Experiencing discomfort around a dental implant years after its placement can be concerning. While dental implants are renowned for their durability and long-term success, persistent pain, swelling, or unusual sensations emerging long after the initial healing period is not normal and always warrants professional evaluation. This article from Dental Implant Education – Dallas TX will help you understand the common causes of implant discomfort years later, the symptoms to watch for, and the crucial steps to take to protect your oral health.
Key Takeaways
- Persistent pain or discomfort around a dental implant years after placement is abnormal and requires immediate dental evaluation.
- The most common long-term complication is peri-implantitis, an infection affecting the gums and bone around the implant, potentially leading to implant failure if untreated.
- Other causes of late-onset discomfort include mechanical issues like loose crowns or abutments, excessive biting force (bruxism), nerve damage, or issues with adjacent teeth.
- Symptoms like bleeding, swelling, bad breath, gum recession, implant mobility, or changes in your bite are critical warning signs.
- Early diagnosis and intervention by a dental professional in Dallas are essential for successful treatment and preventing further complications.
- Treatment options range from non-surgical interventions (professional cleaning, antibiotics) to surgical procedures, depending on the cause and severity.
- Regular dental check-ups and diligent oral hygiene are crucial for the long-term health and stability of your dental implants.
- Ignoring late-onset implant discomfort can lead to more serious issues, including implant failure and the need for costly revision surgery.
Quick Answer
If you’re experiencing implant discomfort years later, it’s crucial to consult a dentist promptly, as this is not a normal part of having a dental implant and often indicates an underlying issue such as infection, bone loss, or a mechanical problem. Early evaluation and diagnosis are key to effectively treating the cause and preserving your long-term oral health [4].
Why Does My Dental Implant Hurt Years Later?
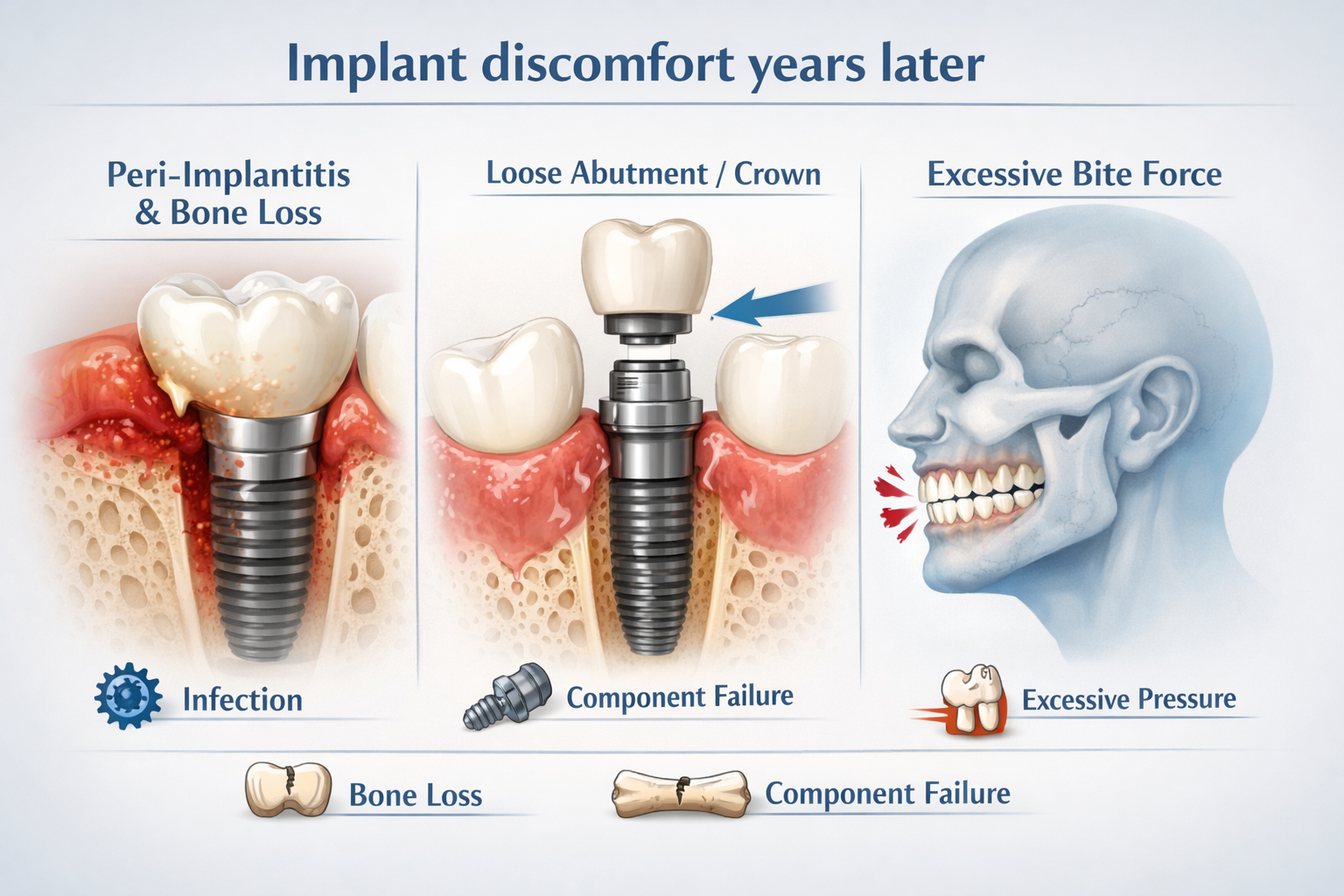
Your dental implant may hurt years later because a new issue has developed, such as an infection (peri-implantitis), mechanical complication, or damage to surrounding structures, none of which are normal for a stable implant [1, 4]. Dental implants are designed for longevity, and discomfort that arises long after the initial healing period typically signals a problem that needs attention.
The stability and success of dental implants depend on a process called osseointegration, where the implant fuses with the jawbone. Once this process is complete, the implant should feel as natural as a real tooth. If discomfort or pain develops years later, it indicates a disruption to this stability or the health of the surrounding tissues.
Common Causes of Late-Onset Implant Discomfort:
