Dental implants offer a durable and aesthetically pleasing solution for missing teeth, providing a foundation that mimics natural tooth roots. However, for these implants to integrate successfully and provide long-term stability, a crucial factor must be met: sufficient dental implant bone density requirements. Without adequate bone, the implant cannot properly fuse with the jawbone, leading to potential failure. For residents in Dallas, Texas, understanding these requirements is the first step toward exploring this popular tooth replacement option.
TL;DR
- Successful dental implant placement critically depends on adequate jawbone density and volume.
- The ideal bone density for implants is often classified as D2, offering a balance of strength and blood supply.
- Specific bone height (8-10mm) and width (5-7mm) are typically required for standard implants.
- Low bone density does not automatically disqualify you; bone grafting and other advanced techniques can often create the necessary support.
- A thorough 3D imaging assessment by a qualified dental professional is essential to evaluate your bone structure and determine the best treatment plan.
What Are the Bone Density Classifications for Dental Implants?
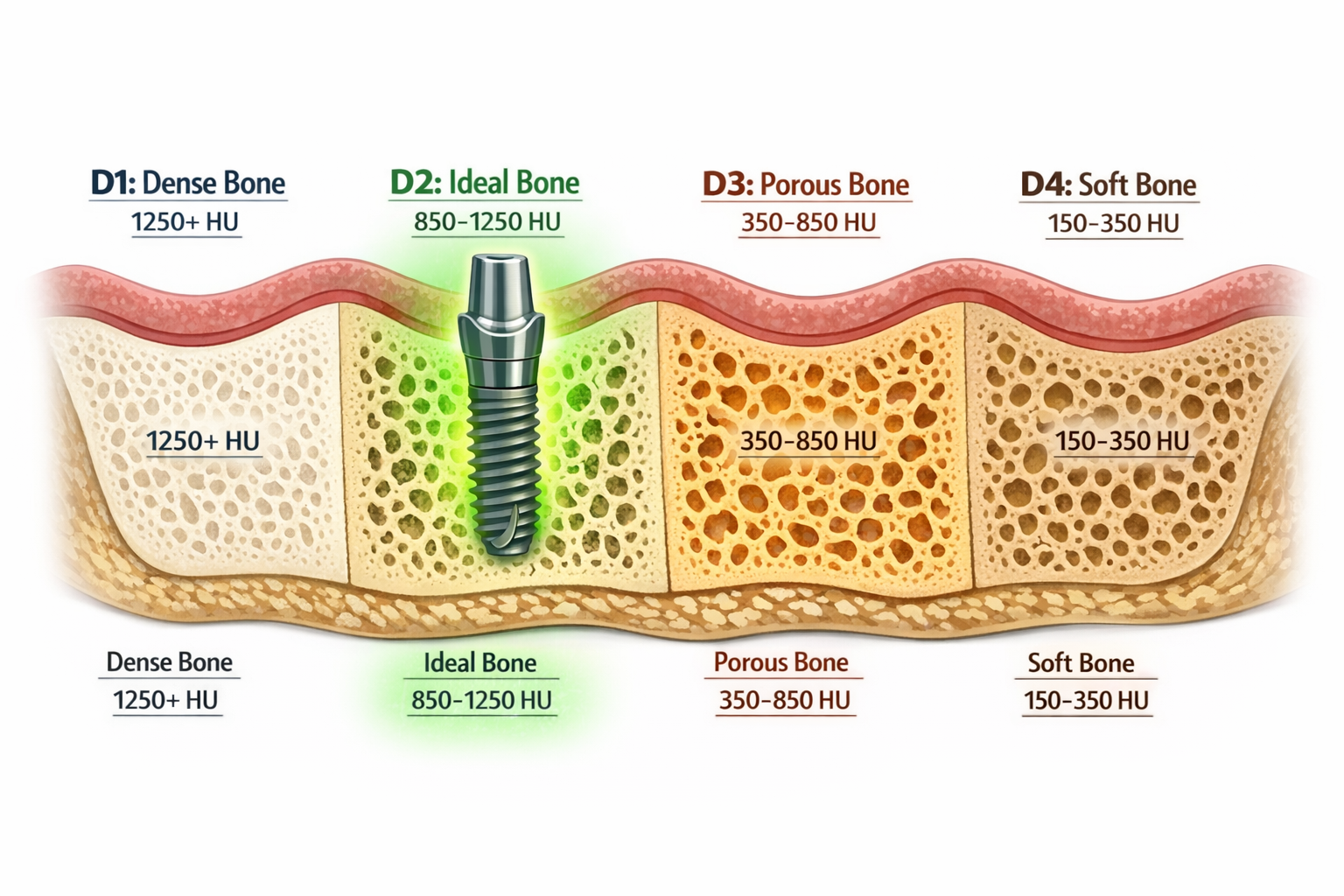
Bone density refers to the quantity and quality of bone present in your jaw, which directly impacts how well a dental implant can anchor and heal. Dentists classify bone density into four types, from D1 to D4, to help assess suitability for dental implant placement [3].
