Choosing dental implants is a significant step towards restoring your oral health and smile, especially if you’re exploring tooth replacement options in Dallas. But what exactly makes these modern tooth replacements so effective and long-lasting? The answer lies in the sophisticated field of dental implant biomechanics, which examines how forces interact with dental implants and the surrounding bone tissue. Understanding these principles is crucial for both dentists and patients, ensuring the success and longevity of your dental implant procedure.
Key Takeaways
- Dental implant biomechanics is the study of forces on implants and their interaction with bone.
- Osseointegration is fundamental, creating a direct bond between the implant and bone.
- Implant design, material, and surface play crucial roles in how forces are managed.
- Proper force distribution prevents complications like implant failure or bone loss.
- Patient-specific factors, such as bone density and bite forces, significantly influence outcomes.
- Advanced planning and technology, like 3D guided surgery, optimize biomechanical success.
- Regular maintenance and addressing issues like grinding are vital for long-term implant health.
- Consulting with a dentist who understands these principles is essential for successful dental implants in Dallas.
Quick Answer
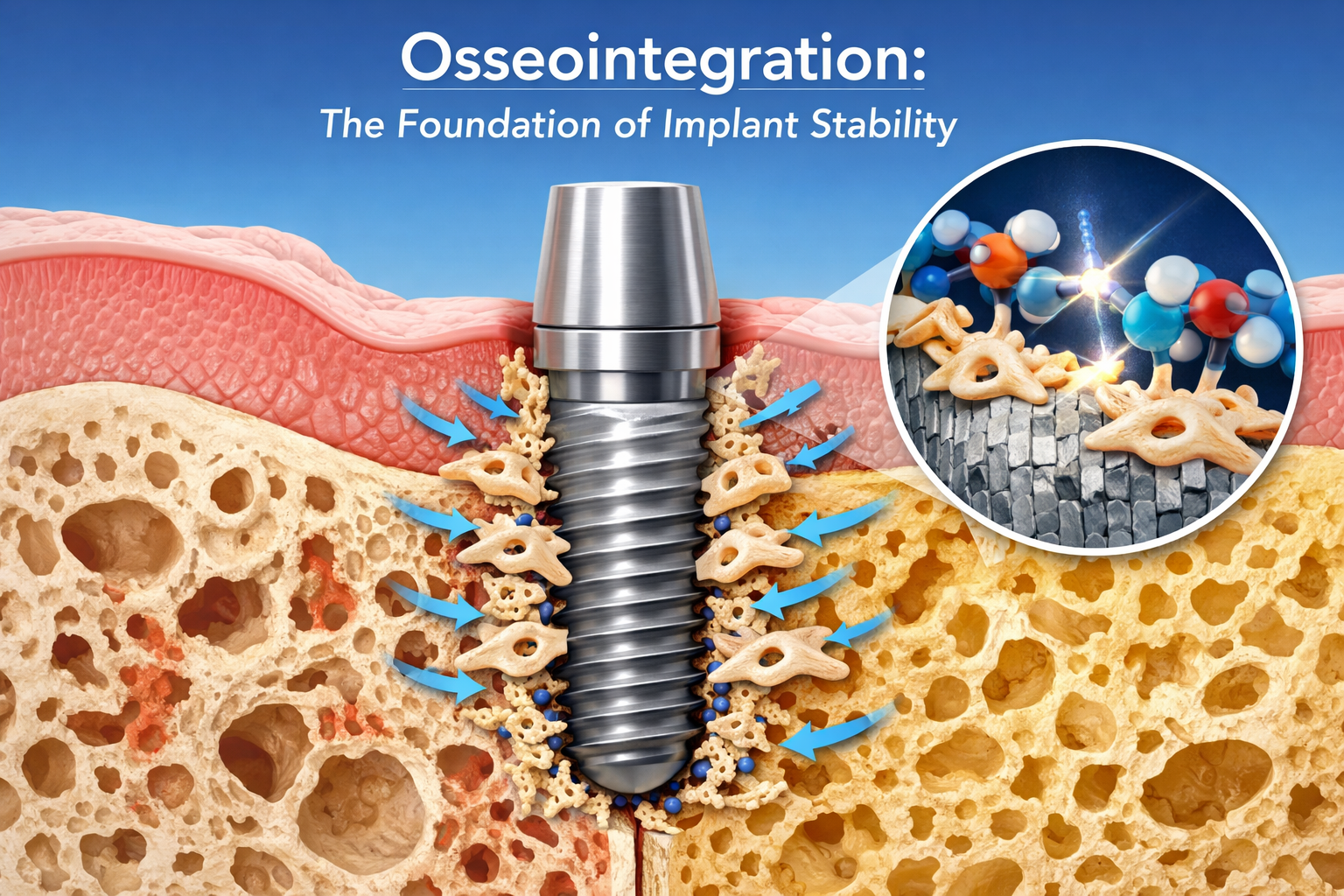
Dental implant biomechanics refers to the scientific principles governing how forces are absorbed, distributed, and managed by a dental implant system within the jawbone and surrounding tissues. This field ensures that implants can withstand daily chewing forces while promoting a stable, long-lasting connection with the bone, which is vital for preventing complications and ensuring the functional success of the restoration.
What is Osseointegration and Why is it Key to Dental Implant Biomechanics?