- Peri-Implantitis (Infection): This is the most common and serious complication, affecting the gums and bone surrounding the implant [1, 7]. Similar to gum disease around natural teeth, peri-implantitis is an inflammatory condition often caused by bacterial accumulation. It can lead to bone loss around the implant, ultimately weakening its support. Some sources indicate this condition affects 10-20% of implants over time [1]. Early signs can include bleeding gums around the implant, swelling, and localized pain. If left untreated, it can lead to implant mobility and eventual failure [7, 9].
- Mechanical Complications:
- Loose Abutment or Crown: The abutment connects the implant to the crown. If this component or the crown itself becomes loose, it can create discomfort, instability, and an improper bite [1, 4].
- Implant Fracture: Although rare, an implant can fracture due to excessive stress or trauma.
- Excessive Force (Bruxism/Clenching): Grinding or clenching your teeth, especially at night (bruxism), can place undue stress on the implant and surrounding bone, leading to pain, bone loss, or even damage to the implant or crown [4]. Wearing a dental implant night guard can help protect against this.
- Nerve or Tissue Damage: While often associated with initial implant surgery, nerve damage can sometimes manifest with delayed symptoms, or irritation to surrounding nerves could occur if the implant is placed too close to a nerve [1].
- Problems with Adjacent Teeth or Structures: Sometimes, discomfort felt near an implant might originate from a neighboring tooth experiencing decay, infection, or root issues, or from issues with the sinus cavity in the upper jaw [1].
- Improper Bite Alignment: If your implant crown is not perfectly aligned with your natural bite, it can create uneven pressure points, leading to discomfort or pain over time [4].
- Poor Oral Hygiene: Inadequate cleaning around the implant can lead to plaque buildup, fostering bacterial growth and increasing the risk of peri-implantitis [7]. Our guide on All-on-4 Cleaning Routine: Master Your Implant Care in 2026 offers excellent tips.
For those considering dental implants in Dallas, understanding these potential long-term issues highlights the importance of choosing an experienced dentist and maintaining rigorous post-treatment care. If you experience any discomfort, it is better to seek prompt evaluation rather than wait for symptoms to worsen.
Recognizing Symptoms of Implant Discomfort Years Later
Recognizing the symptoms of implant discomfort years later is critical because early detection significantly improves the chances of successful intervention and prevents more serious complications, such as implant failure [7, 8]. While minor initial discomfort is normal after dental implant surgery, any new or persistent pain, swelling, or unusual sensations emerging long after the implant has healed and integrated should be evaluated by a dental professional.