These classifications help your dental professional understand the structural support available and predict the success rate of the osseointegration process—the fusion of the implant with your natural bone.
Understanding the Bone Density Scale
- D1: Dense Cortical Bone. This type is very strong and hard, often found in the front of the lower jaw (anterior mandible). While it offers excellent initial stability for an implant, its limited blood supply can sometimes slow down the healing process [3]. Implants placed here typically require careful drilling techniques to prevent overheating the bone.
- D2: Dense Corticocancellous Bone. This is often considered the ideal bone type for dental implants [2, 9]. It combines a dense outer layer (cortical bone) with a rich, spongy inner core (cancellous bone). This balance provides strong initial stability along with a good blood supply, promoting optimal healing and osseointegration [2].
- D3: Porous Corticocancellous Bone. This bone type has a thinner cortical layer and a more porous cancellous interior. It’s common in the back of the upper jaw (posterior maxilla). While still suitable for implants, it may offer less initial stability than D1 or D2 bone, potentially requiring a longer healing period or a different implant placement strategy.
- D4: Very Porous Cancellous Bone. This is the softest and least dense bone type, frequently found in the back of the upper jaw. Placing implants in D4 bone presents challenges due to its low density, which can compromise initial stability and the success of osseointegration [2]. In many cases, bone grafting is necessary to augment D4 bone before implant placement.
Hounsfield Units (HU) in Bone Density Measurement
Beyond subjective classification, Hounsfield Units (HU) provide a more objective, quantitative measure of bone density, typically derived from Cone Beam Computed Tomography (CBCT) scans. This imaging technique gives your dentist a detailed 3D view of your jawbone.
- Optimal HU Range: For dental implants, bone density values between 850-1250 HU generally indicate good bone quality [2].
- Dense Cortical Bone: Scores above 850 HU.
- Soft Cancellous Bone: Measures between 150-400 HU [2].
A precise HU measurement allows your Dallas dental implant specialist to tailor the treatment plan, selecting the appropriate implant size and type for your specific bone structure.
What Are the Minimum Bone Volume Requirements (Height and Width)?
Beyond just density, the actual volume of your jawbone—its height and width—is equally critical for the successful placement and long-term stability of dental implants. Think of it like building a house: you need a strong foundation (density) and enough space to build on (volume).
Essential Dimensions for Dental Implants
