Discovering that your dental implant, a cornerstone of modern tooth replacement options, might be experiencing bone loss can be concerning. However, recognizing implant bone loss symptoms early is crucial for successful intervention and protecting your long-term oral health. As a leading resource for dental implants in Dallas, TX, we understand the importance of informed decision-making and want to empower you with knowledge about this vital aspect of implant care.
Key Takeaways
- Early detection of implant bone loss is critical for effective treatment and preserving your dental implant.
- Common early symptoms include persistent discomfort, gum recession, swelling, bleeding, and subtle implant mobility.
- Peri-implantitis, an infection around the implant, is a primary cause of early bone loss.
- Factors like poor oral hygiene, smoking, certain medical conditions, and excessive biting forces can increase the risk.
- Regular dental check-ups and professional cleanings are essential for monitoring implant health.
- If you notice any concerning signs, consult with a dentist promptly to prevent further complications.
- Initial bone loss of up to 1.0 mm in the first year after implant loading can be considered normal in some cases, but anything beyond that or progressive loss warrants immediate attention [1, 3].
- Dallas residents seeking dental implants should prioritize dentists who emphasize detailed post-operative care and patient education on symptom recognition.
Quick Answer
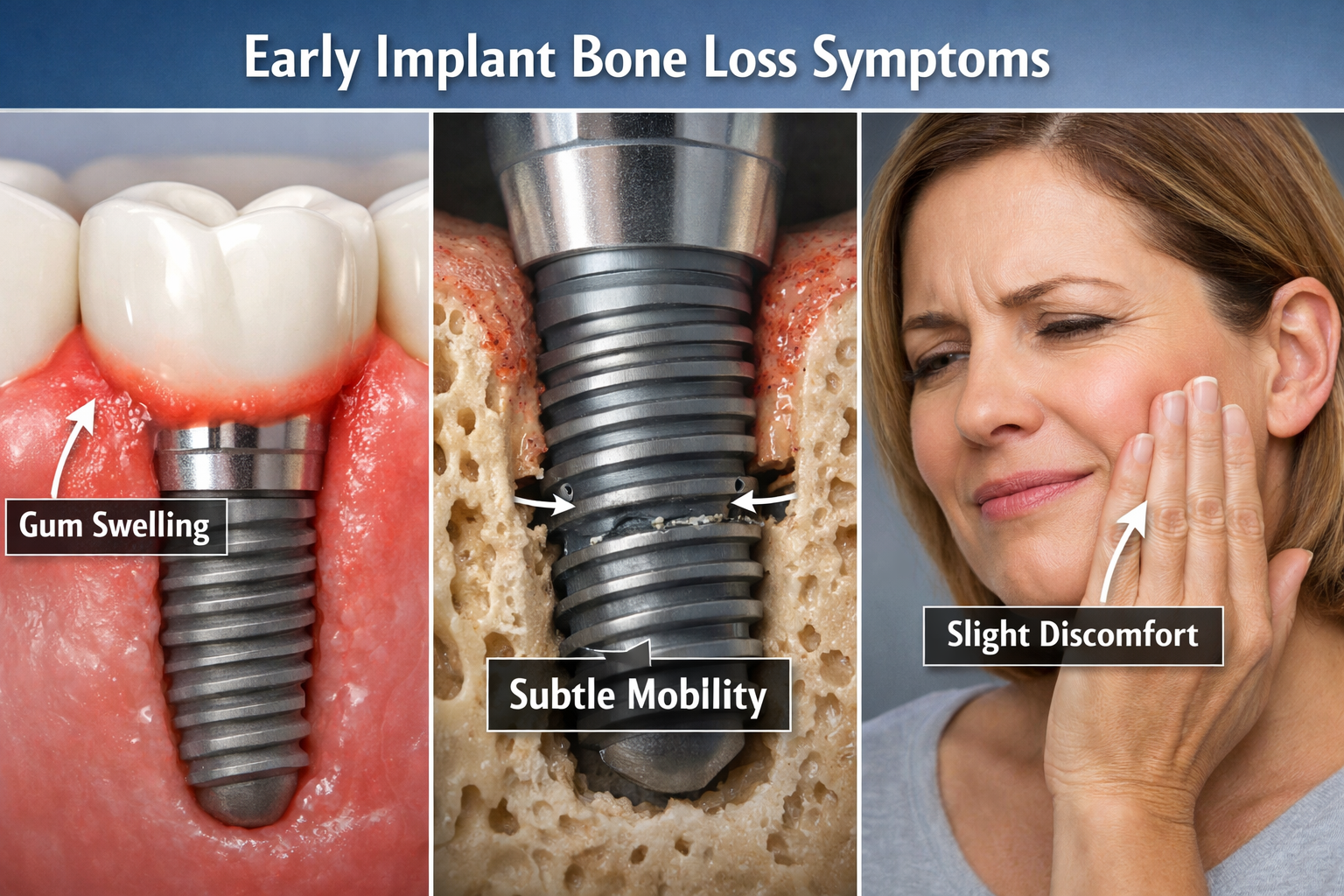
Implant bone loss symptoms early often manifest as subtle changes around your dental implant, including persistent mild pain or discomfort, gum inflammation (redness, swelling, or bleeding), a receding gum line, or a feeling of slight looseness or “weirdness” in the implant itself [2]. These signs, while sometimes mild, indicate potential underlying issues such as infection (peri-implantitis) or problems with osseointegration and require prompt evaluation by a dental professional to prevent more significant complications.
