Quick Answer: Yes, you absolutely can get peri-implantitis even with good oral hygiene. While excellent daily oral care is crucial for the long-term success of dental implants, various other factors, including systemic health conditions, a history of gum disease, and certain implant design elements, can increase your risk of developing this inflammatory condition around your implants [5, 7].
Key Takeaways
- Peri-implantitis Risk is Multifactorial: Good oral hygiene alone is not a guarantee against peri-implantitis.
- Systemic Conditions Play a Role: Diabetes, smoking, and heart disease significantly increase risk [5].
- Prior Gum Disease is a Major Factor: A history of periodontitis makes you more susceptible [5].
- Implant Design Matters: Crown and abutment design can create areas difficult to clean, even with diligent care [7].
- Soft Tissue Health: Insufficient gum tissue around the implant elevates risk [5].
- Regular Professional Care is Essential: Consistent dental check-ups and cleanings are vital for early detection and prevention.
- Early Detection is Key: Peri-implantitis progresses faster than natural gum disease, making prompt intervention critical [5].
Understanding Peri-Implantitis: More Than Just Plaque
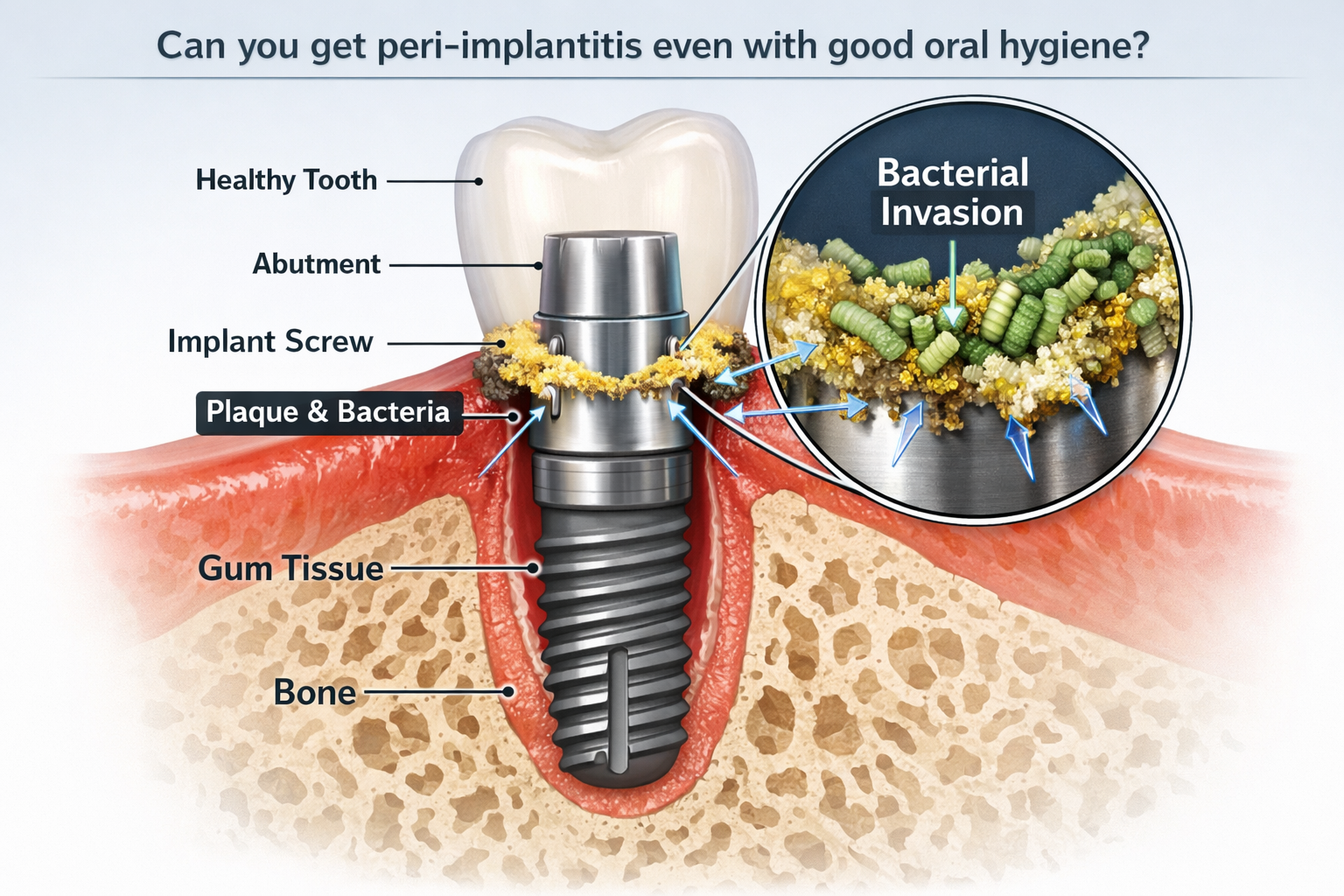
Peri-implantitis is an inflammatory condition affecting the tissues surrounding a dental implant, characterized by inflammation of the peri-implant mucosa (gums) and progressive loss of supporting bone [3]. While poor oral hygiene and plaque accumulation are primary contributors to peri-implant diseases, it is important to understand that these conditions can develop even in individuals who meticulously care for their teeth and implants daily. This means that while brushing and flossing are necessary, they are not always sufficient to prevent all cases of peri-implantitis.
Peri-implantitis is defined by several key features:
- Inflammation of the Soft Tissues: Redness, swelling, and bleeding around the implant.
- Progressive Bone Loss: A hallmark of the condition, leading to reduced support for the implant.
- Pus Formation: In advanced stages, pus may be present.
- Increased Probing Depths: The gum pocket around the implant becomes deeper.