For a standard dental implant, specific bone dimensions are generally required to ensure proper anchorage and to prevent damage to surrounding anatomical structures like nerves or sinuses.
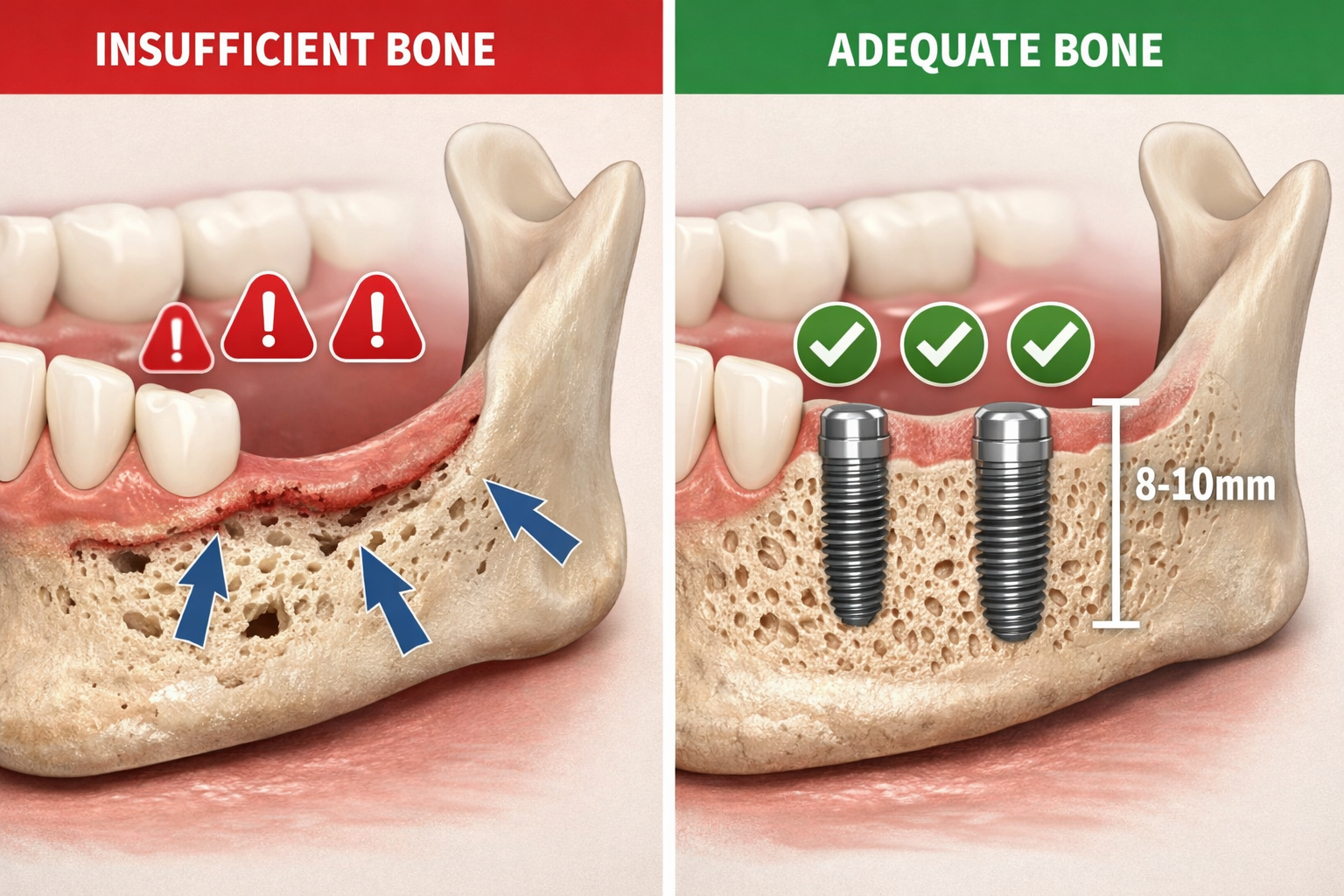
- Vertical Bone Height: At least 8-10 millimeters (mm) of vertical bone is typically necessary for standard implant placement [1, 4]. This height ensures that the implant can be securely embedded without encroaching on the sinus cavity in the upper jaw or the inferior alveolar nerve in the lower jaw. If insufficient height is present, a sinus lift or vertical bone augmentation may be recommended.
- Horizontal Bone Width: The jawbone should be at least 5-7 millimeters thick (wide) in the region where the implant will be placed [1, 4]. This width allows for sufficient bone to surround the implant on all sides, providing crucial stability and promoting successful osseointegration. A minimum of 1-2 millimeters of bone is required around all sides of the implant [5]. If the bone is too narrow, a horizontal ridge augmentation (bone graft) may be necessary.
Why are these dimensions so important?
- Primary Stability: Adequate height and width provide the initial mechanical stability that an implant needs immediately after surgery. This “primary stability” is crucial for the subsequent biological process of osseointegration [2].
- Osseointegration: Sufficient bone volume allows for a greater surface area for bone cells to grow into and fuse with the implant over time. This process typically takes three to six months [2].
- Protection of Adjacent Structures: Proper bone dimensions prevent the implant from impinging on vital structures, reducing the risk of complications such and nerve damage or sinus perforation [8].
- Long-Term Success: Implants placed in sufficient bone tend to have higher long-term success rates, better withstand chewing forces, and are less prone to complications like peri-implantitis (gum disease around the implant).
If you are considering dental implants in Dallas, your dentist will use advanced imaging, such as CBCT scans, to precisely measure these dimensions and determine if your jawbone meets the necessary dental implant bone density requirements. If not, they will discuss options to augment your bone.
Bone Volume Requirements for Different Implant Types
While standard implants have specific requirements, certain specialized implants can accommodate different bone volumes:
- Short Implants: These are shorter in length and can be used when vertical bone height is limited, sometimes avoiding the need for extensive bone grafting procedures.
- Narrow Implants: Used in areas with limited bone width, these implants have a smaller diameter than standard implants.
