Quick Answer: While dental implants boast a high success rate, understanding the signs and causes of failed dental implants / pictures of failed is crucial for early intervention. Failure can manifest as pain, swelling, mobility, or gum recession, typically stemming from infection, inadequate bone integration, or mechanical issues. Prompt consultation with a qualified dental professional in Dallas is essential to diagnose and address any problems effectively, often leading to successful corrective measures.
Key Takeaways
- Dental implant success rates are high, with 95-98% lasting 5-10 years, but failures can occur [1].
- Early implant failures often happen within the first year, primarily due to issues with osseointegration [3].
- Common signs of a failed dental implant include persistent pain, swelling, mobility, and gum recession around the implant site.
- Major causes of failure include peri-implantitis (infection), poor bone quality, uncontrolled systemic diseases (like diabetes), and improper surgical placement.
- Patients with chronic periodontitis face significantly higher failure rates [3].
- Preventative measures like excellent oral hygiene, regular dental check-ups, and addressing risk factors are vital for long-term success.
- If you suspect a failed implant, seek immediate professional evaluation in Dallas to determine the best course of action.
What Are the Early Warning Signs of Failed Dental Implants?
Recognizing the early warning signs of failed dental implants is crucial for timely intervention and potentially saving the implant or planning effective corrective measures. While initial discomfort is normal after dental implant surgery, persistent or worsening symptoms typically indicate a problem.
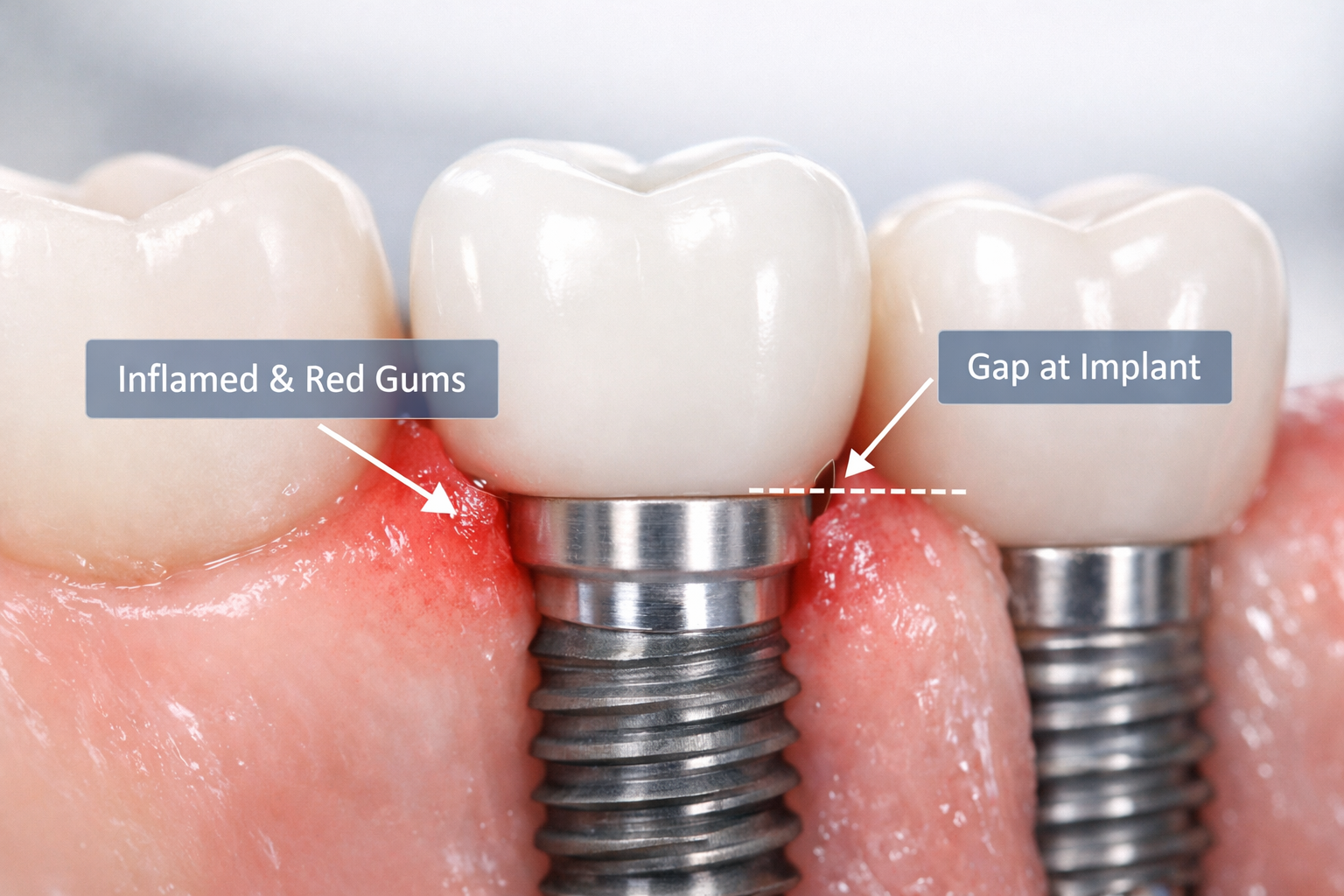
Common Indicators of Early Failure:
