When considering permanent solutions for missing teeth, dental implants often emerge as a leading choice, praised for their stability and natural look. However, not everyone is an immediate candidate for this advanced tooth replacement option. The crucial first step is understanding how dentists evaluate implant candidacy to ensure a successful, long-lasting outcome. This comprehensive guide from Dental Implant Education – Dallas TX will walk you through the detailed assessment process that dental professionals undertake to determine if dental implants are right for you in 2026, focusing on ensuring patient safety and promoting long-term oral health.
Key Takeaways
- Dentists conduct a thorough evaluation of your oral health, jawbone structure, and overall medical history to determine implant candidacy.
- Adequate bone quality and quantity in the jaw are paramount for successful implant integration, often requiring 3D imaging for precise assessment.
- Active gum disease or other oral infections must be treated and resolved before any implant surgery can proceed.
- While certain medical conditions or medications can impact candidacy, many patients with controlled health issues can still receive dental implants with proper planning.
- A consultation with a dentist specializing in dental implants is essential to receive a personalized assessment and discuss all tooth replacement options.
Quick Answer
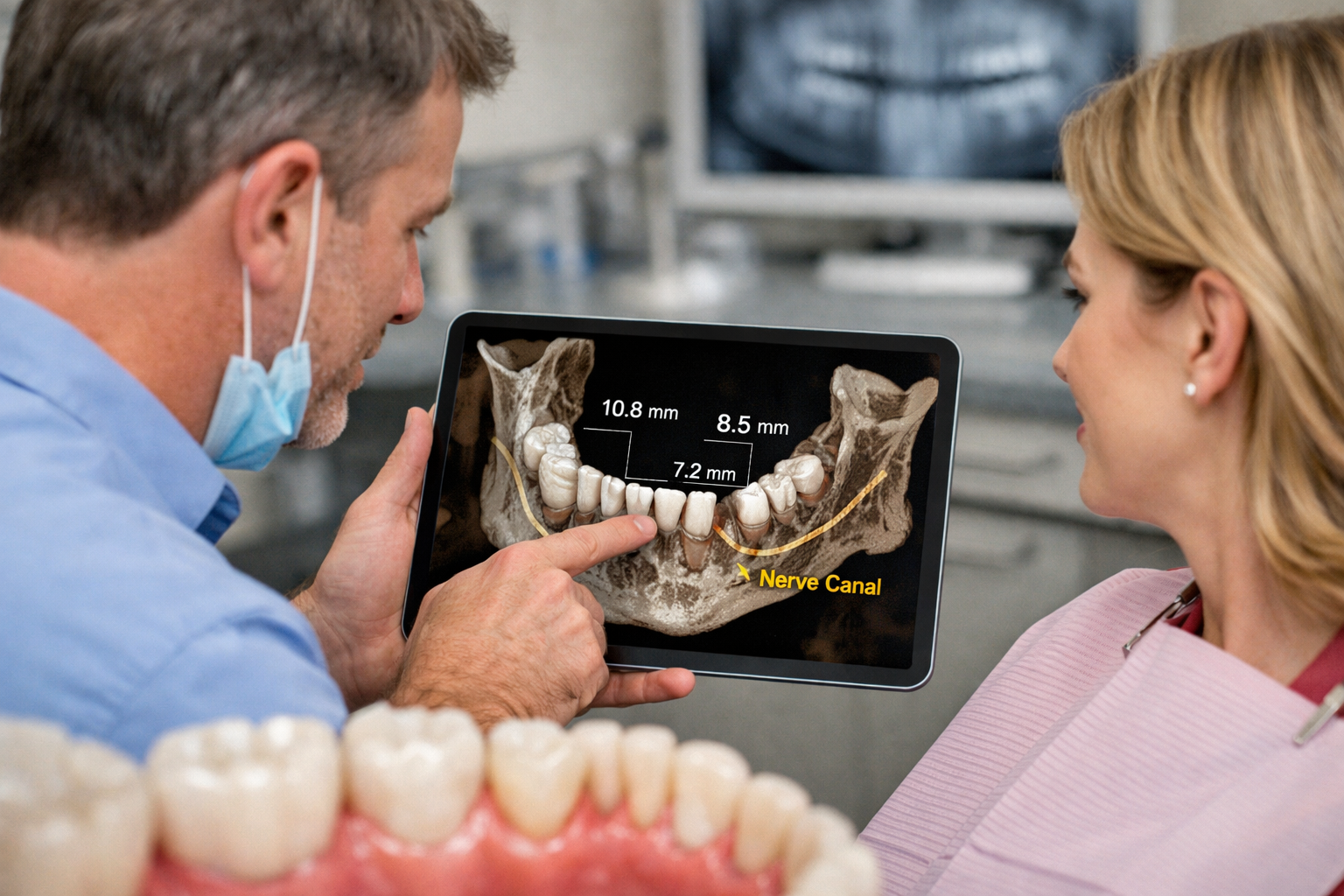
Dentists evaluate implant candidacy through a comprehensive assessment that includes reviewing your oral health, examining your jawbone structure using advanced imaging, and thoroughly assessing your general medical history. This multi-faceted approach ensures that the foundation for the implant—your jawbone and gums—is healthy enough to support the implant and that your body can heal properly after the implant surgery process [1, 3]. Factors like bone density, gum health, and systemic conditions like diabetes are carefully considered to maximize the success and longevity of your dental implants in Dallas [1, 2, 3].