Key Symptoms to Watch For:
- Persistent Pain or Tenderness: Unlike the initial post-surgical pain that subsides, new or lingering pain, aching, or tenderness around the implant site is a significant red flag [1, 4]. This pain might be mild at first but can worsen over time, especially when chewing or applying pressure.
- Swelling and Inflammation: Noticeable swelling or redness of the gum tissue surrounding the implant, which persists for more than a few days, indicates inflammation or infection [1, 7].
- Bleeding Gums: Gums that bleed easily when brushing, flossing, or even spontaneously around the implant site are a common sign of peri-implantitis [1, 7].
- Bad Breath or Bad Taste (Halitosis): Persistent bad breath or a foul taste in your mouth, specifically originating from the implant area, can signal a bacterial infection [1]. Our article on Bad Breath from Dental Implants: Causes & Solutions 2026 provides more insights.
- Gum Recession: If the gum tissue around the implant appears to be receding, exposing more of the implant post or abutment, this could indicate bone loss or gum inflammation [1].
- Implant Mobility: Any feeling that the implant or its crown is loose or wobbly is a serious sign of potential implant failure and requires immediate dental attention [1, 8]. This is a late-stage symptom, and by this point, intervention is urgent.
- Difficulty Chewing or Biting: If chewing food becomes painful or difficult on the side of the implant, it could be due to pain, a loose component, or an improper bite [4].
- Changes in Bite: A feeling that your bite has changed, or that the implant crown feels “high” or different when you close your mouth, can indicate a mechanical issue with the crown or abutment [4].
- Pus or Discharge: The presence of pus or any discharge from the gum tissue around the implant is a clear sign of infection and requires immediate evaluation [1].
If you notice any of these symptoms, especially if they are persistent or worsening, do not delay seeking professional dental care. Early intervention is crucial for diagnosing the specific cause of implant discomfort years later and implementing the most effective treatment plan, often preventing the need for more complex or costly procedures, like revision dental implant surgery in Dallas.
Diagnosing Implant Discomfort Years Later
Diagnosing implant discomfort years later typically involves a comprehensive dental examination, including visual inspection, probing around the implant, and advanced imaging such as X-rays or 3D scans, to pinpoint the underlying cause [7]. A thorough diagnostic process is essential to differentiate between various issues, from infection to mechanical complications, ensuring the correct treatment plan is developed.
Diagnostic Steps:
- Clinical Examination: Your dentist in Dallas will visually inspect the implant site, looking for signs of inflammation, swelling, redness, gum recession, or pus. They will also assess your bite and look for any looseness in the crown or abutment [7].
- Periodontal Probing: A specialized probe is gently used around the implant to measure the depth of the gum pockets. Increased pocket depths can indicate inflammation or bone loss, similar to how gum disease is diagnosed around natural teeth. Bleeding upon probing is also a key indicator of inflammation [7].
- Radiographic Evaluation (X-rays and 3D Scans):
- X-rays: Conventional dental X-rays are crucial for assessing the bone level around the implant. A significant change in bone level compared to previous X-rays (taken when the implant was healthy) strongly suggests peri-implantitis or other bone-related issues [7].
- 3D Cone Beam Computed Tomography (CBCT): For more complex cases, a 3D CBCT scan provides a detailed, three-dimensional view of the implant, surrounding bone, and adjacent anatomical structures. This can help identify subtle bone loss, implant fractures, nerve impingement, or issues with the sinus cavity that might not be visible on standard X-rays. Many Dallas TX dentists use 3D guided implant surgery in 2026 and also for diagnostics.
- Bite Analysis: Your dentist will evaluate your bite using articulating paper to identify any premature contacts or excessive force being placed on the implant, which can contribute to discomfort or mechanical issues [4].
- Review of Medical History: Your dentist will review your complete medical history, including any systemic conditions (like diabetes) or medications that might impact oral health or implant success [2]. Smoking, for instance, is a significant risk factor for peri-implantitis.
- Patient Symptoms and History: A detailed discussion about your symptoms—when they started, how severe they are, and what makes them better or worse—is vital for diagnosis.
By combining these diagnostic tools, your dental professional can accurately identify the cause of implant discomfort years later and develop a targeted treatment strategy. If you are experiencing discomfort, do not hesitate to schedule a consultation with a dentist experienced in dental implant care.
Treatment Options for Late-Onset Implant Discomfort
Treatment options for late-onset implant discomfort vary widely depending on the underlying cause and severity, ranging from non-surgical interventions like professional cleanings and antibiotics to surgical procedures for more advanced cases [7]. The primary goal of treatment is to eliminate the source of discomfort, preserve the implant, and restore optimal oral health.