- Persistent or Worsening Pain: While some post-surgical pain is expected, severe or continuous pain around the implant site long after the initial healing period is a significant red flag. This pain might also radiate to other areas of the mouth.
- Swelling and Inflammation: Noticeable swelling, redness, or tenderness of the gums surrounding the implant that does not subside or worsens can point to an infection or inflammation.
- Mobility of the Implant: A healthy dental implant should feel completely stable, just like a natural tooth. Any noticeable movement or wobbling, even slight, indicates that the implant has not successfully integrated with the bone or has become compromised. This is one of the most definitive signs of failure.
- Gum Recession and Exposed Implant Threads: If the gum tissue around the implant begins to pull back, exposing the metal threads of the implant, it suggests bone loss or tissue inflammation. This can also make the area more susceptible to bacterial buildup.
- Difficulty Chewing or Biting: If chewing becomes painful or feels “off” on the side of the implant, it could be a sign that the implant is not stable or is putting undue pressure on surrounding structures.
- Pus or Discharge: The presence of pus or any unusual discharge from the gum line around the implant is a clear indicator of infection (peri-implantitis) and requires immediate dental attention.
If you experience any of these symptoms related to your dental implants in Dallas, it’s important to contact your dental professional right away. Delaying evaluation can lead to more complex and difficult-to-treat issues.
What Are the Primary Causes and Risk Factors for Failed Dental Implants?
Dental implant failure is a multifactorial issue, meaning it can arise from a combination of patient-specific conditions, surgical technique, and post-operative care. Understanding these factors is key to both prevention and successful treatment.