What Oral Health Factors Do Dentists Assess for Implant Candidacy?
Dentists rigorously assess several key oral health factors to determine if a patient is a suitable candidate for dental implants, primarily focusing on the health of the gums and any existing dental issues. A healthy oral environment is fundamental because active gum disease and other infections can compromise the success of implant integration and long-term stability [1, 3].
First and foremost, dentists look for signs of periodontal (gum) disease. Active gum disease is a significant contraindication for immediate implant placement [1]. This is because the bacteria associated with gum disease can lead to peri-implantitis, an inflammatory condition around dental implants that can cause bone loss and implant failure [3]. Therefore, if gum disease is present, it must be thoroughly treated and brought under control before implant surgery can be considered [1]. This treatment process might involve deep cleanings, antibiotics, or even surgical interventions, and it can take several months of maintenance therapy (typically 3-6 months) to achieve the necessary stable gum health [3].
Beyond gum health, dentists will also examine:
- Presence of infection: Any active infections in the mouth, such as abscesses or severe decay in adjacent teeth, must be resolved prior to implant placement to prevent contamination of the surgical site [1].
- Remaining teeth: The overall condition of your remaining teeth is assessed. If there are other significant dental issues, these may need to be addressed first to create a stable oral environment.
- Oral hygiene habits: Your commitment to excellent oral hygiene is crucial for the long-term success of dental implants [1]. Dentists will review your brushing and flossing routines and provide guidance on maintaining optimal oral health. Patients who struggle with consistent oral hygiene may face a higher risk of complications.
If you have underlying oral health issues, it does not necessarily disqualify you from receiving dental implants; rather, it means these issues must be addressed first. For example, if you have chronic gum inflammation, a period of dedicated periodontal treatment will be required before your dentist in Dallas can proceed with evaluating the next steps for your dental implant procedure.
How Does Jawbone Health Influence Dental Implant Candidacy?
Jawbone health is arguably the single most critical factor in determining dental implant candidacy, as the implant post fuses directly with the bone in a process called osseointegration [1, 3]. Dentists must ensure there is sufficient bone volume and quality to securely anchor the implant.
To assess jawbone health, dentists utilize advanced imaging techniques, primarily 3D Cone Beam Computed Tomography (CBCT) scans [1, 3]. Unlike traditional X-rays, a CBCT scan provides a detailed, three-dimensional view of your jawbone, allowing the dentist to measure precise bone dimensions, including height, width, and density [1, 3]. This imaging is essential for:
- Measuring bone quantity: The scan reveals the actual amount of bone available at the implant site. For standard implants, minimum measurements often required include 10mm of jawbone height and 5mm of width in the lower jaw [3]. The bone height must also be adequate from the top of the ridge to critical anatomical structures like nerves or sinus cavities [1].
- Assessing bone quality: Beyond volume, the density and overall health of the bone are crucial. High-quality bone provides a strong foundation for the implant, promoting successful fusion.
- Identifying vital structures: The CBCT scan precisely locates nerves (like the inferior alveolar nerve in the lower jaw) and sinus cavities in the upper jaw [1, 3]. This information is vital for surgical planning to avoid damage to these structures during the implant surgery process.
- Detecting bone loss: Over time, when a tooth is lost, the jawbone in that area can resorb or shrink [2]. The CBCT scan clearly shows areas where bone volume is insufficient, indicating the need for a bone graft [3].
If the jawbone is found to be deficient in height, width, or density, patients are not immediately disqualified from dental implants. Instead, procedures like bone grafting or sinus lifts may be recommended to augment the bone and create a suitable foundation for the implant [1]. These procedures involve adding bone material (either from your own body, a donor, or synthetic sources) to the deficient area, which then heals and integrates with your natural bone over several months. For instance, if you’ve been missing a back tooth in your upper jaw for a while, a sinus lift might be necessary to provide enough bone to support a dental implant without encroaching on the sinus cavity. For more information on healing, see our guide on Bone Graft Healing for Dental Implants: Your 2026 Timeline.
