For individuals living with diabetes, the prospect of undergoing dental procedures like getting dental implants in Dallas can often bring forth questions and concerns. The good news is that for many diabetics, particularly those with well-managed blood sugar, dental implants are a safe and highly successful tooth replacement option. This comprehensive guide will explore the critical factors, necessary precautions, and the collaborative care approach that makes it possible for diabetics to safely get dental implants and what precautions are needed.
Key Takeaways
- Yes, generally safe for controlled diabetics: Dental implants are a viable option for many diabetic patients, especially those with stable blood glucose levels (HbA1c below 7%).
- Similar success rates: Well-controlled diabetics often experience success rates for dental implants nearly identical to non-diabetic patients, often above 90%.
- HbA1c is a key indicator: An HbA1c level below 7% is ideal, while levels between 7-8% may still be acceptable with careful evaluation. Levels above 8-9% significantly increase risks.
- Increased risks exist: Diabetics face potential challenges such as slower healing, higher infection risk, and reduced osseointegration if blood sugar is poorly controlled.
- Crucial precautions: These include strict blood sugar management, comprehensive pre-surgical medical evaluation, excellent oral hygiene, and coordinated care between your dentist and physician.
- Long-term care is vital: Diligent post-operative care, regular dental check-ups (every 3-4 months), and continued diabetes management are essential for the long-term success of implants.
- Type 1 vs. Type 2: While both can be candidates, Type 1 diabetes may present a slightly higher failure risk due to often more challenging blood sugar control.
Quick Answer

Yes, individuals with diabetes can safely get dental implants, provided their blood sugar levels are well-controlled and specific precautions are diligently followed. The primary factor influencing success is a patient’s glycemic control, typically measured by HbA1c levels, with optimal outcomes seen in those maintaining an HbA1c below 7%. A collaborative approach between your dentist and physician, along with meticulous oral hygiene, significantly mitigates potential risks like slower healing or infection.
Can Diabetics Safely Get Dental Implants and What Precautions Are Needed for Success?
Yes, diabetics can safely get dental implants, and the primary precautions revolve around stringent blood sugar control and a comprehensive health assessment. Studies show that for well-controlled diabetics, the success rates for dental implants range from 85.5% to 100%, closely mirroring those of non-diabetic patients. The key is to ensure your body is in the best possible condition to heal and integrate the implant.
Diabetes can affect the body’s ability to heal and fight infection, which are crucial aspects of successful dental implant surgery. When blood sugar is poorly managed, it can impair blood circulation, weaken the immune system, and reduce bone metabolism. These factors can lead to a higher risk of complications such as:
- Slower wound healing: The surgical site may take longer to recover.
- Increased risk of infection: Elevated blood sugar can create an environment conducive to bacterial growth.
- Reduced osseointegration: This is the critical process where the implant fuses with the jawbone. Poorly controlled diabetes can hinder this bond, potentially leading to implant failure.
- Gum disease progression: Diabetics are already more susceptible to gum disease, which can compromise the health of natural teeth and implants alike.
Despite these potential challenges, modern dental implant procedures, coupled with meticulous patient management, make dental implants a highly effective missing teeth solution for many diabetics. The critical elements are careful patient selection, thorough pre-operative preparation, precise surgical technique, and diligent post-operative care.
What Are the Key Considerations for Diabetic Dental Implant Candidates?