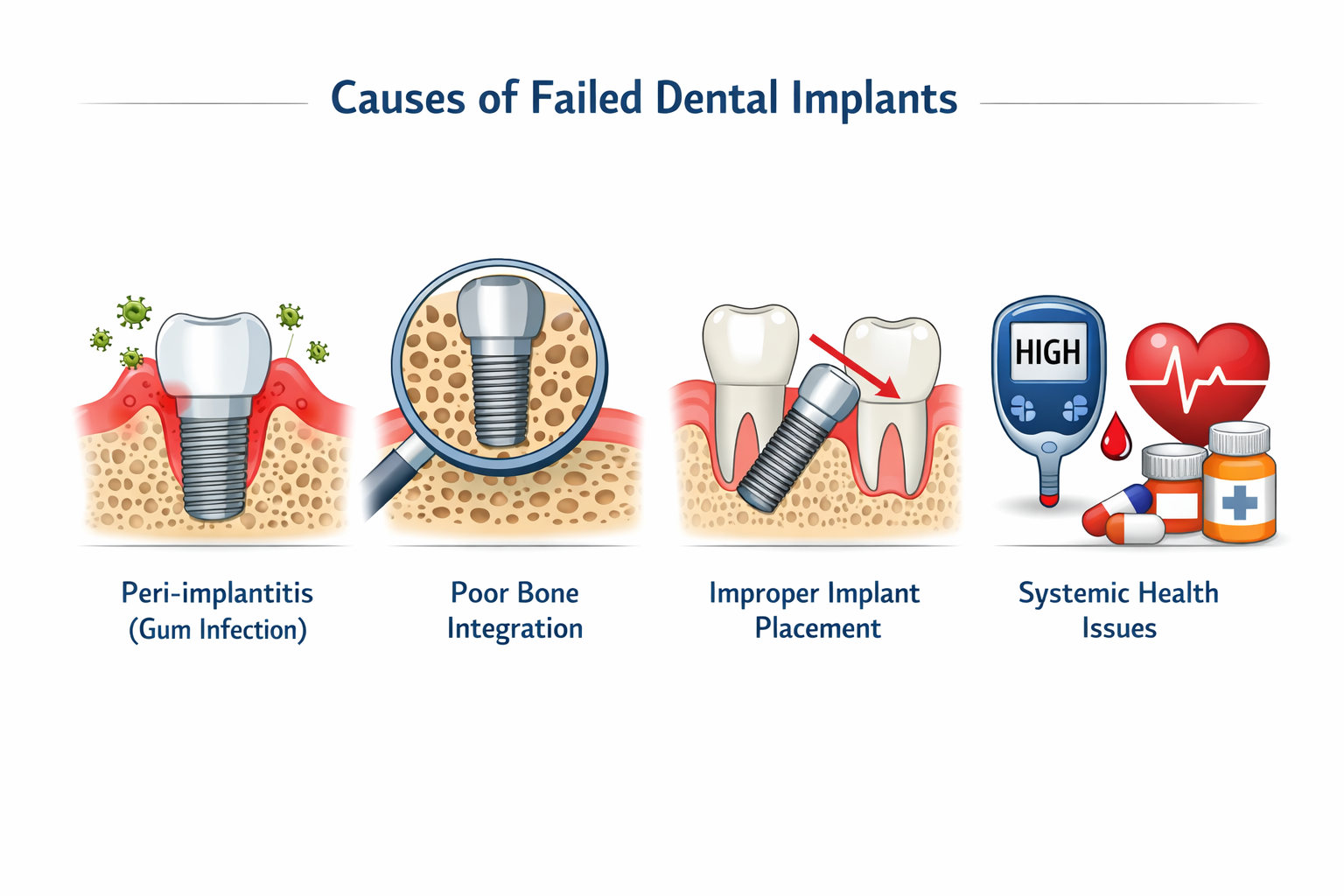
Leading Causes of Dental Implant Failure:
- Peri-implantitis (Infection): This is the most common cause of late-stage implant failure, affecting approximately 19.53% of patients and 12.53% of implants [1]. It’s an inflammatory condition resembling gum disease, where bacteria infect the gum tissue and bone surrounding the implant, leading to bone loss and eventually implant instability. Poor oral hygiene is a primary contributor.
- Lack of Osseointegration: Osseointegration is the critical process where the implant fuses with the jawbone. If this doesn’t occur successfully, the implant remains loose and fails. This can be due to:
- Inadequate Bone Quality or Quantity: Implants placed in Type IV bone (softest, least dense) have a significantly higher failure rate, at 20.6% [2]. A sufficient amount of dense, healthy bone is essential for stable integration. Sometimes, a bone graft may be necessary before implant placement.