- Zygomatic Implants: For patients with severe bone loss in the upper jaw, zygomatic implants anchor into the cheekbone (zygoma) instead of the jawbone, bypassing the need for extensive sinus lifts and bone grafts. You can learn more about the cost of zygomatic dental implants in 2025 if this is an option for you.
Can You Still Get Dental Implants with Low Bone Density or Insufficient Bone Volume?
Yes, absolutely! Having low bone density or insufficient bone volume does not necessarily disqualify you from getting dental implants [7]. While meeting the ideal dental implant bone density requirements is preferred, modern dentistry offers several advanced techniques to address bone deficiencies and prepare the jaw for successful implant placement.
Solutions for Low Bone Density or Volume
For patients in Dallas who may not initially meet the optimal bone requirements, your dental implant specialist can recommend procedures to augment the existing bone:
- Bone Grafting: This is one of the most common procedures to increase bone volume. It involves adding bone material (either from your own body, a donor, animal source, or synthetic materials) to the deficient area of your jaw [7]. The graft stimulates your body to grow new, healthy bone.
- Types of Bone Grafts:
- Autogenous Graft: Bone taken from another part of your own body (e.g., hip, tibia, or another area of the jaw). This is often considered the gold standard as it contains living bone cells.
- Allograft: Bone from a human donor.
- Xenograft: Bone from an animal source, typically bovine (cow).
- Alloplast: Synthetic bone material.
- Healing Time: After a bone graft, it typically takes several months for the graft to integrate with your existing bone and create a strong foundation. You can read more about bone graft healing for dental implants for a detailed timeline.
- Cost Considerations: Bone grafting adds to the overall cost of the dental implant procedure. For information on this, see our article on decoding bone grafting costs for dental implants.
- Types of Bone Grafts:
- Sinus Lift (Sinus Augmentation): If you need implants in your upper back jaw and there isn’t enough bone height due to the maxillary sinuses being too close to the oral cavity, a sinus lift can be performed [7]. This procedure involves gently lifting the sinus membrane and placing bone graft material into the space, creating new bone for implant support.
- Ridge Augmentation: This procedure addresses deficiencies in the width or height of the jawbone ridge. Bone graft material is used to widen or heighten the bone, providing a more substantial base for implants.
- Guided Bone Regeneration (GBR): Often performed alongside other grafting procedures, GBR uses a barrier membrane to protect the bone graft material and guide the growth of new bone cells, preventing soft tissue from growing into the space where bone should form.
When is Bone Grafting Not an Option?
While bone grafting is highly effective, it may not be suitable for everyone. Factors like severe underlying health conditions, heavy smoking, or certain medications can impact the success of a bone graft. In such cases, your dentist may explore alternative tooth replacement options or consider specialized implant techniques that don’t rely as heavily on grafting.
Alternative Implant Strategies for Limited Bone
Even without extensive grafting, some implant designs can work with less-than-ideal bone:
- Mini Dental Implants (MDIs): These are smaller in diameter than traditional implants and can sometimes be placed in areas with less bone. They are often used to stabilize dentures.
- Tilting Implants (e.g., All-on-4® concept): In systems like All-on-4, implants are strategically angled to take advantage of existing denser bone, often in the front of the jaw, reducing the need for extensive grafting in the posterior areas.
The most crucial step is a comprehensive evaluation by an experienced dental implant specialist. Using advanced 3D imaging, they can accurately assess your bone density and volume, discuss all available options, and formulate a personalized treatment plan that ensures patient safety and long-term oral health.
How is Bone Density Assessed for Dental Implants?
Accurate assessment of bone density and volume is paramount before embarking on any dental implant procedure. It ensures that the treatment plan is safe, effective, and tailored to the individual patient’s anatomical needs. For those seeking dental implants in Dallas, your initial consultation will involve a thorough examination using state-of-the-art diagnostic tools.
Diagnostic Tools for Bone Assessment
- Clinical Examination: Your dentist will visually inspect your mouth and physically examine your jawbone and gums to identify any obvious signs of bone loss or other oral health issues. This initial step helps guide further imaging.
- Traditional X-rays (2D): While useful for general overview, traditional 2D X-rays (like panoramic X-rays or periapical films) provide limited information about bone density and cross-sectional bone volume. They offer a flattened image, making it difficult to gauge the precise width and 3D structure of the jawbone. However, they can show signs of significant bone loss or the presence of underlying pathology. You can learn more about optimal dental implant X-ray frequency for ongoing monitoring.
- Cone Beam Computed Tomography (CBCT) Scans: This is the gold standard for assessing dental implant bone density requirements. A CBCT scan provides highly detailed 3D images of your jawbone, nerves, and sinus cavities.