Osseointegration is the critical biological process where a dental implant forms a direct, structural, and functional connection with the living bone, acting as the foundation for the implant’s stability and success. Without proper osseointegration, the implant cannot adequately support the forces of chewing and speaking, which is a core concept in dental implant biomechanics.
Osseointegration is not merely the implant sitting in bone; it’s a dynamic biological process where bone cells grow directly onto and into the surface of the implant. This firm anchorage allows the implant to function like a natural tooth root, transmitting forces directly to the jawbone, which in turn helps stimulate and preserve bone density. Factors affecting osseointegration include:
- Implant Material: Biocompatible materials like titanium or zirconia are preferred because they don’t cause adverse reactions and actively encourage bone growth.
- Surface Treatment: The implant’s surface is often treated to create microscopic roughness, which increases the surface area for bone cells to attach and can accelerate the osseointegration process.
- Surgical Technique: Minimally traumatic surgery is essential to preserve bone vitality and allow for optimal healing. Precise implant placement also plays a role in how well forces are distributed later.
- Bone Quality and Quantity: Sufficient healthy bone is necessary for the implant to integrate. Patients with insufficient bone may require a bone graft before implant placement.
If osseointegration is compromised, the implant can become mobile, leading to pain, discomfort, and eventually implant failure. This highlights why ensuring successful osseointegration is the primary objective of the initial phases of the dental implant procedure.

How Do Forces Affect Dental Implants and Surrounding Bone?