What Are the Early Signs of Implant Bone Loss?
The early signs of implant bone loss are often subtle and can easily be mistaken for minor irritation, but recognizing them promptly is crucial for the longevity of your dental implant. These symptoms typically involve changes in the soft tissues surrounding the implant and a feeling of discomfort that persists beyond the initial healing period.
Initially, you might experience symptoms such as persistent, mild pain or discomfort around the implant site that doesn’t subside after the first week or two post-surgery [2]. Unlike the normal post-operative soreness that gradually improves, pain associated with early bone loss may linger or even worsen [2]. Other key indicators include gum recession, where the gum tissue around the implant begins to pull away, exposing more of the implant surface, or the presence of redness, swelling, and bleeding in the gums [2]. If you notice bleeding or pus when you gently probe the area or during routine brushing, this is a significant clinical sign of inflammation or infection [1]. Additionally, a subtle feeling of the implant being “weird” or slightly loose, even without noticeable movement, can be an early warning [2]. If you’re seeking dental implants in Dallas, understanding these indicators is vital for your long-term oral health.
Recognizing Subtle Changes Around Your Implant
It’s important to differentiate between normal post-surgical healing and early signs of complications. For the first few days to a week after implant surgery, some discomfort, minor swelling, and bruising are typical. However, any symptoms that persist or intensify beyond this initial period should be cause for concern.
Consider these specific early indicators:
- Persistent Mild Discomfort or Pain: If the area around your dental implant continues to ache or feels tender long after the expected healing period (typically one to two weeks), it could signal an underlying issue [2]. This isn’t the sharp, acute pain of a fresh injury, but a dull, nagging discomfort.
- Gum Inflammation: Look for gums that appear redder than usual, are swollen, or feel tender to the touch around the implant [2]. This inflammation is often an early sign of peri-implantitis, an infection that can lead to bone loss [1].
- Bleeding Gums: If your gums bleed easily when brushing, flossing, or during a routine dental check-up, especially around the implant, it indicates inflammation [1]. Healthy gum tissue around an implant should not bleed.
- Gum Recession: Observe if the gum line around your implant appears to be receding or pulling away from the implant crown, potentially exposing part of the metal post. This can be a visual cue of underlying bone loss.
- Suppuration (Pus): The presence of pus or a white discharge from the gum tissue surrounding the implant is a clear sign of infection and requires immediate attention [1].
- Changes in Feel or Mobility: While a fully integrated implant should feel completely stable, a very subtle change in how the implant feels—perhaps a slight rocking sensation, or just a general feeling that “something isn’t quite right”—can be an early warning of inadequate osseointegration or beginning bone loss [2].
If you experience any of these symptoms, it’s crucial to schedule a consultation with your dentist in Dallas without delay. Early intervention can often prevent more severe complications and ensure the success of your dental implant procedure.
What Causes Early Bone Loss Around Dental Implants?
Early bone loss around dental implants is primarily caused by peri-implantitis, which is an inflammatory condition affecting the tissues surrounding a dental implant, leading to progressive bone destruction [1]. Beyond infection, other significant factors include inadequate osseointegration, which is the failure of the implant to properly fuse with the jawbone, and excessive biomechanical stress on the implant [1].