How Does Overall Health and Lifestyle Affect Implant Candidacy?
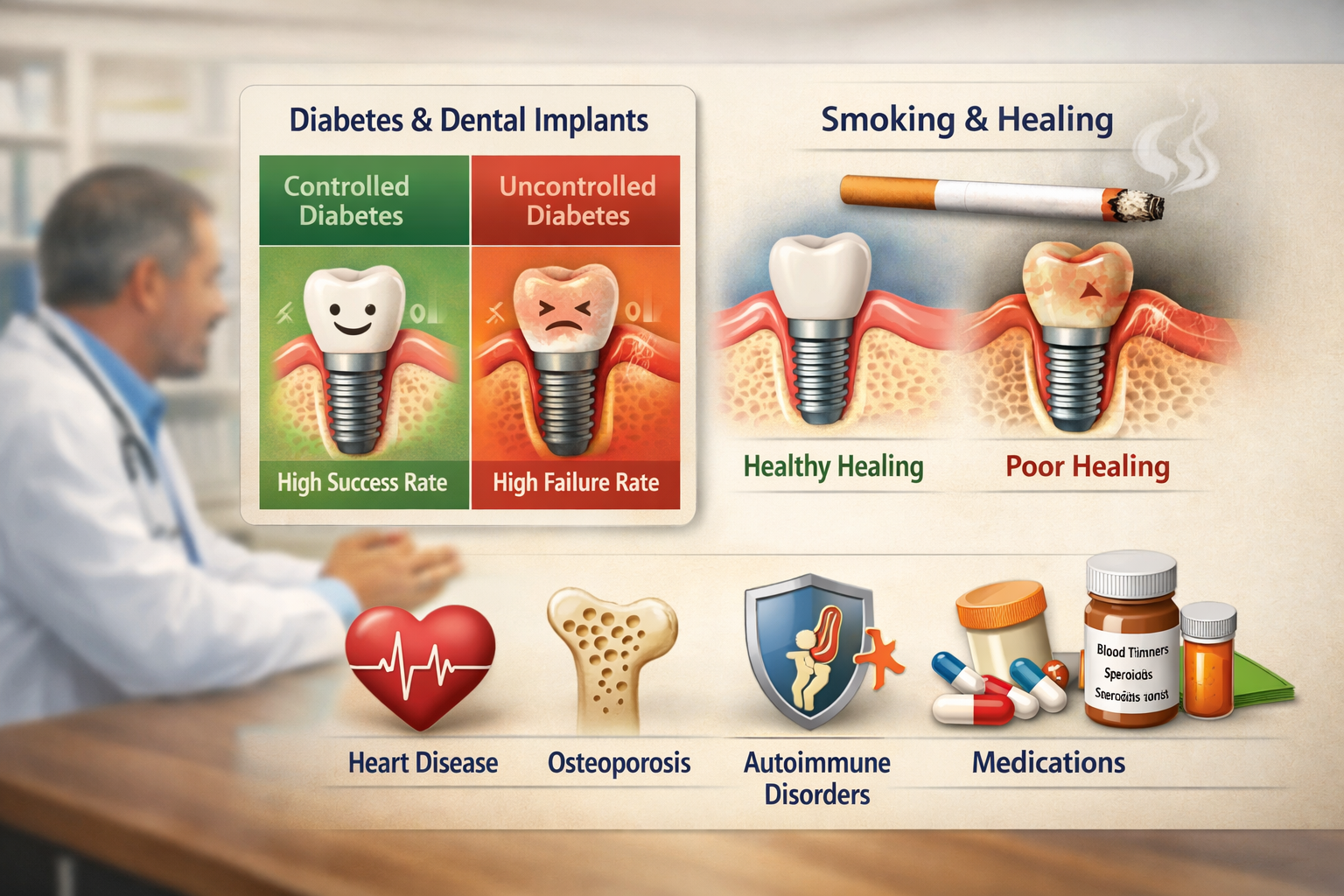
Beyond oral health, a patient’s overall medical history and lifestyle choices play a significant role in determining dental implant candidacy. Dentists perform a thorough review to identify any systemic conditions or habits that could impact the success of the implant surgery and healing process [3].
Medical Conditions
Many chronic conditions do not automatically disqualify patients but require careful management and communication with both your dentist and primary care physician [1, 3].