For patients with missing teeth solutions, understanding the risks and preventive measures for their dental implants in Dallas is paramount for long-term oral health.
Why Can You Get Peri-Implantitis Even With Good Oral Hygiene?
You can get peri-implantitis even with good oral hygiene because several non-hygiene-related factors significantly influence the health and longevity of dental implants. These factors often interact with plaque accumulation, exacerbating the inflammatory response or making the implant more vulnerable to bacterial invasion [5]. For example, certain medical conditions can alter the body’s immune response, making it harder to fight off infections even with optimal cleaning.
Key non-hygiene risk factors include:
Systemic Health Conditions:
- Smoking: Tobacco use is a well-established risk factor, significantly impairing healing and increasing susceptibility to infection around implants [5]. If you are considering dental implants in Dallas, it’s crucial to discuss smoking habits with your dentist.
- Diabetes: Poorly controlled diabetes can compromise the immune system and impair bone metabolism, increasing the risk of peri-implantitis [5].
- Cardiovascular Disease: Certain heart conditions and associated medications may indirectly affect oral health and implant stability [5].
- Immunosuppression: Conditions or medications that suppress the immune system can make individuals more vulnerable to infections [5].
- Osteoporosis: While not a direct cause, severe osteoporosis can affect bone density and healing capacity, potentially impacting implant outcomes.
History of Periodontal Disease:
- Individuals with a history of periodontitis (gum disease) are at a substantially higher risk for peri-implantitis, even after successful treatment of their natural teeth [5].
- Periodontal pathogens, such as Aggregatibacter actinomycetemcomitans, Porphyromonas gingivalis, and Prevotella intermedia, can persist or recur years later, leading to inflammation around implants [5]. This is a critical consideration for anyone seeking missing teeth solutions with dental implants. Our article on “Peri-Implantitis Prevention Dallas: Early Signs, Treatment C” can offer more insight into this.
Genetic Predisposition:
- Some individuals may have a genetic susceptibility to inflammatory diseases, including those affecting dental implants.