- Overheating During Drilling: Excessive heat generated during implant placement can damage bone cells, hindering integration.
- Early Loading: Placing a crown on the implant too soon after surgery, before full integration has occurred, can disrupt the healing process.
- Systemic Health Conditions: Certain medical conditions can compromise the body’s ability to heal and integrate implants:
- Uncontrolled Diabetes: Diabetes impairs osseointegration and increases the odds of early failure [1].
- Autoimmune Diseases: Conditions that affect bone metabolism or immune response can be problematic.
- Osteoporosis: While not a direct contraindication, severe osteoporosis can affect bone density and healing.
- Radiation Therapy: Prior radiation to the head and neck can impair bone healing.
- Smoking: Smoking is a consistent and significant risk factor, increasing complication rates, especially for upper jaw implants [1]. It compromises blood flow, impairs healing, and increases the risk of infection.
- Poor Surgical Technique:
- Improper Placement: Incorrect angulation or depth of the implant can lead to excessive stress, nerve damage, or encroachment on vital structures.
- Insufficient Sterilization: Contamination during surgery can lead to infection.
- Mechanical Complications: Though less common as a primary cause of failure, these can stress the implant:
- Overload: Excessive biting forces, often from grinding (bruxism) or clenching, can stress the implant and surrounding bone, leading to breakdown. A dental implant night guard may be recommended.
- Component Fracture: Although rare, the implant itself or an abutment can fracture under extreme pressure.
- Medications: Certain medications, particularly bisphosphonates (used for osteoporosis), can affect bone metabolism and increase the risk of osteonecrosis of the jaw, which can impact implant success.
Patients with pre-existing periodontal disease have a much higher failure rate (14.3% at one year) compared to those with healthy gums (4.9%) [3]. Before considering dental implants in Dallas, it’s essential for a comprehensive evaluation to address any underlying risk factors.
What Does a Failed Dental Implant Look Like (Pictures of Failed Implants)?