- Diabetes: Well-controlled diabetes is generally compatible with dental implants. The key is maintaining blood sugar levels within target ranges, as uncontrolled diabetes can impair healing and increase the risk of infection [1, 3]. Patients with well-controlled diabetes can often be excellent candidates [1]. Our article, Navigating Diabetic Dental Implant Recovery: A Comprehensive Guide for 2026, offers more specific guidance.
- Heart Disease: Patients with certain heart conditions or those taking blood thinners may require special considerations. Your dentist will consult with your cardiologist to ensure the procedure can be performed safely, potentially adjusting medication regimens temporarily [1].
- Immunocompromised Conditions: Conditions that weaken the immune system can increase the risk of infection and slow healing. A thorough discussion with your medical team is crucial.
- Osteoporosis: While osteoporosis itself isn’t always a contraindication, certain medications for osteoporosis, specifically bisphosphonates, can affect bone healing and may increase the risk of osteonecrosis of the jaw [1]. Your dentist will carefully evaluate your medication history.
- Radiation Therapy: Patients who have undergone radiation therapy to the head and neck area may have compromised bone quality and reduced blood supply, requiring a more cautious approach and sometimes specialized protocols.
Medications
A comprehensive list of all medications, including over-the-counter drugs, supplements, and prescription medications, is essential. Some medications, such as certain antidepressants, heartburn medications, or corticosteroids, can potentially affect bone metabolism or healing [3]. Blood thinners are particularly important to note as they can increase bleeding risk during surgery. Your dentist will assess these and coordinate with your physician if any adjustments are needed before the dental implant procedure.
Lifestyle Habits
- Smoking: Smoking significantly reduces the success rate of dental implants [1, 3]. It impairs blood flow, compromises the immune system, and slows down the healing process, making osseointegration less predictable. Dentists often strongly advise patients to quit smoking or at least reduce it substantially before and after implant surgery [3]. Smokers have a higher risk of developing peri-implantitis.
- Alcohol Consumption: Excessive alcohol consumption can also impede healing and overall health, potentially affecting implant success.
- Bruxism (Teeth Grinding): Chronic teeth grinding or clenching can place excessive force on dental implants, especially during the healing phase, potentially leading to implant failure. Patients with bruxism may require a nightguard or other interventions to protect their new implants [1].
In conclusion, understanding how dentists evaluate implant candidacy involves a holistic review of your health. A well-controlled chronic condition often means you are still a candidate, but meticulous planning and coordination between your dental and medical teams are paramount. It’s about ensuring your body is in the best possible condition to support and heal around the new dental implants.
| Medical Condition | Impact on Implant Candidacy | Considerations for Treatment |
|---|---|---|
| Well-Controlled Diabetes | Generally good candidate | Maintain blood sugar levels within target range [1] |
| Uncontrolled Diabetes | Increased risk of infection & poor healing | Requires medical management before surgery [1] |
| Osteoporosis (no bisphosphonates) | Often good candidate | Bone density may be a factor; imaging is crucial [1] |
| Osteoporosis (on bisphosphonates) | Potential risk of osteonecrosis of the jaw | Thorough review with physician required; alternative treatments may be explored [1] |
| Active Gum Disease | Not a candidate until treated | Must be fully treated and stable before implants [1, 3] |
| Heavy Smoking | Increased risk of failure, poor healing | Strong recommendation to quit or significantly reduce smoking [1, 3] |
| Heart Disease (well-managed) | Often good candidate with physician clearance | May require temporary medication adjustments; careful monitoring [1] |
| Immunocompromised Conditions | Increased risk of infection | Requires close consultation with medical specialists [1] |
What Diagnostic Imaging and Tools Do Dentists Use?
Dentists rely on a range of advanced diagnostic imaging and tools to meticulously evaluate implant candidacy, providing a detailed understanding of the patient’s oral anatomy and underlying bone structure [1, 3]. This precision is vital for effective treatment planning and to maximize the success of dental implants in Dallas.
The most critical diagnostic tool is the 3D Cone Beam Computed Tomography (CBCT) scan [1, 3]. Unlike traditional 2D X-rays that offer a flat image, a CBCT scan provides high-resolution, three-dimensional views of the jawbone, teeth, and surrounding anatomical structures. This allows dentists to:
- Precisely measure bone dimensions: This includes the height, width, and density of the jawbone at the proposed implant site. Accurate measurements are crucial because implants require a specific amount of healthy bone to integrate successfully [1, 3].
- Map critical structures: The scan clearly shows the exact location of vital nerves (such as the inferior alveolar nerve in the lower jaw) and sinus cavities in the upper jaw [1, 3]. This information is essential for avoiding damage to these structures during implant surgery, which is a key aspect of patient safety.