Understanding the underlying reasons for early implant bone loss is key to prevention and successful long-term outcomes. While dental implants boast a high success rate, typically over 90% over 10 years, failures can occur, and bone loss is a significant contributor [2]. For patients considering missing teeth solutions, especially in a metropolitan area like Dallas, being aware of these potential causes can help in preventative care and prompt action.
Common Factors Contributing to Early Bone Loss
Several factors can contribute to the development of early bone loss around dental implants:
- Peri-Implantitis: This is the most common cause of implant bone loss [1]. It’s essentially gum disease around an implant, triggered by bacterial infection similar to periodontitis around natural teeth. If left untreated, the inflammation can destroy the surrounding bone tissue, weakening the implant’s support. Poor oral hygiene is a primary risk factor for peri-implantitis, as plaque and bacteria accumulate around the implant.
- Decision Rule: If you notice redness, swelling, or bleeding around your implant, especially with pus, it’s critical to seek professional evaluation for peri-implantitis immediately. Early treatment can halt bone loss. You can learn more about Peri-Implantitis Prevention in Dallas.
- Inadequate Osseointegration: For a dental implant to be successful, it must securely fuse with the surrounding jawbone in a process called osseointegration. If this process is compromised—due to insufficient bone density at the implant site, improper surgical technique, or early loading of the implant—the implant may never fully integrate, leading to instability and eventual bone loss [1, 5].
- Common Mistake: Applying too much pressure or chewing hard foods on a newly placed implant before it has fully integrated can disrupt osseointegration.
- Biomechanical Stress: Excessive force or improper bite alignment on the dental implant can lead to biomechanical stress, which essentially overloads the implant and causes the surrounding bone to resorb or break down [1]. This can happen if the implant is placed incorrectly, if the crown is not properly adjusted, or if the patient has habits like teeth grinding (bruxism) without proper protection.
- Edge Case: Patients with bruxism often require a nightguard to protect their dental implants from excessive nocturnal forces.
- Systemic Health Conditions: Certain medical conditions can impact bone health and the body’s ability to heal, thereby increasing the risk of implant bone loss. These include uncontrolled diabetes, osteoporosis, and autoimmune diseases [6]. Smoking also significantly impairs healing and increases the risk of complications, including peri-implantitis and bone loss [6].
- Poorly Fitted Prosthesis: If the crown, bridge, or denture attached to the implant does not fit correctly, it can create uneven pressure on the implant, leading to stress on the bone and subsequent loss [1].
- Inadequate Bone Volume or Quality: Sometimes, patients may not have sufficient bone volume or quality at the implant site to begin with. While bone grafting can address this (see Bone Graft Costs for Dental Implants in Dallas), if the underlying bone support is weak or compromised, the implant’s long-term stability can be affected [5].
Regular follow-ups with your dentist, particularly in the first year after the dental implant procedure, are essential for monitoring these factors and addressing any concerns before they escalate.
How is Early Implant Bone Loss Diagnosed?
Early implant bone loss is primarily diagnosed through a combination of clinical examination and radiographic imaging. During a clinical examination, the dentist will assess the gums around the implant for signs of inflammation, bleeding, or recession, and may gently probe the area to check for pus or pocketing [1]. Radiographs, specifically dental X-rays, are critical for visualizing the bone level around the implant and detecting any changes that are not visible during a physical examination [1].
For anyone with dental implants in Dallas, understanding the diagnostic process is important. It ensures that any potential issues are caught early, allowing for timely and effective intervention. The goal is to detect subtle changes in bone support before they become severe, preserving the implant’s stability and your long-term oral health.
Diagnostic Tools and Procedures
The diagnostic process for early implant bone loss involves several key steps:
- Clinical Examination:
- Visual Inspection: Your dentist will carefully examine the soft tissues surrounding your dental implant for any signs of redness, swelling, or recession [2]. They will also look for any exposed threads of the implant, which can indicate bone loss.
- Probing Depths: A specialized periodontal probe is used to measure the depth of the gum pocket around the implant. Increased probing depths can indicate inflammation or bone loss, similar to how gum disease is assessed around natural teeth [1]. The presence of bleeding or pus upon probing is a strong indicator of peri-implantitis [1].
- Mobility Check: While significant implant mobility is a sign of advanced failure, very subtle, almost imperceptible movement might be detected by an experienced clinician during an early stage examination [2].
- Radiographic Imaging (X-rays):
- Periapical and Bitewing X-rays: These standard dental X-rays provide a two-dimensional view of the bone levels around the implant. Dentists compare current X-rays with baseline images taken shortly after implant placement to identify any changes in bone height.