While explicit clinical images can be sensitive, understanding the visual cues associated with failed dental implants is important for patients. Rather than graphic depictions, we can describe what a dental professional would observe and interpret as signs of failure, which aligns with the visual evidence you might see in educational materials or discuss during a consultation.
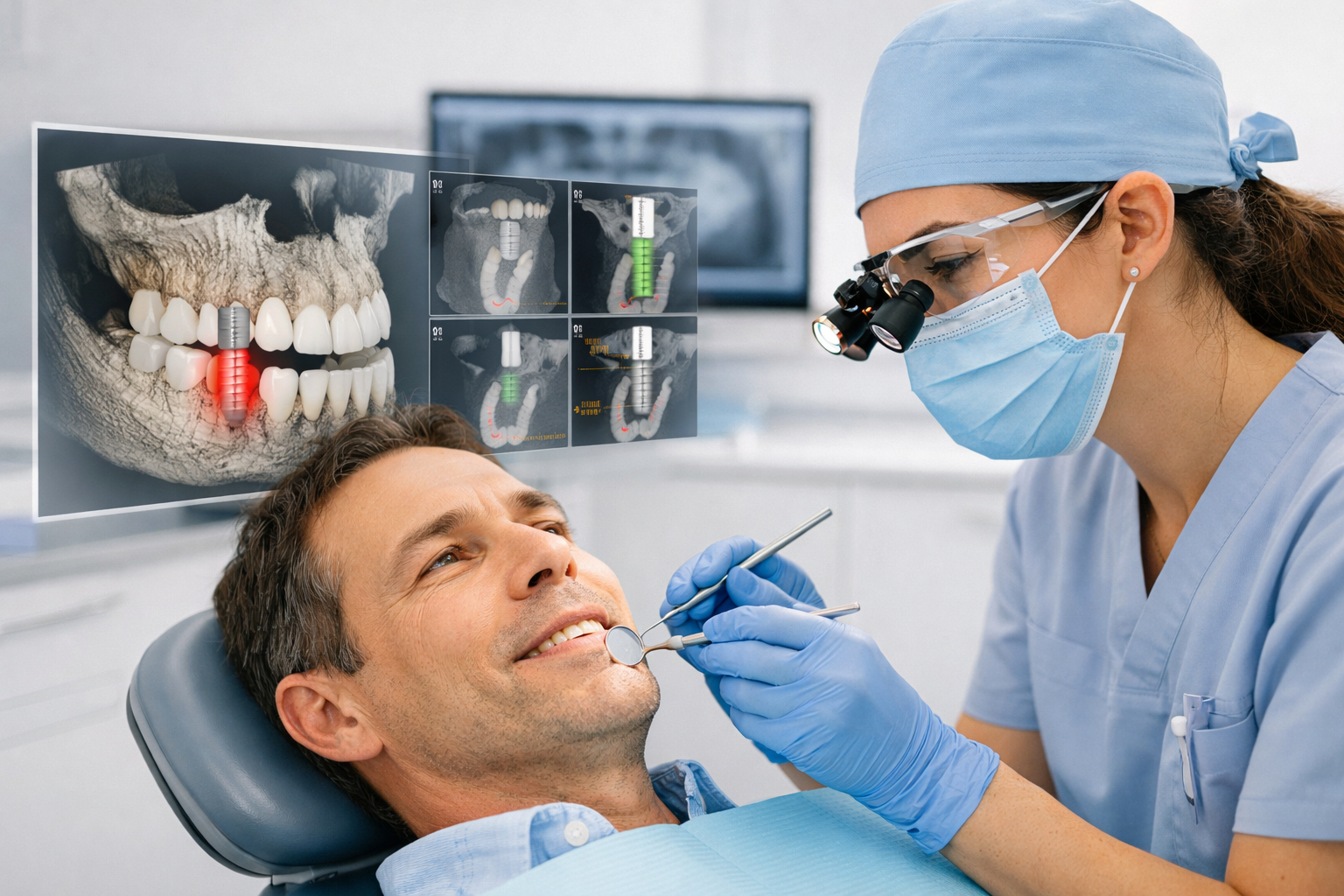
Visual Manifestations of Failed Dental Implants:
- Red, Swollen, or Bleeding Gums: Healthy gum tissue around an implant should be pink and firm. Redness, puffiness, or bleeding upon brushing or probing indicates inflammation, often a sign of peri-implantitis.
- Pus or Suppuration: Visible pus or a cloudy discharge from the gum margin around the implant is a clear sign of active infection.
- Receding Gums: When the gum tissue pulls away from the implant, exposing the metallic implant collar or threads, it suggests bone loss beneath the gum line. This can make the implant appear longer than adjacent teeth.
- Darkening Around the Implant: In some cases, if significant bone loss occurs, the implant itself might appear darker or more visible through the thinning gum tissue.
- Visible Mobility: While typically felt by the patient, a severely failed implant might show visible movement when gently prodded by a dentist. This is a critical indicator of non-integration or significant bone loss.
- Changes in Bite or Crown Position: If the crown or bridge supported by the implant shifts, becomes crooked, or feels uneven in the bite, it can suggest underlying implant instability.
- Radiographic Evidence (X-rays): A dental professional will rely on X-rays to confirm suspected failure. Pictures of failed implants on an X-ray will typically show:
- Bone Loss Around the Implant: A healthy implant will have a solid ring of bone around it. Failure often presents as a dark, irregular space around the implant body, indicating bone resorption.
- Lack of Osseointegration: An early failure might show a radiolucent (dark) line between the implant and the bone, indicating that fusion never occurred.
- Fractured Implant: Though rare, an X-ray can reveal a crack or break in the implant post itself.
A thorough clinical examination combined with radiographic imaging is essential for accurate diagnosis. Never attempt to self-diagnose based on pictures of failed implants online; always consult a dentist in Dallas for any concerns.