- Identify bone deficiencies: The CBCT scan highlights areas where bone loss has occurred, indicating whether bone grafting or a sinus lift procedure might be necessary before implant placement [3].
- Assess bone quality: The scan helps evaluate the density and architecture of the bone, which influences the type of implant and surgical technique used.
In addition to CBCT scans, dentists may also utilize:
- Panoramic X-rays: These provide a broad view of the entire mouth, including all teeth, jaws, and surrounding structures. While not as detailed as CBCT, they offer a good initial overview.
- Periapical X-rays: These focus on individual teeth and their roots, helping to assess the health of adjacent teeth and the bone immediately surrounding them.
- Intraoral Cameras: These allow the dentist to capture detailed images of the gums and teeth, aiding in the assessment of oral hygiene and soft tissue health.
- Dental Models/Impressions: Physical or digital impressions of your teeth and jaws help the dentist plan the precise positioning of the implant and the design of the final crown or prosthesis.
- Treatment Planning Software: Dentists use specialized software to analyze the CBCT data, virtually place implants, and simulate the surgical procedure. This allows for highly accurate planning, ensuring optimal implant placement and predictable outcomes.
By combining these advanced diagnostic tools with a thorough clinical examination, dentists gain a comprehensive understanding of your oral health and jawbone structure. This detailed evaluation allows them to determine how dentists evaluate implant candidacy for your unique situation, craft a personalized treatment plan, and discuss all available missing teeth solutions, including the potential costs involved (e.g., Demystifying Dental Implant Costs: A 2025 Guide to Average Prices & Value).
What if I Don’t Meet All the Candidacy Criteria? Are There Alternatives or Solutions?
If your initial assessment reveals that you don’t meet all the standard criteria for dental implants, it doesn’t necessarily mean you can’t get them or that you’re out of options. Dentists are often able to address deficiencies through adjunctive procedures or propose alternative tooth replacement options [1].
Solutions to Address Candidacy Issues
- Bone Grafting: This is a common solution for insufficient jawbone density or volume [1]. If the CBCT scan shows you lack the necessary bone height or width, a bone graft can augment the area. This involves placing bone material (from your own body, a donor, or synthetic sources) into the deficient site, which then integrates with your natural bone over several months (typically 3-9 months). Once the graft has healed and created sufficient bone, the dental implant procedure can proceed [3].
- Sinus Lift: Specifically for the upper jaw, if the maxillary sinuses are too close to the implant site due to bone loss, a sinus lift procedure may be performed [3]. This involves gently lifting the sinus membrane and placing bone graft material underneath it, creating a new, stable floor for implant placement.
- Gum Disease Treatment: If active gum disease is present, it must be treated and resolved before any implant surgery [1]. This might involve scaling and root planing, antibiotic therapy, or periodontal surgery. Once the gums are healthy and stable (often after 3-6 months of maintenance therapy), implant placement can be re-evaluated [3].
- Medication Adjustments/Medical Management: For patients with certain medical conditions or on specific medications, your dentist will collaborate with your primary care physician or specialist. This might involve temporarily adjusting medication dosages (e.g., blood thinners), ensuring conditions like diabetes are well-controlled, or obtaining medical clearance before surgery [1].
- Smoking Cessation: For smokers, the most impactful solution is to quit or significantly reduce smoking [1]. This dramatically improves healing capabilities and the long-term success rate of dental implants.
Alternative Tooth Replacement Options
If, even after considering adjunctive procedures, dental implants are not feasible or desired, your dentist in Dallas can discuss other effective tooth replacement options:
- Dental Bridges: A dental bridge uses adjacent healthy teeth as anchors to support a prosthetic tooth that fills the gap [2]. While effective, it requires altering the healthy adjacent teeth and does not stimulate the jawbone, potentially leading to bone loss over time. You can learn more about costs at Dental Bridge vs. Implant Cost in 2025: Which Tooth Replacement Option is Right for Your Wallet and Your Smile?.
- Removable Partial or Complete Dentures: These are prosthetic devices that can replace one or more missing teeth (partial dentures) or an entire arch (complete dentures). Dentures are less stable than implants and may require adhesives, but they are a non-invasive and often more affordable option. For those considering dentures, but wanting added stability, implant-supported dentures are a hybrid option (see Unlocking Your Smile: What’s the Average Cost of Dental Implants for Dentures in 2025?).
- Mini Dental Implants: In cases of moderate bone loss, mini dental implants might be an option. These are smaller in diameter than traditional implants and are often used to stabilize dentures, though they may not be suitable for single tooth replacement in all cases.
The ultimate decision on the best course of action is made collaboratively between you and your dental professional after a thorough consultation with a dentist. It’s about finding the safest and most effective solution for your unique oral health education needs and long-term oral health goals.