Occlusal Overload (Excessive Biting Forces):
- While controversial, some research suggests that excessive biting forces on an implant can contribute to bone loss, especially in combination with bacterial factors [3]. This type of stress can lead to micro-trauma, potentially initiating or accelerating peri-implantitis.
Quality and Quantity of Gingival and Mucosal Tissue:
- Patients with insufficient or thin soft tissue around their implants are at an elevated risk of peri-implantitis, regardless of their oral care practices [5]. Adequate keratinized mucosa provides a protective barrier and is easier to clean.
The Role of Implant Design and Placement in Peri-Implantitis
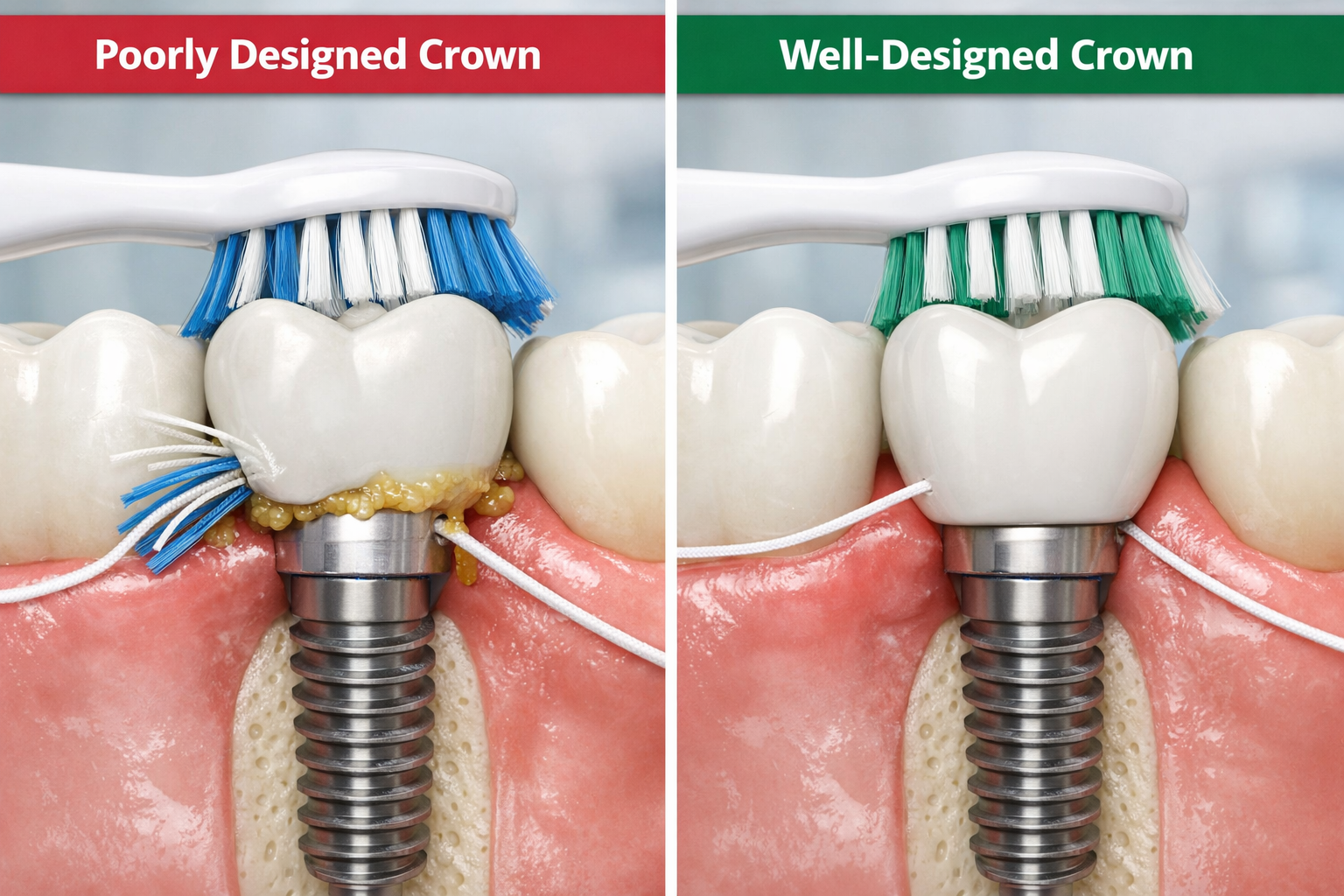
Implant crown and abutment design can indeed obstruct proper cleaning, making certain implant configurations inherently more difficult to maintain plaque-free, even for patients with excellent oral hygiene practices [7]. The way an implant is designed and placed directly influences how accessible it is for cleaning, which in turn impacts the risk of peri-implantitis.