What Corrective Actions and Solutions Are Available for Failed Dental Implants?
Addressing failed dental implants depends heavily on the cause and severity of the problem. Early detection and prompt action by a qualified professional in Dallas significantly improve the chances of successful intervention.
Corrective Solutions for Failed Dental Implants:
- Non-Surgical Management (for early-stage peri-implantitis):
- Thorough Cleaning (Debridement): Similar to a deep cleaning for gum disease, the area around the implant is meticulously cleaned to remove plaque and calculus.
- Antimicrobial Rinses/Medications: Topical or systemic antibiotics may be prescribed to control bacterial infection.
- Improved Oral Hygiene Instruction: Patients receive guidance on proper brushing and flossing techniques specifically for their implants.
- Surgical Intervention (for advanced peri-implantitis or bone loss):
- Debridement and Detoxification: The implant surface is surgically exposed, cleaned, and detoxified to remove bacteria and contaminated tissue.
- Bone Grafting: If bone loss has occurred, a bone graft procedure may be performed to regenerate lost bone around the implant, enhancing its stability. This often requires a healing period before further steps. Learn more about bone graft costs for dental implants in Dallas.
- Guided Bone Regeneration (GBR): A membrane may be placed over the bone graft to protect it and encourage new bone growth.
- Soft Tissue Grafting: If gum recession is significant, a soft tissue graft can help cover exposed implant surfaces and improve aesthetics.
- Implant Removal and Replacement:
- When Removal is Necessary: If the implant is severely mobile, extensively infected, or has completely failed to integrate with the bone, removal is often the most appropriate step.
- Healing Period: After removal, the site needs time to heal. This might involve bone grafting to rebuild the site.
- Replacement: Once the bone has adequately healed and rebuilt, a new dental implant can often be placed. In some cases, a larger or different type of implant may be used, or a different tooth replacement option explored.
- Prosthetic Adjustments:
- If the issue is related to the crown or bridge (e.g., poor fit, excessive force), the prosthesis may need adjustment, repair, or replacement.
- Occlusal (bite) adjustments can help reduce undue stress on the implant.
The best course of action is determined by a thorough examination, including clinical assessment and X-rays. A qualified dentist in Dallas will discuss your options, outlining the pros and cons of each, to help you make an informed decision for your long-term oral health.
How Can You Prevent Dental Implant Failure?
Preventing dental implant failure largely revolves around meticulous oral hygiene, regular professional care, and managing systemic health conditions. Proactive steps are crucial for ensuring the long-term success of your dental implants in Dallas.
Key Strategies for Prevention:
- Choose an Experienced Dental Professional: The success of dental implant surgery begins with proper planning and execution. Selecting a highly skilled and experienced oral surgeon or periodontist in Dallas who uses advanced techniques, such as 3D guided dental implant surgery, can significantly reduce the risk of surgical complications and improper placement.
- Maintain Excellent Oral Hygiene: This is paramount. Brush twice daily with a soft-bristled toothbrush and floss daily, paying special attention to the areas around your implants. Interdental brushes or water flossers can be particularly effective for cleaning around implant posts. Poor oral hygiene is a primary driver of peri-implantitis.
- Attend Regular Dental Check-ups and Professional Cleanings: Schedule routine check-ups and cleanings with your dentist, typically every six months, or more frequently if recommended. These appointments allow your dental professional to monitor the health of your implants, assess your bite, and remove plaque and tartar that regular brushing might miss. Your dentist will also check your dental implant X-ray frequency to ensure proper monitoring.
- Manage Systemic Health Conditions: If you have chronic conditions like diabetes, ensure they are well-managed. Work closely with your medical doctor to keep blood sugar levels under control, as uncontrolled diabetes impairs healing and increases infection risk for dental implants.
- Quit Smoking: If you smoke, quitting is one of the most impactful steps you can take to improve the long-term prognosis of your dental implants. Smoking dramatically increases the risk of complications and failure.