Non-Surgical Treatments:
- Enhanced Oral Hygiene: For early-stage peri-implant mucositis (inflammation of the gums around the implant without bone loss), meticulous professional cleaning and instructions for improved at-home oral hygiene are often sufficient. This may involve specialized tools to clean around the implant gently.
- Antibiotics: Depending on the severity of infection, your dentist might prescribe oral antibiotics or apply local antibiotic gels directly to the infected area around the implant [7]. This helps to reduce bacterial load.
- Deeper Cleaning (Debridement): In cases of mild peri-implantitis, a deep cleaning, or debridement, can remove plaque and calculus from the implant surface, combined with antiseptic rinses.
- Occlusal Adjustment/Night Guard: If excessive biting forces (bruxism or misaligned bite) are causing the discomfort, adjustments to the implant crown or the fabrication of a custom night guard can alleviate pressure on the implant and surrounding bone [4].
- Repair or Replacement of Components: If the issue is a loose or fractured abutment or crown, the dentist can often tighten or replace these components, resolving the discomfort [4].
Surgical Treatments:
- Debridement and Detoxification with Access Surgery: For more advanced peri-implantitis where non-surgical methods are insufficient, a minor surgical procedure might be necessary. This involves lifting the gum tissue to gain direct access to the implant surface for thorough cleaning and detoxification, removing all bacterial biofilm [7].
- Bone Grafting: If significant bone loss has occurred around the implant due to peri-implantitis, bone grafting procedures may be performed alongside debridement to regenerate lost bone support and stabilize the implant [7]. This is often combined with guided tissue regeneration membranes.
- Implant Surface Decontamination: Various methods, including laser therapy, air-abrasive devices, or specific chemical agents, can be used to thoroughly decontaminate the implant surface to promote healing and re-integration.
- Explant (Implant Removal) and Revision: In severe cases where the implant has failed, is highly mobile, or has caused extensive bone loss that cannot be salvaged, the implant may need to be removed. After a healing period, and potentially further bone grafting, a revision dental implant surgery Dallas might be considered [9].
The key to successful treatment for implant discomfort years later is prompt action. Ignoring the symptoms can lead to progressive bone loss and ultimately implant failure, requiring more invasive and costly interventions. Regular check-ups with your dentist, especially if you have dental implants in Dallas, are vital for early detection and prevention.
Preventing Late-Onset Implant Discomfort
Preventing late-onset implant discomfort hinges primarily on consistent, excellent oral hygiene practices, regular dental check-ups, and addressing lifestyle factors that can impact implant health. Proactive care is the most effective strategy for ensuring the long-term success and comfort of your dental implants.
Essential Prevention Strategies:
- Maintain Exemplary Oral Hygiene: This is paramount. Brush at least twice a day with a soft-bristled brush, paying special attention to the areas around your implants. Floss daily, using dental floss or interdental brushes designed for implants, to remove plaque and food particles from hard-to-reach areas. Water flossers can also be beneficial [1]. Our guide on Mini Implant Denture Maintenance Guide for 2026 has applicable tips for all implants.
- Regular Dental Check-ups and Cleanings: Schedule routine appointments with your dentist or dental hygienist, typically every six months, or more frequently if recommended. These visits allow your dental team to professionally clean around your implants, monitor your oral health, and detect any early signs of issues like peri-implantitis before they become serious [1, 7]. For optimal care, refer to our Optimal Dental Implant X-Ray Frequency: Your 2026 Guide to ensure proper monitoring.
- Address Bruxism (Teeth Grinding/Clenching): If you grind or clench your teeth, especially at night, discuss this with your dentist. They may recommend a custom-fitted night guard to protect your implants and natural teeth from excessive forces that can lead to discomfort or damage [4].
- Avoid Harmful Habits: Refrain from smoking or using tobacco products, as they significantly increase the risk of peri-implantitis and implant failure [1]. Also, avoid chewing on hard objects like ice, pens, or fingernails, which can put undue stress on your implants.
- Manage Systemic Health Conditions: Conditions like diabetes can impact healing and increase the risk of infection. If you have a systemic health condition, ensure it is well-managed, and inform your dentist about any changes in your health or medications [2]. See our guide on Diabetic Dental Implant Recovery: Guide & Timeline (2026).