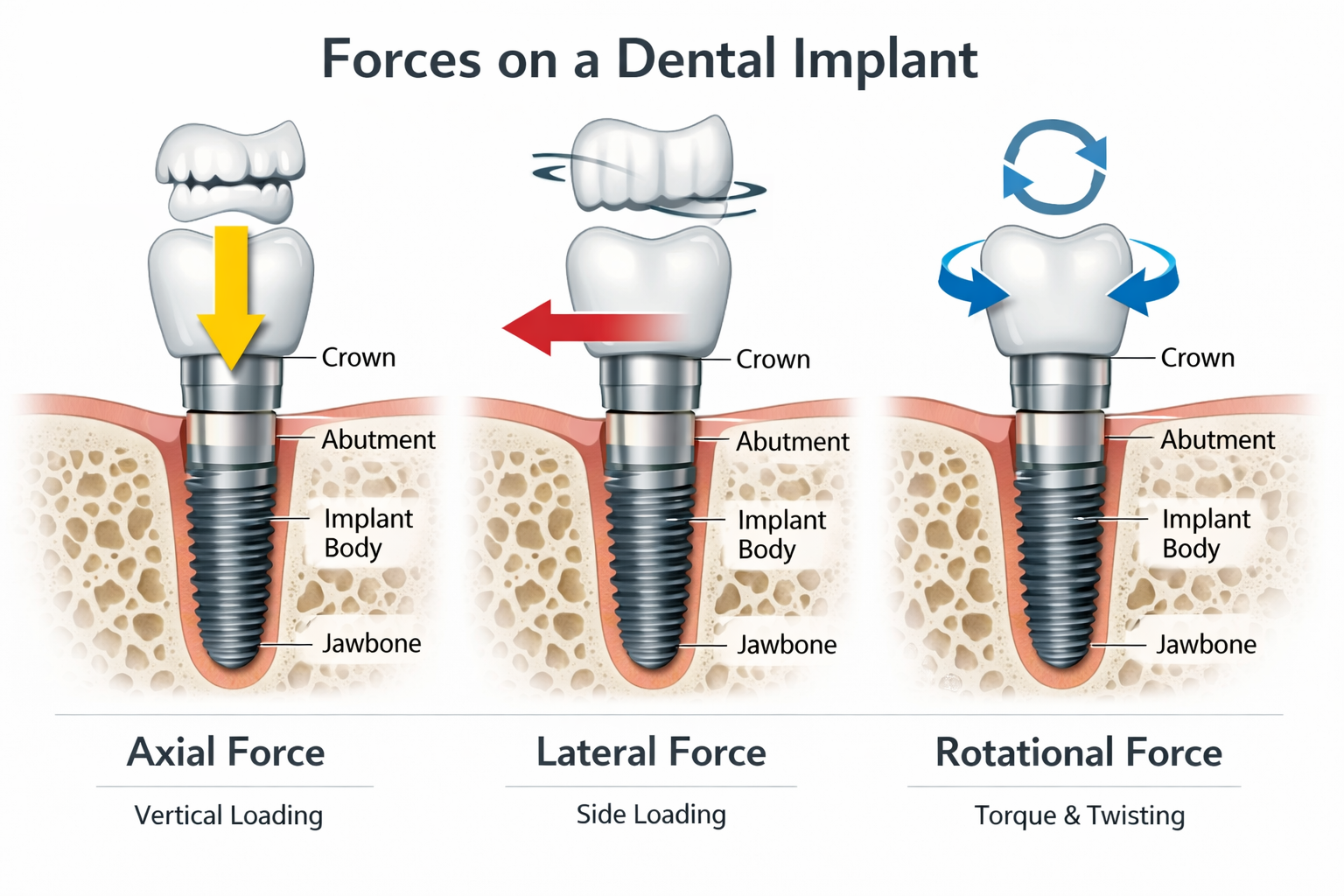
Forces applied to dental implants, primarily from biting and chewing (occlusal forces), directly influence the implant’s long-term stability and the health of the surrounding bone. Understanding these force dynamics is central to dental implant biomechanics, as excessive or misdirected forces can lead to complications such as bone loss, implant fracture, or even implant failure.
The way forces are transferred from the prosthetic crown, through the abutment, and down to the implant body is critical. Ideally, these forces should be distributed evenly along the implant and into the surrounding bone, mimicking the natural tooth. However, several factors can alter this:
- Magnitude of Force: Patients with strong bite forces or habits like bruxism (teeth grinding) apply greater stress, potentially overloading the implant system. A night guard is often recommended to protect implants from excessive nocturnal forces. For more details on protecting your investment, read about the dental implant night guard.
- Direction of Force: Axial forces (straight down) are generally well-tolerated as they distribute stress evenly. Lateral or off-axis forces, however, create bending moments that can concentrate stress at the crestal bone (the bone directly around the top of the implant), potentially leading to bone resorption.
- Implant Location: Implants in the posterior (back) regions of the mouth typically endure heavier chewing forces than those in the anterior (front). This difference influences material selection and implant design.