What to Expect During Your Initial Dental Implant Consultation in Dallas
The initial consultation is a critical first step in exploring dental implants in Dallas. It’s an opportunity for your dentist to gather all necessary information and for you to have your questions answered, fostering informed decision-making about missing teeth solutions.
During this appointment, you can expect a thorough and personalized evaluation:
- Comprehensive Oral Examination: The dentist will perform a detailed visual inspection of your mouth, gums, and remaining teeth. They will look for signs of gum disease, decay, or other oral health issues that need to be addressed before implant consideration [3].
- Review of Medical and Dental History: You’ll be asked to provide a complete medical history, including any chronic conditions (like diabetes or heart disease), previous surgeries, current medications (prescription, over-the-counter, and supplements), and allergies. This also includes your dental history, outlining past treatments and any concerns you may have [1, 3].
- Diagnostic Imaging: Expect to have X-rays, and most importantly, a 3D Cone Beam CT (CBCT) scan [1, 3]. As discussed, this advanced imaging provides a detailed view of your jawbone, helping the dentist assess bone quantity, quality, and the location of vital structures like nerves and sinuses.
- Discussion of Treatment Goals and Expectations: Your dentist will listen to your concerns, understand your aesthetic and functional goals for tooth replacement, and discuss what you hope to achieve with dental implants [5]. This is where you can clearly communicate your needs.
- Assessment of Candidacy: Based on the clinical exam, medical history, and imaging, the dentist will determine if you are a suitable candidate for dental implants. They will explain how dentists evaluate implant candidacy specifically for your case, highlighting any potential challenges or necessary pre-procedures like bone grafting [1].
- Presentation of Treatment Options: If you are a candidate, the dentist will outline a personalized treatment plan, explaining the recommended dental implant procedure, including the number of implants, type of restoration, and any necessary preparatory steps. If implants aren’t suitable, they will discuss alternative tooth replacement options [2].
- Detailed Explanation of Process, Timeline, and Costs: You’ll receive a clear overview of the implant surgery process, the expected timeline from start to finish (which can range from a few months to over a year, depending on individual needs), and an estimate of the implant cost in Dallas [2, 5]. This is an ideal time to ask about various payment options and insurance coverage. For a deeper dive into financial aspects, consider reviewing Unpacking the Cost of Dental Implants in 2025: Your Complete Guide to a Confident Smile.
- Opportunity for Questions: This is your dedicated time to ask any questions you have about dental implants, the procedure, risks, benefits, and what to expect during recovery. Many patients find our guide on Essential Questions to Ask Your Dentist About Implants in 2026 very helpful.
The goal of this initial consultation is to provide you with a clear, factual understanding of your options, empowering you to make an informed decision about your long-term oral health without any pressure.