Factors related to implant design and placement that can contribute to peri-implantitis:
Crown Design and Contours:
- Overhangs: Crowns that extend too far beyond the implant abutment can create ledges where plaque and food debris accumulate, making it impossible to clean effectively with a toothbrush or floss [7].
- Bulky Contours: Overly bulky or wide crowns can encroach on the gum tissue, making it difficult to access the implant collar for proper cleaning.
- Emergence Profile: The way the crown emerges from the gum line must be smooth and natural, allowing for easy cleaning. An abrupt or sharp emergence profile can create plaque traps.
Abutment Design:
- Connection Type: The connection between the implant and the abutment (the part that connects the implant to the crown) can sometimes harbor bacteria, especially if the seal is not perfect.
- Abutment Height and Shape: A short or poorly contoured abutment can make it challenging to create a cleansable crown.
Implant Position and Angulation:
- Too Deep or Too Shallow Placement: Implants placed too deep subgingivally can make the implant-abutment interface inaccessible for cleaning and more prone to bacterial colonization. If an implant is too shallow, it might not have adequate bone support.
- Angulation: An implant placed at an awkward angle can result in an improperly aligned crown, leading to difficult-to-clean areas or uneven biting forces.
Material Choice:
- While titanium is highly biocompatible, some research explores how different surface textures and materials might influence bacterial adhesion and tissue response. Our article on “Understanding Dental Implant Material Costs in Dallas: Zirconia vs. Titanium and Their Impact on Your Budget” delves into this.