- Number of Implants: Using multiple implants to support a bridge or full-arch restoration helps distribute forces across a wider area, reducing stress on individual implants. This is a key principle in solutions like All-on-4 dental implants.
Excessive force can lead to what’s known as “biomechanical overload.” This doesn’t necessarily mean the implant will immediately break, but it can trigger a biological response in the bone where it starts to resorb, leading to peri-implantitis (inflammation around the implant) and ultimately implant mobility. Therefore, meticulous planning of the bite and occlusal scheme is a cornerstone of successful implant dentistry.

How Do Implant Design and Materials Influence Dental Implant Biomechanics?
The physical design and material composition of a dental implant are engineered to optimize its interaction with the jawbone and manage occlusal forces, forming a crucial aspect of dental implant biomechanics. These choices directly impact osseointegration, stress distribution, and the long-term success of the implant.
Key Aspects of Implant Design and Materials:
Implant Body Shape:
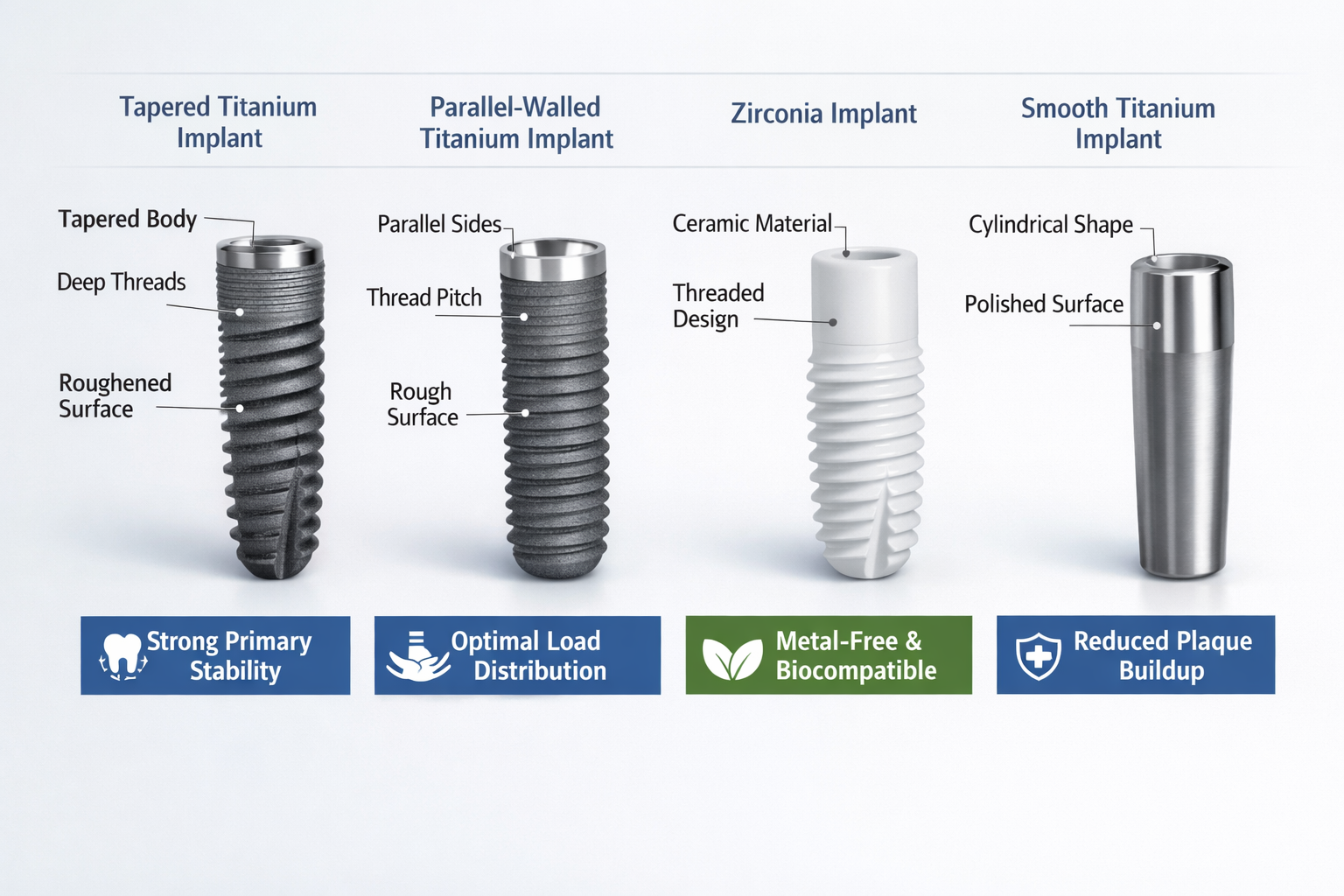
- Cylindrical/Parallel-Walled: These implants have a consistent diameter along their length and primarily rely on the bone-to-implant contact area for stability.
