potentially specialized cleaning tools. Proper oral health education is vital for the longevity of your implant.
Secondly, pay close attention to your diet and habits. While your implant is healing, a soft diet can prevent undue pressure on the new implant site. Avoid hard, chewy, or crunchy foods that could dislodge the healing cap or place excessive stress on the integrating implant. If you suspect that clenching or grinding your teeth (bruxism) is contributing to the tightness, discuss this with your dentist. They might recommend a nightguard to protect your implant and natural teeth, which can also help alleviate muscle tension that contributes to a tight feeling.
Practical Steps for Managing Tightness:
- Maintain Excellent Oral Hygiene: Gently clean around the implant area as instructed. This prevents infection and promotes healthy tissue response.
- Adhere to a Soft Diet: Especially in the early healing stages, consuming soft foods minimizes stress on the implant.
- Manage Clenching/Grinding: If your dentist suspects bruxism, a nightguard can significantly reduce stress and discomfort.
- Cold Compress (Early Stages): In the immediate post-operative period, applying a cold compress to the outside of your cheek can help reduce swelling and numb the area, easing tightness.
- Over-the-Counter Pain Relievers: If the tightness is accompanied by mild discomfort, over-the-counter pain relievers (like ibuprofen or acetaminophen) can help manage it, as advised by your dentist [10].
- Avoid Smoking: Smoking significantly impairs healing and can increase the risk of implant complications. It’s best to avoid it completely during the healing process.
- Stay Hydrated: Drinking plenty of water supports overall healing processes.
- Rest: Adequate rest allows your body to dedicate energy to healing.
It’s important to differentiate management of normal tightness from ignoring actual problems. If the tightness evolves into severe pain, swelling, or any other warning signs discussed previously, these home care steps are not substitutes for professional dental advice. Always consult your dentist if you notice any concerning changes. Your dentist in Dallas will provide specific guidance tailored to your individual healing process and can offer solutions for any persistent discomfort.
Long-Term Outlook: What to Expect from a Well-Integrated Implant
The long-term outlook for a well-integrated dental implant, even one that initially made you think, “my implant feels tight but dentist says normal,” is exceptionally positive. Dental implants are renowned for their durability, stability, and ability to function much like natural teeth, offering a reliable solution for missing teeth. With proper care and regular maintenance, dental implants in Dallas can last for decades, often a lifetime.
Once osseointegration is complete and the final restoration (crown, bridge, or denture) is placed, a successful implant should feel comfortable and natural. The initial sensation of tightness typically fades, replaced by a feeling of stability and belonging. You should be able to chew, speak, and smile with confidence, without awareness of the implant itself [8]. The goal of a dental implant procedure is to restore both function and aesthetics, and a well-integrated implant achieves this by becoming a seamless part of your oral anatomy.
Maintaining this long-term success hinges on a few critical factors:
- Excellent Oral Hygiene: Just like natural teeth, implants require diligent brushing and flossing to prevent plaque buildup, which can lead to peri-implantitis [6]. Regular cleaning helps protect the gum tissue and bone supporting the implant.
- Regular Dental Check-ups: Routine visits to your Dallas dentist are essential. These appointments allow your dental team to monitor the implant’s health, check for any early signs of complications, and perform professional cleanings that specifically address implant care.
- Avoid Destructive Habits: Habits like nail-biting, chewing on ice, or using your teeth as tools can damage both natural teeth and implants. If you clench or grind your teeth, wearing a nightguard is crucial to protect your investment.
- Healthy Lifestyle: A balanced diet and overall good health contribute to the health of your gums and jawbone, supporting the long-term integrity of your implant.
The functional benefits of well-integrated implants are significant. They preserve bone structure, prevent the shifting of adjacent teeth, and allow for a diverse diet without restrictions. The aesthetic benefits are equally important, as implants can restore a natural-looking smile, boosting self-confidence. For those in Dallas seeking comprehensive oral health education, understanding the long-term commitment to care is as important as the initial implant cost in Dallas.
**Long-Term Benefit:** A well-maintained dental implant can significantly enhance your quality of life, allowing you to eat your favorite foods, speak clearly, and smile without hesitation for many years to come.
While dental implants boast a high success rate, typically over 95%, challenges can occasionally arise. However, with vigilant home care and consistent professional oversight by your dental implant specialist, most patients enjoy a lifetime of healthy, functional implants. If you ever have questions about the care or longevity of your implants, consulting with a dentist specializing in dental implant procedures is always the best course of action.
Frequently Asked Questions
Is it normal for my dental implant to feel tight after the crown is placed?
Yes, it is often normal for a dental implant to feel tight after the crown is placed. This sensation usually indicates that the crown is securely seated and properly fitted, which is essential for stability and function. It typically subsides as your mouth adjusts.
How long does the tight feeling last after a dental implant?