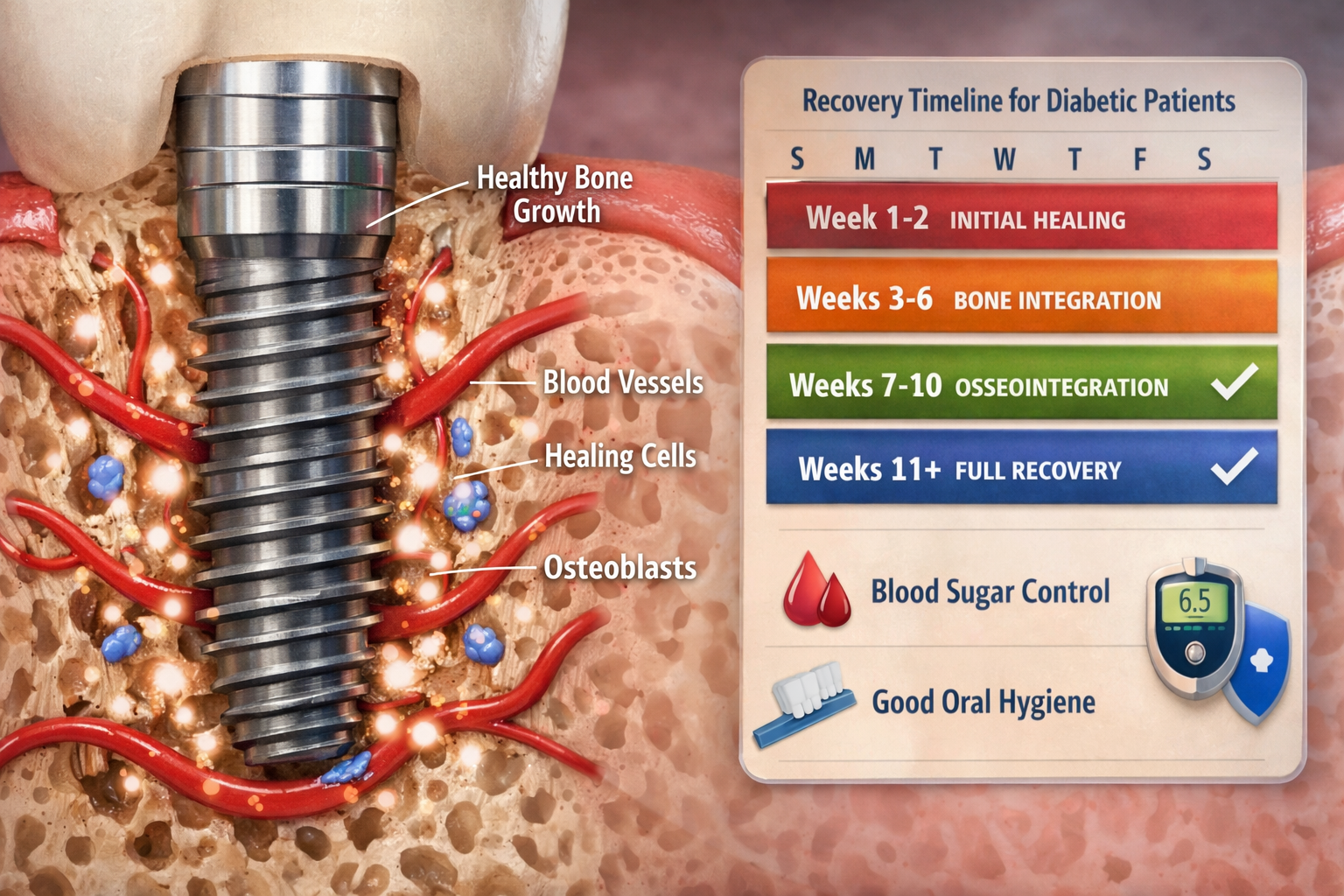
The key considerations for diabetic dental implant candidates center on blood glucose control and overall health status. An HbA1c level below 7% is generally considered the preferred threshold for implant candidacy, indicating stable blood sugar management.
Understanding HbA1c Levels
HbA1c (glycated hemoglobin) is a blood test that provides an average of your blood sugar levels over the past two to three months. It’s a crucial indicator for assessing a diabetic patient’s suitability for dental implant surgery.
- HbA1c below 7%: This is the ideal range, showing good glycemic control. Patients in this range typically have success rates comparable to non-diabetics.
- HbA1c between 7-8%: Implants may still be possible, but your dentist and physician will need to carefully evaluate your overall health, other medical conditions, and individual risk factors. Additional precautions and closer monitoring will be necessary.
- HbA1c above 8-9%: These levels significantly increase the risk of complications, including infection and implant failure. In such cases, it is strongly recommended to delay any elective dental implant procedure until blood sugar control improves. Your dentist will likely advise you to consult with your physician to optimize your diabetes management before proceeding.