- Precise Measurements: CBCT allows your dental professional to measure the exact height, width, and angle of the bone in the proposed implant site.
- Bone Density Mapping: It helps categorize bone density using Hounsfield Units (HU), providing an objective measure of bone quality [2].
- Identification of Obstacles: The 3D view helps identify the precise location of nerves, blood vessels, and sinus membranes, crucial for avoiding complications during surgery [8].
- Treatment Planning: The detailed images enable your dentist to select the appropriate implant size, shape, and position, and to plan any necessary bone grafting procedures with high precision.
The Importance of a Comprehensive Evaluation
A thorough evaluation goes beyond just imaging. It includes:
- Medical History Review: Discussion of your general health, existing medical conditions (like osteoporosis or diabetes), and medications that could affect bone healing or implant success.
- Dental History: Understanding previous dental treatments, reasons for tooth loss, and oral hygiene habits.
- Lifestyle Factors: Habits like smoking or excessive alcohol consumption can negatively impact implant success and will be discussed.
- Discussion of Expectations: A clear conversation about your aesthetic and functional goals for your tooth replacement options.
By combining all this information, your dental implant specialist can accurately determine if you meet the necessary dental implant bone density requirements or if additional steps, such as bone grafting, are needed to ensure a predictable and successful outcome. This patient-first approach is key to informed decision-making and long-term oral health.
Why is Optimal Bone Density Critical for Implant Success?
Optimal bone density is not just a recommendation; it’s a fundamental requirement for the long-term success and stability of dental implants. The process hinges on a biological phenomenon called osseointegration, and bone quality plays a starring role.
The Role of Osseointegration
Osseointegration is the direct structural and functional connection between living bone and the surface of a load-bearing artificial implant. For dental implants, this means your jawbone cells must grow onto and fuse with the titanium surface of the implant, effectively making it a part of your jaw [2].
- Primary Stability: Immediately after implant placement, the implant relies on mechanical stability within the bone, known as primary stability. Higher bone density provides better primary stability, reducing micromovement of the implant [2].
- Secondary Stability: Over the next several months, secondary stability develops as your bone cells actively grow onto the implant surface. This biological fusion is what makes dental implants so strong and durable.
- Healing Timeline: Optimal bone density speeds up osseointegration. This creates stronger bonds between the natural bone and the implant, allowing for quicker progression to the final restoration phase [2]. The typical osseointegration process takes three to six months [2].
Risks Associated with Low Bone Density
When bone density is insufficient, several problems can arise, jeopardizing the success of the implant:
- Failed Osseointegration: If the bone lacks sufficient cells or minerals, osseointegration may not occur properly or can fail completely [2]. This means the implant will not fuse with the bone, remaining loose and eventually needing removal.
- Implant Instability: Even if osseointegration partially occurs, low bone density can lead to a weaker bond, making the implant less stable under chewing forces. This can result in implant movement or fracture.
- Increased Risk of Complications: Low bone density can increase the risk of implant complications, including infection around the implant (peri-implantitis) or even implant loss [8].
- Longer Healing Times: The body may take significantly longer to integrate the implant in less dense bone, prolonging the overall treatment process.
Success Rates and Bone Density
Research consistently shows a strong correlation between adequate bone density and high implant success rates. Patients with a minimum bone density of 1.2 g/cm³ have demonstrated success rates of up to 90% [10]. While bone density is crucial, it’s also important to remember that overall patient health, oral hygiene, and the skill of the dental implant specialist significantly contribute to success.
For individuals considering dental implants in Dallas, understanding these fundamental principles helps manage expectations and underscores the importance of a thorough diagnostic phase to assess dental implant bone density requirements. It also highlights why procedures like bone grafting, though they extend treatment time and cost, are vital investments in the long-term success of your implant.
Table: Bone Density Classification and Implications for Dental Implants
Understanding the different types of bone density and their implications is crucial for anyone considering dental implants. This table summarizes the classifications and their impact on implant treatment.
| Bone Density Type | Characteristics | Hounsfield Units (HU) | Implications for Dental Implants |
|---|---|---|---|
| D1 | Very dense, cortical bone (e.g., anterior mandible) | > 850 | Excellent initial stability; slower healing due to lower blood supply. Requires careful surgical technique to avoid overheating. |
| D2 | Dense cortical layer with dense cancellous core | 850-1250 | Ideal bone for implants [2, 9]. Provides strong initial stability and good blood supply for optimal osseointegration and healing. |
| D3 | Thinner cortical layer, porous cancellous core | 350-850 | Good for implants but may have less initial stability. May require longer healing or specific implant types/placement. |
| D4 | Very porous, soft cancellous bone (e.g., posterior maxilla) | < 350 | Challenging for implants due to low initial stability. Often requires bone grafting before implant placement [2]. |
Note: Hounsfield Unit ranges are general guidelines and may vary slightly based on specific imaging equipment and interpretation.