- Cone Beam Computed Tomography (CBCT): In more complex cases or when a clearer three-dimensional view is needed, a CBCT scan may be utilized. This advanced imaging technique offers detailed information about bone volume and density around the implant, helping to precisely quantify bone loss and plan treatment.
- Bone Loss Thresholds: Radiographic diagnosis is guided by established thresholds. While some initial marginal bone loss of up to 1.0 mm in the first year after functional loading is sometimes considered acceptable, anything beyond this, or progressive bone loss exceeding 0.2 mm per year thereafter, is generally indicative of a problem and signals potential implant failure [1, 3]. It’s crucial for your dentist to track these measurements accurately over time.
Monitoring Implant Health
Regular dental check-ups and follow-up appointments are indispensable for monitoring the health of your dental implants. Your dentist will typically recommend periodic X-rays to assess bone levels, even if you report no symptoms. This proactive approach helps detect early implant bone loss before it becomes clinically apparent or problematic. These visits are also an opportunity to assess your oral hygiene practices and provide guidance on proper implant care. For optimal results and long-term success of your tooth replacement options, especially with your dental implants in Dallas, consistent professional monitoring is key.
What Are the Treatment Options for Early Implant Bone Loss?
Treatment options for early implant bone loss focus on halting the progression of bone loss, managing any infection, and stabilizing the implant. The specific approach depends on the severity of the bone loss and the underlying cause, but often involves non-surgical interventions, enhanced oral hygiene, and, in some cases, minor surgical procedures.
The goal is always to intervene as early as possible to prevent the situation from deteriorating, which could eventually lead to implant failure [1]. For patients with dental implants in Dallas, early and effective treatment is critical to protecting their investment in their long-term oral health.
Non-Surgical and Surgical Interventions
Here’s a breakdown of potential treatment options:
- Enhanced Oral Hygiene and Professional Cleaning:
- Initial Step: If early bone loss is linked to peri-implantitis caused by plaque accumulation, the first line of defense is meticulous professional cleaning. This involves thorough debridement (removal of plaque, calculus, and granulation tissue) around the implant using specialized instruments that won’t damage the implant surface [1].
- Patient Education: You will receive detailed instructions on improving your at-home oral hygiene routine, including proper brushing techniques (using soft brushes or electric toothbrushes), interdental cleaning tools (such as interdental brushes or water flossers), and possibly antimicrobial rinses [1]. Consistent and effective daily cleaning is paramount.
- Antibiotic Therapy:
- Targeting Infection: If a bacterial infection is present, your dentist may prescribe local or systemic antibiotics to help eliminate the pathogens causing peri-implantitis [1]. Local antibiotics might be delivered directly into the gum pocket around the implant, while systemic antibiotics are taken orally.
- Non-Surgical Decontamination:
- Surface Cleaning: This involves cleaning the implant surface below the gum line to remove bacterial biofilm. Various methods can be used, including specialized curettes, ultrasonic scalers with non-metallic tips, or air-abrasive devices with specific powders.
- Surgical Interventions (when non-surgical methods are insufficient):
- Open Flap Debridement: If bone loss is more advanced or non-surgical treatments don’t resolve the infection, a minor surgical procedure might be necessary. This involves lifting the gum tissue to gain direct access to the implant surface and the underlying bone. The area is thoroughly cleaned, infected tissue is removed, and the implant surface is decontaminated [1].
- Bone Grafting: In cases where significant bone loss has occurred but the implant is still stable, a bone graft procedure may be considered to regenerate lost bone around the implant [1]. This aims to restore lost support and improve the prognosis of the implant. This can be a complex procedure, and understanding Bone Graft Healing for Dental Implants is crucial.
- Resective Surgery (Implantoplasty): In some instances, it might be necessary to reshape or smooth the exposed implant threads (implantoplasty) to make them easier to clean and less prone to bacterial colonization [1]. This procedure is often combined with open flap debridement.
Important Consideration: The key to successful treatment is early detection. If you experience any of the implant bone loss symptoms early, it’s vital to consult your dental professional promptly. Ignoring these signs can lead to worsening conditions, increasing the complexity and cost of treatment, and potentially resulting in the loss of the implant. Patients with missing teeth solutions and those with existing implants should maintain vigilant oral hygiene and regular dental check-ups.