During your initial consultation with a dentist in Dallas for tooth replacement options, it is important to discuss these design considerations to ensure your long-term oral health. Selecting an experienced provider who uses 3D guided implant surgery can significantly improve precision and reduce such risks [https://dallasdentalimplantcost.com/dallas-tx-dentists-using-3d-guided-implant-surgery-2026-precision-cost-faster-recovery/].
How Does Peri-Implantitis Progress Differently from Periodontitis?
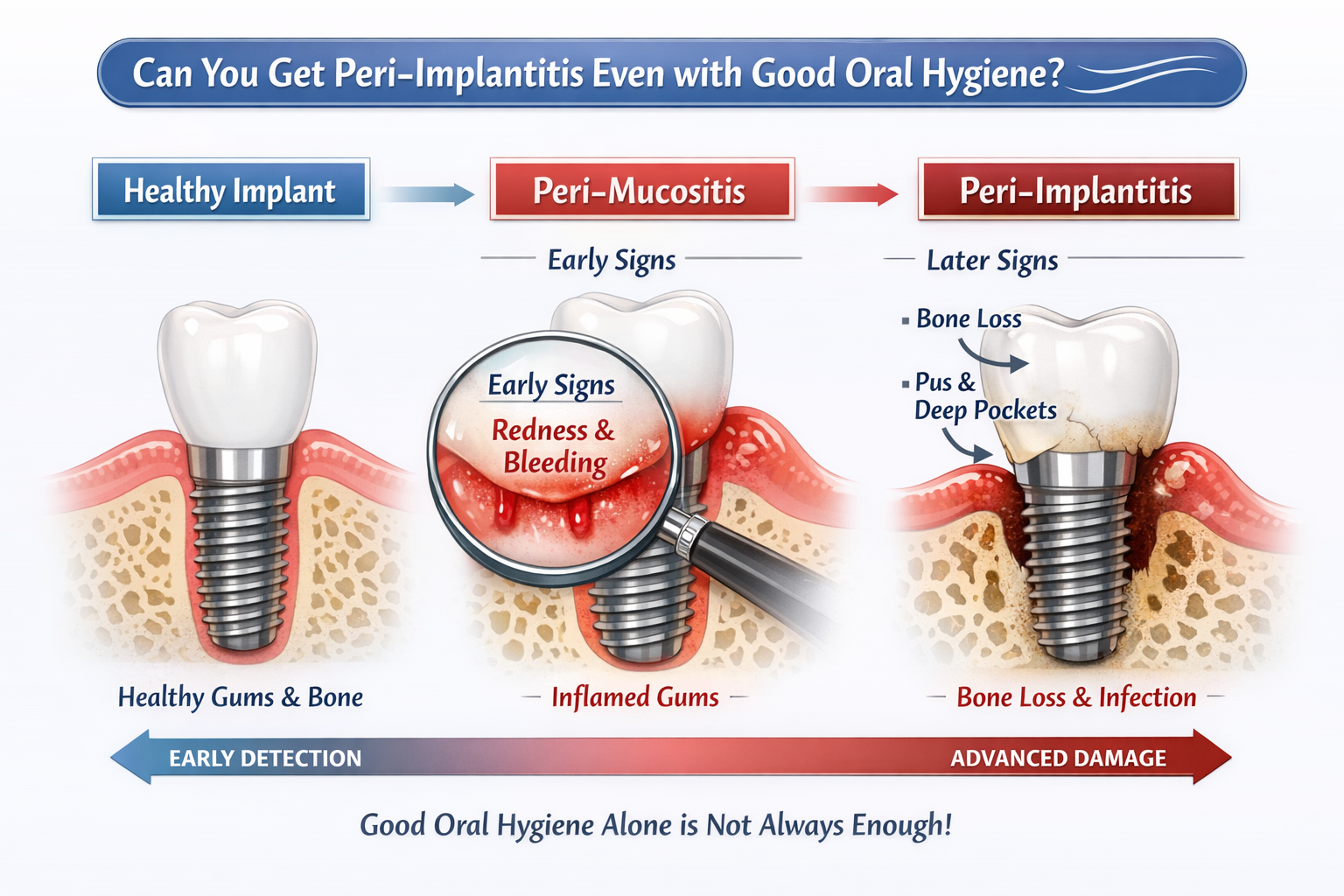
Peri-implant disease is generally more aggressive and causes significantly more damage in a shorter timeframe compared to periodontal disease [5]. This accelerated progression means that early detection and prompt intervention are even more critical for dental implants than for natural teeth. The primary reason for this difference lies in the unique anatomical structure surrounding an implant versus a natural tooth.
Here’s how their progression differs:
Anatomy:
- Natural Tooth: Has a periodontal ligament, a fibrous attachment system that helps resist bacterial invasion and distributes biting forces.
- Dental Implant: Lacks a periodontal ligament. The implant integrates directly with the bone (osseointegration), and the soft tissue attachment to the implant surface is a “seal” rather than a strong ligamentous attachment [6]. This seal is less resistant to bacterial penetration.
Blood Supply:
- Natural Tooth: Benefits from a rich, robust blood supply to the surrounding tissues, aiding in defense and repair.
- Dental Implant: Has a less vascularized soft tissue cuff compared to natural teeth, which can hinder the immune response and lead to faster tissue destruction once an infection sets in [5].
Inflammatory Response:
- Once bacteria establish around an implant, the inflammatory response can be more pronounced and less contained due to the lack of the protective periodontal ligament [5]. This leads to rapid breakdown of the supporting bone.