The tight feeling after a dental implant can vary. If it’s related to initial healing and osseointegration, it might last for several weeks or months. If it’s due to the crown seating, it usually resolves within a few days to a couple of weeks as you adapt to the new bite.
Should my dental implant feel tight when I bite down?
A feeling of firm pressure or solidness when you bite down is generally normal, especially in the early stages or if your bite is still adjusting. However, it should not be accompanied by sharp pain. If you experience increasing pain or discomfort, consult your dentist.
Can a tight dental implant indicate a problem?
While a tight feeling is often normal, if it’s accompanied by increasing pain, swelling, redness, pus, or any looseness of the implant or crown, it could indicate a complication like infection or implant failure. Always discuss these symptoms with your dentist.
What should I do if my implant feels tight and causes discomfort?
If your implant feels tight and causes discomfort, first adhere to your dentist’s post-operative instructions. You can try over-the-counter pain relievers if cleared by your dentist. If the discomfort persists, worsens, or is accompanied by other concerning symptoms, contact your dental implant specialist in Dallas immediately.
Why would my dentist say “normal” if my implant feels tight?
Your dentist says “normal” when an implant feels tight because they have evaluated the site, potentially with X-rays, and determined that the sensation is consistent with healthy healing, osseointegration, or proper seating of prosthetic components, rather than a complication.
Does “tight” mean the implant is integrating well?
Often, a feeling of solidity or “tightness” can be a positive sign that the implant is integrating well with the jawbone through osseointegration. This means the bone is fusing around the implant, creating a stable foundation.
Can clenching or grinding cause my implant to feel tight?
Yes, clenching or grinding your teeth (bruxism) can cause surrounding muscles to tense, leading to a feeling of tightness or pressure around your dental implant. Your dentist might recommend a nightguard to alleviate this.
When should I be concerned about a tight-feeling implant?
You should be concerned if the tightness is accompanied by severe or worsening pain, new or persistent swelling, redness, a bad taste, pus, or any movement of the implant or crown. These are signs that require immediate dental attention.
How do dentists check if an implant is normally tight or problematic?
Dentists check by performing a clinical examination, assessing the gum tissue, probing for any pockets, and taking X-rays to evaluate the bone level around the implant. They also test the implant for any mobility and check the bite.
Conclusion
The experience of having your “implant feels tight but dentist says normal” is a common one for many dental implant patients in Dallas, TX, and around the world. This sensation is often a positive indicator of the healing process, particularly the crucial phase of osseointegration, where your jawbone fuses with the implant to create a stable foundation. It can also arise from the secure placement of the final crown or abutment, which must fit snugly for optimal function.
Understanding the difference between normal healing sensations and potential warning signs is paramount for your peace of mind and the long-term success of your dental implant. While a feeling of solidness or firm pressure is usually benign and will typically diminish over time, any accompanying symptoms such as increasing pain, persistent swelling, redness, pus, or implant mobility warrant immediate consultation with your dental professional.
At Dental Implant Education – Dallas TX, we emphasize patient education, open communication, and diligent follow-up care as cornerstones of a successful dental implant journey. By adhering to your dentist’s post-operative instructions, maintaining excellent oral hygiene, and attending all scheduled check-ups, you empower yourself to achieve lasting oral health and enjoy the full benefits of your missing teeth solutions. If you have any concerns about your dental implant, never hesitate to reach out to your dentist. Your long-term oral health is our priority.
References
[1] 7 Warning Signs Of Dental Implant Trouble – https://www.mystuartfamilydentist.com/7-warning-signs-of-dental-implant-trouble/
[2] Is Your Dental Implant Failing – https://grandrapidsdentist.com/blog/is-your-dental-implant-failing/
[3] Warning Signs Of Dental Implant Failure – https://www.drjaydental.com/warning-signs-of-dental-implant-failure/
[4] Why Is My South Jersey Dental Implant Suddenly Hurting – https://sagedentalnj.com/why-is-my-south-jersey-dental-implant-suddenly-hurting/
[5] Signs Your Dental Implant Is Failing – https://drmatthenry.com/signs-your-dental-implant-is-failing/
[6] 6 Reasons For Sensitivity In Dental Implant – https://www.udcwhiting.com/blog/6-reasons-for-sensitivity-in-dental-implant/
[7] Signs Your Dental Implant Needs To Be Repaired – https://www.smileforeveratlanta.com/signs-your-dental-implant-needs-to-be-repaired
[8] Pain After Dental Implants Understanding Whats Normal While You – https://www.smilesofwilliamsburg.com/dental-services/restorative/blog/pain-after-dental-implants-understanding-whats-normal-while-you
[9] Dental Implant Discomfort What It Could Be Telling You – https://www.barclayfamilydental.com/dental-implant-discomfort-what-it-could-be-telling-you
[10] How Long Do Dental Implants Hurt – https://www.ufbergdental.com/how-long-do-dental-implants-hurt


Leave a Reply
Share your thoughts or ask a question about dental implants. Your email address will not be published.