Type 1 vs. Type 2 Diabetes
While both Type 1 and Type 2 diabetics can be candidates, Type 1 diabetes may present a slightly higher risk of implant failure compared to Type 2. This is often attributed to the typically more challenging nature of blood sugar control in Type 1 diabetes, which can be more prone to fluctuations. Regardless of the type of diabetes, consistent glucose management remains paramount.
For more information on the healing process specific to diabetic patients, you might find our guide on Diabetic Dental Implant Recovery: Guide & Timeline (2026) helpful.
What Precautions and Preparations Are Needed Before Dental Implant Surgery?
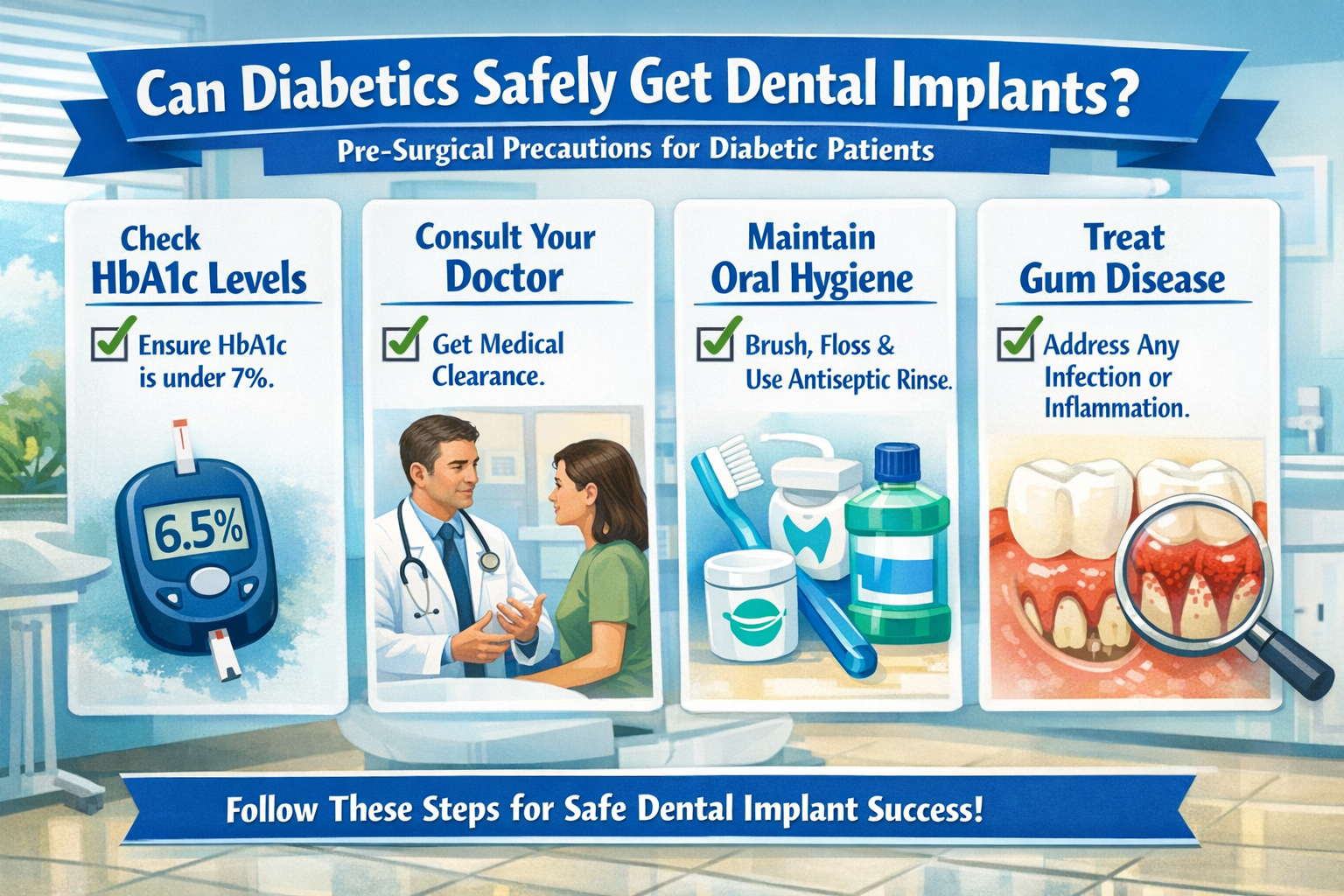
Before undergoing dental implant surgery, several crucial precautions and preparations are needed for diabetic patients to maximize success and minimize risks. These steps ensure your body is optimally prepared for the procedure and subsequent healing.