Progression Speed:
- Studies indicate that peri-implantitis can lead to substantial bone loss in a relatively short period, often months, compared to years for severe periodontitis [5]. This makes regular monitoring of dental implants in Dallas extremely important.
Because of these differences, even patients with excellent oral health education and practices need vigilant professional care to protect their implant investment.
Preventing Peri-Implantitis: Beyond Daily Brushing and Flossing
Preventing peri-implantitis goes far beyond just daily brushing and flossing; it requires a comprehensive, multi-faceted approach that involves patient education, lifestyle management, regular professional care, and careful dental implant procedure planning. While diligent home care is foundational, it’s only one piece of the puzzle for long-term oral health [2].
Here are key strategies for comprehensive peri-implantitis prevention:
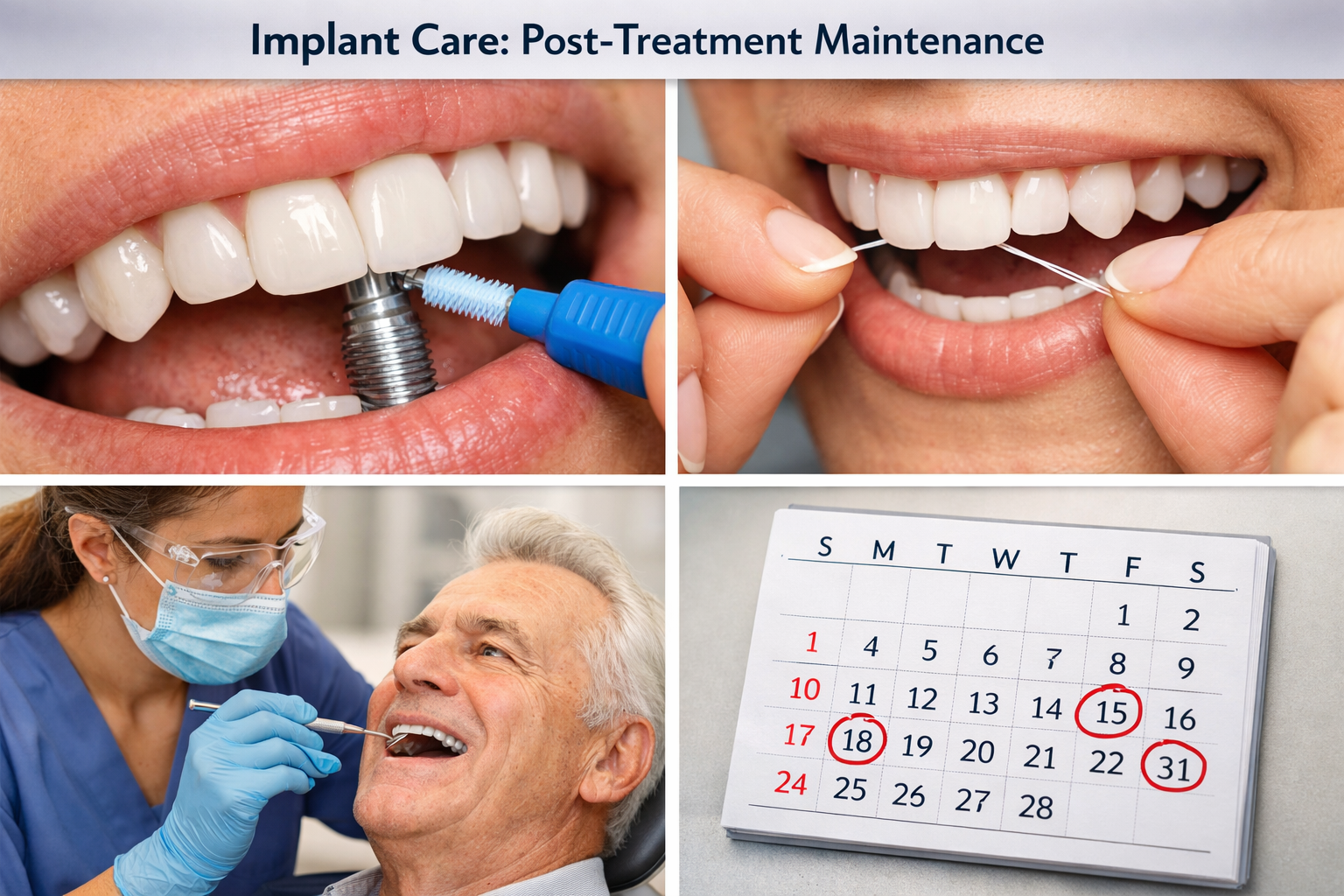
Strict Oral Hygiene, Adapted for Implants:
- Correct Brushing Technique: Use a soft-bristled toothbrush or an electric toothbrush, paying special attention to the gum line around the implant.