Preventing Dental Implant Bone Loss
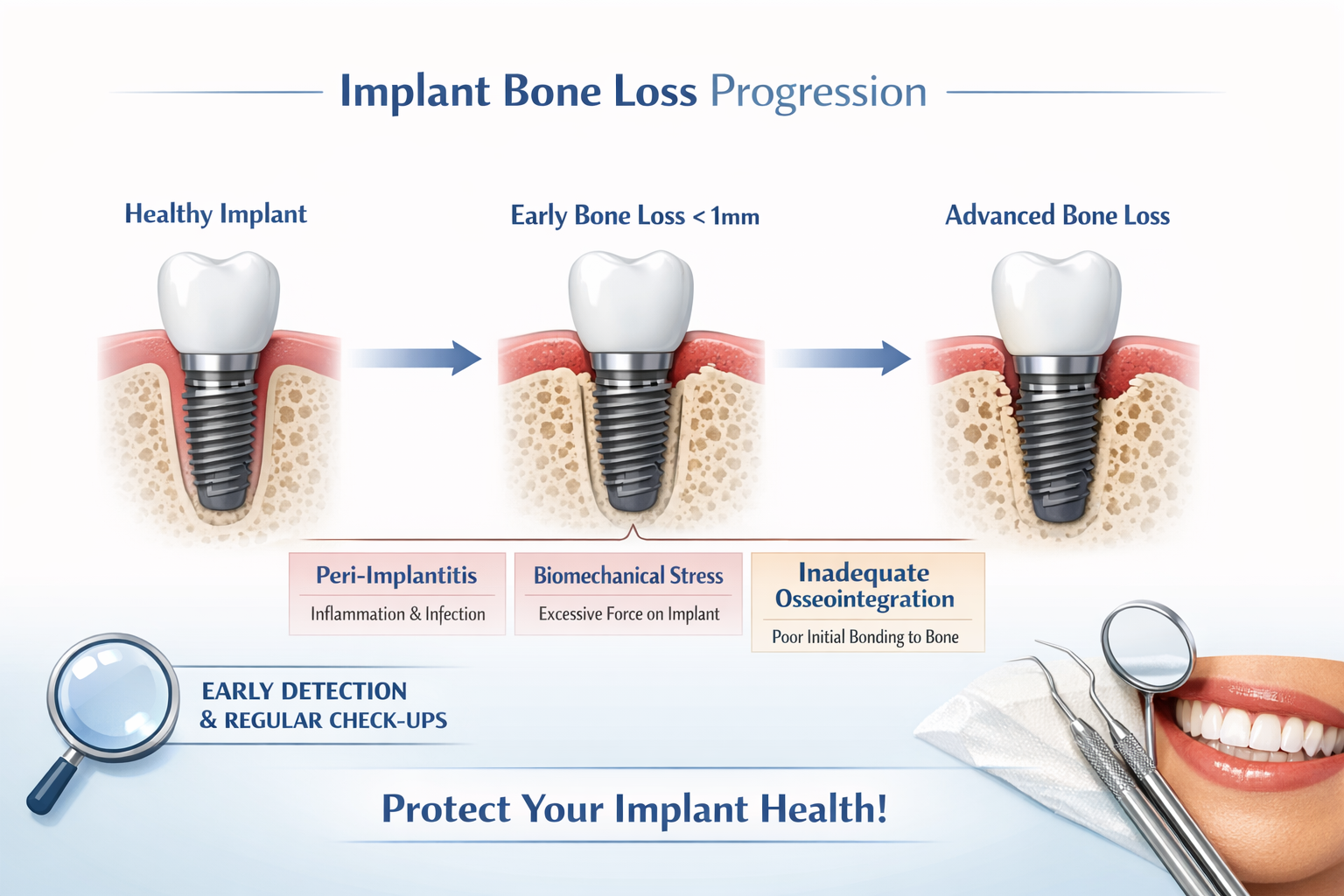
Preventing dental implant bone loss hinges on a combination of excellent oral hygiene, regular professional dental care, and managing risk factors. Proactive steps are far more effective than reactive treatments, ensuring the long-term success and stability of your dental implants.
For individuals who have invested in dental implants in Dallas, adopting a preventative mindset is essential to safeguard their smile and overall well-being. By following recommended care guidelines, you can significantly reduce the risk of developing complications such as peri-implantitis and associated bone loss.