Why Choosing the Right Dental Implant Specialist Matters in Dallas
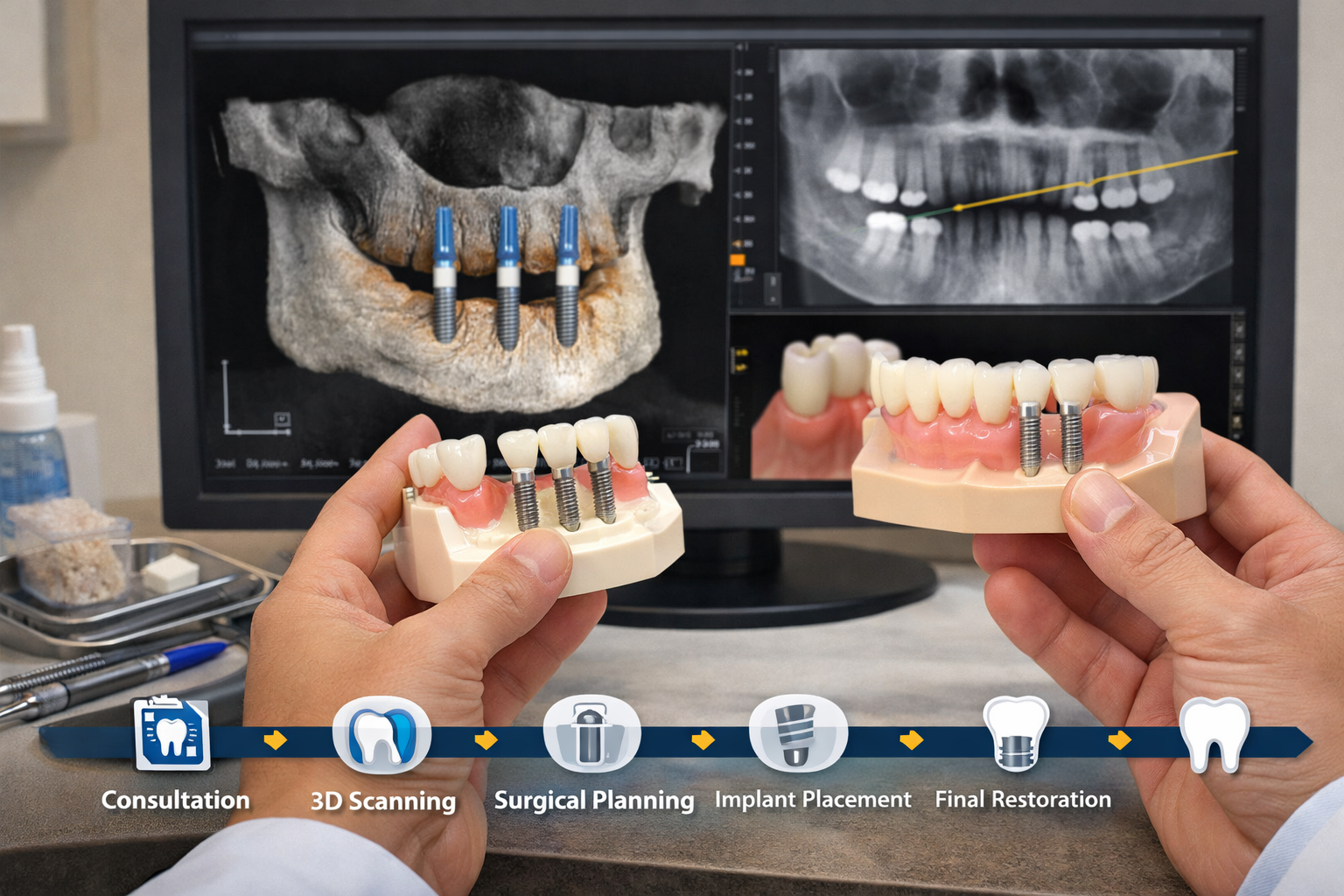
Choosing the right dental implant specialist in Dallas is paramount to the success and longevity of your dental implants. The expertise, experience, and specialized training of the dental professional performing your implant surgery can significantly impact the outcome, patient safety, and your overall experience.
Here’s why selecting an experienced specialist is crucial:
- Specialized Knowledge and Training: Dental implant placement is a complex surgical procedure that requires specialized training beyond general dentistry. Specialists like oral surgeons, periodontists, or prosthodontists have advanced education in dental implantology, including surgical techniques, bone grafting, and managing potential complications [1]. They understand the intricacies of jaw anatomy and how to integrate implants seamlessly.
- Accurate Candidacy Assessment: An experienced specialist excels at determining how dentists evaluate implant candidacy thoroughly. They are adept at interpreting advanced imaging like CBCT scans, accurately assessing bone quality and quantity, and identifying potential risks or complications from your medical history. Their ability to precisely plan the implant placement is superior, minimizing surprises during surgery [3].
- Minimizing Risks and Complications: While dental implant surgery is generally safe, complications can arise. A seasoned specialist is highly skilled at anticipating, preventing, and managing these issues, ensuring a smoother procedure and recovery. This expertise is crucial for patient safety.
- Advanced Technology and Techniques: Leading dental implant specialists invest in state-of-the-art technology, such as advanced 3D imaging, computer-guided implant surgery, and high-quality implant materials. This technology allows for more precise planning, predictable results, and often a less invasive procedure.
- Comprehensive Treatment Planning: The process of getting dental implants often involves multiple phases and may require adjunctive procedures like bone grafting. An expert specialist can orchestrate a comprehensive treatment plan, coordinating with other dental professionals if needed, to achieve the best possible long-term oral health outcome.
- Long-Term Success and Follow-Up: An experienced specialist is committed to the long-term success of your implants. They provide detailed post-operative care instructions, establish a proper follow-up schedule (see Dallas Dental Implant Follow-Up: Ensuring Lasting Smile Success), and are equipped to address any concerns that may arise years down the line.
When choosing a specialist for dental implants in Dallas, consider their credentials, years of experience with implant procedures, patient testimonials, and their approach to patient care and education. A transparent and patient-focused practice will always prioritize your understanding and comfort throughout the entire process. For further guidance, refer to our article on How to Choose a Dental Implant Dentist Near You | Expert Guide.
FAQ: How Dentists Evaluate Implant Candidacy
Q1: Is age a factor in dental implant candidacy?