- Interdental Cleaning: Utilize interdental brushes, water flossers, or specialized implant floss designed to clean the areas between implants and natural teeth or between adjacent implants [7]. Your dental hygienist can demonstrate proper techniques during your visits for dental implants in Dallas.
- Antimicrobial Rinses: Your dentist might recommend specific mouthrinses to help control bacterial plaque.
Regular Professional Maintenance:
- Consistent Check-ups: Schedule regular check-ups, typically every 3-6 months, with your dentist or periodontist in Dallas [2]. These appointments are crucial for monitoring the health of your implants and detecting any early signs of inflammation or bone loss.
- Professional Cleanings: Dental hygienists use specialized tools to clean around implants without damaging their surfaces, removing plaque and calculus that home care might miss [7].
- Radiographic Monitoring: X-rays taken periodically help assess bone levels around the implants to detect subtle bone loss early.
Address Systemic Risk Factors:
- Smoking Cessation: Quitting smoking is one of the most impactful steps you can take to protect your implants [5].
- Diabetes Management: Maintaining good control of blood sugar levels is vital for diabetic patients.
- Manage Other Health Conditions: Work with your physician to manage any other chronic health conditions that could impact your immune system or healing capacity.
Optimal Implant Design and Placement:
- Careful Planning: Ensure your implant surgeon uses advanced imaging (like 3D CBCT scans) and planning software to achieve optimal implant position and angulation [https://dallasdentalimplantcost.com/the-role-of-3d-imaging-and-digital-planning-in-dallas-dental-implant-costs-and-success-rates/].
- Appropriate Crown & Abutment: Discuss with your dentist the design of your final restoration to ensure it’s cleansable and doesn’t create plaque traps.
Soft Tissue Management:
- In cases of thin or insufficient keratinized tissue around an implant, a soft tissue graft procedure might be recommended to improve tissue quality and resistance to disease [5].
By embracing these comprehensive strategies, patients can significantly reduce their risk of peri-implantitis and ensure the long-term success of their dental implants. Our “Dental Implant Post-Op Care & Maintenance Costs in Dallas: Protecting Your Investment for Decades” article provides additional guidance.
When to Consult a Dentist About Your Dental Implants in Dallas
It’s vital for anyone with dental implants in Dallas to know when to seek professional evaluation, especially since peri-implantitis can progress rapidly. Waiting for significant pain or mobility can mean more advanced disease that is harder to treat [5].
You should consult your dentist immediately if you experience any of the following signs or symptoms:
- Bleeding around the implant: Especially during brushing or flossing, or spontaneously.
- Redness or swelling of the gums: The tissue around the implant appears inflamed.
- Pus discharge: Any sign of pus coming from the gum around the implant.
- Persistent bad taste or bad breath: Can indicate an ongoing infection.
- Pain or discomfort around the implant: While some initial tenderness after the dental implant procedure is normal, persistent or new pain warrants investigation.
- Recession of the gum tissue: The gum line around the implant appears to be pulling away, exposing more of the implant or abutment.
- Looseness or mobility of the implant: This is a late sign of significant bone loss and requires urgent attention.