Best Practices for Long-Term Implant Health
Here are critical strategies to prevent dental implant bone loss:
- Maintain Exemplary Oral Hygiene:
- Daily Routine: Brush your teeth and implants at least twice a day using a soft-bristled brush, paying special attention to the areas around your implants. Use non-abrasive toothpaste.
- Interdental Cleaning: Floss daily, or use interdental brushes or a water flosser to clean thoroughly around and between your implants. This helps remove plaque and food debris that can lead to infection.
- Antimicrobial Rinses: Your dentist might recommend an antimicrobial mouthrinse, especially if you have a history of gum inflammation.
- Schedule Regular Dental Check-ups and Professional Cleanings:
- Frequency: Visit your dentist or dental hygienist every six months, or more frequently if recommended, for professional cleanings and examinations.
- Specialized Care: Dental hygienists trained in implant care use specific tools that clean implants without scratching their surface, preventing bacterial colonization. These visits also allow your dentist to monitor bone levels with X-rays and detect any implant bone loss symptoms early [1]. You can also ask your dentist about Optimal Dental Implant X-Ray Frequency.
- Manage Risk Factors:
- Quit Smoking: Smoking is a significant risk factor for peri-implantitis and can severely compromise healing and long-term implant success [6]. Quitting smoking is one of the most impactful steps you can take.
- Control Systemic Diseases: If you have conditions like diabetes, ensure they are well-managed. Uncontrolled diabetes can impair healing and increase susceptibility to infections [6].
- Address Bruxism (Teeth Grinding): If you grind or clench your teeth, your dentist may recommend a custom nightguard to protect your implants from excessive force that can lead to biomechanical stress and bone loss.
- Choose a Qualified and Experienced Implant Dentist:
- Expertise Matters: The initial planning and placement of your dental implant procedure are crucial. An experienced dentist specializing in dental implants in Dallas will ensure proper implant positioning, adequate bone support, and correct prosthetic design to minimize future complications. Ask Questions to Ask Dentist About Implants to ensure you choose wisely.
- Follow Post-Operative Instructions Diligently:
- Healing Phase: Adhere strictly to all post-operative care instructions provided by your dentist, especially during the initial healing period. This includes dietary restrictions, medication schedules, and activity limitations.
- Avoid Excessive Force on Implants:
- Chewing Habits: Be mindful of chewing very hard or sticky foods directly on your implants, especially immediately after restoration. While implants are strong, repeated excessive force can be detrimental.
By committing to these preventative measures, you significantly enhance the longevity and success of your dental implants, ensuring you continue to enjoy the benefits of your tooth replacement options for many years to come.
When to Consult a Dentist in Dallas for Implant Concerns
You should consult a dentist in Dallas immediately if you notice any persistent discomfort, swelling, redness, bleeding, or gum recession around your dental implant, or if the implant feels loose or “weird” [2]. Early intervention is paramount, as waiting can allow minor issues to escalate into more complex and costly problems, potentially leading to implant failure [1].
Our commitment at Dental Implant Education – Dallas TX is to patient safety and long-term oral health. We encourage anyone with dental implant concerns to seek professional advice promptly. Recognizing implant bone loss symptoms early can make a significant difference in the outcome.
Urgent Signs Requiring Dental Consultation
Don’t delay seeking professional help if you experience any of these signs:
- Persistent or Worsening Pain: While some discomfort is normal after surgery, pain that lasts beyond a week or two, or pain that steadily increases, is a red flag [2]. This could indicate infection, nerve damage, or a failing implant.
- Visible Swelling or Redness: Inflammation around the implant site that doesn’t subside or appears suddenly warrants immediate attention. These are classic signs of infection, such as peri-implantitis [2].
- Bleeding or Pus: Any bleeding when brushing, flossing, or spontaneously, or the presence of pus (a yellowish-white discharge) from the gum around the implant, is a clear indicator of infection that needs urgent treatment [1].
- Gum Recession: If you notice your gums pulling away from the implant, exposing more of the metal or ceramic abutment, it suggests gum tissue and potentially bone loss.
- Implant Mobility or Looseness: Even a slight feeling of movement or looseness in the implant—whether you can visibly see it move or it just “feels off” when you touch it or bite down—is a critical sign of implant failure or severe bone loss and requires immediate evaluation [2]. A healthy implant should be entirely stable.
- Difficulty Chewing or Biting: If chewing becomes painful, uncomfortable, or you feel the implant shifting when you eat, it could signal an issue with the implant’s stability or bite alignment [2].