What Happens if Bone Density is Found to Be Insufficient?
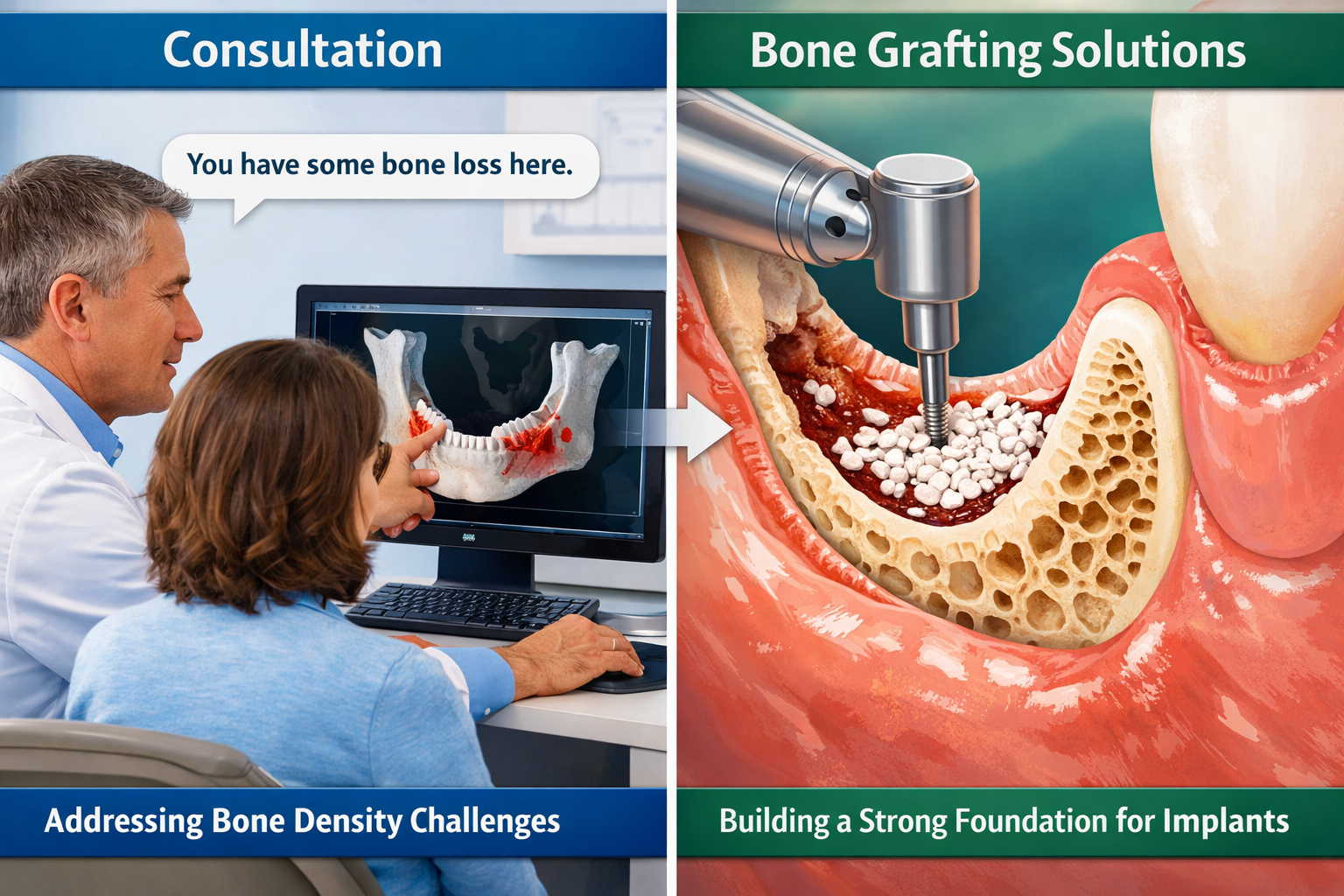
Discovering that your bone density or volume is insufficient for immediate dental implant placement can be disheartening, but it’s far from the end of your journey to a restored smile. For patients in Dallas, if your initial assessment reveals that you don’t meet the dental implant bone density requirements, your dental professional will discuss several well-established strategies to improve your candidacy.