Early signs of peri-implantitis, such as inflammation without bone loss (peri-implant mucositis), are much easier to treat and often reversible [2]. Therefore, proactive monitoring and quick action are key to preserving your dental implant investment. Regular dental check-ups are specifically designed to catch these issues before they escalate.
FAQs About Peri-Implantitis and Oral Hygiene
Can an implant fail even if I brush and floss perfectly?
Yes, an implant can fail even with perfect brushing and flossing due to factors like systemic diseases, a history of periodontitis, genetic predisposition, or issues with implant design and placement [5, 7].
Is peri-implantitis common?
Peri-implantitis is a growing concern. Studies indicate that peri-implant mucositis (early inflammation without bone loss) can affect up to 43% of patients, and peri-implantitis (with bone loss) can affect 1-47% of implants, varying by study and definition [1, 8].
What is the most common cause of peri-implantitis?
The most common cause of peri-implantitis is bacterial plaque accumulation around the implant. However, other modifying factors, such as smoking and a history of gum disease, significantly increase susceptibility [5].
Can stress cause peri-implantitis?
While stress itself doesn’t directly cause peri-implantitis, chronic stress can weaken the immune system, making an individual more susceptible to infections and impacting the body’s ability to heal, which could indirectly contribute to the condition [4].
How is peri-implantitis treated?
Treatment for peri-implantitis varies based on severity. It can range from non-surgical approaches like debridement and antimicrobial therapy to surgical interventions to remove diseased tissue, clean the implant surface, and potentially regenerate lost bone [2].
Is peri-implantitis reversible?
Peri-implant mucositis (inflammation without bone loss) is generally reversible with improved oral hygiene and professional cleaning. However, peri-implantitis (inflammation with bone loss) is more challenging and often requires surgical intervention, and the lost bone may not fully regenerate [2].
How can I find a dentist in Dallas experienced in treating peri-implantitis?
When comparing dental implant clinics in Dallas, look for dentists or periodontists with specific experience in implantology and advanced training in managing peri-implant diseases. Asking about their success rates and treatment protocols for peri-implantitis is a good approach.
Conclusion
The question, “Can you get peri-implantitis even with good oral hygiene?” receives a clear answer: yes. While diligent oral care is foundational, it’s not the sole determinant of implant health. Systemic conditions like diabetes and smoking, a history of gum disease, and certain implant design elements all play significant roles in increasing your risk for peri-implantitis. As dental implants in Dallas continue to be a popular and effective solution for missing teeth, understanding these multifaceted risks is crucial. We encourage patients to prioritize regular professional check-ups, manage their overall health, and maintain open communication with their dental care providers. For anyone considering the dental implant procedure, or those already enjoying the benefits, proactive prevention and early detection are your best defense for long-term oral health.
References
[1] Pmc12756408 – https://pmc.ncbi.nlm.nih.gov/articles/PMC12756408/
[2] Protect Your Dental Implants In 2025 A Guide To Peri Implantitis – https://www.barclayfamilydental.com/protect-your-dental-implants-in-2025-a-guide-to-peri-implantitis
[3] Jper.25 0270 – https://aap.onlinelibrary.wiley.com/doi/full/10.1002/JPER.25-0270
[4] Full – https://www.frontiersin.org/journals/dental-medicine/articles/10.3389/fdmed.2026.1774378/full
[5] Peri Implant Diseases The Hygienists Role In Preserving Implant Health – https://www.todaysrdh.com/peri-implant-diseases-the-hygienists-role-in-preserving-implant-health/
[6] The Peri Implant Challenge – https://the-probe.co.uk/blog/2025/10/the-peri-implant-challenge/
[7] Preventing Peri Implantitis – https://dimensionsofdentalhygiene.com/article/preventing-peri-implantitis/
[8] Pmc10138758 – https://pmc.ncbi.nlm.nih.gov/articles/PMC10138758/

Leave a Reply
Share your thoughts or ask a question about dental implants. Your email address will not be published.