- Bad Breath or Foul Taste: While bad breath can have many causes, a persistent foul taste or odor specifically emanating from around the implant could indicate a bacterial infection. You can read more about Bad Breath from Dental Implants.
- Fever or Systemic Symptoms: In rare cases, a severe infection around an implant can lead to systemic symptoms like fever. If accompanied by any local implant symptoms, seek urgent dental and medical care.
If you are experiencing any of these issues, contact a qualified dental professional in Dallas right away. They can accurately diagnose the problem and recommend the most appropriate course of action. Delaying treatment can lead to more significant bone loss, increased discomfort, and a higher chance of losing the implant. For comprehensive care and a consultation with a dentist specializing in implant surgery, reach out to a reputable Dallas dental practice.
Frequently Asked Questions
What does early bone loss around an implant feel like?
Early bone loss around an implant might feel like persistent mild discomfort or a dull ache, tenderness when you press on the gum around the implant, or a sensation that “something isn’t quite right” or is slightly different from how it used to feel [2]. You might also notice sensitive, swollen, or bleeding gums.
Can a dental implant bone loss be reversed?
While some initial inflammation and bone loss can be managed and halted, severely lost bone tissue around an implant is challenging to fully reverse, though bone grafting procedures can sometimes regenerate some support [1]. Early detection and intervention are key to preventing irreversible damage.
How much bone loss is normal after implant placement?
Normally, some marginal bone remodeling (loss) can occur during the first year after a dental implant is loaded, typically averaging around 0.2 mm to 1.0 mm [1, 3]. However, any bone loss exceeding 0.2 mm per year after the first year is considered abnormal and a sign of potential complications [1].
Can a loose dental implant be saved?
A slightly loose dental implant, if caught very early, might be saved if the underlying cause (e.g., infection or occlusal trauma) can be effectively treated [2]. However, significant or progressive mobility often indicates severe bone loss or failed osseointegration, making salvage less likely [1].
What is peri-implantitis and how does it relate to bone loss?
Peri-implantitis is an inflammatory disease affecting the soft and hard tissues surrounding a dental implant, similar to gum disease around natural teeth [1]. It is primarily caused by bacterial infection and, if left untreated, leads to progressive destruction of the supporting bone around the implant, resulting in bone loss and potentially implant failure [1].
Are there any preventative measures for implant bone loss?
Yes, preventative measures include excellent daily oral hygiene (brushing, flossing, interdental cleaning), regular dental check-ups and professional cleanings, avoiding smoking, managing systemic health conditions like diabetes, and wearing a nightguard if you grind your teeth [6].
What happens if implant bone loss is left untreated?
If implant bone loss is left untreated, the infection and inflammation will progress, leading to further destruction of the supporting jawbone [1]. This can result in increasing implant mobility, severe pain, functional problems, and ultimately, the complete failure and loss of the dental implant [2].
Conclusion
Understanding implant bone loss symptoms early is paramount for anyone with dental implants, especially for those in Dallas seeking to protect their investment in a healthy, functional smile. While dental implants are remarkably successful tooth replacement options, vigilance regarding your oral health is key. Persistent discomfort, gum inflammation, bleeding, recession, or any feeling of looseness are not minor issues; they are critical early warning signs that demand your attention.
By recognizing these signs and promptly seeking a consultation with a dentist, you can often intercept potential problems like peri-implantitis before they escalate into more significant bone loss and potential implant failure. Proactive measures, including diligent oral hygiene and regular check-ups with your trusted Dallas dental professional, are your best defense. Don’t hesitate to reach out to a dental clinic specializing in implant surgery for any concerns about your dental implants in Dallas. Your long-term oral health depends on it.
References
[1] Failed Dental Implant Due To Bone Loss – https://int.livhospital.com/failed-dental-implant-due-to-bone-loss/
[2] 5 Signs Of Dental Implant Failure – https://shoalcreeksmilestudio.com/5-signs-of-dental-implant-failure/
[3] What Are The 10 Year Outcomes Of Dental Implants In Narrow Alveolar Ridges – https://www.efp.org/publications-hub/jcp-digest/what-are-the-10-year-outcomes-of-dental-implants-in-narrow-alveolar-ridges/
[6] Dental Implant Risks Complications In 2026 – https://www.oceanicdental.com/resource/dental-implant-risks-complications-in-2026

Leave a Reply
Share your thoughts or ask a question about dental implants. Your email address will not be published.