- Maintain a Healthy Diet: A balanced diet supports overall health, including oral health, and can aid in gum tissue integrity and bone health.
By adhering to these preventative measures, individuals with dental implants in Dallas can significantly reduce their risk of experiencing implant discomfort years later and enjoy the long-term benefits of their tooth replacement options. Prevention is always more effective and less costly than treating complications.
The Importance of Early Intervention for Implant Discomfort Years Later
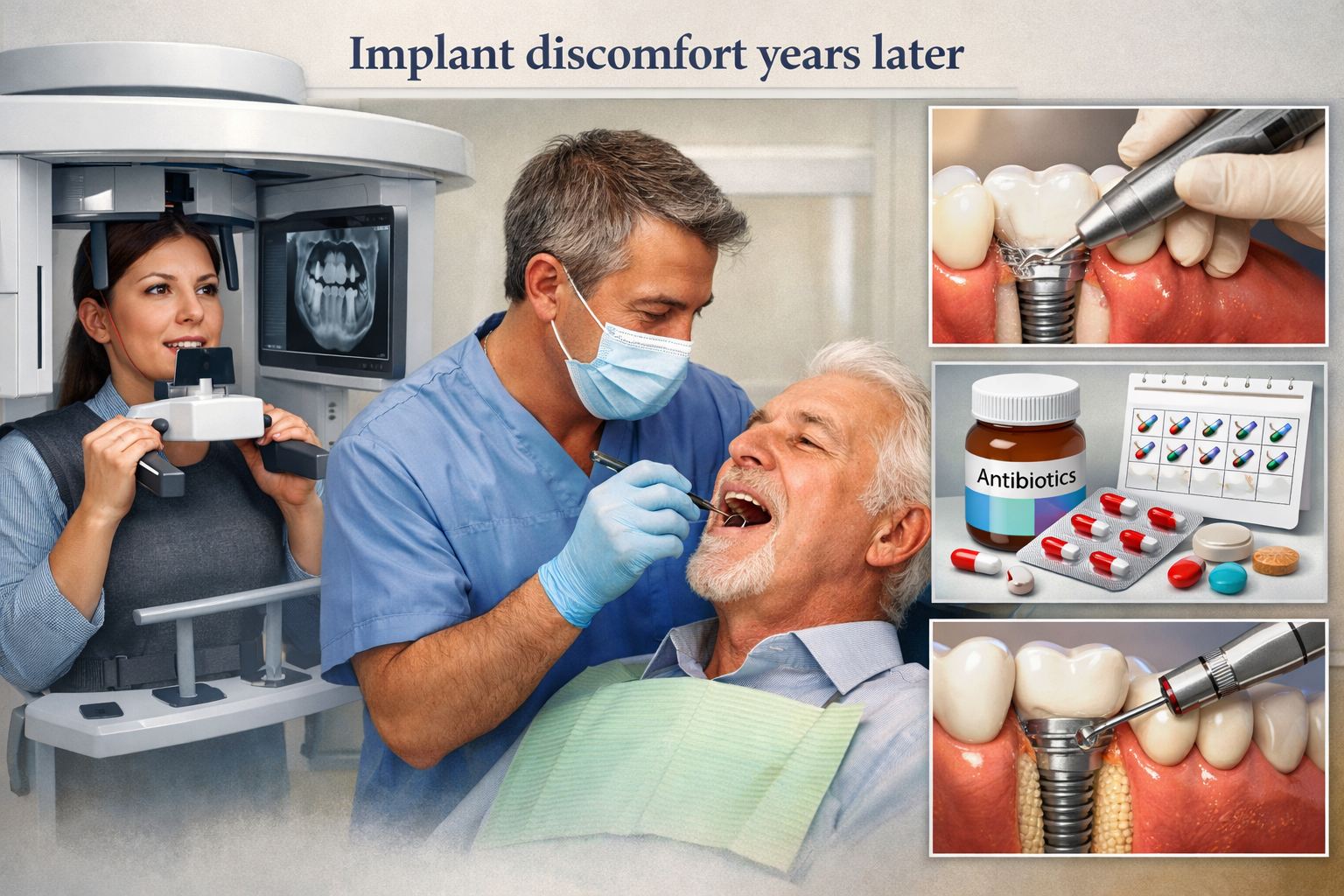
Early intervention for implant discomfort years later is paramount because it dramatically increases the likelihood of successfully treating the underlying issue, preserving the implant, and preventing more complex and costly complications, including potential implant failure [7, 8]. Ignoring persistent symptoms allows conditions like peri-implantitis to progress, making treatment more challenging and unpredictable.