Step-by-Step Approach to Addressing Insufficient Bone
- Comprehensive Discussion: Your dentist will clearly explain why your bone density is insufficient, using your 3D imaging results to illustrate the specific areas of concern. They will outline all viable solutions, potential risks, benefits, and the expected timeline. This is a critical opportunity to ask questions to ensure you understand your tooth replacement options fully.
- Bone Grafting Recommendations: As previously discussed, bone grafting is the most common solution. Based on the type and extent of bone loss, your dentist will recommend a specific type of graft (e.g., sinus lift, ridge augmentation, or a more localized graft).
- Decision Rule: Choose bone grafting if you desire dental implants and your bone deficiency is localized and treatable.
- Common Mistake: Rushing into implant placement without allowing adequate healing time post-graft. The graft needs time to integrate and mature into viable bone.
- Healing Period: Following a bone graft, a dedicated healing period is essential. This can range from a few months to over a year, depending on the graft type and individual healing capabilities [7]. During this time, the grafted material integrates with your natural bone, forming a strong, dense foundation. Regular follow-up appointments will monitor the healing progress.
- Re-evaluation: Once the healing period is complete, another CBCT scan will be performed to re-evaluate the bone density and volume. This confirms that the bone has regenerated sufficiently to meet the dental implant bone density requirements for successful implant placement.
- Implant Placement: If the re-evaluation shows adequate bone, the dental implant surgery can proceed.
- Alternative Treatment Options: In cases where bone grafting is not feasible, desired by the patient, or has a low probability of success, your dentist may discuss alternative missing teeth solutions such as:
- Dental Bridges: A traditional option that uses adjacent teeth as anchors. Learn more about dental implant versus bridge cost.
- Removable Partial or Full Dentures: Though less stable than implants, modern dentures can be comfortable and aesthetically pleasing. Consider removable dental implant options for a stable smile for a hybrid approach.
- Specialized Implants: As mentioned, options like mini dental implants or zygomatic implants may be considered in specific severe cases to bypass the need for extensive bone grafting.
The journey to dental implants, especially when bone augmentation is needed, requires patience and a commitment to the treatment plan. However, the long-term benefits of a stable, functional, and aesthetically pleasing smile often make these extra steps a worthwhile investment in your oral health. A consultation with a dentist specializing in dental implants is the best way to understand your individual situation and available options.
FAQ: Dental Implant Bone Density Requirements
Here are answers to common questions about bone density and dental implants, particularly for those researching dental implants in Dallas, Texas.
Q1: What is the ideal bone density for dental implants?
The ideal bone density is typically classified as D2 bone, which offers a balance of cortical (dense outer) and cancellous (spongy inner) bone, providing both strong initial stability and good blood supply for healing [2, 9].
Q2: How much bone height and width do I need for an implant?
Generally, you need at least 8-10 millimeters of vertical bone height and 5-7 millimeters of horizontal bone width for standard dental implant placement [1, 4]. A minimum of 1-2 millimeters of bone is required around all sides of the implant [5].
Q3: Can I get dental implants if I have low bone density?
Yes, in many cases, you can still get dental implants even with low bone density. Procedures like bone grafting (sinus lifts, ridge augmentation) can augment the existing bone, creating sufficient support for the implant [7].
Q4: How is my bone density measured?
Bone density is primarily assessed using Cone Beam Computed Tomography (CBCT) scans, which provide detailed 3D images of your jawbone. These scans can also measure bone density in Hounsfield Units (HU) [2].
Q5: How long does bone grafting take to heal before implant placement?
The healing time after a bone graft varies depending on the type and extent of the graft, but it typically ranges from three to twelve months before the jawbone is ready for implant placement.
Q6: What are Hounsfield Units (HU) and why are they important?
Hounsfield Units are a quantitative measure of bone density obtained from CBCT scans. Values between 850-1250 HU are generally considered good for dental implant success, providing an objective assessment of bone quality [2].
Q7: Are there alternatives to bone grafting for low bone density?
In some specific cases, alternatives like short implants, narrow implants, or strategically angled implants (e.g., All-on-4 concept) may be used. For severe bone loss in the upper jaw, zygomatic implants might be an option.
Q8: What happens if I don’t have enough bone for an implant and don’t get a graft?