A1: Age itself is generally not a disqualifying factor for dental implants; what matters most is your overall health, bone density, and oral health [1]. Healthy older adults can be excellent candidates.
Q2: Can I get dental implants if I have gum disease?
A2: No, active gum disease must be completely treated and controlled before dental implant surgery can proceed, as it can significantly increase the risk of implant failure [1, 3].
Q3: What if I don’t have enough jawbone for an implant?
A3: If you lack sufficient jawbone, procedures like bone grafting or a sinus lift can be performed to augment the bone and create a suitable foundation for the implant [1, 3].
Q4: Does smoking prevent me from getting dental implants?
A4: Smoking significantly reduces the success rate of dental implants and can lead to complications. While not an absolute disqualifier, dentists strongly advise quitting or reducing smoking to improve healing and long-term success [1, 3].
Q5: What medical conditions might affect my implant candidacy?
A5: Conditions like uncontrolled diabetes, certain heart conditions, or medications for osteoporosis (bisphosphonates) can affect candidacy. However, many chronic conditions, if well-managed, do not prevent implant placement [1, 3].
Q6: How long does the candidacy evaluation process take?
A6: The initial consultation, including examination and imaging, typically takes one visit. If pre-procedures like bone grafting or gum disease treatment are needed, those will extend the overall timeline before implant placement can begin [3].
Q7: Are dental implants painful?
A7: Dental implant surgery is typically performed under local anesthesia, often with sedation, meaning you should not feel pain during the procedure [1]. Discomfort after surgery is manageable with prescribed medication. You can learn more about managing pain in Demystifying Dental Implant Pain: Your 2025 Guide to a Confident Smile.
Q8: What is a 3D CBCT scan, and why is it important?
A8: A 3D Cone Beam CT (CBCT) scan provides a detailed, three-dimensional view of your jawbone, allowing the dentist to precisely measure bone volume and density, and map vital structures like nerves and sinuses, which is crucial for safe and accurate implant planning [1, 3].
Q9: What are the alternatives if I’m not a candidate for dental implants?
A9: Alternatives include dental bridges, removable partial or complete dentures, and sometimes mini dental implants, depending on your specific needs and oral health [2].
Conclusion
Understanding how dentists evaluate implant candidacy is a crucial step for anyone considering dental implants as a solution for missing teeth. This comprehensive assessment goes beyond a simple glance, delving into the intricate details of your oral health, jawbone structure, and overall medical well-being. From the meticulous analysis of gum health and bone density using advanced 3D imaging to a thorough review of your medical history and lifestyle, every factor is weighed to ensure the highest likelihood of long-term success and patient safety for your dental implants in Dallas.
While factors like active gum disease, insufficient bone, or uncontrolled systemic conditions might initially present challenges, many can be successfully addressed through adjunctive procedures like bone grafting or medical management. Ultimately, the goal of this detailed evaluation is to empower you with knowledge and guide you toward the most appropriate, safe, and effective tooth replacement options tailored to your unique needs. We encourage you to schedule a consultation with a qualified dental professional in Dallas to receive a personalized assessment and explore the path to a healthier, more confident smile.
References
[1] Dental Implant Candidate Eligibility – https://www.novaimplantfamilydentistry.com/dental-implant-candidate-eligibility/
[2] Are You A Candidate For Dental Implants Key Factors To Consider – https://www.mirrorlakedentistry.com/heartland/heartland-blog/are-you-a-candidate-for-dental-implants-key-factors-to-consider
[3] Dental Implant Candidacy Criteria – https://www.northwestoralsurgeons.com/blog/dental-implant-candidacy-criteria/
[4] Are You A Candidate For Dental Implants Key Factors To Consider – https://medicalartsdentistry.com/are-you-a-candidate-for-dental-implants-key-factors-to-consider/
[5] Determining Your Candidacy For Dental Implants – https://newburydentalgroup.com/determining-your-candidacy-for-dental-implants/
[6] Dental Implant Candidacy – https://www.allinthefamilydental.com/blog/dental-implant-candidacy/
[7] Am I A Good Candidate For Dental Implants Find Out – http://www.gurudentistry.com/am-i-a-good-candidate-for-dental-implants-find-out
[8] Dental Implants Complete Guide – https://www.magrabihealth.com/blog/dental-implants-complete-guide
[9] Dental Implants What You Should Know – https://www.fda.gov/medical-devices/dental-devices/dental-implant-what-you-should-know
[10] Are You A Good Candidate For Dental Implants Heres How To Tell – https://www.pickettfamilydental.com/blog/are-you-a-good-candidate-for-dental-implant-heres-how-to-tell/


Leave a Reply
Share your thoughts or ask a question about dental implants. Your email address will not be published.