Why Early Intervention Matters:
- Higher Success Rates for Treatment: When issues like peri-implantitis are caught in their early stages (e.g., peri-implant mucositis), non-surgical treatments like professional cleaning and improved oral hygiene are often highly effective in resolving the inflammation and preventing bone loss [7]. If significant bone loss has already occurred, surgical interventions become necessary, and their success can be less predictable.
- Prevention of Bone Loss: Peri-implantitis directly leads to bone loss around the implant [1]. Once bone is lost, it can be difficult and sometimes impossible to regenerate it fully. Early intervention aims to halt this process, protecting the structural integrity of the implant.
- Preserving the Implant: Addressing discomfort promptly can prevent the situation from escalating to the point where the implant becomes unstable or mobile. An unstable implant is at high risk of failure and often needs to be removed [8]. Early treatment gives the implant the best chance of remaining a functional part of your smile.
- Avoidance of More Invasive Procedures: Catching and treating issues early can often negate the need for more invasive and expensive procedures, such as advanced surgical debridement, bone grafting, or ultimately, implant removal and revision dental implant surgery Dallas.
- Reduced Discomfort and Improved Quality of Life: Prompt treatment alleviates pain and discomfort, restoring your ability to chew and speak comfortably. Living with chronic implant discomfort can significantly impact your quality of life.
- Cost-Effectiveness: Treating a problem in its early stages is almost always less expensive than addressing a full-blown complication or replacing a failed implant. For example, peri-implantitis treatment costs in Dallas 2026 for early stages may be significantly less than for advanced cases requiring complex surgery.
If you suspect you have implant discomfort years later, especially if accompanied by symptoms like bleeding, swelling, or changes in your bite, contact your dental professional in Dallas immediately. Your long-term oral health depends on it.
When to See a Dentist for Implant Discomfort Years Later
You should see a dentist immediately if you experience any new or persistent discomfort, pain, swelling, or unusual sensations around your dental implant years after it has healed, as these symptoms are not normal and indicate an underlying issue requiring professional evaluation [4, 7]. Prompt consultation is critical to diagnose the problem early and initiate effective treatment.
Do not delay seeking professional advice if you notice any of the following:
- Persistent pain or tenderness that doesn’t go away.
- Swelling or redness of the gums around the implant.
- Bleeding when you brush or floss around the implant.
- A bad taste in your mouth or persistent bad breath coming from the implant area.
- Gum recession, exposing more of the implant.
- Any mobility or looseness of the implant itself or the crown attached to it.
- Changes in your bite or difficulty chewing.
- Pus or discharge from the implant site.
Even if the discomfort is mild, it’s essential to have it checked. Early signs of complications like peri-implantitis can often be managed with less invasive treatments. Waiting until symptoms become severe or the implant becomes mobile can lead to more extensive and costly interventions, potentially including the removal and replacement of the implant. For residents of Dallas, Texas, seeking professional care for missing teeth solutions and long-term implant maintenance is crucial for optimal oral health.
Frequently Asked Questions About Implant Discomfort Years Later
Q1: Is it normal for a dental implant to hurt years after placement?
No, it is not normal for a dental implant to hurt years after placement. Once an implant has fully healed and integrated, it should feel stable and comfortable. New or persistent discomfort indicates an underlying problem that requires dental evaluation [4].
Q2: What is peri-implantitis?
Peri-implantitis is a serious inflammatory condition that affects the gum tissue and bone surrounding a dental implant, similar to gum disease around natural teeth. It’s often caused by bacterial infection and can lead to bone loss and potential implant failure if left untreated [1, 7].
Q3: Can a loose crown or abutment cause implant discomfort years later?
Yes, a loose crown or abutment (the connector between the implant and the crown) can definitely cause discomfort, instability, and an improper bite, leading to pain years after the implant was placed [4].
Q4: What are the main symptoms of peri-implantitis?
Key symptoms of peri-implantitis include persistent pain, swelling, bleeding gums around the implant, gum recession, pus, and eventually, implant mobility [1, 7, 8].
Q5: Can teeth grinding (bruxism) affect my dental implant years later?
Yes, excessive force from teeth grinding or clenching (bruxism) can place undue stress on your dental implant, potentially leading to pain, bone loss, or damage to the implant components over time [4]. A night guard can often help.