- Tapered: Tapered implants mimic the natural root shape, allowing for increased primary stability immediately after placement, especially in softer bone. They can also aid in load distribution.
- Thread Design: The threads on an implant are not just for insertion. The pitch (distance between threads) and depth influence how stress is distributed to the bone. Deeper, wider threads can increase the surface area for bone contact and improve load transfer.
Implant Dimensions:
- Diameter: Wider implants provide a larger surface area for osseointegration and can better withstand forces, particularly in areas of high stress like molars.
- Length: Longer implants offer more bone-to-implant contact, enhancing stability. However, anatomical limitations (like nerves or sinuses) often dictate maximum length.
Material Composition:
- Titanium: The gold standard, titanium is biocompatible, corrosion-resistant, and strong. Its ability to osseointegrate effectively is well-documented.
- Zirconia: A ceramic material, zirconia offers excellent aesthetics due to its tooth-like color and is highly biocompatible. It’s an alternative for patients with metal allergies or those seeking a metal-free option. For a comparison of maintenance, see our guide on Titanium vs Zirconia Implant Maintenance.
Surface Treatment:
- Roughness: Micro-roughened surfaces (e.g., sandblasted, acid-etched) increase the surface area, promoting faster and stronger bone apposition.
- Biologically Active Coatings: Some implants feature coatings (e.g., hydroxyapatite) designed to further enhance bone cell attachment and growth.
The selection of implant design and material is a critical decision made by your dental professional based on your specific bone quality, location of the missing tooth, and overall treatment plan. This careful consideration ensures optimal biomechanical performance for your long-term oral health.