If an implant is placed in insufficient bone, it may not achieve proper osseointegration, leading to implant instability, failure, or potential damage to surrounding anatomical structures [2, 8].
Q9: Does osteoporosis affect dental implant success?
Osteoporosis can affect bone density, but it doesn’t automatically rule out dental implants. Your dentist will carefully evaluate your condition, medications, and overall bone health to determine if implants are a safe and viable option.
Q10: What is osseointegration and how does bone density affect it?
Osseointegration is the process where the dental implant fuses directly with your living jawbone. Optimal bone density provides better primary stability and a richer environment for bone cells to grow, speeding up and strengthening this crucial fusion process [2].
Key Takeaways
- Bone Density is Foundational: Adequate bone density and volume are non-negotiable for successful dental implant integration and long-term stability.
- D2 Bone is Ideal: Type D2 bone, characterized by a balance of dense cortical and cancellous bone, is generally considered the most favorable for dental implants due to its strength and good blood supply [2, 9].
- Specific Dimensions Matter: Standard implants require specific bone height (8-10mm) and width (5-7mm) to ensure proper placement and avoid anatomical structures [1, 4].
- Low Bone Density is Often Treatable: Insufficient bone does not automatically disqualify you. Advanced procedures like bone grafting (sinus lifts, ridge augmentation) can effectively build up the necessary bone volume [7].
- Advanced Imaging is Key: Cone Beam Computed Tomography (CBCT) scans are essential for accurately assessing your unique bone structure, density (via Hounsfield Units), and planning your personalized treatment [2].
- Consultation is Crucial: A comprehensive consultation with an experienced dental implant specialist in Dallas is the first and most important step to evaluate your specific dental implant bone density requirements and explore your best tooth replacement options.
- Patience for Grafting: If bone grafting is needed, allow for the recommended healing time (several months) to ensure the graft fully integrates and matures before implant placement.
Conclusion
Understanding the dental implant bone density requirements is a critical aspect of your journey towards restoring your smile with dental implants. While these requirements are stringent, they are designed to ensure the highest possible success rate and longevity for your investment in long-term oral health. Whether your bone structure is naturally robust or requires augmentation through advanced procedures like bone grafting, the goal remains the same: to create a stable, healthy foundation for your new tooth.
For those considering dental implants in Dallas, we emphasize the importance of seeking out a qualified and experienced dental implant professional. They will utilize advanced diagnostic tools, such as CBCT scans, to accurately assess your individual bone density and volume. This thorough evaluation will allow them to discuss all available options, including bone augmentation procedures if necessary, to help you achieve your goal of a healthy, confident smile. Don’t let concerns about bone density deter you from exploring this life-changing tooth replacement option; with modern dental science, solutions are often available.
Actionable Next Steps:
- Schedule a Consultation: Contact a local dental implant specialist in Dallas, Texas, for a comprehensive evaluation.
- Undergo 3D Imaging: Request a CBCT scan to get an accurate assessment of your bone density and volume.
- Discuss All Options: Have an open conversation with your dentist about your specific bone conditions, potential bone grafting needs, and overall treatment plan.
- Ask Questions: Be prepared with questions about the dental implant procedure, implant cost in Dallas, healing times, and maintenance to ensure you make an informed decision.
References
[1] How Much Bone Do You Need For Dental Implants – https://www.rankmydentist.com/kb/dental-implants/how-much-bone-do-you-need-for-dental-implants
[2] Bone Density And Implant Success – https://www.renaissancedentalimplant.com/blog/bone-density-and-implant-success/
[3] Bone Density Requirement For Dental Implants – https://www.minotdentalpartners.com/blog/bone-density-requirement-for-dental-implants/
[4] Dental Implant Candidacy Criteria – https://www.northwestoralsurgeons.com/blog/dental-implant-candidacy-criteria/
[5] Denture Implants For Low Bone Density – https://www.imagineyoursmile.com/blog/denture-implants-for-low-bone-density/
[7] Can You Still Get Dental Implants With Low Bone Density – https://www.drdeanglasser.com/dental-implants/can-you-still-get-dental-implants-with-low-bone-density/
[8] Dental Implant Risks Complications In 2026 – https://www.oceanicdental.com/resource/dental-implant-risks-complications-in-2026
[9] Bone Density For Dental Implants – https://adalyadentalclinic.com/bone-density-for-dental-implants/
[10] Bone Density Success Dental Implants – https://www.allsmilesdentalcare.ca/bone-density-success-dental-implants/

Leave a Reply
Share your thoughts or ask a question about dental implants. Your email address will not be published.