Q6: What should I do if my implant feels loose after several years?
If your dental implant feels loose after several years, you should contact your dentist immediately. Implant mobility is a significant sign of potential implant failure and requires urgent professional assessment [1, 8].
Q7: Are dental implants prone to infection years later?
Dental implants are generally resistant to decay, but they can be prone to bacterial infections like peri-implantitis, especially with poor oral hygiene or certain risk factors [1, 7]. This can occur years after placement.
Q8: What kind of dental professional should I see for implant discomfort?
You should see a general dentist initially, who may then refer you to a periodontist (a gum specialist) or an oral surgeon, as these specialists have extensive experience in diagnosing and treating implant-related complications.
Q9: Can implant discomfort be a sign of nerve damage?
While nerve damage is more commonly a concern shortly after surgery, it can sometimes manifest with delayed symptoms or be irritated by an implant if it’s placed too close to a nerve [1]. A comprehensive diagnostic evaluation can determine this.
Q10: How much does it cost to fix implant discomfort in Dallas?
The cost to fix implant discomfort in Dallas varies widely depending on the cause and severity. Simple adjustments or cleanings may be minimal, while treating peri-implantitis can range from a few hundred to several thousand dollars, especially if bone grafting or revision surgery is needed. For specific cost estimates, a consultation with a dentist is essential.
Q11: Can my dental implant be saved if I have discomfort years later?
In many cases, yes, especially if the issue is caught early. Non-surgical and surgical treatments are available to address infections, mechanical issues, and bone loss, often allowing the implant to be saved [7].
Q12: How often should I get X-rays for my dental implants?
Your dentist will recommend a schedule, but typically, regular check-ups including X-rays every 1-3 years are advised to monitor the bone level around your implants and detect issues early. Refer to our Optimal Dental Implant X-Ray Frequency: Your 2026 Guide for more information.
Conclusion
Experiencing implant discomfort years later can be a concerning development for anyone with dental implants. However, it’s crucial to remember that this discomfort is rarely normal and almost always indicates an underlying issue that requires professional attention. From peri-implantitis, a common long-term infection, to mechanical problems with the crown or abutment, various factors can contribute to late-onset pain or instability.
The key to successfully addressing implant discomfort lies in early detection and intervention. Paying close attention to warning signs such as persistent pain, swelling, bleeding, bad breath, or any noticeable mobility around your implant is vital. If you reside in Dallas, Texas, and notice any of these symptoms, do not hesitate to schedule a consultation with a dentist experienced in dental implant procedures. A thorough examination, including advanced imaging, can accurately diagnose the problem and guide the most effective treatment plan, ranging from simple adjustments and improved oral hygiene to more involved surgical procedures.
By prioritizing regular dental check-ups, maintaining diligent oral hygiene, and promptly addressing any new discomfort, you can significantly enhance the long-term health and success of your dental implants, ensuring they continue to provide a stable and comfortable foundation for your smile for many years to come. Your long-term oral health is our priority at Dental Implant Education – Dallas TX.
References
[1] Side Effects Of Dental Implants – https://www.magnoliadentistry.com/blog/side-effects-of-dental-implants/
[2] Long Term Side Effects Of Dental Implants – https://mcandental.com/blog/long-term-side-effects-of-dental-implants/
[3] Long Term Side Effects Of Dental Implants What To Expect – https://www.signaturesmilesdentalgroup.com/long-term-side-effects-of-dental-implants-what-to-expect/
[4] Why Does My Tooth Implant Hurt Years Later – https://madisondentalny.com/why-does-my-tooth-implant-hurt-years-later/
[5] How Long Do Dental Implants Hurt – https://www.ufbergdental.com/how-long-do-dental-implant-hurt
[6] Dental Implant Discomfort What It Could Be Telling You – https://www.barclayfamilydental.com/dental-implant-discomfort-what-it-could-be-telling-you
[7] Common Complications Of Dental Implants – https://torrancedentalspa.com/common-complications-of-dental-implants/
[8] Dental Implant Risks Complications In 2026 – https://www.oceanicdental.com/resource/dental-implant-risks-complications-in-2026
[9] Can Dental Implants Cause Problems Years Later – https://abadindental.com/can-dental-implants-cause-problems-years-later/


Leave a Reply
Share your thoughts or ask a question about dental implants. Your email address will not be published.