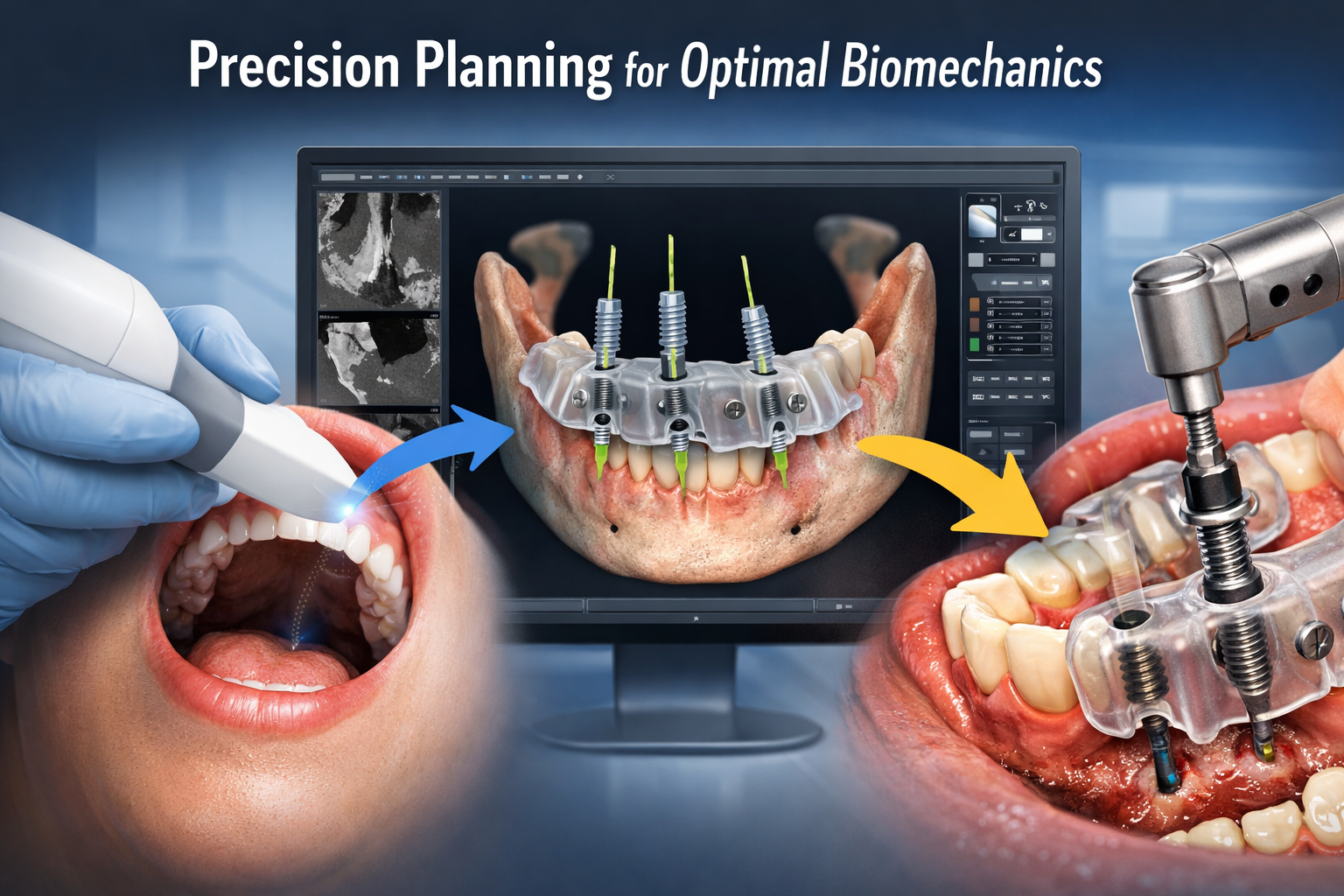
How Does Precision Planning and Technology Optimize Biomechanics for Dental Implants in Dallas?
Precision planning, often utilizing advanced technologies like 3D imaging and computer-guided surgery, is crucial for optimizing the biomechanics of dental implants. For patients seeking dental implants in Dallas, this approach enhances safety, predictability, and long-term success by ensuring optimal implant placement.
Role of Advanced Technology:
3D Cone Beam Computed Tomography (CBCT):
- Detailed Anatomical Mapping: CBCT scans provide a comprehensive 3D view of the patient’s jawbone, including bone density, nerve pathways, sinus cavities, and the exact dimensions of the bone. This eliminates guesswork.
- Bone Quality Assessment: Dentists can accurately assess bone volume and density, which are critical for determining the appropriate implant size and predicting osseointegration success.
- Identification of Risks: Critical structures like nerves and blood vessels are clearly visualized, allowing the surgical team to avoid them during placement.
Computer-Guided Implant Planning Software:
- Virtual Implant Placement: Dentists use specialized software to virtually place the implant in the ideal position, considering biomechanical factors such as bone availability, angulation relative to opposing teeth, and optimal force distribution.
- Prosthetic-Driven Planning: The software allows planning the implant’s position based on the final prosthetic crown’s ideal position, ensuring the restoration will function correctly and look natural. This is particularly important for dental implants for missing front teeth.