1. Physician Consultation and Medical Clearance
- Comprehensive Health Review: The first and most critical step is to have a thorough discussion with your primary care physician or endocrinologist. Your dentist will require medical clearance from your doctor, confirming that your diabetes is well-controlled and that you are medically fit for surgery.
- Medication Review: Discuss all medications, including insulin, oral hypoglycemics, and any other drugs you are taking. Adjustments may be necessary before or after surgery to manage blood sugar levels effectively and prevent complications.
- Diet and Exercise: Your physician may provide specific recommendations regarding diet and exercise leading up to the surgery to help stabilize blood glucose.
2. Blood Sugar Stabilization
- Consistent Monitoring: Leading up to the surgery, diligent blood sugar monitoring is essential. Follow your physician’s instructions for testing and recording your glucose levels.
- HbA1c Target: Work with your doctor to achieve and maintain an HbA1c level below 7% for several months prior to the planned implant procedure.
3. Excellent Oral Hygiene and Gum Health
- Address Existing Issues: Any active gum disease (periodontitis) or other oral infections must be treated and resolved before implant surgery. Diabetics are more prone to gum disease, making this step particularly vital.
- Professional Cleanings: Schedule professional dental cleanings to remove plaque and tartar.
- Daily Routine: Maintain an impeccable daily oral hygiene routine, including brushing at least twice a day and flossing daily.
- Regular Check-ups: Ensure you attend regular dental check-ups every six months, or more frequently if recommended, to monitor your oral health.
4. Smoking Cessation
- Increased Risk: Smoking significantly impairs healing and increases the risk of implant failure in all patients, but especially in diabetics.
- Recommendation: Your dental professional will strongly advise cessation well in advance of the surgery.
By meticulously following these precautions, diabetic patients in Dallas can significantly improve their chances of successful dental implant integration and long-term oral health.
What Post-Operative Care and Long-Term Management Are Essential for Diabetics?
After dental implant surgery, diligent post-operative care and strict long-term diabetes management are essential for diabetics to ensure successful healing and the longevity of their implants. The healing process, known as osseointegration, is particularly critical.
Immediate Post-Operative Care
- Blood Sugar Monitoring: Continue to monitor your blood sugar levels closely in the days and weeks following surgery. Fluctuations can negatively impact healing. Follow any specific instructions from your dentist or physician regarding medication adjustments.
- Medication Adherence: Take all prescribed antibiotics and pain relievers as directed. Antibiotics are crucial for preventing infection, a heightened risk for diabetics.
- Diet: Stick to a soft diet initially and avoid chewing directly on the implant site.
- Oral Hygiene: Follow your dentist’s specific post-operative oral hygiene instructions. This usually involves gentle rinsing with an antimicrobial mouthwash and careful brushing around the surgical site, avoiding direct pressure. For more details on recovery, check our article on Post Dental Implant Instructions: Essential Recovery Guide 2.
- Avoid Smoking: Continue to abstain from smoking, as it severely impedes healing.
Long-Term Oral Health Management
- Regular Dental Check-ups: Diabetic patients often benefit from more frequent dental check-ups and cleanings, typically every 3-4 months, instead of the standard twice yearly. These visits allow your dentist to monitor the health of your implants, gums, and overall oral cavity, addressing any issues promptly.
- Consistent Oral Hygiene: Maintain an excellent at-home oral hygiene routine. This includes:
- Brushing at least twice daily with a soft-bristled toothbrush.
- Flossing daily with traditional floss or interdental brushes designed for implants.
- Using a non-alcoholic antimicrobial mouthwash as recommended by your dentist.