- Address Bruxism (Teeth Grinding/Clenching): If you grind or clench your teeth, especially at night, discuss this with your dentist. They may recommend a custom night guard to protect your implants from excessive force.
- Follow Post-Operative Instructions Diligently: After your implant surgery, carefully adhere to all instructions provided by your Dallas dental professional regarding diet, medications, oral hygiene, and activity levels during the healing phase. This includes avoiding crunchy or hard foods initially and using prescribed antibiotics.
- Nutritious Diet: A balanced diet supports overall health and bone strength, which is vital for implant integration and longevity.
By committing to these preventative measures, you can significantly enhance the success rate and longevity of your dental implants, ensuring a healthy, confident smile for years to come.
What is the Overall Success Rate for Dental Implants, and How Common are Failures?
Dental implants are widely recognized as a highly successful and predictable tooth replacement option, boasting impressive long-term survival rates. However, like any medical procedure, there is a small percentage of cases where complications or failures can occur.
Dental Implant Success and Failure Statistics:
- High Survival Rates: Across numerous studies, dental implants demonstrate a remarkably high success rate. A large-scale study of over 158,000 implants reported a 97.79% survival rate, with only a 2.21% failure rate [1]. Over a 5-10 year period, success rates typically range from 95-98% [1].
- Long-Term Durability: Even over extended periods, implants show excellent longevity. A cohort study tracking 10,871 implants for up to 22 years found cumulative survival rates of 98.9% at 3 years, 98.5% at 5 years, 96.8% at 10 years, and 94.0% at 15 years [2]. A 20-year meta-analysis also revealed a mean survival rate of 92% [4].
- Early vs. Late Failures: Most failures tend to occur relatively early. National averages indicate that 1-3% of failures happen within the first year in low-risk patients, primarily due to issues with osseointegration, while additional failures accumulate gradually over the next decade [3]. Late failures are more commonly associated with peri-implantitis or mechanical complications.
- Factors Influencing Rates: The survival rates can vary based on several factors, including patient health (e.g., smoking, diabetes), bone quality, implant size (smaller implants have higher failure rates) [2], and the skill of the surgical team. Research is continually being funded, such as a $2.9 million award to the Eastman Institute for Oral Health, to further understand and prevent implant failures [5].
While the overall odds of success are overwhelmingly in your favor, it’s important to be aware that dental implant failure, though uncommon, is a possibility. Discussing your specific risk factors and expected outcomes with your Dallas dentist is a crucial part of the informed decision-making process for tooth replacement options.
When Should You Consult a Dental Professional in Dallas for Implant Concerns?
It is always advisable to consult a dental professional in Dallas if you have any concerns about your dental implants, even if the symptoms seem minor. Early diagnosis and intervention can prevent minor issues from escalating into significant failures.
Immediate Consultation is Recommended If You Experience:
- New or Worsening Pain: Any pain that develops after the initial healing period, or pain that persists and doesn’t respond to typical pain relievers.
- Swelling, Redness, or Tenderness: Persistent inflammation around the implant site.
- Implant Mobility: Any feeling that the implant, crown, or bridge is loose. This is a critical sign and should be evaluated immediately.
- Pus or Discharge: Signs of infection around the implant.
- Gum Recession: If the gums around the implant are pulling back, exposing more of the implant structure.
- Changes in Your Bite: If your bite feels off or uncomfortable.
- Unexplained Bleeding: Any bleeding from the implant area that is not related to brushing or flossing, or is excessive.
What to Expect During Your Consultation in Dallas:
When you consult a dental professional about implant concerns, they will typically:
- Conduct a Thorough Clinical Examination: This involves visually inspecting the implant site, checking for swelling, redness, and gum health, and gently probing around the implant.
- Assess Implant Stability: They will gently check for any mobility of the implant.