Surgical Guides:
- Precision and Accuracy: Based on the 3D plan, a custom surgical guide (often 3D-printed) is created. This guide fits over the patient’s existing teeth or gums and dictates the exact angle, depth, and position for drilling the implant site.
- Reduced Trauma: Guided surgery minimizes the invasiveness of the procedure, leading to less post-operative pain and faster healing.
- Optimal Biomechanics: By ensuring implants are placed in the precise, pre-planned position, guided surgery significantly optimizes force distribution and long-term implant stability, reducing the risk of biomechanical overload.
This level of precision in the implant surgery process leads to predictable outcomes, enhanced patient safety, and a higher success rate for dental implants, reinforcing their value as a durable missing teeth solution.
Conclusion
Understanding dental implant biomechanics is fundamental to appreciating the sophistication and success of modern dental implants. From the initial biological process of osseointegration to the intricate interplay of forces, materials, and design, every aspect contributes to the long-term stability and functionality of your tooth replacement. Advanced planning and technology, particularly 3D imaging and computer-guided surgery, further enhance precision, ensuring that your implant can withstand the demands of daily life and provide a durable solution for missing teeth.
If you are considering dental implants in Dallas, it’s essential to consult with a dental professional who possesses a deep understanding of these biomechanical principles. They can assess your individual needs, bone quality, and bite dynamics to design a treatment plan that optimizes the success and longevity of your investment. Don’t hesitate to seek a consultation with a dentist to explore how dental implants can restore your smile and improve your long-term oral health.
FAQ

What is the most important factor for dental implant success from a biomechanical perspective?
The most important biomechanical factor for dental implant success is successful osseointegration, which establishes a direct, stable connection between the implant and the bone, allowing for proper force distribution.
Can teeth grinding (bruxism) affect dental implant biomechanics?
Yes, bruxism can significantly impact dental implant biomechanics by introducing excessive, non-axial forces that can lead to bone loss around the implant, implant fracture, or even failure over time. A night guard is often recommended.
How long do dental implants typically last, considering biomechanical factors?
With proper osseointegration, optimal biomechanical loading, good oral hygiene, and regular dental check-ups, dental implants can last for many decades, often a lifetime. Poor biomechanics can significantly reduce their lifespan.
Are wider or longer implants always better biomechanically?
Wider and longer implants generally offer more surface area for osseointegration and can better distribute forces. However, anatomical constraints and bone quality often dictate the appropriate implant dimensions, making “always better” an oversimplification.
What role does the implant material play in biomechanics?
Biocompatible materials like titanium and zirconia are crucial because they integrate well with bone and can withstand chewing forces. Titanium is known for its strength and osseointegration properties, while zirconia offers aesthetic benefits and metal-free alternatives.
How does a dental professional ensure optimal biomechanics during the planning phase?
Dental professionals use 3D imaging (CBCT scans) and specialized software to virtually plan the ideal implant position, considering bone density, anatomical structures, and the final prosthetic’s position to ensure balanced force distribution.
Can an implant fail due to poor biomechanics even after successful osseointegration?
Yes, even after successful osseointegration, chronic excessive or misdirected forces (biomechanical overload) can lead to complications such as peri-implantitis (inflammation around the implant) or late-stage implant failure.
What are axial versus lateral forces in dental implant biomechanics?
Axial forces are directed straight down the long axis of the implant, which are generally well-tolerated. Lateral (or off-axis) forces are applied at an angle, creating bending moments that can concentrate stress and be more detrimental to the implant-bone interface.
References
- Branemark, P.I., Zarb, G.A., & Albrektsson, T. (1985). Tissue-Integrated Prostheses: Osseointegration in Clinical Dentistry. Quintessence Publishing Co.
- Misch, C.E. (2008). Contemporary Implant Dentistry. Mosby Elsevier.

Leave a Reply
Share your thoughts or ask a question about dental implants. Your email address will not be published.