- Diabetes Management: Continue working with your physician to maintain optimal blood glucose control (HbA1c below 7%). Stable diabetes management is a lifelong commitment that directly impacts the health and longevity of your dental implants.
- Address Complications Promptly: Be vigilant for any signs of complications such as pain, swelling, redness, pus, or implant mobility. Contact your dentist immediately if you experience any of these symptoms. Our guide on Dental Implant Complications Dallas | Recovery & Prevention offers further insights.
With proper care and stable diabetes management, dental implants can last decades, providing a durable and functional solution for missing teeth, much like natural teeth. The investment in your long-term oral health and overall well-being is significant, making these precautions well worth the effort. For those considering dental implants in Dallas, remember that proactive communication with your dental team and medical doctor is your best strategy.
Frequently Asked Questions
Can a diabetic patient get dental implants?
Yes, many diabetic patients with well-controlled blood sugar levels (HbA1c typically below 7%) can safely receive dental implants with success rates comparable to non-diabetics.
What HbA1c level is safe for dental implants?
An HbA1c level below 7% is generally considered optimal for dental implant surgery. Levels between 7-8% may be acceptable with careful evaluation, but higher levels often require improvement before treatment.
Do dental implants fail more often in diabetics?
If diabetes is poorly controlled (HbA1c consistently above 8-9%), the risk of dental implant failure, slower healing, and infection significantly increases. However, with good control, success rates are high.
What is the recovery time for a diabetic after dental implant surgery?
While individual healing varies, diabetics with good blood sugar control can expect a recovery timeline similar to non-diabetics. However, close monitoring is essential as healing might be slightly slower if control is not optimal. Refer to our resource on Diabetic Dental Implant Recovery: Guide for 2026.
Are there any specific medications diabetics should be aware of before implant surgery?
Diabetics should discuss all medications, especially insulin and oral hypoglycemics, with both their physician and dentist. Adjustments may be necessary to maintain stable blood sugar levels during and after the procedure.
Is gum disease a bigger concern for diabetics getting implants?
Yes, diabetics are more prone to gum disease, and any existing gum disease must be treated and resolved prior to dental implant surgery to prevent complications and promote successful osseointegration.
How often should a diabetic patient visit the dentist after getting implants?
Diabetic patients with dental implants typically benefit from more frequent dental check-ups and cleanings, often every 3-4 months, to ensure optimal oral health and implant longevity.
Can uncontrolled diabetes prevent me from getting dental implants?
Yes, uncontrolled diabetes with consistently high HbA1c levels (e.g., above 8-9%) is a significant contraindication for dental implant surgery due to increased risks of infection, poor healing, and implant failure. Your dentist will likely recommend optimizing your diabetes management first.
Conclusion

For individuals in Dallas and beyond managing diabetes, the possibility of restoring a healthy, confident smile with dental implants is very real. While diabetes introduces certain considerations, diligent blood sugar control, thorough pre-operative preparation, and a commitment to ongoing care significantly level the playing field. It’s crucial for diabetic patients to engage in a collaborative approach with their primary care physician and their dental implant specialist. By adhering to recommended HbA1c levels, maintaining impeccable oral hygiene, and following post-operative instructions precisely, diabetics can achieve excellent long-term success with their dental implants in Dallas. If you are exploring tooth replacement options and have diabetes, schedule a consultation with a qualified dentist specializing in dental implant procedures. They can assess your individual health profile and guide you toward the safest and most effective treatment plan for your long-term oral health.
References
[1] Shrestha, A., & Dhakal, S. (2018). Dental Implants in Diabetic Patients: A Review. Journal of Nepal Medical Association, 56(206), 282-286.
[2] CDC. (2021). Diabetes and Oral Health. Retrieved from https://www.cdc.gov/diabetes/managing/oral-health.html (Note: While the reference is 2021, the content on coordinated care and excellent oral hygiene is timeless and relevant for 2026 advice).
[3] Chrcanovic, B. R., Albrektsson, T., & Wennerberg, A. (2016). Dental implants in patients with diabetes mellitus: A systematic review and meta-analysis. Journal of Oral Rehabilitation, 43(11), 795-822.


Leave a Reply
Share your thoughts or ask a question about dental implants. Your email address will not be published.