- Take X-rays: Radiographs are crucial for evaluating the bone level around the implant, assessing osseointegration, and identifying any underlying issues not visible to the naked eye.
- Discuss Your Medical History: They will review any changes in your health or medications that could impact your implant.
- Discuss Lifestyle Factors: Questions about smoking, oral hygiene habits, and teeth grinding may be asked.
- Formulate a Diagnosis and Treatment Plan: Based on their findings, your dentist will explain the likely cause of the issue and outline the recommended treatment options, including potential costs and expected outcomes.
For anyone in Dallas considering dental implants or experiencing concerns, a timely consultation is your best step toward maintaining your long-term oral health. Don’t hesitate to reach out to a trusted local dental expert.
Frequently Asked Questions About Failed Dental Implants
What is the most common reason for dental implant failure?
The most common reason for late dental implant failure is peri-implantitis, an infection affecting the gums and bone around the implant [1]. For early failures, lack of proper osseointegration (fusion with the jawbone) is a primary cause [3].
Can a failed dental implant be saved?
Yes, in many cases, a failed dental implant can be saved, especially if the issue is detected and treated early. Treatment options range from non-surgical cleaning to surgical bone grafting, depending on the cause and severity.
How painful is a failed dental implant?
The pain level can vary from mild discomfort to severe, throbbing pain, depending on the cause of the failure. Pain, swelling, and tenderness are common signs of infection or other complications.
How long do dental implants typically last?
Dental implants are designed for long-term durability. With proper care, they can last a lifetime. Studies show success rates of 95-98% over 5-10 years, and many last 15-20 years or more [1, 2].
Can you get another implant after a failed one?
Often, yes. After a failed implant is removed and the site has time to heal, possibly with bone grafting, another dental implant can typically be placed successfully in the same location.
Does insurance cover failed dental implants?
Coverage for failed dental implants can vary significantly based on your insurance plan and the cause of failure. It’s essential to consult your provider and your Dallas dental office regarding your specific dental implant insurance coverage.
Is it normal for a dental implant to feel weird?
It’s normal for a dental implant to feel slightly “weird” or different from a natural tooth initially, but this sensation should gradually subside as you adapt. Persistent weird feelings or discomfort might warrant a check-up. More information can be found in our guide on how long until a dental implant stops feeling weird.
Can a dental implant fail years later?
Yes, a dental implant can fail years after placement, even after successful osseointegration. Late failures are often due to peri-implantitis, excessive biting forces, or changes in systemic health.
What are the risks of leaving a failed dental implant untreated?
Leaving a failed dental implant untreated can lead to worsening infection, further bone loss, damage to adjacent teeth, and persistent pain or discomfort. It’s crucial to seek professional evaluation.
Are there any natural remedies for a failed dental implant?
There are no natural remedies for a failed dental implant. Dental implant complications require professional medical and dental intervention to diagnose and treat effectively. Attempting natural remedies can delay proper treatment and worsen the condition.
Conclusion
Understanding the potential for failed dental implants, including the visual signs and underlying causes, is an important part of the dental implant journey. While dental implants boast a high success rate, being aware of the warning signs like persistent pain, swelling, or mobility, is key to timely intervention. Factors such as peri-implantitis, poor bone quality, and certain systemic health conditions are common contributors to failure, but many of these risks can be mitigated through proper patient selection, meticulous surgical technique, and diligent post-operative care.
If you suspect you have a failed dental implant or are experiencing any concerns, it is crucial to consult with an experienced dental professional in Dallas without delay. Early diagnosis allows for a wider range of corrective actions, from non-surgical treatments to implant removal and replacement, often leading to a successful resolution. By prioritizing excellent oral hygiene, attending regular check-ups, and addressing risk factors, you can significantly enhance the long-term success of your dental implants and maintain your oral health for years to come.


Leave a Reply
Share your thoughts or ask a question about dental implants. Your email address will not be published.